Abstract
Purpose
Anatomical variation of the cystic duct (CD) is rare but can result in misunderstanding of the CD anatomy during laparoscopic cholecystectomy, potentially leading to bile duct injury. Therefore, the precise preoperative identification of CD variation is important. However, preoperative imaging analyses of the biliary system are not always possible or sufficient. We therefore investigated CD variations based on the anatomy of the hepatic vasculature.
Methods
This study enrolled 480 patients who underwent imaging before hepatobiliary pancreatic surgery. We assessed the variation of the CD and hepatic vasculature and evaluated the correlations among these variations.
Results
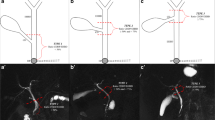
A variant CD anatomy was identified in 12 cases (2.5%) as CD draining into the right hepatic bile duct (BD) in 4 cases and into the right posterior BD in 8 cases. CD variation was significantly more common in cases with portal vein (PV) and BD variation than in those without the variation. We developed a scoring system based on the presence of PV and BD variations that showed good discriminatory power for identification of CD variants.
Conclusion
Cases with a variant CD anatomy were more likely to exhibit variant PV and BD anatomies than cases with a normal CD anatomy. These findings will be useful for the preoperative identification of CD variants.



Similar content being viewed by others
References
National institutes of health consensus development conference statement on gallstones and laparoscopic cholecystectomy. Am J Surg. 1993;165(4):390–398.
Soper NJ, Stockmann PT, Dunnegan DL, Ashley SW. Laparoscopic cholecystectomy. The new 'gold standard'? Arch Surg. 1992;127(8):917–21 (Discussion 921–913).
Dubois F, Berthelot G, Levard H. Laparoscopic cholecystectomy: historic perspective and personal experience. Surg Laparosc Endosc. 1991;1(1):52–7.
Strasberg SM, Hertl M, Soper NJ. An analysis of the problem of biliary injury during laparoscopic cholecystectomy. J Am Coll Surg. 1995;180(1):101–25.
Davidoff AM, Pappas TN, Murray EA, Hilleren DJ, Johnson RD, Baker ME, et al. Mechanisms of major biliary injury during laparoscopic cholecystectomy. Ann Surg. 1992;215(3):196–202.
14th Nationwide Survey of Endoscopic Surgery in Japan. J Jpn Soc Endosc Surg. 2018;23(6):730–890.
Flum DR, Cheadle A, Prela C, Dellinger EP, Chan L. Bile duct injury during cholecystectomy and survival in medicare beneficiaries. JAMA. 2003;290(16):2168–73.
Gouma DJ, Go PM. Bile duct injury during laparoscopic and conventional cholecystectomy. J Am Coll Surg. 1994;178(3):229–33.
Hashimoto M, Ishikawa T, Iizuka T, Matsuda M, Watanabe G. Right hepatic duct emptying into the cystic duct: report of a case. Surg Endosc. 2002;16(2):359.
Kurata M, Honda G, Okuda Y, Kobayashi S, Sakamoto K, Iwasaki S, et al. Preoperative detection and handling of aberrant right posterior sectoral hepatic duct during laparoscopic cholecystectomy. J Hepatobiliary Pancreat Sci. 2015;22(7):558–62.
Hugh TB. New strategies to prevent laparoscopic bile duct injury–surgeons can learn from pilots. Surgery. 2002;132(5):826–35.
Seibert D, Matulis SR, Griswold F. A rare right hepatic duct anatomical variant discovered after laparoscopic bile duct transection. Surg Laparosc Endosc. 1996;6(1):61–4.
Chung YH, Kim DJ, Kim IG, Kim HJ, Chon SE, Jeon JY, et al. Relationship between the risk of bile duct injury during laparoscopic cholecystectomy and the types of preoperative magnetic resonance cholangiopancreatiocography (MRCP). Korean J Hepato Biliary Pancreatic Surg. 2012;16(1):17–23.
Schnelldorfer T, Sarr MG, Adams DB. What is the duct of Luschka? A systematic review. J Gastrointest Surg. 2012;16(3):656–62.
