Abstract
Purpose
Video-assisted thoracoscopic surgery (VATS) has changed the surgical approach to non-small cell lung cancer (NSCLC) dramatically. The current study compares the outcomes of older and younger patients who underwent VATS lobectomy for NSCLC.
Methods
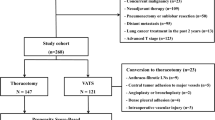
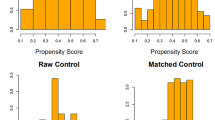
In total, 424 eligible patients with pathological stage I NSCLC underwent VATS lobectomy between 2007 and 2017. Patients were classified into two groups (< 75 and ≥ 75 years old), after which propensity score-matching was performed.
Results
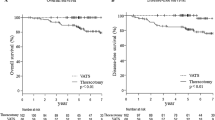
After matching, 143 patients were identified. No significant difference in postoperative complication rates was observed; however, the ≥ 75-year-old group had a longer postoperative hospital stay (p = 0.001). The 5-year overall survival, relapse-free survival, and lung cancer-specific survival rates of the < 75- and ≥ 75-year-old groups were 87.1% vs. 85.6% (p = 0.537), 82.1% vs. 79.0% (p = 0.531), and 93.5% vs. 92.7% (p = 0.832), respectively.
Conclusion
Despite the longer postoperative recovery following VATS lobectomy, the short- and long-term outcomes of older patients did not differ from those of younger patients. Thus, for early-stage NSCLC, older age alone was not a negative factor for lobectomy performed via minimally invasive surgery. Naturally, the systemic condition of this population must be evaluated carefully before surgery.


Similar content being viewed by others
Data Availability
The data underlying this article cannot be shared publicly due to the privacy of individuals that participated in the study.
Abbreviations
- CCI:
-
Charlson comorbidity index
- CI:
-
Confidence interval
- CT:
-
Computed tomography
- CSS:
-
Cancer-specific survival
- DLCO:
-
Diffusing capacity of the lung carbon monoxide
- FEV 1.0:
-
Forced expiratory volume in 1.0 s
- JATS:
-
Japanese Association for Thoracic Surgery
- NSCLC:
-
Non-small cell lung cancer
- OS:
-
Overall survival
- PS:
-
Performance status
- RFS:
-
Relapse-free survival
- TTE:
-
Transthoracic echocardiography
- VATS:
-
Video-assisted thoracoscopic surgery
References
Agostini P, Cieslik H, Rathinam S, Bishay E, Kalkat MS, Rajesh PB, et al. Postoperative pulmonary complications following thoracic surgery: are there any modifiable risk factors? Thorax. 2010;65:815–8.
Lee JY, Jin SM, Lee CH, Lee BJ, Kang CH, Yim JJ, et al. Risk factors of postoperative pneumonia after lung cancer surgery. J Korean Med Sci. 2011;26:979–84.
Berry MF, Hanna J, Tong BC, Burfeind WR, Harpole DH, D’Amico TA, et al. Risk factors for morbidity after lobectomy for lung cancer in elderly patients. Ann Thorac Surg. 2009;88:1093–9.
Flores RM, Park BJ, Dycoco J, Aronova A, Hirth Y, Rizk NP, et al. Lobectomy by video-assisted thoracic surgery (VATS) versus thoracotomy for lung cancer. J Thorac Cardiovasc Surg. 2009;138:11–8.
Cai YX, Fu XN, Xu QZ, Sun W, Zhang N. Thoracoscopic lobectomy versus open lobectomy in stage I non-small cell lung cancer: a meta-analysis. PLoS ONE. 2013;8: e82366.
Laursen LO, Petersen RH, Hansen HJ, Jensen TK, Ravn J, Konge L. Video-assisted thoracoscopic surgery lobectomy for lung cancer is associated with a lower 30-day morbidity compared with lobectomy by thoracotomy. Eur J Cardiothorac Surg. 2016;49:870–5.
Cattaneo SM, Park BJ, Wilton AS, Seshan VE, Bains MS, Downey RJ, et al. Use of video-assisted thoracic surgery for lobectomy in the elderly results in fewer complications. Ann Thorac Surg. 2008;85:231–5; discussion 235–6.
Pei G, Zhou S, Han Y, Liu Z, Xu S. Risk factors for postoperative complications after lung resection for non-small cell lung cancer in elderly patients at a single institution in China. J Thorac Dis. 2014;6:1230–8.
Colice GL, Shafazand S, Griffin JP, Keenan R, Bolliger CT. American College of Chest P. Physiologic evaluation of the patient with lung cancer being considered for resectional surgery: ACCP evidenced-based clinical practice guidelines (2nd edition). Chest. 2007;132:161S-77S.
UICC International Union Against Cancer. TNM Classification of Malignant Tumours: Lung and pleural tumors. 2009. http://www.inen.sld.pe/portal/documentos/pdf/educacion/13072015_TNM%20-Classification.pdf. Accessed 12 July 2022.
