Abstract
Background
The molecular mechanism of hemorrhagic stroke is unclear, and the identification of therapeutic agents for attenuating post-stroke brain damage remains an unresolved challenge. Dexamethasone (DEX) is used clinically to treat spinal cord injury and brain tumor patients by reducing edema formation, but has produced conflicting results in stroke management.
Methods
In this study, intracerebral hemorrhage (ICH) was induced in rats by intracranial stereotactic injection of collagenase into the caudate nucleus. DEX was given immediately and 3 days after ICH. The expression of intercellular adhesion molecule-1 (ICAM-1), matrix metalloproteinase-9 (MMP-9), nuclear factor (NF)-κB, and IκB were analyzed by Western blotting, and perihematomal edema formation was evaluated by magnetic resonance imaging.
Results
The results showed that ICH caused an increase of ICAM-1 and MMP-9 expression from 4 h to 7 days, which was inhibited following the administration of DEX. The perihematomal edema volume in ICH rats was high, with two peak periods at 12 h and 3 days, which was also reduced in DEX-treated groups. Furthermore, the administration of DEX not only maintained IκB in cytoplasm, but also decreased NF-κB elevation in the nucleus at 3 and 5 days in ICH rats.
Conclusions
In conclusion, these data show that DEX successfully reduced post-stroke brain edema by decreasing MMP-9 and ICAM-1 levels, partially through the IκB/NF-κB signaling pathway. The timing of DEX administration in relation to the onset of brain injury may be critical.




Similar content being viewed by others
References
Abbott NJ, Patabendige AA, Dolman DE, Yusof SR, Begley DJ (2010) Structure and function of the blood-brain barrier. Neurobiol Dis 37:13–25
Aid S, Silva AC, Candelario-Jalil E, Choi SH, Rosenberg GA, Bosetti F (2010) Cyclooxygenase-1 and −2 differentially modulate lipopolysaccharide-induced blood-brain barrier disruption through matrix metalloproteinase activity. J Cereb Blood Flow Metab 30:370–380
Davis SM, Donnan GA (2004) Steroid for stroke: another potential therapy discarded prematurely? Stroke 35:230–231
Desai P, Prasad K (1998) Dexamethasone is not necessarily unsafe in primary supratentorial intracerebral haemorrhage. J Neurol Neurosurg Psychiatry 65:799–800
Dietrich JB (2002) The adhesion molecule ICAM-1 and its regulation in relation with the blood-brain barrier. J Neuroimmunol 128:58–68
Gomes JA, Stevens RD, Lewin ШJJ, Mirski MA, Bhardwaj A (2005) Glucocorticoid therapy in neurologic critical care. Crit Care Med 33:1214–1224
Gu YT, Zhang H, Xue YX (2007) Dexamethasone treatment modulates aquaporin-4 expression after intracerebral hemorrhage in rats. Neurosci Lett 413:126–131
Hall ED, Braughler JM (1982) Glucocorticoid mechanisms in acute spinal cord injury: a review and therapeutic rationale. Surg Neurol 18:320–327
Harkness KA, Adamson P, Sussman JD, Davies-Jones GAB, Greenwood J, Woodroofe MN (2000) Dexamethasone regulation of matrix metalloproteinase expression in CNS vascular endothelium. Brain 123:698–709
Kasselman LJ, Kintner J, Sideris A, Pasnikowski E, Krellman JW, Shah S, Rudge JS, Yancopoulos GD, Wiegand SJ, Croll SD (2007) Dexamethasone treatment and ICAM-1 deficiency impair VEGF-induced angiogenesis in adult brain. J Vasc Res 44:283–291
Katsu M, Niizuma K, Yoshioka H, Okami N, Sakata H, Chan PH (2010) Hemoglobin-induced oxidative stress contributes to Matrix metalloproteinase activation and blood-brain barrier dysfunction in vivo. J Cereb Blood Flow Metab 30:1939–1950
Kothari RU, Brott T, Broderick JP, Barsan WG, Sauerbeck LR, Zuccarello M, Khoury J (1996) The ABCs of measuring intracerebral hemorrhage volumes. Stroke 27:1304–1305
Lee ST, Chu K, Jung KH, Kim J, Kim EH, Kim SJ, Sinn DI, Ko SY, Kim M, Roh JK (2006) Memantine reduces hematoma expansion in experimental intracerebral hemorrhage, resulting in functional improvement. J Cereb Blood Flow Metab 26:536–544
Lema PP, Girard C, Vachon P (2005) High doses of methylprednisolone are required for the treatment of collagenase-induced intracerebral hemorrhage in rats. Can J Vet Res 69:253–259
Li ZQ, Liang GB, Xue YX, Liu YH (2009) Effects of combination treatment of dexamethasone and Melatonin on brain injury in intracerebral hemorrhage model in rats. Brain Res 1264:98–103
Norris JW (2004) Steroids may have a role in stroke therapy. Stroke 35:228–229
Poungvarin N (2004) Steroids have no role in stroke therapy. Stroke 35:229–230
Poungvarin N, Bhoopat W, Viriyavejakul A, Rodprasert P, Buranasiri P, Sukondhabhant S, Hensley MJ, Strom BL (1987) Effects of dexamethasone in primary supratentorial intracerebral hemorrhage. N Engl J Med 316:1229–1233
