Summary
Background. Cranial neurosurgical procedures utilising burr-holes lead to development of cosmetically unacceptable puckered scars on the scalp over burr-hole sites. Ceramics, especially Hydroxyapatite (HA) are good bone substitutes owing to their biocompatibility and osteoconduction i.e. ability to lay down bone over the implant by fibrovascular invasion and later bone formation. The Sree Chitra Tirunal Institute for Medical Sciences and Technology in India has pioneered research in this direction and has developed a unique porous-dense bilayer HA burr-hole button. This study evaluates the safety, cosmetic effect, as well as the radiological outcome following implantation of these bilayer HA buttons.
Method. Sixty-five HA buttons were implanted in 22 patients who underwent cranial neurosurgical procedures at the Sree Chitra Tirunal Institute for Medical Sciences and Technology. We assessed the cosmetic outcome (absence of puckered scar over burr hole sites, absence of allergic reactions or infections associated with the implant) as well as the radiological outcome with X-rays at specified intervals and looked for interference in the postoperative neurological imaging due to the implants.
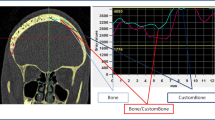
Results. There were no adverse events related to the HA buttons in the form of allergic reactions or infections. The implants persisted as radio-dense opacities on skull X-rays of recipients for up to two years. It did not lead to artefacts on postoperative CT or MR imaging of the brain. In particular, the HA buttons could be subtracted on Digital Subtraction Angiography and did not obstruct visualisation of the cerebral vasculature.
Conclusion. The bi-layer porous-dense HA buttons are useful in preventing cosmetic defects over burr-hole sites on the scalp after cranial neurosurgical procedures. It does not interfere with current radiological imaging methods in the postoperative phase.
Similar content being viewed by others
References
FCPM Adraansen HL Verwoerd-Verhoef RO van der Heul CDA Verwoed (1986) Implants of hydroxyapatite in the cricoid P Christel A Meunier AJC Lee (Eds) Biological and biomechanical performances of biomaterials Elsevier Science Amsterdam 5–8
RHB Alfred JGN Swart (1982) ArticleTitleOrbital roof reconstruction with a hydroxyapatite implant J Oral Maxillofac Surg 40 237–239 Occurrence Handle10.1016/0278-2391(82)90320-2
ME Cabanela MD Coventry CS MacCarty WE Miller (1972) ArticleTitleThe fate of patients with methyl methacrylate cranioplasty J Bone Joint Surg 54 278–281 Occurrence Handle4651261 Occurrence Handle1:STN:280:DyaE3s%2Fptl2rtQ%3D%3D
S Kobayashi H Hara H Okudera T Takemae K Sugita (1987) ArticleTitleUsefulness of ceramic implants in neurosurgery Neurosurgery 21 751–755 Occurrence Handle3696417 Occurrence Handle10.1097/00006123-198711000-00032 Occurrence Handle1:STN:280:DyaL1c%2FpsFSmuw%3D%3D
L Linder (1976) ArticleTitleTissue reaction to methyl methacrylate monomer: a comparative study in the rabbit’s ear on the toxicity of methyl metacrylate of varying composition Acta Orthop Scand 47 3–9 Occurrence Handle1266590 Occurrence Handle1:CAS:528:DyaE2sXlt1Kqur4%3D Occurrence Handle10.3109/17453677608998965
K Matsumoto E Kohmura A Kato T Hayakawa (1998) ArticleTitleRestoration of small bone defects at craniotomy using autologous bone dust and fibrin glue Surg Neurol 50 344–346 Occurrence Handle9817457 Occurrence Handle10.1016/S0090-3019(98)00081-0 Occurrence Handle1:STN:280:DyaK1M%2Fjt1eqtw%3D%3D
KV Menon HK Varma (2005) ArticleTitleRadiological outcome of tibial plateau fractures treated with percutaneously introduced synthetic porous hydroxyapatite granules Eur J Orthop Surg Traumatol 15 205–213 Occurrence Handle10.1007/s00590-005-0238-6
A Pompili F Caroli L Carpenese M Caterino L Raus GBS Sestili E Occhipinti (1998) ArticleTitleCranioplasty performed with new osteoconductive, osteoinducing hydroxyapatite-derived material J Neurosurg 89 236–242 Occurrence Handle9688118 Occurrence Handle1:STN:280:DyaK1czltFCjtg%3D%3D Occurrence Handle10.3171/jns.1998.89.2.0236
C Rawlings (1993) ArticleTitleModern bone substitutes with emphasis on calcium phosphate ceramics and osteoinductors Neurosurgery 33 935–938 Occurrence Handle8264898 Occurrence Handle10.1097/00006123-199311000-00027
CE Rawlings SuffixIII RH Wilkins (1996) Calcium phosphate ceramics as bone substitutes RH Wilkins SS Rengachary (Eds) Neurosurgery McGraw Hill New York 625–630
A Sanan SJ Haines (1997) ArticleTitleRepairing holes in the head: a history of cranioplasty Neurosurgery 40 588–603 Occurrence Handle9055300 Occurrence Handle10.1097/00006123-199703000-00033 Occurrence Handle1:STN:280:DyaK2s3gvVSltg%3D%3D
PD Waite RB Morawetz E Zeiger JL Pincock (1989) ArticleTitleReconstruction of cranial defects with porous Hydroxyapatite blocks Neurosurgery 25 214–217 Occurrence Handle2549443 Occurrence Handle10.1097/00006123-198908000-00010 Occurrence Handle1:STN:280:DyaL1MzmsFClsQ%3D%3D
T Yamashima (1988) ArticleTitleReconstruction of surgical skull defects with hydroxyapatite ceramic buttons and granules Acta Neurochir (Wien) 90 157–162 Occurrence Handle10.1007/BF01560572 Occurrence Handle1:STN:280:DyaL1c7otVCgug%3D%3D
T Yamashima (1989) ArticleTitleCranioplasty with ceramic plates that can be easily be trimmed during surgery Acta Neurochir (Wien) 96 149–153 Occurrence Handle10.1007/BF01456175 Occurrence Handle1:STN:280:DyaL1M3isFehsw%3D%3D
T Yamashima (1993) ArticleTitleModern cranioplasty with hydroxyapatite ceramic granules, buttons and plates Neurosurgery 33 939–940 Occurrence Handle8264899 Occurrence Handle10.1097/00006123-199311000-00028 Occurrence Handle1:STN:280:DyaK2c%2FovVylug%3D%3D
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Easwer, H., Rajeev, A., Varma, H. et al. Cosmetic and radiological outcome following the use of synthetic hydroxyapatite porous-dense bilayer burr-hole buttons. Acta Neurochir (Wien) 149, 481–486 (2007). https://doi.org/10.1007/s00701-007-1131-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-007-1131-3