Abstract
Purpose
To investigate the prognostic factors of peripheral-type intrahepatic cholangiocarcinoma (PP-IHCC) and evaluate the surgical outcomes according to surgical strategy alterations.
Methods
Twenty-two patients were divided into two groups according to the surgical strategy: an extended surgery group (Ex group: n = 10), composed of those who underwent hepatic lobectomy combined with lymph node (LN) dissection and bile duct resection; and a customized surgery group (Cx group: n = 12), composed of those who underwent hepatectomy and bile duct resection according to tumor spread. LN dissection was not performed in patients without LN metastasis.
Results
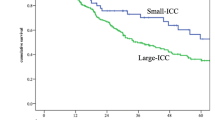
Multivariate analysis revealed that R2 resection, LN metastasis, and intrahepatic metastasis were independent prognostic factors. LN dissection was significantly infrequent in the Cx group. Survival after curative resection was similar in the two groups (3-year survival: 42.9 vs. 57.1%). Liver metastasis was the most frequent primary recurrence, occurring in more than 80% of patients from both groups.
Conclusions
Curative surgery might improve the prognosis of patients with PP-IHCC, but routine LN dissection is not recommended, particularly for patients without LN metastasis. Surgery alone, including LN dissection, cannot control this type of tumor, and additional treatment should be given.



Similar content being viewed by others
References
The Liver Study Group of Japan. The 16th report: surveillance of primary liver cancer patients in National Registry. Kyoto: LCSGJ; 2005.
Washburn WK, Lewis WD, Jenkins RL. Aggressive surgical resection for cholangiocarcinoma. Arch Surg. 1995;130:270–6.
Roayaie S, Guarrena JV, Ye MQ, Thung SN, Emre S, Fishbein TM, et al. Aggressive surgical treatment of intrahepatic cholangiocarcinoma: predictors of outcomes. J Am Coll Surg. 1998;187:365–72.
Kacznski J, Hanson G, Wallerstedt S. Incidence, etiologic aspects and clinicopathological features in intrahepatic cholangiocarcinoma: a study of 51 cases from a low endemicity area. Acta Oncol. 1988;37:77–83.
Shimada M, Sugimoto K, Iwahashi S, Utsunomiya T, Morine Y, Imura S, et al. CD133 expression is a potential prognostic indicator in intrahepatic cholangiocarcinoma. J Gastroenterol. 2010;45:896–902.
Chu KM, Lai ECS, Al-Hadeede S, Arcilla CE Jr, Lo CM, Liu CL, et al. Intrahepatic cholangiocarcinoma. World J Surg. 1997;21:301–6.
Casavila FA, Marsh JW, Iwatsuki S, Todo S, Lee RG, Madariaga R, et al. Hepatic resection and transplantation for peripheral cholangiocarcinoma. J Am Coll Surg. 1997;185:429–36.
Chou FF, Sheen-Chen SM, Chen YS, Chen MC, Chen CL. Surgical treatment of cholangiocarcinoma. Hepatogastroenterology. 1997;44:760–5.
Hasegawa K, Kokudo N. Surgical treatment of hepatocellular carcinoma. Surg Today. 2009;39:833–43.
Yamamoto M, Takasaki K, Otsubo T, Katsuragawa H, Katagiri S. Recurrence after surgical resection of intrahepatic cholangiocarcinoma. J Hepatobiliary Pancreat Surg. 2001;8:154–7.
Miwa S, Miyagawa S, Kobayashi A, Akahane Y, Nakata T, Mihara M, et al. Predictive factors for intrahepatic cholangiocarcinoma recurrence in the following surgery. J Gastroenterol. 2006;41:893–900.
Uenishi T, Kubo S, Yamazaki O, Yamada T, Sasaki Y, Nagano H, et al. Indications for surgical treatment of intrahepatic cholangiocarcinoma with lymph node metastasis. J Hepatobiliary Pancreat Surg. 2008;15:417–22.
Inoue K, Makuuchi M, Takayama T, Torzilli G, Yamamoto J, Shimada K, et al. Long-term survival and prognostic factors in the surgical treatment of mass-forming type cholangiocarcinoma. Surgery (St. Louis). 2000;127(5):498–505.
Shimada M, Yamashita Y, Aishima S, Shirabe K, Takenaka K, Sugimachi K. Value of lymph nodes dissection during resection of intrahepatic cholangiocarcinoma. Br J Surg. 2001;88:1463–6.
Liver Cancer Study Group of Japan. Classification of primary liver cancer, 1st English edition. Tokyo: Kanehara; 1997.
Nimura Y, Kamiya J, Nagino M, Kanai M, Uesaka K, Kondo S, et al. Aggressive surgical treatment of hilar cholangiocarcinoma. J Hepatobiliary Pancreat Surg. 1998;5:52–61.
Shirabe K, Shimada M, Harimoto N, Sugimachi K, Yamashita Y, Tsujita E, et al. Intrahepatic cholangiocarcinoma: its mode of spreading and therapeutic modalities. Surgery (St. Louis). 2002;131(1 suppl):S159–64.
Uenishi T, Hirohashi K, Kubo S, Yamamoto T, Yamazaki O, Kinoshita H. Clinicopathological factors predicting outcome after resection of mass-forming intrahepatic cholangiocarcinoma. Br J Surg. 2001;88:969–74.
Inoue K, Makuuchi M, Takayama T, Torzilli G, Yamamoto J, Shimada K, et al. Long-term survival and prognostic factors in the surgical treatment of mass-forming type cholangiocarcinoma. Surgery (St. Louis). 2000;127:498–505.
Shimada K, Sano T, Nara S, Esaki M, Sakamoto Y, Kosuge T, et al. Therapeutic value of lymph node dissection during hepatectomy in patients with intrahepatic cholangiocellular carcinoma with negative lymph node involvement. Surgery (St. Louis). 2009;145:411–6.
Morimoto Y, Tanaka Y, Ito T, Nakahara M, Nakaba H, Nishida T, et al. Long-term survival and prognostic factors in the surgical treatment for intrahepatic cholangiocarcinoma. J Hepatobiliary Pancreat Surg. 2003;10:432–40.
Ohtsuka M, Ito H, Kimura F, Shimizu H, Togawa A, Yoshidome H, et al. Results of surgical treatment for intrahepatic cholangiocarcinoma and clinicopathological factors influencing survival. Br J Surg. 2002;89:1525–31.
Nakagawa T, Kamiyama T, Kurauchi N, Matsushita M, Nakanishi K, Kamachi H, et al. Number of lymph node metastases is a significant prognostic factor in intrahepatic cholangiocarcinoma. World J Surg. 2005;29:728–33.
Suzuki S, Sakaguchi T, Yokoi Y, Okamoto K, Kurachi K, Tsuchiya Y, et al. Clinicopathological prognostic factors and impact of surgical treatment of mass-forming intrahepatic cholangiocarcinoma. World J Surg. 2002;26:687–93.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Morine, Y., Shimada, M., Utsunomiya, T. et al. Clinical impact of lymph node dissection in surgery for peripheral-type intrahepatic cholangiocarcinoma. Surg Today 42, 147–151 (2012). https://doi.org/10.1007/s00595-011-0057-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-011-0057-9