Abstract
Aims
High glycemic variability (GV) is the major indication for islet transplantation (IT) in patients with type 1 diabetes (T1D). The actual criteria used to assess graft function do not consider GV improvement. Our study aimed to describe GV indices’ evolution in T1D patients who benefited from IT during the TRIMECO trial and to evaluate if thresholds might be defined to diagnose IT success.
Methods
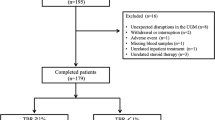
We collected data from 29 patients of the TRIMECO trial, a clinical trial (NCT01148680) comparing the metabolic efficacy of IT with intensive insulin therapy. Based on CGM data, we analyzed mean glucose level and four GV indices (standard deviation, coefficient of variation, MAGE and GVP) before (M0) and 6 months (M6) after IT.
Results
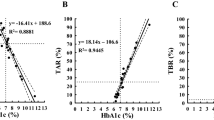
Each GV index decreased significantly between M0 and M6: SD 53.9 mg/dL [44.6–61.5] versus 20.1 mg/dL [13.5–24.3]; CV 35.2% [30.6–37.7] versus 17.3% [12.0–20.5]; MAGE 134.9 mg/dl [111.2–155.8] versus 51.9 mg/dL [32.4–62.4]; GVP 35.3% [24.9–47.2] versus 12.2% [6.2–18.8] (p ≤ 0.0001). Thresholds diagnosing IT success at 6 months post-transplant were an SD at 22.76 mg/dL (sensibility 88.89%, specificity 80.00%), a CV at 17.47% (sensibility 88.89%, specificity 70.00%), a MAGE at 54.81 mg/dL (sensibility 88.89%, specificity 80.00%) and a GVP at 12.27% (sensibility 88.89%, specificity 70.00%).
Conclusions
This study confirms a positive impact of IT on GV. The proposed thresholds allow an easy evaluation of IT success using only CGM data and may be a clinical tool for the follow-up of transplanted patients.




Similar content being viewed by others
Abbreviations
- CGM:
-
Continuous glucose monitoring
- CV:
-
Coefficient of variation
- GV:
-
Glycemic variability
- GVP:
-
Glycemic variability percentage
- HbA1c:
-
Glycated hemoglobin
- IT:
-
Islet transplantation
- MAGE:
-
Mean amplitude glycemic excursion
- ROC curve:
-
Receiver operating characteristic curve
- SD:
-
Standard deviation
- Se:
-
Sensibility
- Spe:
-
Specificity
- T1D:
-
Type 1 diabetes
- TIR:
-
Time in range
References
Hirsch IB (2005) Glycemic variability: it’s not just about A1C anymore! Diabetes Technol Ther 7(5):780–783
Ceriello A, Monnier L, Owens D (2019) Glycaemic variability in diabetes: clinical and therapeutic implications. Lancet Diabetes Endocrinol 7(3):221–230
Guerci B (2003) Asymptomatic glycemic instability: How to measure it and which clinical applications? Diabetes Metab 29(2 Pt 1):179–188
Saisho Y (2014) Glycemic variability and oxidative stress: a link between diabetes and cardiovascular disease? Int J Mol Sci 15(10):18381–18406
Rodbard D (2009) Interpretation of continuous glucose monitoring data: glycemic variability and quality of glycemic control. Diabetes Technol Ther 11(Suppl 1):S55–S67
Fabris C, Facchinetti A, Sparacino G et al (2014) Glucose variability indices in type 1 diabetes: parsimonious set of indices revealed by sparse principal component analysis. Diabetes Technol Ther 16(10):644–652
Miller KM, Foster NC, Beck RW et al (2015) Current state of type 1 diabetes treatment in the U.S.: updated data from the T1D Exchange clinic registry. Diabetes Care 38(6):971–978
Gill GV (1992) The spectrum of brittle diabetes. J R Soc Med 85(5):259–261
Benhamou PY, Milliat-Guittard L, Wojtusciszyn A et al (2009) Quality of life after islet transplantation: data from the GRAGIL 1 and 2 trials. Diabet Med J Br Diabet Assoc 26(6):617–621
Kent LA, Gill GV, Williams G (1994) Mortality and outcome of patients with brittle diabetes and recurrent ketoacidosis. Lancet Lond Engl 344(8925):778–781
Wojtusciszyn A, Branchereau J, Esposito L, et al (2019) Indications for islet or pancreatic transplantation: statement of the TREPID working group on behalf of the Société francophone du diabète (SFD), Société francaise d’endocrinologie (SFE), Société francophone de transplantation (SFT) and Société française de néphrologie-dialyse-transplantation (SFNDT). Diabetes Metab 45(3):224–237
CITR 9th annual report | CITR [Internet]. [cited 2018 May 2]. Available from: https://citregistry.org/content/citr-9th-annual-report. Accessed 2 May 2018
Lablanche S, Vantyghem M-C, Kessler L et al (2018) Islet transplantation versus insulin therapy in patients with type 1 diabetes with severe hypoglycaemia or poorly controlled glycaemia after kidney transplantation (TRIMECO): a multicentre, randomised controlled trial. Lancet Diabetes Endocrinol 6(7):527–537
Ryan EA, Paty BW, Senior PA, Lakey JRT, Bigam D, Shapiro AMJ (2005) Beta-score: an assessment of beta-cell function after islet transplantation. Diabetes Care 28(2):343–347
Rickels MR, Stock PG, de Koning EJP et al (2018) Defining outcomes for β-cell replacement therapy in the treatment of diabetes: a consensus report on the igls criteria from the IPITA/EPITA opinion leaders workshop. Transplantation 102(9):1479–1486
