Abstract
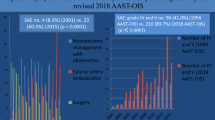
Non-operative management (NOM) of hemodynamically stable patients with blunt splenic injury (BSI) is the standard of care, although it is associated with a potential risk of failure. Hemodynamically unstable patients should always undergo immediate surgery and avoid unnecessary CT scans. Angioembolization might help to increase the NOM rates, as well as NOM success rates. The aim of this study was to review and critically analyze the data from BSI cases managed at the Maggiore Hospital Trauma Center during the past 5 years, with a focus on NOM, its success rates and outcomes. A further aim was to develop a proposed clinical practical algorithm for the management of BSI derived from Clinical Audit experience. During the period between January 1, 2009 and December 31, 2013 we managed 293 patients with splenic lesions at the Trauma Center of Maggiore Hospital of Bologna. The data analyzed included the demographics, clinical parameters and characteristics, diagnostic and therapeutic data, as well as the outcomes and follow-up data. A retrospective evaluation of the clinical outcomes through a clinical audit has been used to design a practical clinical algorithm. During the five-year period, 293 patients with BSI were admitted, 77 of whom underwent immediate surgical management. The majority (216) of the patients was initially managed non-operatively and 207 of these patients experienced a successful NOM, with an overall rate of successful NOM of 70 % among all BSI cases. The success rate of NOM was 95.8 % in this series. All patients presenting with stable hemodynamics underwent an immediate CT-scan; angiography with embolization was performed in 54 cases for active contrast extravasation or in cases with grade V lesions even in absence of active bleeding. Proximal embolization was preferentially used for high-grade injuries. After a critical review of the cases treated during the past 5 years during a monthly clinical audit meeting, a clinical algorithm has been developed with the aim of standardizing the clinical management of BSI by a multidisciplinary team to include every patient within the correct diagnostic and therapeutic pathway, in order to improve the outcomes by potentially decreasing the NOM failure rates and to optimize the utilization of resources.

Similar content being viewed by others
References
Peitzman AB, Ferrada P, Puyana JC. Nonoperative management of blunt trauma: have we gone too far? Surg Infect. 2009;10(5):427–33.
Eastern Association for the Surgery of Trauma Practice Management Guidelines Work Group. Practice management guidelines for the nonoperative management of blunt injury to the liver and spleen. East Assoc Surg Trauma. 2001
Fata P, Robinson L, Fahkry M. A survey of EAST member practice in blunt splenic injury: a descrption of current trends and opportunities for improvement. J Trauma. 2005;59(4):836–42.
Hurtuk M, Lawrence R, Esposito TJ, Kimberly AD, Luchette FA. Trauma surgeon practice what they preach: the NTDB story on solid organ injury management. J Trauma. 2006;61(2):243–55.
Weinberg JA, Magnotti LJ, Croce MA, Edwards NM. The utility of serial computed tomography imaging of blunt splenic injury: still worth a second look? J Trauma. 2007;62:1143–8.
Harbrecht BG, Sae HK, Watson GA, Forsythe RM, Rosengart MR, Peitzman AB. Angiography for blunt splenic trauma does not improve the success rate of nonoperative management. J Trauma. 2007;63:44–9.
Fata P, Robinson L, Fahkry M. EAST member practices in blunt splenic injury: inpatient e post-discharge care. J Trauma. 2004;57(6):1382.
Stassen NA, Bhullar I, Cheng JD, Crandall ML, Friese RS, et al. Selective nonoperative management of blunt splenic injury: An Eastern Association for the Surgery of Trauma practice management guideline. J Trauma Acute Care Surg. 2012;73(5):294–300.
Todd SR, Arthur M, Newgard C, Hedges JR, Mullins RJ. Hospital factors associated with splenectomy for splenic injury: a national perspective. J Trauma. 2004;57:1065–71.
Harbrecht BG, Zenati MS, Alarcon LH, Ochoa JB, Puyana JC, Schuschert VD, Peitzman AB. Is outcome after blunt splenic injury in adults better in high-volume trauma centers? Am Surg. 2005;71(11):942–8.
Banerjee A, Duane TM, Wilson SP, Haney S, O’Neill PJ, Evans HL, Como JJ, Claridge JA. Trauma center variation in splenic artery embolization and spleen salvage: a multicenter analysis. J Trauma Acute Care Surg. 2013;75(1):69–74.
Bhullar IS, Frykberg ER, Tepas JJ 3rd, Siragusa D, Loper T, Kerwin AJ. At first blush: absence of computed tomography contrast extravasation in Grade IV or V adult blunt splenic trauma should not preclude angioembolization. J Trauma Acute Care Surg. 2013;74(1):105–11.
