Abstract
Purpose
Acute compartment syndrome (ACS) is often difficult to diagnose in pediatric patients due to their erratic symptomatology. Therefore, it is of paramount importance to identify at-risk patients to facilitate a prompt diagnosis. This study aims to identify risk factors for the development of ACS in the pediatric population.
Methods
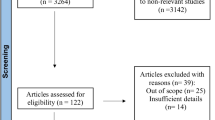
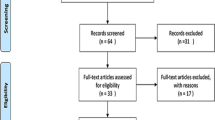
We included studies comprised of pediatric patients with traumatic ACS. We excluded studies evaluating compartment syndrome secondary to exertion, vascular insult, abdominal processes, burns, and snake bites. Heterogeneity was addressed by subgroup analysis, and whenever it remained significant, we utilized a random-effects meta-analysis for data pooling. The protocol has been registered at PROSPERO (ID = CRD42019126603).
Results
We included nine studies with 380,411 patients, of which 1144 patients were diagnosed with traumatic ACS. The average age was 10 years old, and 67% of patients were male. Factors that were significantly associated with ACS were: open radius/ulna fractures (OR 3.56 CI 1.52–8.33, p = 0.003), high-energy trauma (OR 3.51 CI 1.71–7.21, p = 0.001), humerus fractures occurring concurrently with forearm fractures (OR 3.49 CI 1.87–6.52, p < 0.001), open tibia fractures (OR 2.29 CI 1.47–3.55, p < 0.001), and male gender (OR 2.06 CI 1.70–2.51, p < 0.001).
Conclusion
In the present study, open fractures, high-energy trauma, concurrent humerus and forearm fractures, and male gender significantly increased the risk of developing ACS in the pediatric population. Clinicians should raise their suspicion for ACS when one or multiple of these factors are present in the right clinical context.
Type of study
Systematic review and meta-analysis.
Level of evidence
III.


Similar content being viewed by others
References
von Keudell AG, Weaver MJ, Appleton PT, Bae DS, Dyer GSM, Heng M, Jupiter JB, Vrahas MS (2015) Diagnosis and treatment of acute extremity compartment syndrome. Lancet 386(10000):1299–1310. https://doi.org/10.1016/S0140-6736(15)00277-9
Lin JS, Balch Samora J (2019) Pediatric acute compartment syndrome: a systematic review and meta-analysis. J Pediatr Orthop B. https://doi.org/10.1097/BPB.0000000000000593
Hak DJ (2019) Acute compartment syndrome in children. In: Mauffrey C, Hak DJ, Martin Iii MP (eds) Compartment syndrome: a guide to diagnosis and management. Springer, Cham, pp 125–132. https://doi.org/10.1007/978-3-030-22331-1_13
Via AG, Oliva F, Spoliti M, Maffulli N (2015) Acute compartment syndrome. Muscles Ligaments Tendons J 5(1):18–22
Heckman MM, Whitesides TE Jr, Grewe SR, Judd RL, Miller M, Lawrence JH 3rd (1993) Histologic determination of the ischemic threshold of muscle in the canine compartment syndrome model. J Orthop Trauma 7(3):199–210. https://doi.org/10.1097/00005131-199306000-00001
Garner MR, Taylor SA, Gausden E, Lyden JP (2014) Compartment syndrome: diagnosis, management, and unique concerns in the twenty-first century. HSS J 10(2):143–152. https://doi.org/10.1007/s11420-014-9386-8
Grottkau BE, Epps HR, Di Scala C (2005) Compartment syndrome in children and adolescents. J Pediatr Surg 40(4):678–682. https://doi.org/10.1016/j.jpedsurg.2004.12.007
Hosseinzadeh P, Talwalkar V, Powers J. Compartment Syndrome pediatric orthopaedic society of North America. https://posna.org/Physician-Education/Study-Guide/Compartment-Syndrome
Bae JM (2016) A suggestion for quality assessment in systematic reviews of observational studies in nutritional epidemiology. Epidemiol Health 38:e2016014. https://doi.org/10.4178/epih.e2016014
Hutton B, Salanti G, Caldwell DM, Chaimani A, Schmid CH, Cameron C, Ioannidis JP, Straus S, Thorlund K, Jansen JP, Mulrow C, Catala-Lopez F, Gotzsche PC, Dickersin K, Boutron I, Altman DG, Moher D (2015) The PRISMA extension statement for reporting of systematic reviews incorporating network meta-analyses of health care interventions: checklist and explanations. Ann Intern Med 162(11):777–784. https://doi.org/10.7326/M14-2385
Burns PB, Rohrich RJ, Chung KC (2011) The levels of evidence and their role in evidence-based medicine. Plast Reconstr Surg 128(1):305–310. https://doi.org/10.1097/PRS.0b013e318219c171
Dickersin K, Berlin JA (1992) Meta-analysis: state-of-the-science. Epidemiol Rev 14:154–176. https://doi.org/10.1093/oxfordjournals.epirev.a036084
