Abstract
Purpose
A type IX SLAP (superior labrum anterior to posterior) lesion involves 360° of the glenohumeral labrum. Only rare reports have been published analyzing the risk factors of this lesion and the success of its arthroscopic management. The aim of our study is to evaluate predisposing factors that lead to SLAP IX and to assess the clinical outcome after arthroscopic treatment. Our treatment algorithm is also presented.
Methods
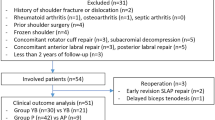
We report on a series of six patients treated in our institution between January 2014 and January 2019 who underwent shoulder arthroscopy and were intraoperatively found to have a SLAP lesion type IX. Arthroscopic labral repair and biceps tenodesis were indicated in all patients. American Shoulder and Elbow Surgeons (ASES) Shoulder Score, Rowe Score and Constant Murley Shoulder Score (CS) were used for clinical evaluation. Patients were evaluated preoperatively and at 12 weeks, 1 year and 2 years postoperatively.
Results
We analyzed six patients of which 83% were males (5/6 patients). The average age at the time of surgery was 37.16 (range 30–42 years). The dominant arm was affected in 50% of patients (3/6 patients). A significant postoperative improvement was seen in all six patients. 83% (5/6) of patients returned to their pre-injury activity level. Average values of all three measured scores show a significant increase comparing preoperative to postoperative period (P-value < 0.05). All patients were able to return to work.
Conclusions
The final diagnosis was established intraoperatively as 83% (5/6) of radiology reports differed from subsequent arthroscopic findings. The mechanism of injury in all our cases was high energy trauma with traction, arm in abduction or anteflexion. We observed great success with arthroscopic treatment as high percentage of our patients returned back to work and sports.





Similar content being viewed by others
References
Andrews JR, Carson WG, Mcleod WD (1985) Glenoid labrum tears related to the long head of the biceps. Am J Sports Med 13:4158
Snyder SJ, Karzel RP, Del PW, Ferkel RD, Friedman MJ (2010) SLAP lesions of the shoulder. Arthrosc J Arthrosc Relat Surg 5:4489
Maffet MW, Gartsman GM, Moseley B (1995) Superior Labrum-Biceps tendon complex lesions of the shoulder. Am J Sports Med 23:9885
Nord KD, RKN R. Further refinement of slap classification...-Google Scholar. provide for approach to SLAP IV lesions dictates tenodesis, performing biceps tenotomy shows a higher rate of leaving a cosmetic deformity but may be preferred in case of elderly patients (8,16,19).
Powell SE, Nord KD, Ryu RKN (2012) The diagnosis, classification, and treatment of SLAP lesions. Oper Tech Sports Med 4:20
Knesek M, Skendzel JG, Dines JS, Altchek DW, Allen AA, Bedi A (2013) Diagnosis and management of superior labral anterior posterior tears in throwing athletes. Am J Sports Med 6:41
Nam EK, Snyder SJ (2017) The diagnosis and treatment of superior labrum, anterior and posterior (SLAP). Lesions 31:798–810
Provencher MT, McCormick F, Dewing C, McIntire S, Solomon D (2013) A prospective analysis of 179 type 2 superior labrum anterior and posterior repairs: outcomes and factors associated with success and failure. Am J Sports Med 41:880–886
Denard PJ, Lädermann A, Parsley BK, Burkhart SS (2014) Arthroscopic biceps tenodesis compared with repair of isolated type II SLAP lesions in patients older than 35 years. Orthopedics 37:4119
Denard PJ, Ldermann A, Burkhart SS (2012) Long-term outcome after arthroscopic repair of type II SLAP lesions: results according to age and workers’ compensation status. Arthrosc Arthrosc 28:451–457
Ek ETH, Shi LL, Tompson JD, Freehill MT, Warner JJP (2014) Surgical treatment of isolated type II superior labrum anterior-posterior (SLAP) lesions: repair versus biceps tenodesis. J Shoulder Elb Surg Mosby 23:1059–1065
