Abstract
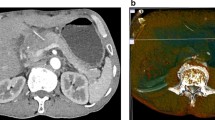
We present herein a case where a benign bile duct stricture developed 16 years after an open cholecystectomy and without any prior symptoms. The patient was thought to have a Klatskin tumor both pre- and intraoperatively and was treated with a resection of the mass and bile duct confluence, while hepaticojejunostomies were also performed to both ducts separately. A pathologic examination of the specimen revealed extensive fibrosis, chronic inflammation, and a nonnecrotizing granulomata. Any hilar mass presenting after upper abdominal surgery should therefore be considered to be potentially a benign bile duct stricture, even with a long symptom-free interval.
Similar content being viewed by others
References
Verbeek PCM, van Leeuwen DJ, de Wit LTh, Reeders JWAJ, Smits NJ, Bosma A, Huibregtse K, van der Heyde MN (1992) Benign fibrosing disease at the hepatic confluence mimicking Klatskin tumors. Surgery 112:866–871
Lillemoe KD, Pitt HA, Cameron JL (1992) Current management of benign bile duct strictures. Adv Surg 25:119–174
Pitt HA, Miyamoto T, Parapatis SK, Tompkins RK, Longmire WP (1982) Factors influencing outcome in patients with postoperative biliary strictures. Am J Surg 144:14–21
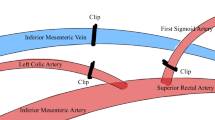
Northover JMA, Terblanche J (1979) A new look at the arterial supply of the bile duct in man and its surgical implications. Br J Surg 66:379–384
Joske RA, Finlay-Jones LR (1966) Amputation neuroma of the cystic duct stump. Br J Surg 53:766–768
Layfield LJ, Wax TD, Lee JG, Cotton PB (1995) Accuracy and morphologic aspects of pancreatic and biliary duct brushings. Acta Cytol 39:11–18
Scudera PL, Koizumi J, Jacobson IM (1990) Brush cytology evaluation of lesions encountered during ERCP. Gastrointest Endosc 36:281–284
Ryan ME (1991) Cytologic brushings of ductal lesions during ERCP. Gastrointest Endosc 37:139–142
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Bayar, S., Saxena, R. & Salem, R.R. Foreign body reaction to a metal clip causing a benign bile duct stricture 16 years after open cholecystectomy: Report of a case. Surg Today 30, 534–536 (2000). https://doi.org/10.1007/s005950070122
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1007/s005950070122