Higgins JP, Thompson SG, Deeks JJ, Altman DG (2003) Measuring inconsistency in meta-analyses. BMJ 327(7414):557–560. https://doi.org/10.1136/bmj.327.7414.557
Begg CB, Mazumdar M (1994) Operating characteristics of a rank correlation test for publication bias. Biometrics 50(4):1088–1101
Mohamadi A, Chan JJ, Lian J, Wright CL, Marin AM, Rodriguez EK, von Keudell A, Nazarian A (2018) Risk factors and pooled rate of prolonged opioid use following trauma or surgery: a systematic review and meta-(regression) analysis. J Bone Joint Surg Am 100(15):1332–1340. https://doi.org/10.2106/JBJS.17.01239
Xu W, Tan L, Wang HF, Jiang T, Tan MS, Tan L, Zhao QF, Li JQ, Wang J, Yu JT (2015) Meta-analysis of modifiable risk factors for Alzheimer’s disease. J Neurol Neurosurg Psychiatry 86(12):1299–1306. https://doi.org/10.1136/jnnp-2015-310548
Blackman AJ, Wall LB, Keeler KA, Schoenecker PL, Luhmann SJ, O’Donnell JC, Gordon JE (2014) Acute compartment syndrome after intramedullary nailing of isolated radius and ulna fractures in children. J Pediatr Orthop 34(1):50–54. https://doi.org/10.1097/BPO.0b013e31829527de
Blakemore LC, Cooperman DR, Thompson GH, Wathey C, Ballock RT (2000) Compartment syndrome in ipsilateral humerus and forearm fractures in children. Clin Orthop Relat Res 376:32–38
Ferlic PW, Singer G, Kraus T, Eberl R (2012) The acute compartment syndrome following fractures of the lower leg in children. Injury 43(10):1743–1746. https://doi.org/10.1016/j.injury.2012.06.025
Harris LR, Arkader A, Broom A, Flynn J, Yellin J, Whitlock P, Miller A, Sawyer J, Roaten J, Skaggs DL, Choi PD (2019) Pulseless supracondylar humerus fracture with anterior interosseous nerve or median nerve injury-an absolute indication for open reduction? J Pediatr Orthop 39(1):E1–E7. https://doi.org/10.1097/bpo.0000000000001238
Robertson AK, Snow E, Browne TS, Brownell S, Inneh I, Hill JF (2018) Who gets compartment syndrome?: a retrospective analysis of the national and local incidence of compartment syndrome in patients with supracondylar humerus fractures. J Pediatr Orthop 38(5):e252–e256. https://doi.org/10.1097/bpo.0000000000001144
Sees JA, Cutler GJ, Ortega HW (2018) Risk factors for compartment syndrome in pediatric trauma patients. Pediatr Emerg Care. https://doi.org/10.1097/pec.0000000000001636
Shore BJ, Glotzbecker MP, Zurakowski D, Gelbard E, Hedequist DJ, Matheney TH (2013) Acute compartment syndrome in children and teenagers with tibial shaft fractures: incidence and multivariable risk factors. J Orthop Trauma 27(11):616–621. https://doi.org/10.1097/BOT.0b013e31828f949c
Villarreal ED, Wrenn JO, Sheffer BW, Sawyer JR, Spence DD, Kelly DM (2019) Do patient-specific or fracture-specific factors predict the development of acute compartment syndrome after pediatric tibial shaft fractures? J Pediatr Orthop. https://doi.org/10.1097/BPO.0000000000001410
Wind TC, Saunders SM, Barfield WR, Mooney JF 3rd, Hartsock LA (2012) Compartment syndrome after low-energy tibia fractures sustained during athletic competition. J Orthop Trauma 26(1):33–36. https://doi.org/10.1097/BOT.0b013e3182163367
McQueen MM, Gaston P, Court-Brown CM (2000) Acute compartment syndrome. Who is at risk? J Bone Joint Surg Br 82(2):200–203. https://doi.org/10.1302/0301-620x.82b2.9799
Joeris A, Lutz N, Wicki B, Slongo T, Audige L (2014) An epidemiological evaluation of pediatric long bone fractures—a retrospective cohort study of 2716 patients from two Swiss tertiary pediatric hospitals. BMC Pediatr 14:314. https://doi.org/10.1186/s12887-014-0314-3
Ortiz-Fullana J, Valentin P, Ramirez N (2016) Epidemiology of pediatric bone fractures across age groups: analysis of a pediatric population at an outpatient clinic in the Southwest region of Puerto Rico. Bol Asoc Med P R 108(2):51–56
Valerio G, Galle F, Mancusi C, Di Onofrio V, Colapietro M, Guida P, Liguori G (2010) Pattern of fractures across pediatric age groups: analysis of individual and lifestyle factors. BMC Public Health 10:656. https://doi.org/10.1186/1471-2458-10-656
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All of the authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mortensen, S.J., Orman, S., Testa, E.J. et al. Risk factors for developing acute compartment syndrome in the pediatric population: a systematic review and meta-analysis. Eur J Orthop Surg Traumatol 30, 839–844 (2020). https://doi.org/10.1007/s00590-020-02643-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-020-02643-0