Stathellis A, Brilakis E, Georgoulis J-D, Antonogiannakis E, Georgoulis A (2018) Send orders for reprints to reprints@benthamscience.ae. Open Orthop J Treat 12:288–294
Vopat ML, Coda RG, Giusti NE, Baker J, Tarakemeh A, Schroeppel JP, Mullen S, Randall J, Provencher MT, Vopat BG (2021) Differences in outcomes between anterior and posterior shoulder instability after arthroscopic bankart repair: a systematic review and meta-analysis. Orthop J Sports Med 9(5):4889
Michener LA, McClure PW, Sennett BJ (2002) American shoulder and elbow surgeons standardized shoulder assessment form, patient self-report section: reliability, validity, and responsiveness. J Shoulder Elb Surg 6:11
Richards RR, An KN, Bigliani LU, Friedman RJ, Gartsman GM, Gristina AG, Iannotti JP, Mow VC, Sidles JA, Zuckerman JD (1994) A standardized method for the assessment of shoulder function. J Shoulder Elb Surg 3:71
Schmidt S, Ferrer M, González M, González N, Valderas JM, Alonso J, Escobar A, Vrotsou K, Montse F, Stefanie S, Olatz G, Gemma V, Angels P, Yolanda P, Gabriela B, Pere C, Carlos GF, Ana R, Virginia B, Ester V, Mireya GD, Sonia R, Oriol C, José María RR (2014) Evaluation of shoulder-specific patient-reported outcome measures: a systematic and standardized comparison of available evidence. J Shoulder Elb Surg 7:23
Rowe CR, Patel D, Southmayd WW (1978) The Bankart procedure. A long-term end-result study. J Bone Jt Surg Ser A 60:1–16
Unger RZ, Burnham JM, Gammon L, Malempati CS, Jacobs CA, Makhni EC (2019) The responsiveness of patient- reported outcome tools in shoulder surgery is dependent on the underlying pathological condition. Am J Sports Med 4:1778
Cr C, AH M (1987) A clinical method of functional assessment of the shoulder. Clin Orthop Relat Res 6:214
Bey MJ, Elders GJ, Huston LJ, Kuhn JE, Blasier RB, Soslowsky LJ (1998) The mechanism of creation of superior labrum, anterior, and posterior lesions in a dynamic biomechanical model of the shoulder: the role of inferior subluxation. J Shoulder Elb Surg 7:21
Clavert P, Bonnomet F, Kempf JF, Boutemy P, Braun M, Kahn JL (2004) Contribution to the study of the pathogenesis of type II superior labrum anterior-posterior lesions: a cadaveric model of a fall on the outstretched hand. J Shoulder Elb Surg 13:896
Familiari F, Huri G, Simonetta R, McFarland EG (2019) SLAP lesions: current controversies. EFORT Open Rev 4:1409
Shepard MF, Dugas JR, Zeng N, Andrews JR (2004) Differences in the ultimate strength of the biceps anchor and the generation of type II superior labral anterior posterior lesions in a cadaveric model. Am J Sports Med 5:32
Shah A, Judge A, Delmestri A, Edwards K, Arden NK, Prieto-Alhambra D, Holt TA, Pinedo-Villanueva RA, Hopewell S, Lamb SE, Rangan A, Carr AJ, Collins GS, Rees JL (2017) Incidence of shoulder dislocations in the UK, 1995–2015: a population-based cohort study. BMJ Open 5:6689
Pfahler M, Haraida S, Schulz C, Anetzberger H, Refior HJ, Bauer GS, Bigliani LU (2003) Age-related changes of the glenoid labrum in normal shoulders. J Shoulder Elb Surg 1:12
Hegedus EJ, Goode A, Campbell S, Morin A, Tamaddoni M, Moorman CT, Cook C (2008) Physical examination tests of the shoulder: a systematic review with meta-analysis of individual tests. Br J Sports Med 42:80–92
Hegedus EJ, Goode AP, Cook CE, Michener L, Myer CA, Myer DM, Wright AA (2012) Which physical examination tests provide clinicians with the most value when examining the shoulder? Update of a systematic review with meta-analysis of individual tests. Br J Sports Med 5:214
Sandrey MA (2013) Special physical examination tests for superior labrum anterior-posterior shoulder tears: an examination of clinical usefulness. J Athl Train 48:856