Scheiner G (2016) CGM retrospective data analysis. Diabetes Technol Ther 18(Suppl 2):S2-14–S2-22
Monnier L, Colette C, Wojtusciszyn A et al (2017) Toward defining the threshold between low and high glucose variability in diabetes. Diabetes Care 40(7):832–838
Service FJ, Molnar GD, Rosevear JW, Ackerman E, Gatewood LC, Taylor WF (1970) Mean amplitude of glycemic excursions, a measure of diabetic instability. Diabetes 19(9):644–655
Su G, Mi S, Tao H et al (2013) Impact of admission glycemic variability, glucose, and glycosylated hemoglobin on major adverse cardiac events after acute myocardial infarction. Diabetes Care 36(4):1026–1032
Peyser TA, Balo AK, Buckingham BA, Hirsch IB, Garcia A (2018) Glycemic variability percentage: a novel method for assessing glycemic variability from continuous glucose monitor data. Diabetes Technol Ther 20(1):6–16
Vantyghem M-C, Raverdy V, Balavoine A-S et al (2012) Continuous glucose monitoring after islet transplantation in type 1 diabetes: an excellent graft function (β-score greater than 7) Is required to abrogate hyperglycemia, whereas a minimal function is necessary to suppress severe hypoglycemia (β-score greater than 3). J Clin Endocrinol Metab 97(11):E2078–E2083
Kessler L, Passemard R, Oberholzer J et al (2002) Reduction of blood glucose variability in type 1 diabetic patients treated by pancreatic islet transplantation: interest of continuous glucose monitoring. Diabetes Care 25(12):2256–2262
Ryan EA, Lakey JR, Rajotte RV et al (2001) Clinical outcomes and insulin secretion after islet transplantation with the Edmonton protocol. Diabetes 50(4):710–719
Brooks AM, Oram R, Home P, Steen N, Shaw JAM (2015) Demonstration of an intrinsic relationship between endogenous C-peptide concentration and determinants of glycemic control in type 1 diabetes following islet transplantation. Diabetes Care 38(1):105–112
Geiger MC, Ferreira JV, Hafiz MM et al (2005) Evaluation of metabolic control using a continuous subcutaneous glucose monitoring system in patients with type 1 diabetes mellitus who achieved insulin independence after islet cell transplantation. Cell Transplant 14(2–3):77–84
Zhou J, Li H, Ran X et al (2011) Establishment of normal reference ranges for glycemic variability in Chinese subjects using continuous glucose monitoring. Med Sci Monit Int Med J Exp Clin Res 17(1):CR9–CR13
Hill NR, Oliver NS, Choudhary P, Levy JC, Hindmarsh P, Matthews DR (2011) Normal reference range for mean tissue glucose and glycemic variability derived from continuous glucose monitoring for subjects without diabetes in different ethnic groups. Diabetes Technol Ther 13(9):921–928
Reddy M, Godsland IF, Barnard KD et al (2015) Glycemic variability and its impact on quality of life in adults with type 1 diabetes. J Diabetes Sci Technol 10(1):60–66
Siegelaar SE, Kilpatrick ES, Rigby AS, Atkin SL, Hoekstra JBL, Devries JH (2009) Glucose variability does not contribute to the development of peripheral and autonomic neuropathy in type 1 diabetes: data from the DCCT. Diabetologia 52(10):2229–2232
Benhamou PY, Somers F, Lablanche S et al (2014) Impact of flexible insulin therapy on blood glucose variability, oxidative stress and inflammation in type 1 diabetic patients: the VARIAFIT study. Diabetes Metab 40(4):278–283
Rodbard D (2011) Clinical interpretation of indices of quality of glycemic control and glycemic variability. Postgrad Med 123(4):107–118
Crenier L, Lytrivi M, Van Dalem A, Keymeulen B, Corvilain B (2016) Glucose complexity estimates insulin resistance in either nondiabetic individuals or in type 1 diabetes. J Clin Endocrinol Metab 101(4):1490–1497
Hanefeld M, Koehler C, Hoffmann C, Wilhelm K, Kamke W, Gerstein H (2010) Effect of targeting normal fasting glucose levels with basal insulin glargine on glycaemic variability and risk of hypoglycaemia: a randomized, controlled study in patients with early Type 2 diabetes. Diabet Med J Br Diabet Assoc 27(2):175–180
Gude F, Díaz-Vidal P, Rúa-Pérez C et al (2017) Glycemic variability and its association with demographics and lifestyles in a general adult population. J Diabetes Sci Technol 11(4):780–790
Juvenile Diabetes Research Foundation Continuous Glucose Monitoring Study Group, Fox LA, Beck RW, Xing D (2010) Variation of interstitial glucose measurements assessed by continuous glucose monitors in healthy, nondiabetic individuals. Diabetes Care 33(6):1297–1299
Danne T, Nimri R, Battelino T et al (2017) International consensus on use of continuous glucose monitoring. Diabetes Care 40(12):1631–1640
Bergenstal RM, Ahmann AJ, Bailey T et al (2013) Recommendations for standardizing glucose reporting and analysis to optimize clinical decision making in diabetes: the ambulatory glucose profile. J Diabetes Sci Technol 7(2):562–578
Funding
This work was supported by a Research Year Scholarship from Grenoble Alpes University.