Eastern Cooperative Oncology Group. ECOG performance status. 1982. http://ecog-acrin.org/resources/ecog-performance-status. Accessed 12 July 2022.
Charlson ME, Pompei P, Ales KL, MacKenzie CR. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40:373–83.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240:205–13.
Kanda Y. Investigation of the freely available easy-to-use software ‘EZR’ for medical statistics. Bone Marrow Trans. 2013;48:452–8.
Cabinet Office Japan. Annual report on the Ageing Society. 2018. https://www8.cao.go.jp/kou-rei/english/annualreport/2018/pdf/c1-1.pdf. Accessed 12 July 2022.
Committee for Scientific Affairs TJAfTS, Shimizu H, Okada M, Toh Y, Doki Y, Endo S, et al. Thoracic and cardiovascular surgeries in Japan during 2018: annual report by the Japanese Association for Thoracic Surgery. Gen Thorac Cardiovasc Surg. 2021;69:179–212.
Ministry of Health, Labour and Welfare Government of Japan. Abridged life tables for Japan. 2018. https://www.mhlw.go.jp/english/database/db-hw/lifetb18/dl/lifetb18-01.pdf. Accessed 12 July 2022.
Kohn RR. Human aging and disease. J Chronic Dis. 1963;16:5–21.
De Leon LE, Rochefort MM, Bravo-Iniguez CE, Fox SW, Tarascio JN, Cardin K, et al. Opportunities for quality improvement in the morbidity pattern of older adults undergoing pulmonary lobectomy for cancer. J Geriatr Oncol. 2021;12:416–21.
Dell’Amore A, Monteverde M, Martucci N, Davoli F, Caroli G, Pipitone E, et al. Surgery for non-small cell lung cancer in younger patients: what are the differences? Heart Lung Circ. 2015;24:62–8.
Cerfolio RJ, Bryant AS. Survival and outcomes of pulmonary resection for non-small cell lung cancer in the elderly: a nested case-control study. Ann Thorac Surg. 2006;82:424–9; discussion 429–30.
Port JL, Kent M, Korst RJ, Lee PC, Levin MA, Flieder D, et al. Surgical resection for lung cancer in the octogenarian. Chest. 2004;126:733–8.
Brokx HA, Visser O, Postmus PE, Paul MA. Surgical treatment for octogenarians with lung cancer: results from a population-based series of 124 patients. J Thorac Oncol. 2007;2:1013–7.
Guerra M, Neves P, Miranda J. Surgical treatment of non-small-cell lung cancer in octogenarians. Interact Cardiovasc Thorac Surg. 2013;16:673–80.
Owonikoko TK, Ragin CC, Belani CP, Oton AB, Gooding WE, Taioli E, et al. Lung cancer in elderly patients: an analysis of the surveillance, epidemiology, and end results database. J Clin Oncol. 2007;25:5570–7.
Higton AM, Monach J, Congleton J. Investigation and management of lung cancer in older adults. Lung Cancer. 2010;69:209–12.
Presley CJ, Reynolds CH, Langer CJ. Caring for the older population with advanced lung cancer. Am Soc Clin Oncol Educ Book. 2017;37:587–96.
Nosaki K, Saka H, Hosomi Y, Baas P, de Castro G, Reck M, et al. Safety and efficacy of pembrolizumab monotherapy in elderly patients with PD-L1-positive advanced non-small-cell lung cancer: Pooled analysis from the KEYNOTE-010, KEYNOTE-024, and KEYNOTE-042 studies. Lung Cancer. 2019;135:188–95.
Hesketh PJ, Lilenbaum RC, Chansky K, Dowlati A, Graham P, Chapman RA, et al. Chemotherapy in patients > or = 80 with advanced non-small cell lung cancer: combined results from SWOG 0027 and LUN 6. J Thorac Oncol. 2007;2:494–8.
Maemondo M, Minegishi Y, Inoue A, Kobayashi K, Harada M, Okinaga S, et al. First-line gefitinib in patients aged 75 or older with advanced non-small cell lung cancer harboring epidermal growth factor receptor mutations: NEJ 003 study. J Thorac Oncol. 2012;7:1417–22.
Goto K, Nishio M, Yamamoto N, Chikamori K, Hida T, Maemondo M, et al. A prospective, phase II, open-label study (JO22903) of first-line erlotinib in Japanese patients with epidermal growth factor receptor (EGFR) mutation-positive advanced non-small-cell lung cancer (NSCLC). Lung Cancer. 2013;82:109–14.
Acknowledgements
We acknowledge the members of the Thoracic Surgery Department at Shimane University Hospital for their assistance with the preparation of this manuscript.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
We have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Fujita, T., Koyanagi, A. & Kishimoto, K. Older age is not a negative factor for video-assisted thoracoscopic lobectomy for pathological stage I non-small cell lung cancer: a single-center, retrospective, propensity score-matching study. Surg Today 53, 824–833 (2023). https://doi.org/10.1007/s00595-022-02628-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-022-02628-y