Ridder DA, Schwaninger M (2009) NF-κB signaling in cerebral ischemia. Neuroscience 158:995–1006
Rincon F, Mayer SA (2008) Clinical review: critical care management of spontaneous intracerebral hemorrhage. Crit Care 12:237–251
Rosell A, Ortega-Aznar A, Alvarez-Sabín Fernández-Cadenas I, Ribó M, Molina CA, Lo EH, Montaner J (2006) Increased brain expression of matrix metalloproteinase-9 after ischemic and hemorrhagic human stroke. Stroke 37:1399–1406
Rosenberg GA, Mun-Bryce S, Wesley M, Kornfeld M (1990) Collagenase-induced intracerebral hemorrhage in rats. Stroke 21:801–807
Saporito MS, Brown ER, Hartpence KC, Wilcox HM, Robbins E, Vaught JL, Carswell S (1994) Systemic dexamethasone administration increases septal Trk autophosphorylation in adult rats via an induction of nerve growth factor. Mol Pharmacol 45:395–401
Savard C, Lema PP, Hélie P, Vachon P (2009) Effects of timing of dexamethasone treatment on the outcome of collagenase-induced intracerebral hematoma in rats. Comp Med 59:444–448
Steiner O, Coisne C, Cecchelli R, Boscacci R, Deutsch U, Engelhardt B, Lyck R (2010) Differential roles for endothelial ICAM-1, ICAM-2, and VCAM-1 in shear-resistant T cell arrest, polarization, and directed crawling on blood-brain barrier endothelium. J Immunol 185:4846–4855
Tellez H, Bauer RB (1973) Dexamethasone as treatment in cerebrovascular disease. 1. A controlled study in intracerebral hemorrhage. Stroke 4:541–546
Thiex R, Tsirka SE (2007) Brain edema after intracerebral hemorrhage: mechanisms, treatment options, management strategies, and operative indications. Neurosurg Focus 22:1–7
Wang J, Doré S (2007) Inflammation after intracerebral hemorrhage. J Cereb Blood Flow Metab 27:894–908
Wang J, Tsirka SE (2005) Neuroprotection by inhibition of matrix metalloproteinases in a mouse model of intracerebral haemorrhage. Brain 128:1622–1633
Wang Q, Tang XN, Yenari MA (2007) The inflammatory response in stroke. J Neuroimmunol 184:53–68
Xi G, Keep RF, Hoff JT (2002) Pathophysiology of brain edema formation. Neurosurg Clin N Am 13:371–383
Xi G, Keep RF, Hoff JT (2006) Mechanisms of brain injury after intracerebral haemorrhage. Lancet Neurol 5:53–63
Xue M, Yong VM (2008) Matrix metalloproteinases in intracerebral hemorrhage. Neurol Res 30:775–782
Yamaguchi M, Jadhav V, Obenaus A, Colohan A, Zhang JH (2007) Matrix metalloproteinase inhibition attenuates brain edema in an in vivo model of surgically-induced brain injury. Neurosurgery 61:1067–1075
Zhang X, Li H, Hu S, Zhang L, Liu C, Zhu C, Liu R, Li C (2006) Brain edema after intracerebral hemorrhage in rats: the role of inflammation. Neurol India 54:402–407
Acknowledgments
This work was supported by grant NSC 96-2314-B-182A-013 from the National Science Council and grant CMRPG 690501 from the Chang Gung Medical Research Council, Taiwan, ROC.
Conflicts of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
Comment
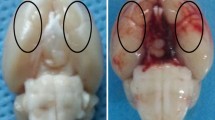
This is an elegantly performed experimental investigation, utilising state-of-the art methodologies to assess the neuroprotective effect of DEX in a well-established rat model of ICH. The results are sound and convincingly discussed. Differently from blood-injection techniques, the collagenase method produces ICH mimicking a more human-like evolving bleeding. There is a more pronounced interindividual variability of size and time course of the resulting ICHs. In this respect, including MRI images used for edema assessment is a useful adjunct, adding value to this paper. The dosing and time course of DEX administration are critical issues. Expression of ICAM-1 was significantly affected by DEX at all experimental time points, expression of MPP-9 only at the very early and very late stages of ICH production. Edema formation was reduced at 12 h and 3–5 days thereafter. It could be that a different dose-response curve could be obtained wiht another dosing. In conclusion, this is an interesting investigation proposing the reassessment of the pharmacodynamics of an old and controversial drug in a modern and sophisticated experimental setting. Translation of these results in the clinical field is still far away.
Domenico d'Avella
Padova, Italy
Rights and permissions
About this article
Cite this article
Yang, JT., Lee, TH., Lee, IN. et al. Dexamethasone inhibits ICAM-1 and MMP-9 expression and reduces brain edema in intracerebral hemorrhagic rats. Acta Neurochir 153, 2197–2203 (2011). https://doi.org/10.1007/s00701-011-1122-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-011-1122-2