Abstract
Aims
To assess the pre- and postoperative responses to each of the 12 individual Oxford Knee Score (OKS) questions and percentages of those that were better, same or worse after primary knee arthroplasty (KA).
Methods
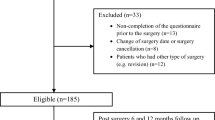
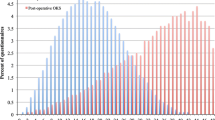
A single centre retrospective cohort study conducted over a 24-month period which included 3259 patients with completed OKS preoperatively and 1-year after KA. There were 1286 males and 1973 females, with an overall mean age of 70.0 (range 34–94). The mean scores for each question of the OKS were compared between baseline and 1-year. The percentage of patients who reported better, the same or worse postoperative symptoms for each question were calculated and represented on a heatmap.
Results
There were significant (p < 0.001) improvements in all 12 questions, all of which demonstrated moderate (Q2, Q7) or large effect sizes. Improvements in individual question responses varied. Symptoms of pain and limping demonstrated the greatest improvement, with 86% of patients enjoying a positive change in their symptoms. Despite this improvement 1067 (41.4%) continued to have mild to severe pain in their knee, and 442 (17.3%) patients limped often to all the time when walking postoperatively. Whereas other questions that did not improve to the same extent for example washing and drying only improved in 53% of patients but only 347 (13.5%) had moderate/extreme trouble or found it impossible to do this postoperatively. Preoperatively four questions (Q1, Q6, Q7, Q8) demonstrated floor effects, postoperatively all questions apart from question 7 (kneeling) demonstrated ceiling effects.
Conclusion
The mean improvement and outcome at 1-year for each of the 12 questions varied according to the patient’s preoperative response. As a clinical tool, the heatmap (improvement, same and worse) will enable communication to patients about their potential change in their knee specific symptoms according to their preoperative responses.
Level of evidence
Retrospective study, Level III.
Similar content being viewed by others
References
Murray DW, Fitzpatrick R, Rogers K et al (2007) The use of the Oxford hip and knee scores. J Bone Jt Surg Ser B 89:1010–1014
Dawson J, Fitzpatrick R, Murray D, Carr A (1998) Questionnaire on the perceptions of patients about total knee replacement. J Bone Jt Surg Ser B 80:63–69. https://doi.org/10.1302/0301-620X.80B1.7859
Ben-Shlomo Y, Blom A, Boulton C et al (2021) The national joint registry 18th annual report 2021. In: National joint registry 18th annual report 2021
Dawson J, Fitzpatrick R, Murray D, Carr A (2006) A response to issues raised in a recent paper concerning the Oxford knee score. Knee 13:66–68. https://doi.org/10.1016/j.knee.2005.08.004
Collins NJ, Misra D, Felson DT et al (2011) Measures of knee function: international knee documentation committee (IKDC) subjective knee evaluation form, knee injury and osteoarthritis outcome score (KOOS), knee injury and osteoarthritis outcome score physical function short form (KOOS-PS), knee Ou. Arthritis Care Res 63:S208–S228. https://doi.org/10.1002/acr.20632
Beswick AD, Wylde V, Gooberman-Hill R et al (2012) What proportion of patients report long-term pain after total hip or knee replacement for osteoarthritis? A systematic review of prospective studies in unselected patients. BMJ Open 2:1–12. https://doi.org/10.1136/bmjopen-2011-000435
Clement ND, MacDonald D, Burnett R (2013) Predicting patient satisfaction using the Oxford knee score: where do we draw the line? Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-013-1728-3
Yap YYW, Edwards KL, Soutakbar H et al (2021) Oxford knee score 1 year after TKR for osteoarthritis with reference to a normative population: what can patients expect? Osteoarthr Cartil Open 3:100143. https://doi.org/10.1016/j.ocarto.2021.100143
Buus AAØ, Laugesen B, El-Galaly A et al (2022) The potential of dividing the oxford knee score into subscales for predicting clinically meaningful improvements in pain and function of patients undergoing total knee arthroplasty. Int J Orthop Trauma Nurs 45:100919. https://doi.org/10.1016/j.ijotn.2021.100919
Harris K, Dawson J, Doll H et al (2013) Can pain and function be distinguished in the Oxford knee score in a meaningful way? An exploratory and confirmatory factor analysis. Qual Life Res 22:2561–2568. https://doi.org/10.1007/s11136-013-0393-x
Scott CEH, Howie CR, MacDonald D, Biant LC (2010) Predicting dissatisfaction following total knee replacement: a prospective study of 1217 patients. J Bone Jt Surg Ser B 92:1253–1258. https://doi.org/10.1302/0301-620X.92B9.24394
