Abstract
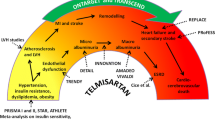
Cardiovascular risk is determined by multiple risk factors, all of which greatly increase the chance of morbidity and mortality. So-called “normal” levels of these factors are not biologically normal, so current strategy is based on estimations of a person’s global cardiovascular risk, and then using appropriate combinations of treatments in higher-risk people. Angiotensin-converting enzyme (ACE) inhibitors and angiotensin II receptor blockers (ARBs) provide multiple actions against many of the risk factors for cardiovascular disease and also show some evidence of an effect that is independent of blood pressure reduction. The ONgoing Telmisartan Alone and in combination with Ramipril Global Endpoint Trial (ONTARGET) is designed to clarify whether an ARB (telmisartan), an ACE inhibitor (ramipril) or a combination of both confers blood pressure-independent cardioprotection in high-risk patients whose blood pressure is well controlled. The Telmisartan Randomized AssessmeNt Study in ACE iNtolerant subjects with cardiovascular Disease (TRANSCEND) trial has the same endpoints, but will compare telmisartan with placebo in patients who are intolerant to an ACE inhibitor. Primary endpoints for both trials are the composite of cardiovascular death, non-fatal myocardial infarction, non-fatal stroke or hospitalisation for heart failure. Recruitment is now complete, with 25 620 patients randomised in ONTARGET and 5926 in TRANSCEND. Baseline patient characteristics are similar to those in the Heart Outcomes Prevention Evaluation (HOPE) study, except that the current trials have greater ethnic diversity (including an important cohort from Asia). The subjects are slightly older and mean blood pressure at randomisation is again normal, but slightly lower than in HOPE. The use of beta-blockers and lipid-lowering therapy, known to reduce mortality and morbidity, is also higher in ONTARGET/TRANSCEND. These trials are the largest comparisons to date of ARB and ACE-inhibitor therapy in high-risk patients with controlled blood pressure, and the results will contribute significantly to the future treatment of cardiovascular disease.
Similar content being viewed by others
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sleight, P. The ONTARGET/TRANSCEND Trial Programme: baseline data. Acta Diabetol 42 (Suppl 1), s50–s56 (2005). https://doi.org/10.1007/s00592-005-0181-3
Issue Date:
DOI: https://doi.org/10.1007/s00592-005-0181-3