Abstract
Background
Large tumors arising from the middle scalene region can displace the middle scalene muscle and distort regional anatomy, placing nerves at risk. Understanding the surgical anatomy of these nerves is key to approaching pathology of the middle scalene muscle and avoiding damage to the dorsal scapular, long thoracic, and spinal accessory nerves, each of which can cause scapular winging and associated morbidity if injured.
Methods
IRB approval was obtained for this study, allowing cases with relevant pathology to be reviewed and presented to highlight the relevant surgical technique. Anatomical depictions were created to correlate intraoperative images with known anatomical relationships.
Results
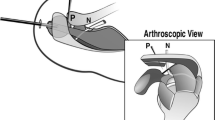
Key to this approach is consideration of the regional anatomy in a standard supraclavicular approach, the superficial plane, containing the anterior scalene muscle and brachial plexus, and the oblique plane containing the middle scalene muscle, long thoracic, spinal accessory, and dorsal scapular nerves. Identification and mobilization of each of these structures prior to lesion removal can not only provide likely boundaries of the tumor, but also allow for protection of the nerves to avoid injury that may lead to scapular winging with associated morbidity and functional impairment of the upper extremity.
Conclusions
Lesions of the middle scalene region often split two important anatomical planes, the superficial and deep, creating an advantageous surgical corridor through an anterolateral approach. Through early identification of known anatomy, these two planes can be developed, and a safe approach to the lesion of the middle scalene region can be exploited.




Similar content being viewed by others
References
Akgun K, Aktas I, Terzi Y (2008) Winged scapula caused by a dorsal scapular nerve lesion: a case report. Arch Phys Med Rehabil 89:2017–2020. https://doi.org/10.1016/j.apmr.2008.03.015
Belmonte R, Monleon S, Bofill N, Alvarado ML, Espadaler J, Royo I (2015) Long thoracic nerve injury in breast cancer patients treated with axillary lymph node dissection. Support Care Cancer 23:169–175. https://doi.org/10.1007/s00520-014-2338-5
Benoit P, Deplante F (1994) Paralysis of the dorsal nerve of the scapula: an unusual cause of scapular displacement. Presse Med 23:348
Bertelli JA, Ghizoni MF (2005) Long thoracic nerve: anatomy and functional assessment. J Bone Joint Surg Am 87:993–998. https://doi.org/10.2106/JBJS.D.02383
Bishop KN, Varacallo M (2018) Anatomy, shoulder and upper limb, dorsal scapular nerve. In: StatPearls. Treasure Island (FL)
Cesmebasi A, Spinner RJ (2015) An anatomic-based approach to the iatrogenic spinal accessory nerve injury in the posterior cervical triangle: how to avoid and treat it. Clin Anat 28:761–766. https://doi.org/10.1002/ca.22555
Crowe MM, Elhassan BT (2016) Scapular and shoulder girdle muscular anatomy: its role in periscapular tendon transfers. J Hand Surg Am 41:306–314; quiz 315. doi:https://doi.org/10.1016/j.jhsa.2015.06.123
Didesch JT, Tang P (2019) Anatomy, etiology, and management of scapular winging. J Hand Surg Am 44:321–330. https://doi.org/10.1016/j.jhsa.2018.08.008
Fardin P, Negrin P, Dainese R (1978) The isolated paralysis of the serratus anterior muscle: clinical and electromyographical follow-up of 10 cases. Electromyogr Clin Neurophysiol 18:379–386
Leinberry CF, Wehbe MA (2004) Brachial plexus anatomy. Hand Clin 20:1–5
Lung K, Lui F (2018) Anatomy, thorax, long thoracic nerve. In: StatPearls. Treasure Island (FL),
Malessy MJ, Thomeer RT, Marani E (1993) The dorsoscapular nerve in traumatic brachial plexus lesions. Clin Neurol Neurosurg 95(Suppl):S17–S23
Mandoorah S, Mead T (2018) Phrenic nerve injury. In: StatPearls. Treasure Island (FL),
Nevola Teixeira LF, Lohsiriwat V, Schorr MC, Luini A, Galimberti V, Rietjens M, Garusi C, Gandini S, Sarian LO, Sandrin F, Simoncini MC, Veronesi P (2014) Incidence, predictive factors, and prognosis for winged scapula in breast cancer patients after axillary dissection. Support Care Cancer 22:1611–1617. https://doi.org/10.1007/s00520-014-2125-3
Restrepo CE, Tubbs RS, Spinner RJ (2015) Expanding what is known of the anatomy of the spinal accessory nerve. Clin Anat 28:467–471. https://doi.org/10.1002/ca.22492
Rizzi SK, Haddad CA, Giron PS, Pinheiro TL, Nazario AC, Facina G (2016) Winged scapula incidence and upper limb morbidity after surgery for breast cancer with axillary dissection. Support Care Cancer 24:2707–2715. https://doi.org/10.1007/s00520-016-3086-5
Stone J, Puffer RC, Spinner RJ (2019) Interfascicular resection of benign peripheral nerve sheath tumors. JBJS Essential Surgical Techniques 9
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors have been compliant with all applicable ethical standards in the publication of this manuscript.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
IRB approval was obtained for this study. All patients included signed consent forms for the use of non-identifying medical information in medical research, including this study. For this type of study, formal consent is not required.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Comments
The brachial plexus and associated pathology can be approached, exposed, and dealt with from different angles and planes. This article from the prolific group at the Mayo Clinic provides an excellent description of how to safely approach and remove tumors in the region of the middle scalene muscle while minimizing or preventing damage to functionally important nerves, especially those involved with stabilization of the scapula so as to prevent winging. The application of their approach is beautifully demonstrated and illustrated using preoperative imaging, intraoperative photographs, and schematic diagrams from three of their cases. Their concept of partitioning and visualizing structures involving upper and middle portions of the brachial plexus into a superficial and deep or oblique plane is useful. They show that masses arising in the region of the middle scalene muscle expand or split these planes apart, thereby providing an anterolateral surgical corridor through which the surgeon can safely identify and preserve early on the dorsal scapular, long thoracic, and spinal accessory nerves which are not always specifically exposed and identified. An advantage in taking this approach is that there is less need to resect the anterior scalene muscle upon which the phrenic nerve courses. Overall, this article provides a very useful conceptual framework for the surgeon that is likely to benefit patients with pathology in the region of the middle scalene muscle.
Michel Kliot
CA, USA
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Neurosurgical Anatomy
Rights and permissions
About this article
Cite this article
Puffer, R.C., Stone, J. & Spinner, R.J. Avoidance of scapular winging while approaching tumors of the middle scalene region. Acta Neurochir 161, 1937–1942 (2019). https://doi.org/10.1007/s00701-019-04009-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-019-04009-w