Abstract
Introduction
Depending on severity of presentation, pituitary apoplexy can be managed with acute surgery or non-operatively. We aim to assess long-term tumour control, visual and endocrinological outcomes following pituitary apoplexy with special emphasis on patients treated non-operatively.
Methods
Multicentre retrospective cohort study. All patients with symptomatic pituitary apoplexy were included. Patients were divided into 3 groups: group 1: surgery within 7 days; group 2: surgery 7 days–3 months; group 3: non-operative. Further intervention for oncological reasons during follow-up was the primary outcome. Secondary outcome measures included visual and endocrinological function at last follow-up.
Results
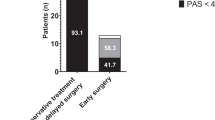
One hundred sixty patients were identified with mean follow-up of 48 months (n = 61 group 1; n = 34 group 2; n = 64 group 3). Factors influencing decision for surgical treatment included visual acuity loss (OR: 2.50; 95% CI: 1.02–6.10), oculomotor nerve palsy (OR: 2.80; 95% CI: 1.08–7.25) and compression of chiasm on imaging (OR: 9.50; 95% CI: 2.06–43.73). Treatment for tumour progression/recurrence was required in 17%, 37% and 24% in groups 1, 2 and 3, respectively (p = 0.07). Urgent surgery (OR: 0.16; 95% CI: 0.04–0.59) and tumour regression on follow-up (OR: 0.04; 95% CI: 0.04–0.36) were independently associated with long-term tumour control. Visual and endocrinological outcomes were comparable between groups.
Conclusion
Urgent surgery is an independent predictor of long-term tumour control following pituitary apoplexy. However, 76% of patients who successfully complete 3 months of non-operative treatment may not require any intervention in the long term.

Similar content being viewed by others
References
Almeida JP, Sanchez MM, Karekezi C et al (2019) Pituitary apoplexy: results of surgical and conservative management clinical series and review of the literature. World Neurosurg 130:e988–e999
Arafah BM, Harrington JF, Madhoun ZT, Selman WR (1990) Improvement of pituitary function after surgical decompression for pituitary tumor apoplexy. J Clin Endocrinol Metab 71(2):323–328
Armstrong MR, Douek M, Schellinger D, Patronas NJ (1991) Regression of pituitary macroadenoma after pituitary apoplexy. J Comput Assist Tomogr 15(5):832–834
Ayuk J, McGregor EJ, Mitchell RD, Gittoes NJL (2004) Acute management of pituitary apoplexy—surgery or conservative management? Clin Endocrinol (Oxf) 61(6):747–752
Bills DC, Meyer FB, Laws ER, Davis DH, Ebersold MJ, Scheithauer BW, Ilstrup DM, Abboud CF (1993) A retrospective analysis of pituitary apoplexy. Neurosurgery 33(4):602–8; discussion 608–9
Bonicki W, Kasperlik-Załuska A, Koszewski W, Zgliczyński W, Wisławski J (1993) Pituitary apoplexy: endocrine, surgical and oncological emergency. Incidence, clinical course and treatment with reference to 799 cases of pituitary adenomas. Acta Neurochir (Wien) 120(3–4):118–22
Bujawansa S, Thondam SK, Steele C, Cuthbertson DJ, Gilkes CE, Noonan C, Bleaney CW, MacFarlane IA, Javadpour M, Daousi C (2014) Presentation, management and outcomes in acute pituitary apoplexy: a large single-centre experience from the United Kingdom. Clin Endocrinol (Oxf) 80(3):419–424
Dubuisson AS, Beckers A, Stevenaert A (2007) Classical pituitary tumour apoplexy: clinical features, management and outcomes in a series of 24 patients. Clin Neurol Neurosurg 109(1):63–70
Giritharan S, Gnanalingham K, Kearney T (2016) Pituitary apoplexy—bespoke patient management allows good clinical outcome. Clin Endocrinol (Oxf) 85(3):415–422
Goshtasbi K, Abiri A, Sahyouni R, Mahboubi H, Raefsky S, Kuan EC, Hsu FPK, Cadena G (2019) Visual and endocrine recovery following conservative and surgical treatment of pituitary apoplexy: a meta-analysis. World Neurosurg 132:33–40
