Abstract
Purpose
To evaluate the clinical efficacy of immediate breast reconstruction with free or pedicled laparoscopically harvested omental flaps (LHOFs).
Methods
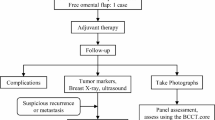
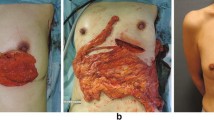
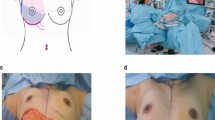
Between March 2011 and 2021, 82 patients who underwent immediate breast reconstruction with free or pediculated omental flaps were enrolled. Breast total or partial mastectomy, laparoscopic greater omentum harvest, and breast reconstruction were carried out in an orderly manner. Postoperative operative results, cosmetic outcomes, and complications were investigated.
Results
Seventeen cases of free LHOF and 65 cases of pedicled LHOF were performed. Cosmetic results were mostly satisfactory (61% excellent, 35% good), with a soft breast that was natural in appearance. Satisfaction investigation showed that 96.2% of patients were satisfied with the reconstructed breast. Uneventful follow-up showed no abdominal complications at the donor site, and the surface skin displayed no swelling. No major complications were found, except for three cases of necrosis. One patient developed slight hematoma. Two patients were found to have local recurrence, and one had distant metastasis. Twenty-four patients accepted radiotherapy, but no size reduction was noted after radiotherapy. We followed the patients to determine their survival status. All patients were alive, except for 1 in the free LHOF group who died 31.2 months after surgery.
Conclusion
Immediate breast reconstruction with LHOF provides a soft reconstructed breast with relatively little donor-site deformity and is useful for breast tumor-specific immediate reconstruction.





Similar content being viewed by others
References
Sakorafas GH, Safioleas M. Breast cancer surgery: an historical narrative. Part III. From the sunset of the 19th to the dawn of the 21st century. Eur J Cancer Care. 2010;19:145–66.
Losken A, Carlson GW, Bostwick J, Jones GE, Culbertson JH, Schoemann M. Trends in unilateral breast reconstruction and management of the contralateral breast: the Emory experience. Plast Reconstr Surg. 2002;110:89–97.
Recht A, Edge SB, Solin LJ, Robinson DS, Estabrook A, Fine RE, et al. Postmastectomy radiotherapy: clinical practice guidelines of the American Society of Clinical Oncology. J Clin Oncol. 2001;19:1539–69.
Zaha H, Inamine S, Naito T, Nomura H. Laparoscopically harvested omental flap for immediate breast reconstruction. Am J Surg. 2006;192:556–8.
Kaya B, Serel S. Breast reconstruction. Exp Oncol. 2013;35:280–6.
Sigurdson L, Lalonde DH. MOC-PSSM CME article: breast reconstruction. Plast Reconstr Surg. 2008;121:1–12.
Costanzo D, Klinger M. The evolution of autologous breast reconstruction. Breast J. 2020;26:2223–5.
Li N, Zheng Z, Li J, Fan J, Wang T, Zhang J, et al. Immediate breast reconstruction with omental flap for luminal breast cancer patients: ten clinical case reports. Medicine. 2017;96: e7797.
Li M, Shi Y, Li Q, Guo X, Han X, Li F. Oncological safety of autologous fFat grafting in breast reconstruction: a meta-analysis based on matched cohort studies. Aesth Plast Surg. 2022;46:1189–200.
van Alphen TC, Fechner MR, Smit JM, Slooter GD, Broekhuysen CL. The laparoscopically harvested omentum as a free flap for autologous breast reconstruction. Microsurgery. 2017;37:539–45.
Craggs B, Vanmierlo B, Zeltzer A, Buyl R, Haentjens P, Hamdi M. Donor-site morbidity following harvest of the transverse myocutaneous gracilis flap for breast reconstruction. Plast Reconstr Surg. 2014;134:682e–91e.
Pinell-White XA, Kapadia SM, Losken A. The management of abdominal contour defects following TRAM flap breast reconstruction. Aesth Surg J. 2014;34:264–71.
Nelson JA, Chung CU, Fischer JP, Kanchwala SK, Serletti JM, Wu LC. Wound healing complications after autologous breast reconstruction: a model to predict risk. J Plast Reconstr Aesth Surg. 2015;68:531–9.
Olsen MA, Lefta M, Dietz JR, Brandt KE, Aft R, Matthews R, et al. Risk factors for surgical site infection after major breast operation. J Am Coll Surg. 2008;207:326–35.
Nykiel M, Sayid Z, Wong R, Lee GK. Management of mastectomy skin flap necrosis in autologous breast reconstruction. Ann Plast Surg. 2014;72(Suppl 1):S31-34.
Zhu H, Xie Y, Xie F, Gu B, Liu K, Zan T, et al. Prevention of necrosis of adjacent expanded flaps by surgical delay. Ann Plast Surg. 2014;73:525–30.
Sui M, Zhang L, Yang J, Zeng L, Zhao W, Zhu Y. A new HC-A II solution for kidney preservation: a multi-center randomized controlled trial in China. Ann Transplant. 2014;19:614–20.
Shimada Y, Okumura T, Nagata T, Sawada S, Matsui K, Hori R, et al. Usefulness of blood supply visualization by indocyanine green fluorescence for reconstruction during esophagectomy. Esophagus. 2011;8:259–66.
Lomonte C, Meola M, Petrucci I, Casucci F, Basile C. The key role of color Doppler ultrasound in the work-up of hemodialysis vascular access. Semin Dial. 2015;28:211–5.
Funding
This work was supported by The National Natural Science Foundation of China (No. 81472598).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shen, G., Yang, Y., Huang, M. et al. Immediate breast reconstruction with laparoscopically harvested omental flap: A retrospective analysis with a maximum 12-year follow-up. Surg Today 54, 186–194 (2024). https://doi.org/10.1007/s00595-023-02718-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-023-02718-5