Author information
Authors and Affiliations
Consortia
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical standard
The institutional review board approved the study (French Committee for the Protection of Persons participating in biomedical research “Sud-Est V”; no 09-CHUG-21) and Clinical Trial Authorization was obtained from the French National Competent Authority (ANSM-no 2008-A01554-51).
Informed consent
Informed consent was obtained from the patients included in this study.
Additional information
Managed by Massimo Federici.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Members listed in the appendix are belongs to TRIMECO Study Group.
Appendix
Appendix
Department of Endocrinology, Diabetes, and Nutrition (Lablanche MD, Prof P-Y Benhamou MD), French National Center for Scientific Research (Prof J-L Bosson MD, K Skaare PhD), Department of Nephrology (R Tetaz MD), Department of Clinical Trial Surveillance, Direction of Clinical Research and Innovation (S Logerot PharmD), and Cellular Therapy Unit, National Blood Service Rhône-Alpes (H Egelhofer PhD), Grenoble University Hospital, and Department of Public Health (Prof J-L Bosson, K Skaare), Grenoble Alpes University, Grenoble, France; Inserm U1055, Laboratory of Fundamental and Applied Bioenergetics Grenoble, Grenoble, France (S Lablanche, Prof P-Y Benhamou); Laboratoire des Techniques de l’Ingénierie Médicale et de la Complexité–Informatique, Mathématiques et Applications de Grenoble, Grenoble, France (Prof J-L Bosson, K Skaare); Department of Endocrinology, Diabetes, and Nutrition, C Huriez Hospital, Lille University Hospital, Lille, France; Inserm 1190, European Genomic Institute for Diabetes, Lille, France (Prof M-C Vantyghem MD, Prof J Kerr-Conte PhD, K Benomar MD, Prof F Pattou MD); Hôpitaux Universitaires de Strasbourg, Service d’Endocrinologie Diabète et Maladies Métaboliques, and Equipe d’Accueil 7293, Fédération de Médecine Translationnelle de Strasbourg, Université de Strasbourg, Strasbourg, France (Prof L Kessler MD); Department of Endocrinology, Diabetes, and Nutrition, Montpellier University Hospital, and Laboratory of Cell Therapy of Diabetes, Institute of Functional Genomics, Mixed Research Unit, French National Center for Scientific Research 5203, Inserm U1191, University of Montpellier, Montpellier, France (Prof A Wojtusciszyn MD, Prof E Renard MD); Centre Hospitalier Universitaire Jean Minjoz, Service d’Endocrinologie-Métabolisme et Diabétologie-Nutrition, Besançon, France (S Borot MD); Service d’Endocrinologie Diabète Nutrition (Prof C Thivolet MD) Pôle de Santé Publique Service Evaluation Economique en Santé (Prof C Colin MD, Gwen Grguric PhD, C Camillo-Brault PharmD), Service de Transplantation, Néphrologie et Immunologie Clinique (Prof E Morelon MD, F Buron MD), and Service d’Urologie et de Chirurgie de la Transplantation (Prof L Badet MD), Hospices Civils de Lyon, Groupement Hospitalier Centre, Université de Lyon, Lyon, France; Service de Néphrologie, Centre Hospitalier Universitaire de Nancy, Nancy, France (S Girerd MD); Department of Surgery, Islet Isolation, and Transplantation, Geneva University Hospitals, Geneva, Switzerland (D Bosco PhD, Prof T Berney MD); F-69003, EA 7425 Health Services and Performance Research, Public Health Service and Health Economic Evaluation, Claude Bernard University Lyon 1, Lyon, France (Prof C Colin, G Grguric, C Camillo-Brault); Department of Diabetes, Sud-Francilien Hospital, Corbeil-Essonnes, France (Prof A Penfornis MD); and Université Paris-Sud, Orsay, France (Prof A Penfornis).
Rights and permissions
About this article
Cite this article
Jalbert, M., Zheng, F., Wojtusciszyn, A. et al. Glycemic variability indices can be used to diagnose islet transplantation success in type 1 diabetic patients. Acta Diabetol 57, 335–345 (2020). https://doi.org/10.1007/s00592-019-01425-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00592-019-01425-3