Abstract
Purpose
We evaluated the impact of advanced age on the morbidity, mortality, and long-term outcome after emergency surgery for diffuse peritonitis.
Methods
We retrospectively evaluated the mortality and morbidity rates in 36 patients who were 80 years of age or older and who had undergone emergency surgery for diffuse peritonitis, and calculated 5-year survival by the Kaplan-Meier method. Factors compromising prognosis were identified by univariate and multivariate analyses.
Results
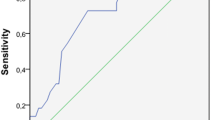
The median patient age was 84 years (range, 80–97 years); 16 patients were men and 20 were women. Preoperative concomitant disease was present in 81% of patients; cardiac disease was most common. Sites of visceral perforation were in the upper gastrointestinal tract in five patients, colon or rectum in 30, and gallbladder in 1. The postoperative morbidity rate was 72%, the surgical mortality rate was 11%, and the in-hospital mortality rate was 28%. The median hospital stay was 56 days. The median survival was 41 months, with a 5-year survival rate of 23%. A multivariate analysis identified number of failing organs as the only independent adverse prognostic factor (P < 0.001; relative risk 5.51, 95% confidence interval 1.97–15.4).
Conclusions
Elderly patients with diffuse peritonitis had an unsatisfactory rate of short-term morbidity and mortality compared with those undergoing elective surgery. Postoperative organ failure was most likely to compromise survival.
Similar content being viewed by others
References
Eguchi T, Fujii M, Takayama T. Mortality for gastric cancer in elderly patients. J Surg Oncol 2003;84:132–136.
Gretschel S, Estevez-Schwarz L, Hunerbein M, Schneider U, Schlag PM. Gastric cancer surgery in elderly patients. World J Surg 2006;30:1468–1474.
Coniglio A, Tiberio GA, Busti M, Gaverini G, Baiocchi L, Piardi T, et al. Surgical treatment for gastric carcinoma in the elderly. J Surg Oncol 2004;88:201–205.
Takeda J, Tanaka T, Koufuji K, Kodama I, Tsuji Y, Kakegawa T. Gastric cancer surgery in patients aged at least 80 years old. Hepatogastroenterology 1994;41:516–520.
Vironen JH, Sainio P, Husa AI, Kellokumpu IH. Complications and survival after surgery for rectal cancer in patients younger than and aged 75 years or older. Dis Colon Rectum 2004;47:1225–1231.
Barrier A, Ferro L, Houry S, Lacaine F, Huguier M. Rectal cancer surgery in patients more than 80 years of age. Am J Surg 2003;185:54–57.
Law WL, Choi HK, Ho JW, Lee YM, Seto CL. Outcomes of surgery for mid and distal rectal cancer in the elderly. World J Surg 2006;30:598–604.
Nishida K, Okinaga K, Miyazawa Y, Suzuki K, Tanaka M, Hatano M, et al. Emergency abdominal surgery in patients aged 80 years and older. Surg Today 2000;30:22–27.
Hinchey EJ, Schaal PG, Richards GK. Treatment of perforated diverticular disease of the colon. Adv Surg 1978;12:85–109.
American Collage of Chest Physicians and Society of Critical Care Medicine Consensus Conference. Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. Crit Care Med 1992;20:864–875.
Bohnen J, Boulanger M, Meakins JL, McLean AP. Prognosis in generalized peritonitis. Relation to cause and risk factors. Arch Surg 1983;118:285–290.
Koperna T, Schulz F. Prognosis and treatment of peritonitis. Do we need new scoring systems? Arch Surg 1996;131:180–186.
Linder MM, Wacha H, Feldmann U, Wesch G, Streifensand RA, Gundlach E. The Mannheim peritonitis index. An instrument for the intraoperative prognosis of peritonitis. Chirurg 1987;58:84–92.
Biondo S, Ramos E, Deiros M, Rague JM, De Oca J, Moreno P, et al. Prognostic factors for mortality in left colonic peritonitis: a new scoring system. J Am Coll Surg 2000;191:635–642.
Kriwanek S, Armbruster C, Beckerhinn P, Dittrich K. Prognostic factors for survival in colonic perforation. Int J Colorectal Dis 1994;9:158–162.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Okubo, R., Yajima, K., Sakai, Y. et al. Short-and long-term outcomes of surgery for diffuse peritonitis in patients 80 years of age and older. Surg Today 38, 413–419 (2008). https://doi.org/10.1007/s00595-007-3658-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00595-007-3658-6