Abstract
Purpose
To define the rate of subsequent TKA following ACLR in a large US cohort and to identify factors that influence the risk of later undergoing TKA after ACLR.
Methods
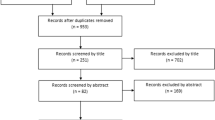
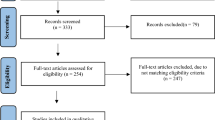
The California’s Office of Statewide Health Planning and Development (OSHPD) database was queried from 2000 to 2014 to identify patients who underwent primary ACLR (ACL group). An age-and gender-matched cohort that underwent appendectomy was selected as the control group. The cumulative incidence of TKA was calculated and ten-year survival was investigated using Kaplan-Meier analysis with failure defined as conversion to arthroplasty. Univariate and multivariate analyses were performed to explore the risk factors for conversion to TKA following ACLR.
Results
A total of 100,580 ACLR patients (mean age 34.48 years, 66.1%male) were matched to 100,545 patients from the general population. The ACL cohort had 1374 knee arthroplasty events; conversion rate was 0.71% at 2-year follow-up, 2.04% at 5-year follow-up, and 4.86% at 10-year follow-up. This conversion rate was higher than that of the control group at all time points, with an odds ratio of 3.44 (p<0.001) at 10-year follow-up. Decreasing survivorship following ACLR was observed with increasing age, female gender, and worker’s compensation insurance, while increased survivorship was found in patients of Hispanic and Asian Pacific Islander racial heritage and those who underwent concomitant meniscal repair.
Conclusions
In this US statewide study, the rate of TKA after ACLR is higher than reported elsewhere, with significantly increased odds when compared to a control group. Age, gender, concomitant knee procedures and other socioeconomic factors influence the rate of conversion to TKA following ACLR.



Similar content being viewed by others
References
Montgomery SR et al (2013) Surgical management of PCL injuries: indications, techniques, and outcomes. Curr Rev Musculoskelet Med 6(2):115–23
Houck DA et al (2019) Doctor, what happens after my anterior cruciate ligament reconstruction? J Bone Joint Surg Am 101(4):372–379
Sanders TL et al (2016) Incidence of anterior cruciate ligament Tears and reconstruction: A 21-year population-based study. Am J Sports Med 44(6):1502–7
Chalmers PN et al (2014) Does ACL reconstruction alter natural history?: a systematic literature review of long-term outcomes. J Bone Joint Surg Am 96(4):292–300
Spahn, G., et al., [The time-related risk for knee osteoarthritis after ACL injury. Results from a systematic review]. Orthopade, 2016. 45(1): p. 81-90
Chen, T., et al., Radiographic Osteoarthritis Prevalence Over Ten Years After Anterior Cruciate Ligament Reconstruction. Int J Sports Med, 2019
Lin SH et al (2017) Association of anterior cruciate ligament injury with knee osteoarthritis and total knee replacement: a retrospective cohort study from the Taiwan National Health Insurance Database. PLoS One 12(5):e0178292
Inacio MCS et al (2017) Projected increase in total knee arthroplasty in the United States - an alternative projection model. Osteoarthr Cartil 25(11):1797–1803
Leroux T et al (2014) The risk of knee arthroplasty following cruciate ligament reconstruction: a population-based matched cohort study. J Bone Joint Surg Am 96(1):2–10
Abram SGF et al (2019) Rates of knee arthroplasty in anterior cruciate ligament reconstructed patients: a longitudinal cohort study of 111,212 procedures over 20 years. Acta Orthopaedica 90:568–574
Lohmander LS et al (2007) The long-term consequence of anterior cruciate ligament and meniscus injuries: osteoarthritis. Am J Sports Med 35(10):1756–69
Watters TS et al (2017) Total knee arthroplasty after anterior cruciate ligament reconstruction: not just a routine primary arthroplasty. J Bone Joint Surg Am 99(3):185–189
Barenius B et al (2014) Increased risk of osteoarthritis after anterior cruciate ligament reconstruction: a 14-year follow-up study of a randomized controlled trial. Am J Sports Med 42(5):1049–57
Group, M.K., et al (2018) Ten-year outcomes and risk factors after anterior cruciate ligament reconstruction a MOON longitudinal prospective cohort study. Am J Sports Med, 46(4): 815-825
Finucane MM et al (2011) National, regional, and global trends in body-mass index since 1980: systematic analysis of health examination surveys and epidemiological studies with 960 country-years and 9.1 million participants. Lancet 377(9765):557–67
Kulkarni K et al (2016) Obesity and osteoarthritis. Maturitas 89:22–8
Wang T, He C (2018) Pro-inflammatory cytokines: the link between obesity and osteoarthritis. Cytokine Growth Factor Rev 44:38–50
Pomey MP et al (2017) Wait time management strategies for total joint replacement surgery: sustainability and unintended consequences. BMC Health Serv Res 17(1):629
Coyte PC et al (1994) Waiting times for knee-replacement surgery in the United States and Ontario. New England J Med 331(16):1068–1071
Siciliani L, Moran V, Borowitz M (2014) Measuring and comparing health care waiting times in OECD countries. Health Policy 118(3):292–303
Lyman S et al (2009) Epidemiology of anterior cruciate ligament reconstruction: trends, readmissions, and subsequent knee surgery. J Bone Joint Surg Am 91(10):2321–8
Sugimoto D et al (2016) Critical components of neuromuscular training to reduce ACL injury risk in female athletes: meta-regression analysis. Br J Sports Med 50(20):1259–1266
Singh N (2018) International epidemiology of anterior cruciate ligament injuries. Orthopedic Res Online J 1:94–6
Montalvo AM et al (2019) Anterior cruciate ligament injury risk in sport: a systematic review and meta-analysis of injury incidence by sex and sport classification. J Athl Train 54(5):472–482
Chechik O et al (2013) An international survey on anterior cruciate ligament reconstruction practices. Int Orthop 37(2):201–6
Chen T et al (2017) Long-term outcomes of anterior cruciate ligament reconstruction using either synthetics with remnant preservation or hamstring autografts: a 10-year longitudinal study. Am J Sports Med 45(12):2739–2750
Luc B, Gribble PA, Pietrosimone BG (2014) Osteoarthritis prevalence following anterior cruciate ligament reconstruction: a systematic review and numbers-needed-to-treat analysis. J Athl Train 49(6):806–19
Magnussen RA et al (2012) Total knee arthroplasty for secondary osteoarthritis following ACL reconstruction: a matched-pair comparative study of intra-operative and early post-operative complications. Knee 19(4):275–8
Grassi A et al (2017) What is the Mid-term failure rate of revision ACL reconstruction? a systematic review. Clin Orthop Relat Res 475(10):2484–2499
Yoshihara H, Yoneoka D (2014) Understanding the statistics and limitations of large database analyses. Spine 39(16):1311–1312
Acknowledgement
Authors would like to acknowledge. The Cappo Family Research Fund.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare they have no financial or non-financial interest.
Ethics approval
No ethics committee review was required due to the utilization of anonymous patient data from a publicly available national database.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bobman, J., Mayfield, C.K., Bolia, I.K. et al. Conversion rates and timing to total knee arthroplasty following anterior cruciate ligament reconstruction: a US population-based study. Eur J Orthop Surg Traumatol 32, 353–362 (2022). https://doi.org/10.1007/s00590-021-02966-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-021-02966-6