Abstract
Background
Some reports suggested that the status of the opposite-side hip affects clinical outcomes of unilateral total hip arthroplasty (THA) for hip osteoarthritis (HOA). This study aimed to determine whether unilateral THA could improve pain and movement of the non-operative hip.
Methods
The analysis included 195 patients divided into three groups according to contralateral hip status based on radiographic change assessed by Kellgren-Lawrence (KL) grade: normal hip (Group N: n = 124), HOA with KL grade > 2 (Group O: n = 39), and THA patients who already underwent THA in their opposite hip joint (Group T: n = 32). All patients were interviewed and examined preoperatively and at 1-year intervals after surgery. Hip function was evaluated with Harris Hip Score (HHS) and range of motion (ROM) preoperatively and at 1-year follow-up. We used the Japanese Orthopedic Association Hip-Disease Evaluation Questionnaire (JHEQ) and the Visual Analogue Scale (VAS) for separately evaluated right and left hip joints.
Results
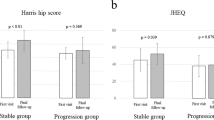
The mJHEQ movement, which indicated the activity, and flexion of ROM in the non-operative hip improved in group N and group T. The VAS and JHEQ pain values did not differ between preoperative and 1-year follow-up in all groups. In the operative side, HHS function, JHEQ movement values in group O were significantly lower than those of groups N and T at 1-year follow-up.
Conclusion
Unilateral THA may improve non-operative hip movement and active daily life except when the non-operated hip shows osteoarthritis. It did not improve non-operative hip pain, regardless of the condition on the other side. Clinical outcomes of unilateral THA may be affected by opposite hip status each other.


Similar content being viewed by others
Data availability
The datasets during and/or analyzed during the current study available from the corresponding author on reasonable request.
References
Amstutz HC, Le Duff MJ (2016) The natural history of osteoarthritis: What happens to the other hip? Clin Orthop Relat Res 474:1802–1809
Ritter MA, Carr K, Herbst SA, Eizember LE, Keating EM, Faris PM, Meding JB (1996) Outcome of the contralateral hip following total hip arthroplasty for osteoarthritis. J Arthroplasty 11:242–246
Matsumoto M, Baba T, Ochi H, Ozaki Y, Watari T, Homma Y, Kaneko K (2017) Influence of the contralateral hip state after total hip arthroplasty on patient-reported outcomes measured with the forgotten joint score-12. Eur J Orthop Surg Traumatol 27:929–936
Nilsdotter A-K, Petersson IF, Roos EM, Lohmander LS (2003) Predictors of patient relevant outcome after total hip replacement for osteoarthritis: a prospective study. Ann Rheum Dis 62:923–930
Aranda-Villalobos P, Fernández-De-Las-Peñas C, Navarro-Espigares JL et al (2013) Normalization of widespread pressure pain hypersensitivity after total hip replacement in patients with hip osteoarthritis is associated with clinical and functional improvements. Arthritis Rheum 65(5):1262–1270
Yoshii T, Jinno T, Morita S, Koga D, Matsubara M, Okawa A, Shinomiya K (2009) Postoperative hip motion and functional recovery after simultaneous bilateral total hip arthroplasty for bilateral osteoarthritis. J Orthop Sci 14:161–166
Kellgren JH, Lawrence JS (1957) Radiological assessment of osteo-arthrosis. Ann Rheum Dis 16:494–502. https://doi.org/10.1136/ard.16.4.494
Lane NE, Nevitt MC, Hochberg MC, Hung Y, Palermo L (2004) Progression of radiographic hip osteoarthritis over 8 years in a community sample of elderly white women. Arthritis Rheum 50:1477–1486
Harris WH (1969) Traumatic arthritis of the hip after dislocation and acetabular fractures: treatment by mold arthroplasty. An end-result study using a new method of result evaluation. J Bone Joint Surg Am 51:737–755
Osawa Y, Hasegawa Y, Seki T, Amano T, Higuchi Y, Ishiguro N (2016) Significantly poor outcomes of total hip arthroplasty after failed periacetabular osteotomy. J Arthroplasty 31:1904–1909
Matsumoto T, Kaneuji A, Hiejima Y, Sugiyama H, Akiyama H, Atsumi T, Ishii M, Izumi K, Ichiseki T, Ito H, Okawa T, Ohzono K, Otsuka H, Kishida S, Kobayashi S, Sawaguchi T, Sugano N, Nakajima I, Nakamura S, Hasegawa Y, Fukuda K, Fujii G, Mawatari T, Mori S, Yasunaga Y, Yamaguchi M (2012) Japanese orthopaedic association hip disease evaluation questionnaire (JHEQ): a patient-based evaluation tool for hip-joint disease. The subcommittee on hip disease evaluation of the clinical outcome committee of the japanese orthopaedic association. J Orthop Sci 17:25–38
Huskisson EC (1974) Measurement of pain. Lancet (London, England) 2:1127–1131
Seki T, Hasegawa Y, Ikeuchi K, Ishiguro N, Hiejima Y (2013) Reliability and validity of the Japanese orthopaedic association hip disease evaluation questionnaire (JHEQ) for patients with hip disease. J Orthop Sci 18:782–787
Kanda Y (2013) Investigation of the freely available easy-to-use software "EZR" for medical statistics. Bone Marrow Transplant 48:452–458
Bohannon RW, Gajdosik RL, LeVeau BF (1985) Relationship of pelvic and thigh motions during unilateral and bilateral hip flexion. Phys Ther 65:1501–1504
Pua YH, Wrigley TV, Cowan SM, Bennell KL (2009) Hip flexion range of motion and physical function in hip osteoarthritis: mediating effects of hip extensor strength and pain. Arthritis Care Res 61:633–640
Blikman T, Rienstra W, Van Raay JJAM, Dijkstra B, Bulstra SK, Stevens M, van den Akker-Scheek I (2018) Neuropathic-like symptoms and the association with joint-specific function and quality of life in patients with hip and knee osteoarthritis. PLoS ONE 13:1–14
Shigemura T, Ohtori S, Kishida S, Nakamura J, Takeshita M, Takazawa M, Harada Y, Takahashi K (2011) Neuropathic pain in patients with osteoarthritis of hip joint. Eur Orthop Traumatol 2:73
Amaro A, Amado F, Duarte JA, Appell H-J (2007) Gluteus medius muscle atrophy is related to contralateral and ipsilateral hip joint osteoarthritis. Int J Sports Med 28:1035–1039. https://doi.org/10.1055/s-2007-965078
Funding
None.
Author information
Authors and Affiliations
Contributions
YT designed the study, and wrote the initial draft of the manuscript. TS contributed to analysis and interpretation of data, and assisted in the preparation of the manuscript. All other authors have contributed to data collection and interpretation, and critically reviewed the manuscript. All authors approved the final version of the manuscript, and agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The approval number in our institute is 2018–0285-14658.
Consent to participate and publication
All patients provided written informed for their data to be used.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Takegami, Y., Seki, T., Osawa, Y. et al. Does unilateral total hip arthroplasty improve pain and function in the non-operative hip joint?. Eur J Orthop Surg Traumatol 30, 1411–1416 (2020). https://doi.org/10.1007/s00590-020-02716-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-020-02716-0