Baker PN, van der Meulen JH, Lewsey J, Gregg PJ (2007) The role of pain and function in determining patient satisfaction after total knee replacement. Data from the national joint registry for England and Wales. J Bone Jt Surg - Ser B 89:893–900. https://doi.org/10.1302/0301-620X.89B7.19091
Tay ML, Monk AP, Frampton CM et al (2023) The strongest Oxford knee score predictors of subsequent revision are overall pain, limping when walking, and knee giving way. J Arthroplast 38:S156-S161.e3. https://doi.org/10.1016/j.arth.2023.03.001
Vijayananthan A, Nawawi O (2008) The importance of good clinical practice guidelines and its role in clinical trials. Biomed Imaging Interv J 4:e5
Makaram N, Lee T, Macdonald D, Clement ND (2020) The verbal Oxford knee score is not clinically different from the written score when assessed before or after total knee arthroplasty. Knee 27:1396–1405. https://doi.org/10.1016/j.knee.2020.07.098
McHorney CA, Tarlov AR (1995) Individual-patient monitoring in clinical practice: are available health status surveys adequate? Qual Life Res 4:293–307. https://doi.org/10.1007/BF01593882
Abbott S, Radha S, Afzal I et al (2023) Patella resurfacing is not associated with a difference in the Oxford knee score after total knee arthroplasty but stair descent is enhanced. Arch Orthop Trauma Surg 143:5333–5343. https://doi.org/10.1007/s00402-022-04733-6
Clement ND, Edwards J, Afzal I et al (2023) Posterior stabilised total knee arthroplasty is associated with improved post-operative knee specific function, health related quality of life and greater satisfaction when compared to cruciate retaining protheses. Eur J Orthop Surg Traumatol 33:3411–3418. https://doi.org/10.1007/s00590-023-03565-3
Leppink J, O’Sullivan P, Winston K (2016) Effect size – large, medium, and small. Perspect Med Educ 5:347–349. https://doi.org/10.1007/s40037-016-0308-y
Luger M, Schopper C, Krottenthaler ES et al (2023) Not all questions are created equal: the weight of the Oxford knee scores questions in a multicentric validation study. J Orthop Traumatol. https://doi.org/10.1186/s10195-023-00722-6
Scott CEH, Oliver WM, MacDonald D et al (2016) Predicting dissatisfaction following total knee arthroplasty in patients under 55 years of age. Bone Jt J 98:1625–1634. https://doi.org/10.1302/0301-620X.98B12.BJJ-2016-0375.R1
Clark GW, Steer RA, Khan RN et al (2023) Maintaining joint line obliquity optimizes outcomes of functional alignment in total knee arthroplasty in patients with constitutionally varus knees. J Arthroplast 38:S239–S244. https://doi.org/10.1016/j.arth.2023.04.004
Clement ND, Afzal I, Demetriou C et al (2020) There is no clinically important difference in the Oxford knee scores between one and two years after total knee arthroplasty: the one-year score could be used as the benchmark timepoint to assess outcome. Knee 27:1212–1218. https://doi.org/10.1016/j.knee.2020.05.015
Beard DJ, Harris K, Dawson J et al (2015) Meaningful changes for the Oxford hip and knee scores after joint replacement surgery. J Clin Epidemiol 68:73–79. https://doi.org/10.1016/j.jclinepi.2014.08.009
Womersley A, Clement · Nick, Jones S, et al (2023) Post-traumatic stress disorder is more likely in younger patients undergoing lower limb arthroplasty: impact on function and quality of life. Arch Orthop Trauma Surg 2023(1):1–9. https://doi.org/10.1007/S00402-023-05050-2
Judge A, Arden NK, Cooper C et al (2012) Predictors of outcomes of total knee replacement surgery. Rheumatol (United Kingdom) 51:1804–1813. https://doi.org/10.1093/rheumatology/kes075
Yapp LZ, Clement ND, Macdonald DJ et al (2020) Changes in expectation fulfillment following total knee arthroplasty: a 10-year follow-up study. J Arthroplast 35:1826–1832. https://doi.org/10.1016/j.arth.2020.02.064
Clement ND, Afzal I, Demetriou C et al (2020) The preoperative oxford knee score is an independent predictor of achieving a postoperative ceiling score after total knee arthroplasty. Bone Jt J 102:1519–1526. https://doi.org/10.1302/0301-620X.102B11.BJJ-2019-1327.R1
Ko Y, Lo NN, Yeo SJ et al (2009) Rasch analysis of the Oxford Knee score. Osteoarthr Cartil 17:1163–1169. https://doi.org/10.1016/j.joca.2009.04.004
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Ethical approval
This study was classed as a service evaluation and did not meet the criteria requiring ethical approval. The project was registered with the institution’s audit department and was conducted in accordance with the Declaration of Helsinki and the guidelines for good clinical practice.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Clement, N.D., Jones, S., Afzal, I. et al. A comprehensive analysis of the pre- and postoperative responses to each of the 12 Oxford knee score questions one year following knee arthroplasty. Eur J Orthop Surg Traumatol (2024). https://doi.org/10.1007/s00590-024-03870-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00590-024-03870-5