Abstract
Purpose
Splenic infarction may occur if the splenic branches are injured or ligated accidentally during gastrectomy. We used three-dimensional computed tomography (3D-CT) imaging to distinguish the vascular anatomy of the splenic hilum in individual patients, focusing on the splenic polar branches and the gastric branches.
Methods
The subjects of this study were 104 patients who underwent computed tomography (CT) with intravenous contrast before gastrectomy. SYNAPSE 3D® (Fujifilm Medical, Tokyo, Japan) was used to generate the 3D-CT images. The total spleen volume and the area supplied by the superior polar artery (SPA) in each patient were estimated using the “liver analysis” function.
Results
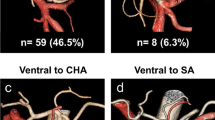
The SPA without the gastric branch (supplying only the spleen), the SPA with the gastric branch (supplying both the stomach and the spleen), and the posterior gastric artery (supplying only the stomach) were present in 14, 45, and 18% of the patients, respectively. The SPA supplied 12% of the total spleen volume on average; however, it supplied over 30% in two patients.
Conclusion
We identified the vascular anatomy around the splenic hilum in over 100 patients. Based on our findings, we recommend preservation of the SPA when it is supplying a large area of the spleen. Preoperative 3D-CT analysis provides useful information to optimize safe gastrectomy.






Similar content being viewed by others
References
Sano T, Sasako M, Mizusawa J, Yamamoto S, Katai H, Yoshikawa T, et al. Randomized controlled trial to evaluate splenectomy in total gastrectomy for proximal gastric carcinoma. Ann Surg. 2017;265:277–83.
Jaroch MT, Broughan TA, Hermann RE. The natural history of splenic infarction. Surgery. 1986;100:743–50.
Nores M, Phillips EH, Morgenstern L, Hiatt JR. The clinical spectrum of splenic infarction. Am Surg. 1998;64:182–8.
Watanabe M, Miyata H, Gotoh M, Baba H, Kimura W, Tomita N, et al. Total gastrectomy risk model: data from 20,011 Japanese patients in a nationwide internet-based database. Ann Surg. 2014;260:1034–9.
Kunisaki C, Miyata H, Konno H, Saze Z, Hirahara N, Kikuchi H, et al. Modeling preoperative risk factors for potentially lethal morbidities using a nationwide Japanese web-based database of patients undergoing distal gastrectomy for gastric cancer. Gastric Cancer. 2017;20:496–507.
Akin K, Kosehan D, Cengiz AY, Dener NC, Koktener A, Inan A, et al. Splenic infarction following conventional open gastrectomy in patients with gastric malignancy: a CT-based study. Abdom Imaging. 2012;37:609–15.
Jung YJ, Seo HS, Lee HH, Kim JH, Song KY, Choi MH, et al. Splenic infarction as a delayed febrile complication following radical gastrectomy for gastric cancer patients: computed tomography-based analysis. World J Surg. 2017. https://doi.org/10.1007/s00268-017-4401-0. [Epub ahead of print].
Lee CM, Leung TK, Wang HJ, Lee WH, Shen LK, Liu JD, et al. Evaluation of the effect of partial splenic embolization on platelet values for liver cirrhosis patients with thrombocytopenia. World J Gastroenterol. 2007;13619–22.
Hayashi H, Beppu T, Okabe K, Masuda T, Okabe H, Baba H. Risk factors for complications after partial splenic embolization for liver cirrhosis. Br J Surg. 2008;95:744–50.
Cai M, Huang W, Lin C, Li Z, Qian J, Huang M, et al. Partial splenic embolization for thrombocytopenia in liver cirrhosis: predictive factors for platelet increment and risk factors for major complications. Eur Radiol. 2016;26:370–80.
Liu DL, Xia S, Xu W, Ye Q, Gao Y, Qian J. Anatomy of vasculature of 850 spleen specimens and its application in partial splenectomy. Surgery. 1996;119:27–33.
Sow ML, Dia A, Ouedraogo T. Anatomic basis for conservative surgery of the spleen. Surg Radiol Anat. 1991;13:81–7.
Redmond HP, Redmond JM, Rooney BP, Duignan JP, Bouchier-Hayes DJ. Surgical anatomy of the human spleen. Br J Surg. 1989;76:198–201.
Zeon SK, Kim SG, Huyn JA, Kim YS. Angiographic branching patterns of the splenic artery. Int J Angiol. 1998;7:57–61.
Japanese Gastric Cancer Association. Japanese classification of gastric carcinoma: 3rd English edition. Gastric Cancer. 2011;14:101–12.
Suzuki K, Prates JC, DiDio LJ. Incidence and surgical importance of the posterior gastric artery. Ann Surg. 1978;187:134–6.
Okabayashi T, Kobayashi M, Morishita S, Sugimoto T, Akimori T, Namikawa T, et al. Confirmation of the posterior gastric artery using multi-detector row computed tomography. Gastric Cancer. 2005;8:209 – 13.
Yu W, Whang I. Surgical implications of the posterior gastric artery. Am J Surg. 1990;159:420–22.
Trubel W, Rokitansky A, Turkof E, Firbas W. Correlations between posterior gastric artery and superior polar artery in human anatomy. Anat Anz. 1988;167:219–23.
Kinoshita T, Shibasaki H, Enomoto N, Sahara Y, Sunagawa H, Nishida T. Laparoscopic splenic hilar lymph node dissection for proximal gastric cancer using integrated three-dimensional anatomic simulation software. Surg Endosc. 2016;30:2613–9.
Zheng CH, Xu M, Huang CM, Li P, Xie JW, Wang JB, et al. Anatomy and influence of the splenic artery in laparoscopic spleen-preserving splenic lymphadenectomy. World J Gastroenterol. 2015;21:8389–97.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
We declare no conflicts of interest.
Ethical approval
All the study procedures were approved by the Ethical Committee of Saitama Cancer Center (approval number 767) and were therefore performed in accordance with the ethical standards laid down in the 1964 Declaration of Helsinki and its later amendments.
Informed consent
Informed consent was obtained from all participants included in the study.
Rights and permissions
About this article
Cite this article
Ishikawa, Y., Ehara, K., Yamada, T. et al. Three-dimensional computed tomography analysis of the vascular anatomy of the splenic hilum for gastric cancer surgery. Surg Today 48, 841–847 (2018). https://doi.org/10.1007/s00595-018-1679-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-018-1679-y