Abstract
Objective
To quantitatively measure surgical degree of freedom (SDF) to the anterior communicating artery (AComA) complex via removal of the orbital rim. Comparisons of SDF quadrants were made between a supraorbital and standard frontotemporal pterional craniotomy according to the surgeons’ geometric microscope compass-based views.
Methods
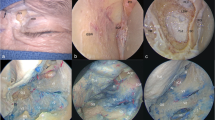
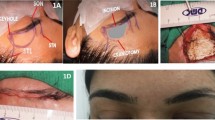
Eleven latex-injected formalin-fixed cadaveric heads; 14 sides (eight unilateral and three bilateral) were dissected. Standard frontotemporal pterional and subsequent supraorbital craniotomy approaches were conducted in each specimen. Point “0” was allocated as a point 1 cm distal to the ipsilateral A1 and A2 junction of AComA. The tip of a 10-cm long pointer was used to locate point 0. The base of the pointer stick was maneuvered outside the craniotomy in eight compass directions, with the most peripheral points expressed as target points 1–8. The center of this octagon was attributed point C. A pyramid was established by connecting the points 0, C, and 2 neighboring target points. A frameless stereotaxic instrument was used as a three-dimensional digitizer to measure pyramid volume. Each neighboring two pyramids form a hexagonal cone and was expressed as a surgical freedom quadrant (cm3). The quadrants are depicted counterclockwise (surgeons view) as orbital-nasal, vertex-nasal, vertex-temporal, and orbital-temporal.
Results
Total SDF obtained via supraorbital and pterional approaches were 122.8 ± 109.66 and 159.94 ± 93.65, respectively (mean ± SD cm3; supraorbital < pterional by 30.2%). Supraorbital to pterional, in the orbital-nasal quadrant was 21.9 ± 35.5 and 13.04 ± 8.7, vertex-nasal 31.3 ± 28.5 and 16.7 ± 13.7, vertex-temporal 39.5 ± 42.14 and 60.4 ± 4.7, and orbital-temporal 30.14 ± 42.14 and 70.01 ± 42.14, respectively (mean ± SD cm3). In the vertex-nasal quadrant, the supraorbital approach provides a 47.3% increase in SDF compared to the standard frontotemporal pterional craniotomy approach.
Conclusion
Given that the AComA complex is located more nasally and the surgeon’s view is more vertex, we propose that a supraorbital craniotomy allows a more contralateral portion of the AComA complex to be visualized during dissection.





Similar content being viewed by others
Abbreviations
- AComA:
-
Anterior communicating artery
- SD:
-
Standard deviation
- PTE:
-
Standard frontotemporal pterional
- SDF:
-
Surgical degree of freedom
- SUP:
-
Supraorbital
References
Ammirati M, Spallone A, Ma J, Cheatham M, Becker D (1993) An anatomicosurgical study of the temporal branch of the facial nerve. Neurosurgery 33:1038–1044. https://doi.org/10.1227/00006123-199312000-00012
Andaluz N, van Loveren HR, Keller JT, Zuccarello M (2003) Anatomic and clinical study of the orbitopterional approach to anterior communicating artery aneurysms. Neurosurgery 52:1140–1149. https://doi.org/10.1227/01.neu.0000057834.83222.9f
Beretta F, Andaluz N, Chalaala C, Bernucci C, Salud L, Zuccarello M (2010) Image-guided anatomical and morphometric study of supraorbital and transorbital minicraniotomies to the sellar and perisellar regions: comparison with standard techniques. J Neurosurg 113:975–981. https://doi.org/10.3171/2009.10.Jns09435
Cheng CM, Noguchi A, Dogan A, Anderson GJ, Hsu FP, McMenomey SO, Delashaw JB Jr (2013) Quantitative verification of the keyhole concept: a comparison of area of exposure in the parasellar region via supraorbital keyhole, frontotemporal pterional, and supraorbital approaches. J Neurosurg 118:264–269. https://doi.org/10.3171/2012.9.Jns09186
Figueiredo EG, Deshmukh P, Zabramski JM, Preul MC, Crawford NR, Siwanuwatn R, Spetzler RF (2005) Quantitative anatomic study of three surgical approaches to the anterior communicating artery complex. Oper Neurosurg 56:397–405. https://doi.org/10.1227/01.neu.0000156549.96185.6d