Viste A, Horn A, Ovrebo K, Christensen B, Angelsen JH, Hoem D. Bile duct injuries following laparoscopic cholecystectomy. Scand J Surg. 2015;104(4):233–7.
Kitami M, Takase K, Murakami G, Ko S, Tsuboi M, Saito H, et al. Types and frequencies of biliary tract variations associated with a major portal venous anomaly: analysis with multi-detector row CT cholangiography. Radiology. 2006;238(1):156–66.
Takeishi K, Shirabe K, Yoshida Y, Tsutsui Y, Kurihara T, Kimura K, et al. Correlation between portal vein anatomy and bile duct variation in 407 living liver donors. Am J Transpl. 2015;15(1):155–60.
Hanley JA, McNeil BJ. The meaning and use of the area under a receiver operating characteristic (ROC) curve. Radiology. 1982;143(1):29–36.
Harrell FE Jr, Lee KL, Mark DB. Multivariable prognostic models: issues in developing models, evaluating assumptions and adequacy, and measuring and reducing errors. Stat Med. 1996;15(4):361–87.
Cheng YF, Huang TL, Chen CL, Sheen-Chen SM, Lui CC, Chen TY, et al. Anatomic dissociation between the intrahepatic bile duct and portal vein: risk factors for left hepatectomy. World J Surg. 1997;21(3):297–300.
Kishi Y, Imamura H, Sugawara Y, Sano K, Kaneko J, Kokudo N, et al. Evaluation of donor vasculobiliary anatomic variations in liver graft procurements. Surgery. 2010;147(1):30–9.
Lee VS, Morgan GR, Lin JC, Nazzaro CA, Chang JS, Teperman LW, et al. Liver transplant donor candidates: associations between vascular and biliary anatomic variants. Liver Transpl. 2004;10(8):1049–54.
Varotti G, Gondolesi GE, Goldman J, Wayne M, Florman SS, Schwartz ME, et al. Anatomic variations in right liver living donors. J Am Coll Surg. 2004;198(4):577–82.
Hirano Y, Tatsuzawa Y, Shimizu J, Kinoshita S, Kawaura Y, Takahashi S. Efficacy of multi-slice computed tomography cholangiography before laparoscopic cholecystectomy. ANZ J Surg. 2006;76(8):693–5.
Mutlu H, Basekim CC, Silit E, Pekkafali Z, Erenoglu C, Kantarci M, et al. Value of contrast-enhanced magnetic resonance cholangiography in patients undergoing laparoscopic cholecystectomy. Surg Laparosc Endosc Percutan Tech. 2005;15(4):195–8 (Discussion 198–201).
Ikeda T, Yonemura Y, Ueda N, Kabashima A, Mashino K, Yamashita K, et al. Intraoperative cholangiography using an endoscopic nasobiliary tube during a laparoscopic cholecystectomy. Surg Today. 2011;41(5):667–73.
Yin P, Wang M, Qin R, Zhang J, Xiao G, Yu H, et al. Intraoperative endoscopic nasobiliary drainage over primary closure of the common bile duct for choledocholithiasis combined with cholecystolithiasis: a cohort study of 211 cases. Surg Endosc. 2017;31(8):3219–26.
Boogerd LSF, Handgraaf HJM, Huurman VAL, Lam HD, Mieog JSD, van der Made WJ, et al. The best approach for laparoscopic fluorescence cholangiography: overview of the literature and optimization of dose and dosing time. Surg Innov. 2017;24(4):386–96.
Vlek SL, van Dam DA, Rubinstein SM, de Lange-de Klerk ESM, Schoonmade LJ, Tuynman JB, et al. Biliary tract visualization using near-infrared imaging with indocyanine green during laparoscopic cholecystectomy: results of a systematic review. Surg Endosc. 2017;31(7):2731–42.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Yoshito Tomimaru and the other co-authors have no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Fujimoto, N., Tomimaru, Y., Yamamoto, T. et al. Clinical investigation of the cystic duct variation based on the anatomy of the hepatic vasculature. Surg Today 50, 396–401 (2020). https://doi.org/10.1007/s00595-019-01904-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-019-01904-8