Abstract
Purpose
To investigate the efficacy and safety of Daikenchuto (DKT) for colorectal cancer patients undergoing surgery with the potential risk of postoperative ileus (POI).
Methods
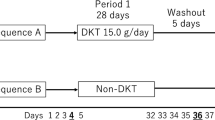
Colorectal cancer patients with abdominal pain and distention, scheduled for surgery, were randomly assigned to a DKT group or a control group. Patients assigned to the DKT group were given 15 g of DKT per day during the perioperative period. We then compared the perioperative gastrointestinal symptoms between the two groups.
Results
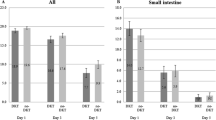
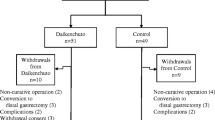
The aim for a sample size of 30 patients per group was not reached in time, so we conducted an analysis on 16 patients in each group. The visual Analogue Scale scores for abdominal pain and distention were similar in the two groups. The number of bowel movements per day on postoperative days (PODs) 1, 2, and 6 were significantly lower in the DKT group. The incidence of a sensation of incomplete bowel evacuation on PODs 3 and 28 was also significantly lower in the DKT group. There were no adverse events thought to be related to DKT.
Conclusions
DKT could potentially inhibit diarrhea and reduce the number of bowel movements per day and the sensation of incomplete bowel evacuation after colorectal surgery. Thus, the perioperative use of DKT may be safe for colorectal cancer patients with abdominal pain and distention, who undergo surgery.



Similar content being viewed by others
References
Spanjersberg WR, van Sambeeck JD, Bremers A, Rosman C, van Laarhoven CJ. Systematic review and meta-analysis for laparoscopic versus open colon surgery with or without an ERAS programme. Surg Endosc. 2015;29:3443–53.
Lassen K, Soop M, Nygren J, Cox PB, Hendry PO, Spies C, et al. consensus review of optimal perioperative care in colorectal surgery: Enhanced Recovery After Surgery (ERAS) Group Recommendations. Arch Surg. 2009;144:961–9.
Vather R, Trivedi S, Bissett I. Defining postoperative ileus: results of a systematic review and global survey. J Gastrointest Surg. 2013;17:962–72.
Vather R, Bissett I. Management of prolonged post-operative ileus: evidence-based recommendations. ANZ J Surg. 2013;83:319–24.
Endo S, Nishida T, Nishikawa K, Nakajima K, Hasegawa J, Kitagawa T, et al. Dai-kenchu-to, a Chinese herbal medicine, improves stasis of patients with total gastrectomy and jejunal pouch interposition. Am J Surg. 2006;192:9–13.
Hayakawa T, Kase Y, Saito K, Hashimoto K, Ishige A, Komatsu Y, et al. Effects of Dai-kenchu-to on intestinal obstruction following laparotomy. J Smooth Muscle Res. 1999;35:47–544.
Hayakawa T, Kase Y, Saito K, Hashimoto K, Ishige A, Komatsu Y, et al. Pharmacological studies of the effect of Daikenchuto on spontaneous contraction of isolated rabbit jejunum. J Smooth Muscle Res. 1999;35:55–62.
Kono T, Shimada M, Nishi M, Maeda K, Koeda K, Morita S, et al. Daikenchuto accelerates the recovery from prolonged postoperative ileus after open abdominal surgery: a subgroup analysis of three randomized controlled trials. Surg Today. 2019;49:704–11.
Yaegashi M, Otsuka K, Itabashi T, Kimura T, Kato K, Fujii H, et al. Daikenchuto stimulates colonic motility after laparoscopic-assisted colectomy. Hepatogastroenterology. 2014;61:85–9.
Svedlund J, Sjödin I, Dotevall G. GSRS—a clinical rating scale for gastrointestinal symptoms in patients with irritable bowel syndrome and peptic ulcer disease. Dig Dis Sci. 1988;33:129–34.
Revicki DA, Wood M, Wiklund I, Crawley J. Reliability and validity of the Gastrointestinal Symptom Rating Scale in patients with gastroesophageal reflux disease. Qual Life Res. 1998;7:75–83.
Kubo N, Uchida Y, Akiyoshi T, Miyahara M, Shibata O, Takeyama M, et al. Effect of Dai-kenchu-to for ileus (in Japanese). Prog Med. 1995;15:1962–7.
Katsuno H, Maeda K, Kaiho T, Kunieda K, Funahashi K, Sakamoto J, et al. Clinical efficacy of Daikenchuto for gastrointestinal dysfunction following colon surgery: a randomized, double-blind, multicenter, placebo-controlled study (JFMC39-0902). Jpn J Clin Oncol. 2015;45:650–6.
Lewis SJ, Heaton KW. Stool form scale as a useful guide to intestinal transit time. Scand J Gastroenterol. 1997;32:920–4.
Abe T, Kunimoto M, Hachiro Y, Ohara K, Murakami M. Clinical efficacy of Japanese herbal medicine Daikenchuto in the management of fecal incontinence: a single-center, observational study. J Anus Rectum Colon. 2019;3:160–6.
Yoshikawa K, Shimada M, Nishioka M, Kurita N, Iwata T, Morimoto S, et al. The effects of the Kampo medicine (Japanese herbal medicine) “Daikenchuto” on the surgical inflammatory response following laparoscopic colorectal resection. Surg Today. 2012;42:646–51.
Yamada T, Matsumoto S, Matsuda MKA, Shinji S, Yokoyama Y, Takahashi G, et al. The effect of Daikenchuto on postoperative intestinal motility in patients with right-side colon cancer. Surg Today. 2017;47:865–71.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors (MW, YS, MT, SU, HA, TN) have no potential conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Wakasugi, M., Suzuki, Y., Tei, M. et al. Effects of Daikenchuto on postoperative gastrointestinal motility in colorectal carcinoma patients with abdominal pain and distension: a prospective, randomized trial. Surg Today 50, 1524–1529 (2020). https://doi.org/10.1007/s00595-020-02052-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-020-02052-0