Abstract
Aims
Maturity-onset diabetes of the young (MODY) is an autosomal dominant monogenic form of diabetes, and glucokinase-maturity-onset diabetes of the young (GCK-MODY), or MODY 2, being the most prevalent type. However, the presence of copy number variants (CNVs) may lead to misdiagnoses, as genetic testing for MODY is typically reliant on sequencing techniques. This study aimed to describe the process of diagnosis in a Chinese pedigree with an exon 8–10 deletion of the GCK gene.
Methods
This study collected clinical data and medical history through direct interviews with the patient and reviewing relevant medical records. Sanger sequencing and whole exome sequencing (WES) were conducted over years of follow up. WES-based CNV sequencing technology was used to detect CNVs and the results were validated by multiplex ligation-dependent amplification dosage assay (MLPA). Additionally, we reviewed the previously reported cases caused by heterozygous exon deletion of the GCK gene.
Results
WES-based CNV detection revealed a heterozygous exon 8–10 deletion in the GCK gene within this particular pedigree after Sanger sequencing and WES failed to find causal variants in single nucleotide variations (SNVs) and small indels. The deletion was considered pathogenic according to ACMG/AMP and ClinGen guidelines. Most of the previously reported cases caused by heterozygous exon deletion or whole gene deletion of the GCK gene present similarly to GCK-MODY caused by SNVs and small indels.
Conclusions
This study contributed to progress in our comprehension of the mutation spectrum of the GCK gene and underscored the significance of CNV detection in the genetic testing of MODY.



Similar content being viewed by others
References
Ellard S, Thomas K, Edghill EL et al (2007) Partial and whole gene deletion mutations of the GCK and HNF1A genes in maturity-onset diabetes of the young. Diabetologia 50(11):2313–2317. https://doi.org/10.1007/s00125-007-0798-6
Wang X, Lam SM, Cao M et al (2021) Localized increases in CEPT1 and ATGL elevate plasmalogen phosphatidylcholines in HDLs contributing to atheroprotective lipid profiles in hyperglycemic GCK-MODY. Redox Biol 40:101855. https://doi.org/10.1016/j.redox.2021.101855
Berberich AJ, Huot C, Cao H et al (2019) Copy number variation in GCK in patients with maturity-onset diabetes of the young. J Clin Endocrinol Metab 104(8):3428–3436. https://doi.org/10.1210/jc.2018-02574
Zhang B, Feng Z, Zhang L (1998) A study on the physical development of newborns of different gestational ages in 15 cities in China. Chin J Pediatr 26(4):206–208
Wang K, Li M, Hakonarson H (2010) ANNOVAR: functional annotation of genetic variants from high-throughput sequencing data. Nucleic Acids Res 38(16):e164–e164. https://doi.org/10.1093/nar/gkq603
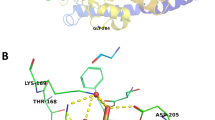
Kamata K, Mitsuya M, Nishimura T, Eiki J, Nagata Y (2004) Structural basis for allosteric regulation of the monomeric allosteric enzyme human glucokinase. Structure 12(3):429–438. https://doi.org/10.1016/j.str.2004.02.005
Concolino P, Tartaglione L, De Paolis E et al (2022) A novel GCK large genomic rearrangement in a patient with MODY-2 detected by clinical exome sequencing. Genes 13(11):2104. https://doi.org/10.3390/genes13112104
Steele AM, Shields BM, Wensley KJ, Colclough K, Ellard S, Hattersley AT (2014) Prevalence of vascular complications among patients with glucokinase mutations and prolonged, mild hyperglycemia. JAMA 311(3):279. https://doi.org/10.1001/jama.2013.283980
Birkebæk NH, Sørensen JS, Vikre-Jørgensen J, Jensen PKA, Pedersen O, Hansen T (2011) A De Novo whole GCK gene deletion not detected by gene sequencing, in a boy with phenotypic GCK insufficiency. Case Rep Genet 2011:1–3. https://doi.org/10.1155/2011/768610
Zhang H, Colclough K, Gloyn AL, Pollin TI (2021) Monogenic diabetes: a gateway to precision medicine in diabetes. J Clin Invest 131(3):e142244. https://doi.org/10.1172/JCI142244
Bitterman O, Tinto N, Franzese A et al (2018) Glucokinase deficit and birthweight: does maternal hyperglycemia always meet fetal needs? Acta Diabetol 55(12):1247–1250. https://doi.org/10.1007/s00592-018-1198-8
De Las HJ, Martínez R, Rica I et al (2010) Heterozygous glucokinase mutations and birth weight in Spanish children: letters. Diabet Med 27(5):608–610. https://doi.org/10.1111/j.1464-5491.2010.02953.x
López Tinoco C, Sánchez Lechuga B, Bacon S et al (2021) Evaluation of pregnancy outcomes in women with GCK-MODY. Diabet Med. https://doi.org/10.1111/dme.14488
Spyer G, Macleod KM, Shepherd M, Ellard S, Hattersley AT (2009) Pregnancy outcome in patients with raised blood glucose due to a heterozygous glucokinase gene mutation. Diabet Med 26(1):14–18. https://doi.org/10.1111/j.1464-5491.2008.02622.x
