Abstract
Purpose
We aimed to 1) identify predictors of delayed and nonunion of tibial shaft fractures in patients treated with intramedullary nailing (IMN), including patient demographics and surgical factors, and 2) determine whether the nail/shaft ratio is associated with delayed and nonunion.
Methods
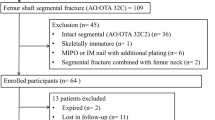
This retrospective, multicenter study included 315 patients with tibial shaft fracture treated with IMN between 2014 and 2019 and excluded patients with insufficient follow-up for 12 months, lost data and inadequate radiographs. Finally, we analyzed 258 patients (184 males; 74 females). Main outcome measurements were delayed union at 6 and nonunion at 12 months after surgery as determined on anteroposterior and lateral radiographs. We extracted the following as risk factors of delayed and nonunion: age, sex, BMI, fracture site, fracture type, injury energy, smoking history, and nail/shaft ratio. We conducted logistic regression analysis to investigate risk factors of delayed and nonunion using these extracted items as explanatory variables.
Results
Type C fracture was independently associated with delayed union (odds ratio 2.9, 95% confidential interval: 1.04–8.09, P = 0.04). Nail/shaft ratio was not an independent factor of delayed union. No independent explanatory factors were related to nonunion.
Conclusions
Type C fractures, which were unstable and fragmented, was associated with delayed union in tibia fractures treated with IMN, whereas nail thickness was not associated with delayed or nonunion fractures.


Similar content being viewed by others
Data availability
The datasets during and/or analyzed during the current study available from the corresponding author on reasonable request.
References
Court-Brown CM, Caesar B (2006) Epidemiology of adult fractures: a review. Injury 37:691–697
Busse JW, Morton E, Lacchetti C, Guyatt GH, Bhandari M (2008) Current management of tibial shaft fractures: a survey of 450 canadian orthopedic trauma surgeons. Acta Orthop 79:689–694
Audigé L, Griffin D, Bhandari M, Kellam J, Rüedi TP (2005) Path analysis of factors for delayed healing and nonunion in 416 operatively treated tibial shaft fractures. Clin Orthop Relat Res 438:221–232
Bhandari M, Tornetta P 3rd, Sprague S et al (2003) Predictors of reoperation following operative management of fractures of the tibial shaft. J Orthop Trauma 17:353–361
O’Halloran K, Coale M, Costales T et al (2016) Will my tibial fracture heal? Predicting nonunion at the time of definitive fixation based on commonly available variables. Clin Orthop Relat Res 474:1385–1395
Schmitz MA, Finnegan M, Natarajan R, Champine J (1999) Effect of smoking on tibial shaft fracture healing. Clin Orthop Relat Res 365:184–200. https://doi.org/10.1097/00003086-199908000-00024
Heppenstall RB, Brighton CT, Esterhai JL Jr, Muller G (1984) Prognostic factors in nonunion of the tibia: an evaluation of 185 cases treated with constant direct current. J Trauma 24:790–795
Donegan DJ, Akinleye S, Taylor RM, Baldwin K, Mehta S (2016) Intramedullary nailing of tibial shaft fractures: size matters. J Orthop Trauma 30:377–380
Rotondi NK, Beaton DE, Sujic R et al (2020) Factors associated with screening positive for high falls risk in fragility fracture patients: a cross-sectional study. BMC Musculoskelet Disord 21:372
Mauffrey C, McGuinness K, Parsons N et al (2012) A randomised pilot trial of “locking plate” fixation versus intramedullary nailing for extra-articular fractures of the distal tibia. J Bone Joint Surg Ser B 94(5):704–708
Müller ME, Nazarian S, Koch PJS (2012) The comprehensive classification of fractures of long bones. Springer
Meinberg EG, Agel J, Roberts CS, Karam MD, Kellam JF (2018) Fracture and dislocation classification compendium-2018. J Orthop Trauma 32(Suppl 1):S1–S170
Morris R, Pallister I, Trickett RW (2019) Measuring outcomes following tibial fracture. Injury 50:521–533
Kanda Y (2013) Investigation of the freely available easy-to-use software “EZR” for medical statistics. Bone Marrow Transpl 48:452–458
Karladani AH, Granhed H, Kärrholm J, Styf J (2001) The influence of fracture etiology and type on fracture healing: a review of 104 consecutive tibial shaft fractures. Arch Orthop Trauma Surg 121:325–328
