Abstract
Purpose
The pulmonary artery (PA) in patients with pulmonary hypertension (PH) becomes dilated. We analyzed the postoperative changes of the main PA after lung transplantation (LuTx).
Methods
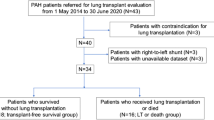
The subjects of this retrospective study were 68 LuTx recipients, divided into a PH group (n = 36) and a non-PH group (n = 32), based on preoperative right heart catheterization findings. The PA diameter was measured on chest computed tomography. We evaluated the correlation between the mean pulmonary arterial pressure (mPAP) and the main PA diameter and compared the main PA diameters before and 3 months after LuTx.
Results
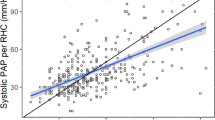
The main PA diameter was significantly correlated with the mPAP (r = 0.423, P < 0.001). Preoperatively, the mean main PA diameter in the PH group was significantly greater than that in the non-PH group. However, by 3 months after LuTx, the main PA diameter in the PH group had decreased significantly from 32.4 ± 6.7 to 26.9 ± 4.8 mm (P < 0.001), while that in the non-PH group had decreased minimally from 28.3 ± 4.9 to 26.4 ± 4.6 mm (P < 0.001), resulting in no significant difference in postoperative main PA diameters between the two groups.
Conclusions
The main PA diameter in recipients with PH was enlarged and correlated with the mPAP. The dilated main PA diameter in PH patients decreased shortly after LuTx.






Similar content being viewed by others
Abbreviations
- DDLT:
-
Deceased donor lung transplantations
- COPD:
-
Chronic obstructive pulmonary disease
- CT:
-
Computed tomography
- IPAH:
-
Idiopathic pulmonary arterial hypertension
- LDLLT:
-
Living donor lobar lung transplantations
- LuTx:
-
Lung transplantation
- mPAP:
-
Mean pulmonary arterial pressure
- PA:
-
Pulmonary artery
- PH:
-
Pulmonary hypertension
- PA/Ao ratio:
-
Ratio of PA to ascending aorta
- RHC:
-
Right heart catheterization
- ROC:
-
Receiver-operating characteristic
- AUC:
-
Area under the ROC curve
- 95% CI:
-
95% Confidence interval
References
Yusen RD, Edwards LB, Kucheryavaya AY, Benden C, Dipchand AI, Goldfarb SB, et al. The registry of the International Society for Heart Lung Transplantation: thirty-second official adult lung and heart-lung transplantation report—2015; focus theme: early graft failure. J Heart Lung Transpl. 2015;34:1264–77.
Iyer AS, Wells JM, Vishin S, Bhatt SP, Wille KM, Dransfield MT. CT scan-measured pulmonary artery to aorta ratio and echocardiography for detecting pulmonary hypertension in severe COPD. Chest. 2014;145:824–32.
Terpenning S, Deng M, Hong-Zohlman SN, Lin CT, Klingerman SJ, Jeudy J, et al. CT measurement of central pulmonary arteries to diagnose pulmonary hypertension (PHTN): more reliable than valid? Clin Imaging. 2016;40:821–7.
Chen X, Liu K, Wang Z, Zhu Y, Zhao Y, Kong H, et al. Computed tomography measurement of pulmonary artery for diagnosis of COPD and its comorbidity pulmonary hypertension. Int J COPD. 2015;10:2525–33.
McCall RK, Ravenel JG, Nietert PJ, Granath A, Silver RM. Relationship of main pulmonary artery diameter to pulmonary arterial pressure in scleroderma patients with and without interstitial fibrosis. J Comput Assist Tomogr. 2014;38:163–8.
Ando K, Kuraishi H, Nagaoka T, Tsutsumi T, Hoshika Y, Kimura T, et al. Potential role of CT metrics in chronic obstructive pulmonary disease with pulmonary hypertension. Lung. 2015;193:911–8.
Shin S, King CS, Brown AW, Albano MC, Atkins M, Sheridan MJ, et al. Pulmonary artery size as a predictor of pulmonary hypertension and outcomes in patients with chronic obstructive pulmonary disease. Respir Med. 2014;108:1626–32.
Pérez-Enguix D, Morales P, Tomás JM, Vera F, Lloret RM. Computed tomographic screening of pulmonary arterial hypertension in candidates for lung transplantation. Transpl Proc. 2007;39:2405–8.
Force SD, Lau CL, Moazami N, Trulock EP, Patterson GA. Bilateral lung transplantation and pulmonary artery reconstruction in a patient with chronic obstructive pulmonary disease and a giant pulmonary artery aneurysm. J Thorac Cardiovasc Surg. 2003;126:864–6.