Bedi A, Allen AA (2008) Superior labral lesions anterior to posterior-evaluation and arthroscopic management. Clin Sports Med 2:7489
Antonio GE, Griffith JF, Yu AB, Yung PSH, Kai MC, Ahuja AT (2007) First-time shoulder dislocation: high prevalence of labral injury and age-related differences revealed by MR arthrography. J Magn Reson Imaging 26:478
Liu F, Cheng X, Dong J, Zhou D, Sun Q, Bai X, Wang D (2019) Imaging modality for measuring the presence and extent of the labral lesions of the shoulder: a systematic review and meta-analysis. BMC Musculoskelet Disord 6:7449
Amin MF, Youssef AO (2012) The diagnostic value of magnetic resonance arthrography of the shoulder in detection and grading of SLAP lesions: comparison with arthroscopic findings. Eur J Radiol 81:2343–2347
Mohana-Borges AVR, Chung CB, Resnick D (2003) Superior labral anteroposterior tear: classification and diagnosis on MRI and MR arthrography. Am J Roentgenol 4:996
Jia X, Yokota A, McCarty EC, Nicholson GP, Weber SC, McMahon PJ, Dunn WR, McFarland EG (2011) Reproducibility and reliability of the snyder classification of superior labral anterior posterior lesions among shoulder surgeons. Am J Sports Med 2:39
Ben KW, Sciascia A (2015) Current practice for the diagnosis of a SLAP lesion: systematic review and physician survey. Arthrosc J Arthrosc Relat Surg 5:140
Hester WA, O’Brien MJ, Heard WMR, Savoie FH (2018) Current concepts in the evaluation and management of type II superior labral lesions of the shoulder. Open Orthop J 5:12
Brockmeyer M, Tompkins M, Kohn DM, Lorbach O (2016) SLAP lesions: a treatment algorithm. Knee Surg Sport Traumatol Arthrosc 6:41
Buscayret F, Edwards TB, Szabo I, Adeleine P, Coudane H, Walch G (2017) Glenohumeral arthrosis in anterior instability before and after surgical treatment. Science 32:1165–1172
Marjanovic B, Poberaj B, Kolar M, Nabergoj M, Kopac C, Gosnik B, Merkac J, Mirnik N (2022) 11% complications rate after Latarjet procedure at up to 14 years follow-up. Musculoskelet Surg Musculoskelet Surg 106:227–237
Boileau P, Parratte S, Chuinard C, Roussanne Y, Shia D, Bicknell R (2009) Arthroscopic treatment of isolated type II slap lesions: Biceps tenodesis as an alternative to reinsertion. Am J Sports Med 37:929–936
Shin SJ, Lee J, Jeon YS, Ko YW, Kim RG (2017) Clinical outcomes of non-operative treatment for patients presenting SLAP lesions in diagnostic provocative tests and MR arthrography. Knee Surg Sport Traumatol Arthrosc 25:3296–3302
Stathellis A, Brilakis E, Georgoulis J-D, Antonogiannakis E, Georgoulis A (2018) Treatment of SLAP lesions. Open Orthop J 12:288–294
Wallace AL (2015) Shoulder arthroscopy, 3rd edn. Shoulder Elb, London
Funding
No founding was received for this study.
Author information
Authors and Affiliations
Contributions
Conceptualization was done by B.M.; methodology was done by B.M.; formal analysis was done by M.N., investigation was done by B.M and M.N, resources were done by B.M.; data curation was done by B.M., T.U., R.T., N.M and M.N., writing was done by B.M., T.U., N.M. and M.N., writing—review and editing were done by B.M. and M.N.; project administration was done by B.M. and N.M. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The operating surgeon B.M. is a consultant at the company Zimmer Biomet. Other authors have no competing interests to declare that are relevant to the content of this article.
Ethical approval
Approved 6/2021, by Orthopaedic Hospital Valdoltra Ethical committee.
Informed consent
Informed consent forms from the patients were obtained.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Marjanovič, B., Ušaj, T., Mirnik, N. et al. SLAP lesion type IX: case series and a review of literature. Eur J Orthop Surg Traumatol 33, 3337–3346 (2023). https://doi.org/10.1007/s00590-023-03547-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-023-03547-5