Gaebler C, Berger U, Schandelmaier P et al (2001) Rates and odds ratios for complications in closed and open tibial fractures treated with unreamed, small diameter tibial nails: a multicenter analysis of 467 cases. J Orthop Trauma 15:415–423
Alemdaroğlu KB, Tiftikçi U, Iltar S et al (2009) Factors affecting the fracture healing in treatment of tibial shaft fractures with circular external fixator. Injury 40:1151–1156
Laigle M, Rony L, Pinet R, Lancigu R, Steiger V, Hubert L (2019) Intramedullary nailing for adult open tibial shaft fracture. an 85-case series. Orthop Traumatol Surg Res 105:1021–1024
Mundi R, Axelrod D, Heels-Ansdell D et al (2020) Nonunion in patients with tibial shaft fractures: Is early physical status associated with fracture healing? Cureus 12:e7649
Chan JK, Harry L, Williams G, Nanchahal J (2012) Soft-tissue reconstruction of open fractures of the lower limb: muscle versus fasciocutaneous flaps. Plast Reconstr Surg 130(2):284e–295e
Fischer MD, Gustilo RB, Varecka TF (1991) The timing of flap coverage, bone-grafting, and intramedullary nailing in patients who have a fracture of the tibial shaft with extensive soft-tissue injury. J Bone Joint Surg Ser A 73(9):1316–1322
Tornetta P III, Ricci WM, Ostrum RFM (2019) Rockwood and green’s fractures in adults, 9th edn. Lippincott Williams & Wilkins (LWW), Philadelphia
Kokubu T, Hak DJ, Hazelwood SJ, Reddi AH (2003) Development of an atrophic nonunion model and comparison to a closed healing fracture in rat femur. J Orthop Res 21(3):503–510
Högel F, Gerber C, Bühren V, Augat P (2013) Reamed intramedullary nailing of diaphyseal tibial fractures: comparison of compression and non-compression nailing. Eur J Trauma Emerg Surg 39(1):73–77
Drosos G, Karnezis IA, Bishay M, Miles AW (2001) Initial rotational stability of distal tibial fractures nailed without proximal locking: the importance of fracture type and degree of cortical contact. Injury 32(2):137–143
Henley MB (1989) Intramedullary devices for tibial fracture stabilization. Clin Orthop Relat Res 240:87–96
Gustilo RB, Gruninger RP, Davis T (1987) Classification of type III (severe) open fractures relative to treatment and results. Orthopedics 10(12):1781–1788
Ibrahim DA, Swenson A, Sassoon A, Fernando ND (2017) Classifications in brief: the tscherne classification of soft tissue injury. Clin Orthop Relat Res 475(2):560–564
Acknowledgements
We thank Taku Watanabe, Tomoki Fujita, Takayuki Fujita, Toshifumi Sato, Fumiki Kondo, Kosuke Bando and Susumu Imai for data collection.
Funding
There is no supporting funding.
Author information
Authors and Affiliations
Consortia
Contributions
YT and SI conceptualized. YT and RU oversaw the methodology. Formal analysis and investigation was conducted by RU and RS. NK wrote the original draft, YT has performed the editing and review. Data provided by the Hospitals team. SI supervised the research. YT and KT reviewed and edited the draft.
Corresponding author
Ethics declarations
Conflict of interest
The author(s) declare that they have no competing interests.
Consent for publication
All patients provided written informed for their data to be used.
Ethical approval
The approval number in our institute is 2020–0190.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The collaborators members of the Hospitals of Trauma Research of Nagoya (TRON) group are listed in “Appendix”.
Supplementary Information
Below is the link to the electronic supplementary material.
Appendix
Appendix
Member of the TRON (sown in alphabetical order of affiliation) are as follows; Dr. Takeshi Oguchi (Anjo Kosei Hospital), Dr. Yoshiharu Oka (Chubu Rosai Hospital), Dr. Tetsuro Takatsu(Gifu Prefectural Tajimi Hospital), Dr. Kazuyoshi Miyasaka (Handa City Hospital), Dr. Hiroyuki Matsubara (Hekinan Municipal Hospital), Dr. Hiroaki Kumagai (Nagoya Ekisaikai Hospital), Dr. Toshihiro Ando (Nagoya Daini Red Cross Hospital), Dr. Kenichi Yamauchi (Toyohashi Municipal Hospital), Dr. Yasuhide Kanayama (Toyota Kosei Hospital) and Dr. Tadahiro Sakai (TOYOTA memorial Hospital).
Rights and permissions
About this article
Cite this article
Kawasaki, N., Takegami, Y., Sakai, R. et al. Prediction of delayed union of tibial shaft fracture treated with intramedullary nailing: multicenter-study analysis and literature review -the TRON study. Eur J Orthop Surg Traumatol 32, 129–135 (2022). https://doi.org/10.1007/s00590-021-02939-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-021-02939-9