Miller PR, Chang MC, Hoth JJ, Mowery NT, Hildreth AN, Martin RS, Holmes JH, Meredith JW, Requarth JA. Prospective trial of angiography and embolization for all grade III to V blunt splenic injuries: nonoperative management success rate is significantly improved. J Am Coll Surg. 2014;218(4):644–8.
Cirocchi R, Boselli C, Corsi A, Farinella E, Listorti C, Trastulli S, Renzi C, Desiderio J, Santoro A, Cagini L, Parisi A, Redler A, Noya G, Fingerhut A. Is non-operative management safe and effective for all splenic blunt trauma? A systematic review. Crit Care. 2013;17(5):R185.
Tugnoli G, Casali M, Villani S, Biscardi A, Baldoni F. The treatment of splenic injuries: from splenectomy to nonoperative management. Our experience on 429 cases. Ann Ital Chir. 2003;1:37–42.
Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP, STROBE Initiative. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. BMJ. 2007;20(335):806–8.
Peitzman AB, Harbrecht BG, Rivera L, Heil B, Eastern Association for the Surgery of Trauma Multiinstitutional Trials Workgroup. Failure of observation of blunt splenic injury in adults: variability in practice and adverse consequences. J Am Coll Surg. 2005;201(2):179–87.
Galvan DA, Peitzman AB. Failure of nonoperative management of abdominal solid organ injuries. Curr Opin Crit Care. 2006;12:590–4.
Di Saverio S, Moore EE, Tugnoli G, Naidoo N, Ansaloni L, Bonilauri S, Cucchi M, Catena F. Non operative management of liver and spleen traumatic injuries: a giant with clay feet. World J Emerg Surg. 2012;7(1):3. doi:10.1186/1749-7922-7-3.
Joseph JD, Brenner M, Scalea TM. Minimally invasive approach and endovascular techniques for vascular trauma. In: Di Saverio S, et al., editors. Trauma Surgery, vol. 1. Heidelberg: Springer-Verlag; 2014. p. 109–19.
Di Saverio S, Giorgini E, Biscardi A, Sibilio A, Villani S, Naidoo N, Catena F, Tugnoli G. Surgical treatment of spleen trauma. In: Di Saverio S, et al., editors. Trauma surgery, vol. 2. Heidelberg: Springer-Verlag; 2014. p. 117–34.
Di Saverio S, Sibilio A, Coniglio C, Bianchi E, Biscardi A, Villani S, Gordini G, Tugnoli G. A proposed algorythm for multimodal liver trauma management from a surgical trauma audit. In: A Western European Trauma Center. Minerva Anestesiol. 2014;29 (Epub ahead of print)
Levin CD, Patel UJ, Silverman PL, Wachsberg RH. Low attenuation of acute traumatic hemoperitoneum on CT scans. AJR. 1996;166:1089–93.
Baert AL, Sartor K. Imaging and intervention in abdominal trauma. Berlin: Springer; 2004. ISBN 3-540-65212-4 Chapter 4, p. 25–67
Author’s contribution
Gregorio Tugnoli, Elisa Bianchi and Salomone Di Saverio conceived and designed the study; Gregorio Tugnoli, Elisa Bianchi, Salomone Di Saverio, Carlo Coniglio, Andrea Biscardi, Salvatore Isceri and Giovanni Gordini made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; Gregorio Tugnoli and Salomone Di Saverio provided study materials or patients; Gregorio Tugnoli, Elisa Bianchi and Salomone Di Saverio collected and assembled the data, performed data analysis and interpretation, wrote the manuscript and the discussion; Salomone Di Saverio and Elisa Bianchi corrected and drafted the manuscript; Gregorio Tugnoli, Elisa Bianchi, Carlo Coniglio, Andrea Biscardi, Salvatore Isceri, Salomone Di Saverio, Giovanni Gordini performed the clinical audit activity; Salomone Di Saverio developed the clinical algorithm; Salomone Di Saverio and Elisa Bianchi designed the clinical algorithm; Gregorio Tugnoli, Elisa Bianchi, Carlo Coniglio, Andrea Biscardi, Salvatore Isceri, Luigi Simonetti, Giovanni Gordini and Salomone Di Saverio revised the manuscript for important intellectual content; Gregorio Tugnoli, Elisa Bianchi, Carlo Coniglio, Andrea Biscardi, Salvatore Isceri, Luigi Simonetti, Giovanni Gordini, Salomone Di Saverio gave final approval of the manuscript.
Conflict of interest
The authors declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
G. Tugnoli and S. Di Saverio contributed equally to this study and both authors certify that each had a “first author” role.
Rights and permissions
About this article
Cite this article
Tugnoli, G., Bianchi, E., Biscardi, A. et al. Nonoperative management of blunt splenic injury in adults: there is (still) a long way to go. The results of the Bologna-Maggiore Hospital trauma center experience and development of a clinical algorithm. Surg Today 45, 1210–1217 (2015). https://doi.org/10.1007/s00595-014-1084-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-014-1084-0