Figueiredo EG, Deshmukh V, Nakaji P, Deshmukh P, Crusius MU, Crawford N, Spetzler RF, Preul MC (2006) An Anatomical evaluation of the mini-supraorbital approach and comparison with standard craniotomies. Oper Neurosurg 59:ONS-212-ONS-220. https://doi.org/10.1227/01.neu.0000223365.55701.f2
Fujitsu K, Kuwabara T (1986) Orbitocraniobasal approach for anterior communicating artery aneurysms. Neurosurgery 18:367–369. https://doi.org/10.1227/00006123-198603000-00023
Hernesniemi J, Dashti R, Lehecka M, Niemelä M, Rinne J, Lehto H, Ronkainen A, Koivisto T, Jääskeläinen JE (2008) Microneurosurgical management of anterior communicating artery aneurysms. Surg Neurol 70:8–28. https://doi.org/10.1016/j.surneu.2008.01.056
Horgan MA, Anderson GJ, Kellogg JX, Schwartz MS, Spektor S, McMenomey SO, Delashaw JB (2000) Classification and quantification of the petrosal approach to the petroclival region. J Neurosurg:108–112. https://doi.org/10.3171/jns.2000.93.1.0108
Hsu FPK, Anderson GJ, Dogan A, Finizio J, Noguchi A, Liu KC, McMenomey SO, Delashaw JB (2004) Extended middle fossa approach: quantitative analysis of petroclival exposure and surgical freedom as a function of successive temporal bone removal by using frameless stereotaxy. J Neurosurg:695–699. https://doi.org/10.3171/jns.2004.100.4.0695
Jane JA, Park TS, Pobereskin LH, Winn RH, Butler AB (1982) The supraorbital approach: technical note. Neurosurgery 11:537–542. https://doi.org/10.1227/00006123-198210000-00016
Petraglia A, Moravan M, Jahromi B, Maurer P, Srinivasan V, Coriddi M, Vates G (2011) Unilateral subfrontal approach to anterior communicating artery aneurysms: a review of 28 patients. Surg Neurol Int 2:124. https://doi.org/10.4103/2152-7806.85056
Riina HA, Lemole GM, Spetzler RF (2002) Anterior communicating artery aneurysms. Neurosurgery 51:993–996. https://doi.org/10.1227/00006123-200210000-00026
Sekhar LN, Natarajan SK, Britz GW, Ghodke B (2007) Microsurgical management of anterior communicating artery aneurysms. Oper Neurosurg 61:ONS273–ONS292. https://doi.org/10.1227/01.neu.0000303980.96504.d9
Solomon RA (2001) Anterior communicating artery aneurysms. Neurosurgery 48:119–123. https://doi.org/10.1227/00006123-200101000-00021
Spektor S, Anderson GJ, McMenomey SO, Horgan MA, Kellogg JX, Delashaw JB (2000) Quantitative description of the far-lateral transcondylar transtubercular approach to the foramen magnum and clivus. J Neurosurg:824–831. https://doi.org/10.3171/jns.2000.92.5.0824
Suzuki J, Mizoi K, Yoshimoto T (1986) Bifrontal interhemispheric approach to aneurysms of the anterior communicating artery. J Neurosurg:183–190. https://doi.org/10.3171/jns.1986.64.2.0183
Vishteh AG, Marciano FF, David CA, Baskin JJ, Spetzler RF (1998) The pterional approach. Oper Tech Neurosurg 1:39–49. https://doi.org/10.1016/s1092-440x(98)80007-8
Acknowledgments
The authors thank Drs. Akio Noguchi, Gregory J. Anderson, Frank H. Hsu, Sean O. McMenomey, and Johnny B. Delashaw for their contributions in the cadaver laboratory, and Shirley McCartney, Ph.D., for her editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Cadaveric heads were provided by OHSU’s Body Donation Program with an Enrolment Form for Individual Donating to OHSU’s Whole Body Donation Program in place.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Neurosurgical Anatomy
Rights and permissions
About this article
Cite this article
Cheng, CM., Dogan, A. Quantitative measurement of the surgical freedom for anterior communicating artery complex—a comparative study between the frontotemporal pterional and supraorbital craniotomy; a laboratory study. Acta Neurochir 161, 2513–2519 (2019). https://doi.org/10.1007/s00701-019-04097-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-019-04097-8