Shayan H, Sareyyupoglu B, Shigemura N, Thacker J, Bermudez C, Toyoda Y. Lung transplant, double valve repair, and pulmonary artery aneurysm resection. Ann Thorac Surg. 2012;93:e3–5.
Yokoyama Y, Chen F, Minakata K, Yamada T, Aoyama A, Sato M, et al. Living-donor lobar lung transplantation for treatment of idiopathic pulmonary arterial hypertension with severe pulmonary arterial dilation. Ann Thorac Surg. 2014;97:e149.
Wells JM, Washko GR, Han MK, Abbas N, Nath H, Mamary AJ, et al. Pulmonary arterial enlargement and acute exacerbations of COPD. N Engl J Med. 2012;367:913–21.
Żyłkowska J, Kurzyna M, Florczyk M, Burakowska B, Grzegorczyk F, Burakowski J, et al. Pulmonary artery dilatation correlates with the risk of unexpected death in chronic arterial or thromboembolic pulmonary hypertension. Chest. 2012;142:1406–16.
Schölzel BE, Post MC, van de Bruaene A, Dymarkowski S, Wuyts W, Meyns B, et al. Prediction of hemodynamic improvement after pulmonary endarterectomy in chronic thromboembolic pulmonary hypertension using non-invasive imaging. Int J Cardiovasc Imaging. 2015;31:143–50.
Kanda Y. Investigation of the freely available easy-to-use software ‘EZR’ for medical statistics. Bone Marrow Transpl. 2013;48:452–8.
Aoyama A, Chen F, Minakata K, Yamazaki K, Yamada T, Sato M, et al. Sparing native upper lobes in living-donor lobar lung transplantation: five cases from a single center. Am J Transpl. 2015;15:3202–7.
Kayawake H, Chen-Yoshikawa TF, Motoyama H, Hamaji M, Hijiya K, Aoyama A, et al. Inverted lobes have satisfactory functions compared with noninverted lobes in lung transplantation. Ann Thorac Surg. 2018;105:1044–9.
Kayawake H, Chen-Yoshikawa TF, Aoyama A, Motoyama H, Hamaji M, Hijiya K, et al. Surgical management of bronchial stumps in lobar lung transplantation. J Thorac Cardiovasc Surg. 2018;156:451–60.
Hoesein FAM, Besselink T, Pompe E, Oudijk EJ, de Graaf EA, Kwakkel-van Erp JM, et al. Accuracy of CT pulmonary artery diameter for pulmonary hypertension in end-stage COPD. Lung. 2016;194:813–9.
Lee SE, Im JH, Sung JM, Cho IJ, Shim CY, Hong GR, et al. Detection of mechanical complications related to the potential risk of sudden cardiac death in patients with pulmonary arterial hypertension by computed tomography. Int J Cardiol. 2017;243:460–5.
Date H, Aoyama A, Hijiya K, Motoyama H, Handa T, Kinoshita H, et al. Outcomes of various transplant procedures (single, sparing, inverted) in living-donor lobar lung transplantation. J Thorac Cardiovasc Surg. 2017;153:479–86.
Miyoshi R, Chen-Yoshikawa TF, Hijiya K, Motoyama H, Aoyama A, Menju T, et al. Significance of single lung transplantation in the current situation of severe donor shortage in Japan. Gen Thorac Cardiovasc Surg. 2016;64:93–7.
Kayawake H, Chen-Yoshikawa TF, Motoyama H, Hamaji M, Nakajima D, Aoyama A, et al. Gastrointestinal complications after lung transplantation in Japanese patients. Surg Today. 2018;48:883–90.
Sugimoto S, Yamane M, Otani S, Kurosaki T, Okahara S, Hikasa Y, et al. Airway complications have a greater impact on the outcomes of living-donor lobar lung transplantation recipients than cadaveric lung transplantation recipients. Surg Today. 2018;48:848–55.
Oishi H, Watanabe T, Matsuda Y, Noda M, Ejima Y, Saiki Y, et al. Single lung transplantation for lymphangioleiomyomatosis: a single-center experience in Japan. Surg Today. 2018;48:944–50.
Funding
No funding was provided.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
No potential conflicts exist.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Kayawake, H., Aoyama, A., Kinoshita, H. et al. Diameter of the dilated main pulmonary artery in patients with pulmonary hypertension decreases after lung transplantation. Surg Today 50, 275–283 (2020). https://doi.org/10.1007/s00595-019-01887-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-019-01887-6