Gruber A, Clayton J, Kumar S, Robertson I, Howlett T, Mansell P (2006) Pituitary apoplexy: retrospective review of 30 patients—is surgical intervention always necessary? Br J Neurosurg. https://doi.org/10.1080/02688690601046678
Maccagnan P, Macedo CL, Kayath MJ, Nogueira RG, Abucham J (1995) Conservative management of pituitary apoplexy: a prospective study. J Clin Endocrinol Metab 80(7):2190–2197
Pangal DJ, Chesney K, Memel Z, Bonney PA, Strickland BA, Carmichael J, Shiroishi M, Jason Liu CS, Zada G (2020) Pituitary apoplexy case series: outcomes after endoscopic endonasal transsphenoidal surgery at a single tertiary center. World Neurosurg 1–7
Patel HC, Bouamra O, Woodford M, King AT, Yates DW, Lecky FE (2005) Trends in head injury outcome from 1989 to 2003 and the effect of neurosurgical care: an observational study. Lancet 366(9496):1538–1544
Rajasekaran S, Vanderpump M, Baldeweg S, et al (2011) UK guidelines for the management of pituitary apoplexy. Pituitary Apoplexy Guidelines Development Group: May 2010. Clin Endocrinol (Oxf) 74(1):9–20
Randeva HS, Schoebel J, Byrne J, Esiri M, Adams CBT, Wass JAH (1999) Classical pituitary apoplexy: clinical features, management and outcome. Clin Endocrinol (Oxf) 51(2):181–188
Reddy NL, Rajasekaran S, Han TS, Theodoraki A, Drake W, Vanderpump M, Baldeweg S, Wass JAH (2011) An objective scoring tool in the management of patients with pituitary apoplexy. Clin Endocrinol (Oxf) 75(5):723
Rutkowski MJ, Kunwar S, Blevins L, Aghi MK (2018) Surgical intervention for pituitary apoplexy: an analysis of functional outcomes. J Neurosurg 129(2):417–424
Seuk J-W, Kim C-H, Yang M-S, Cheong J-H, Kim J-M (2011) Visual outcome after transsphenoidal surgery in patients with pituitary apoplexy. J Korean Neurosurg Soc 49(6):339
Sibal L, Ball SG, Connolly V et al (2004) Pituitary apoplexy: a review of clinical presentation, management and outcome in 45 cases. Pituitary 7(3):157–163
Singh TD, Valizadeh N, Meyer FB, Atkinson JLD, Erickson D, Rabinstein AA (2015) Management and outcomes of pituitary apoplexy. J Neurosurg 122(6):1450–1457
Tu M, Lu Q, Zhu P, Zheng W (2016) Surgical versus non-surgical treatment for pituitary apoplexy: a systematic review and meta-analysis. J Neurol Sci 370:258–262
Woo H-J, Hwang J-H, Hwang S-K, Park Y-M (2010) Clinical outcome of cranial neuropathy in patients with pituitary apoplexy. J Korean Neurosurg Soc 48(3):213–218
Zhang X, Fei Z, Zhang W et al (2007) Emergency transsphenoidal surgery for hemorrhagic pituitary adenomas. Surg Oncol 16(2):115–120
Zieliński G, Witek P, Koziarski A, Podgórski J (2013) Spontaneous regression of non-functioning pituitary adenoma due to pituitary apoplexy following anticoagulation treatment—a case report and review of the literature. Endokrynol Pol 64(1):54–58
Funding
HJM is supported by the NIHR University College London (UCL) Biomedical Research Centre (BRC) and the Wellcome/EPSRC Centre for Interventional and Surgical Sciences (WEISS).
Author information
Authors and Affiliations
Contributions
KPB and SK participated in the design of the study, collected data, performed the statistical analysis and prepared the manuscript draft. SS, TS, RM and RWK participated in the design of the study and preparation of the manuscript. All authors participated in data collection and data analysis and reviewed and accepted the content of the manuscript.
Corresponding author
Ethics declarations
Ethics approval
Study was registered as audit. Study was approved by Institutional Review Boards and was not required to undergo Research Ethics Review.
Competing of interests
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Pituitaries
Rights and permissions
About this article
Cite this article
Budohoski, K.P., Khawari, S., Cavalli, A. et al. Long-term oncological outcomes after haemorrhagic apoplexy in pituitary adenoma managed operatively and non-operatively. Acta Neurochir 164, 1115–1123 (2022). https://doi.org/10.1007/s00701-022-05119-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-022-05119-8