Stride A, Shields B, Gill-Carey O et al (2014) Cross-sectional and longitudinal studies suggest pharmacological treatment used in patients with glucokinase mutations does not alter glycaemia. Diabetologia 57(1):54–56. https://doi.org/10.1007/s00125-013-3075-x
Carmody D, Naylor RN, Bell CD et al (2016) GCK-MODY in the US national monogenic diabetes registry: frequently misdiagnosed and unnecessarily treated. Acta Diabetol 53(5):703–708. https://doi.org/10.1007/s00592-016-0859-8
Shields BM, McDonald TJ, Ellard S, Campbell MJ, Hyde C, Hattersley AT (2012) The development and validation of a clinical prediction model to determine the probability of MODY in patients with young-onset diabetes. Diabetologia 55(5):1265–1272. https://doi.org/10.1007/s00125-011-2418-8
Fu J, Ping F, Wang T et al (2021) A clinical prediction model to distinguish maturity-onset diabetes of the young from type 1 and type 2 diabetes in the chinese population. Endocr Pract 27(8):776–782. https://doi.org/10.1016/j.eprac.2021.05.002
Zhang H, Kleinberger JW, Maloney KA et al (2022) Model for integration of monogenic diabetes diagnosis into routine care: the personalized diabetes medicine program. Diabetes Care 45(8):1799–1806. https://doi.org/10.2337/dc21-1975
Pinelli M, Acquaviva F, Barbetti F, Caredda E, Cocozza S, Delvecchio M, Italian Study Group on Diabetes of the Italian Society of Pediatric Endocrinology and Diabetology (ISPED). (2013) Identification of candidate children for maturity-onset diabetes of the young type 2 (MODY2) gene testing: a seven-item clinical flowchart (7-iF). PLoS One, 8(11): e79933
Chakera AJ, Steele AM, Gloyn AL et al (2015) Recognition and management of individuals with hyperglycemia because of a heterozygous glucokinase mutation. Diabetes Care 38(7):1383–1392. https://doi.org/10.2337/dc14-2769
Garin I, Rica I, Estalella I et al (2008) Haploinsufficiency at GCK gene is not a frequent event in MODY2 patients. Clin Endocrinol (Oxf) 68(6):873–878. https://doi.org/10.1111/j.1365-2265.2008.03214.x
Yorifuji T, Fujimaru R, Hosokawa Y et al (2012) Comprehensive molecular analysis of Japanese patients with pediatric-onset MODY-type diabetes mellitus. Pediatr Diabetes 13(1):26–32. https://doi.org/10.1111/j.1399-5448.2011.00827.x
Kawakita R, Hosokawa Y, Fujimaru R et al (2014) Molecular and clinical characterization of glucokinase maturity-onset diabetes of the young (GCK-MODY) in Japanese patients. Diabet Med 31(11):1357–1362. https://doi.org/10.1111/dme.12487
Katashima R, Matsumoto M, Watanabe Y, Moritani M, Yokota I (2021) Identification of novel GCK and HNF4α gene variants in japanese pediatric patients with onset of diabetes before 17 years of age. J Diabetes Res. https://doi.org/10.1155/2021/7216339
Trhanint S, Bouguenouch L, Abourazzak S et al (2022) Molecular and clinical assessment of maturity-onset diabetes of the young revealed low mutational rate in Moroccan families. Int J Pediatr Adolesc Med 9(2):98–103. https://doi.org/10.1016/j.ijpam.2021.03.006
Acknowledgements
The authors would like to thank the participants in this study.
Funding
This work was supported by the grants from National Natural Science Foundation of China (No. 82170854, 81870579, 81870545, 81570715, 81170736), Beijing Natural Science Foundation (7202163), Beijing Municipal Science & Technology Commission (Z201100005520011), National High Level Hospital Clinical Research Funding (2022-PUMCH-C-019, 2022-PUMCH-B-121), National Key Research and Development Program of China (2018YFC2001100), CAMS Innovation Fund for Medical Sciences (CIFMS2021-1-I2M-002, CIFMS2017-I2M-1–008).
Author information
Authors and Affiliations
Contributions
RY analyzed the clinical data and wrote the manuscript. HZ contributed with gene analysis and was a major contributor to the writing of the manuscript. XX was contributed to acquisition and interpretation of the data, and revised the manuscript. All authors approved the final manuscript as submitted and agree to be accountable for all aspects of the work.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare no conflict of interest.
Ethical approval
The study was approved by the ethics committee of Peking Union Medical College Hospital, China. The reference number is K2985, and the date of approval is 2023–3-13.
Informed consent
Guardian provided informed consent for genetic testing and analysis.
Human and animal rights
Informed consent was provided by the patient.
Additional information
Managed by Fabrizio Barbetti.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yu, R., Zhang, H. & Xiao, X. Partial GCK gene deletion mutations causing maturity-onset diabetes of the young. Acta Diabetol 61, 107–115 (2024). https://doi.org/10.1007/s00592-023-02173-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-023-02173-1