Abstract
Purpose
To elucidate clinical outcomes using a digital drainage system (DDS) for massive air leakage (MAL) after pulmonary resection.
Methods
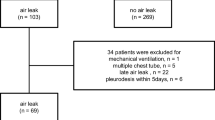
A total of 135 consecutive patients with pulmonary resection air leakage of > 100 ml/min on the DDS were evaluated retrospectively. In this study, MAL was defined as ≥ 1000 ml/min on the DDS. We analyzed the clinical characteristics and surgical outcomes of patients with MAL compared with non-MAL (101–999 ml/min). Using the DDS data, the duration of the air leak was plotted with the Kaplan‒Meier method and compared using the log-rank test.
Results
MAL was detected in 19 (14%) patients. The proportions of heavy smokers (P = 0.04) and patients with emphysematous lung (P = 0.03) and interstitial lung disease (P < 0.01) were higher in the MAL group than in the non-MAL group. The MAL group had a higher persistence rate of air leakage at 120 h after surgery than the non-MAL group (P < 0.01) and required significantly more frequent pleurodesis (P < 0.01). Drainage failure occurred in 2 (11%) and 5 (4%) patients from the MAL and non-MAL groups, respectively. Neither reoperation nor 30-day surgical mortality was observed in patients with MAL.
Conclusions
MAL was able to be treated conservatively without surgery using the DDS.


Similar content being viewed by others
References
Okereke L, Murthy SC, Alster JA, Blackstone EH, Rice TW. Characterization and importance of air leak after lobectomy. Ann Thorac Surg. 2005;79(4):1167–73.
Brunelli A, Xiume F, Al Refai M, Salati M, Marasco R, Sabbatini A. Air leaks after lobectomy increase the risk of empyema but not of cardiopulmonary complications—a case-matched analysis. Chest. 2006;130(4):1150–6.
DeCamp MM, Blackstone EH, Naunheim KS, Krasna MJ, Wood DE, Meli YM, et al. Patient and surgical factors influencing air leak after lung volume reduction surgery: Lessons learned from the National Emphysema Treatment Trial. Ann Thorac Surg. 2006;82(1):197–207.
Liang SY, Ivanovic J, Gilbert S, Maziak DE, Shamji FM, Sundaresan RS, et al. Quantifying the incidence and impact of postoperative prolonged alveolar air leak after pulmonary resection. J Thorac Cardiovasc Surg. 2013;145(4):948–54.
Attaar A, Luketich JD, Schuchert MJ, Winger DG, Sarkaria IS, Nason KS. Prolonged air leak after pulmonary resection increases risk of noncardiac complications, readmission, and delayed hospital discharge: a propensity score-adjusted analysis. Ann Surg. 2021;273:163–72.
Takamochi K, Imashimizu K, Fukui M, Maeyashiki T, Suzuki M, Ueda T, et al. Utility of objective chest tube management after pulmonary resection using a digital drainage system. Ann Thorac Surg. 2017;104(1):275–83.
Shintani Y, Funaki S, Ose N, Kawamura T, Kanzaki R, Minami M, et al. Air leak pattern shown by digital chest drainage system predict prolonged air leakage after pulmonary resection for patients with lung cancer. J Thorac Dis. 2018;10(6):3714–21.
Brunelli A, Salati M, Pompili C, Refai M, Sabbatini A. Regulated tailored suction vs regulated seal: a prospective randomized trial on air leak duration. Eur J Cardiothorac Surg. 2013;43(5):899–904.
Evans JM, Ray A, Dale M, Morgan H, Dimmock P, Carolan-Rees G. Thopaz+ portable digital system for managing chest drains: a NICE Medical Technology guidance. Appl Health Econ Health Policy. 2019;17(3):285–94.
Pompili C, Detterbeck F, Papagiannopoulos K, Sihoe A, Vachlas K, Maxfield MW, et al. Multicenter international randomized comparison of objective and subjective outcomes between electronic and traditional chest drainage systems. Ann Thorac Surg. 2014;98(2):490–6 (discussion 6–7).
Cerfolio RJ, Bryant AS. The benefits of continuous and digital air leak assessment after elective pulmonary resection: a prospective study. Ann Thorac Surg. 2008;86(2):396–401.
De Waele M, Agzarian J, Hanna WC, Schieman C, Finley CJ, Macri J, et al. Does the usage of digital chest drainage systems reduce pleural inflammation and volume of pleural effusion following oncologic pulmonary resection? A prospective randomized trial. J Thorac Dis. 2017;9(6):1598–606.
Cerfolio RJ, Bryant AS, Singh S, Bass CS, Bartolucci AA. The management of chest tubes in patients with a pneumothorax and an air leak after pulmonary resection. Chest. 2005;128(2):816–20.
Venuta F, Rendina EA, De Giacomo T, Coloni GF. Postoperative strategies to treat permanent air leaks. Thorac Surg Clin. 2010;20(3):391–7.
Yang Y, Gao P, Song Y, Sun J, Chen X, Zhao J, et al. The prognostic nutritional index is a predictive indicator of prognosis and postoperative complications in gastric cancer: a meta-analysis. EJSO. 2016;42(8):1176–82.
Goddard PR, Nicholson EM, Laszlo G, Watt I. Computed tomography in pulmonary emphysema. Clin Radiol. 1982;33:379–87.
Makita H, Nasuhara Y, Nagai K, Ito Y, Hasegawa M, Betsuyaku T, et al. Characterisation of phenotypes based on severity of emphysema in chronic obstructive pulmonary disease. Thorax. 2007;62(11):932–7.
Takamochi K, Oh S, Miyasaka Y, Matsunaga T, Kitamura Y, Fukui M, et al. Prospective randomized trial comparing buttressed versus nonbuttressed stapling in patients undergoing pulmonary lobectomy. Thorac Cardiovasc Surg. 2014;62(8):696–704.
Takamochi K, Nojiri S, Oh S, Matsunaga T, Imashimizu K, Fukui M, et al. Comparison of digital and traditional thoracic drainage systems for postoperative chest tube management after pulmonary resection: a prospective randomized trial. J Thorac Cardiovasc Surg. 2018;155(4):1834–40.
Kircher LT Jr, Swartzel RL. Spontaneous pneumothorax and its treatment. JAMA. 1954;155(1):24–9.
Chang PC, Chen KH, Jhou HJ, Lee CH, Chou SH, Chen PH, et al. Promising effects of digital chest tube drainage system for pulmonary resection: a systematic review and network meta-analysis. J Pers Med. 2022;12(4):512.
Cerfolio RJ, Bass C, Katholi CR. Prospective randomized trial compares suction versus water seal for air leaks. Ann Thorac Surg. 2001;71(5):1613–7.
Marshall MB, Deeb ME, Bleier JIS, Kucharczuk JC, Friedberg JS, Kaiser LR, et al. Suction vs water seal after pulmonary resection—a randomized prospective study. Chest. 2002;121(3):831–5.
Author information
Authors and Affiliations
Contributions
TU contributed to the design and coordination of the study, conducted research, prepared the manuscript, and read and approved the final version of the manuscript. KT and AH contributed to the design and coordination of the study, revised the manuscript for important intellectual content, and read and approved the final version. MF, TM, and KS contributed to the preparation of the manuscript and read and approved the final version.
Corresponding author
Ethics declarations
Conflict of interest
Ueda T. and other coauthors have no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ueda, T., Takamochi, K., Hattori, A. et al. Postoperative management using a digital drainage system for massive air leakage after pulmonary resection. Surg Today 54, 130–137 (2024). https://doi.org/10.1007/s00595-023-02703-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-023-02703-y