Abstract
Background
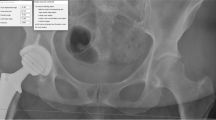
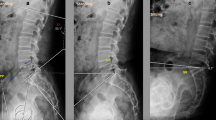
The purpose of this study was to conduct a prospective clinical trial to investigate the accuracy of an MRI-based patient-specific acetabular instrument guide during THA.
Methods
We conducted a prospective consecutive review of 14 hips in 14 patients who underwent primary THA with a posterolateral approach between September 2016 and February 2018. All preoperative planning and postoperative evaluations were completed on CT-based templating software. A pelvic MRI was taken to create a patient-specific surgical instrument guide. In order to assess the effect of increased experience on accuracy, we divided the cases into two groups according to when surgery was performed and investigated the absolute error in the acetabular component angle between preoperative planning and the postoperative state for each of the groups.
Results
We did not experience postoperative complications such as implant early dislocation in any of the cases. The absolute errors of acetabular implant angle using the patient-specific instrument guide were 3.7° ± 2.2° inclination and 4.5° ± 3.9° anteversion. The absolute error of the initial group was 4.7° ± 2.1° inclination and 6.1° ± 4.0° anteversion; for the later group, it was 2.8° ± 1.8° inclination and 3.2° ± 2.9° anteversion. There was a significant difference in the absolute error of acetabular implant placement between the initial group and the later group.
Conclusions
We believe this study shows that MRI-based patient-specific instrumentation may be a useful alternative to surgical tracking during THA once the slight learning curve has been overcome.





Similar content being viewed by others
References
Devane PA, Wraighte PJ, Ong DCG, Horne JG (2012) Do joint registries report true rates of hip dislocation? Clin Orthop Relat Res 470(11):3003–3006
Siebenrock KA, Kalbermatten DF, Ganz R (2003) Effect of pelvic tilt on acetabular retroversion: a study of pelves from cadavers. Clin Orthop Relat Res 407:241
Dorr LD, Wolf AW, Chandler R, Conaty JP (1983) Classification and treatment of dislocations of total hip arthroplasty. Clin Orthop Relat Res 173:151
Fackler CD, Poss R (1980) Dislocation in total hip arthroplasties. Clin Orthop Relat Res 151:169
Lewinnek GE, Lewis JL, Tarr R, Compere CL, Zimmerman JR (1978) Dislocations after total hip-replacement arthroplasties. J Bone Jt Surg Am 60:217
Widmer KH, Zurfluh B (2004) Compliant positioning of total hip components for optimal range of motion. J Orthop Res 22(4):815–821
Callanan MC, Jarrett B, Bragdon CR, Zurakowski D, Rubash HE, Freiberg AA, Malchau H (2011) The John Charnley award: risk factors for cup malpositioning: quality improvement through a joint registry at a tertiary hospital. Clin Orthop Relat Res 469(2):319–329
Grammatopoulos G, Pandit HG, da Assunção R, Taylor A, McLardy-Smith P, De Smet KA, Murray DW, Gill HS (2014) Pelvic position and movement during hip replacement. Bone Joint J 96-B(7):876–883
Inoue D, Kabata T, Maeda T, Kajino Y, Fujita K, Hasegawa K, Yamamoto T, Tsuchiya H (2015) Value of computed tomography-based three-dimensional surgical preoperative planning software in total hip arthroplasty with developmental dysplasia of the hip. J Orthop Sci 20(2):340–346
Kajino Y, Kabata T, Maeda T, Iwai S, Kuroda K, Tsuchiya H (2012) Does degree of the pelvic deformity affect the accuracy of computed tomography-based hip navigation? J Arthroplasty 27(9):1651–1657
Inaba Y, Kobayashi N, Ike H, Kubota S, Saito T (2016) The current status and future prospects of computer-assisted hip surgery. J Orthop Sci 21(2):107–115
Sugano N, Takao M, Sakai T, Nishii T, Miki H (2012) Does CT-based navigation improve the long-term survival in ceramic-on-ceramic THA? Clin Orthop Relat Res 470(11):3054–3059
Paprosky WG, Muir JM (2016) Intellijoint HIP®: a 3D mini-optical navigation tool for improving intraoperative accuracy during total hip arthroplasty. Med Devices (Auckl) 18(9):401–408
Hananouchi T, Saito M, Koyama T, Sugano N, Yoshikawa H (2010) Tailor-made surgical guide reduces incidence of outliers of cup placement. Clin Orthop Relat Res 468(4):1088–1095
Shandiz MA, MacKenzie JR, Hunt S, Anglin C (2014) Accuracy of an adjustable patient-specific guide for acetabular alignment in hip replacement surgery (Optihip). Proc Inst Mech Eng H 228(9):876–889
Small T, Krebs V, Molloy R, Bryan J, Klika AK, Barsoum WK (2014) Comparison of acetabular shell position using patient specific instruments versus standard surgical instruments: a randomized clinical trial. J Arthroplasty 29(5):1030–1037
Crowe JF, Mani VJ, Ranawat CS (1979) Total hip replacement in congenital dislocation and dysplasia of the hip. J Bone Joint Surg Am 61(1):15–23
Kajino Y, Kabata T, Maeda T, Iwai S, Kuroda K, Fujita K, Tsuchiya H (2013) Strict component positioning is necessary in hip resurfacing. J Orthop Sci. 18(2):290–297
Murray DW (1993) The definition and measurement of acetabular orientation. J Bone Joint Surg Br 75(2):228–232
Krismer M, Bauer R, Tschupik J, Mayrhofer P (1995) EBRA: a method to measure migration of acetabular components. J Biomech 28(10):1225–1236
Bosker BH, Verheyen CC, Horstmann WG, Tulp NJ (2007) Poor accuracy of freehand cup positioning during total hip arthroplasty. Arch Orthop Trauma Surg 127(5):375–379
Dorr LD, Malik A, Wan Z, Long WT, Harris M (2007) Precision and bias of imageless computer navigation and surgeon estimates for acetabular component position. Clin Orthop Relat Res 465:92–99
Kitada M, Nakamura N, Iwana D, Kakimoto A, Nishii T, Sugano N (2011) Evaluation of the accuracy of computed tomography-based navigation for femoral stem orientation and leg length discrepancy. J Arthroplasty 26(5):674–679
Spencer-Gardner L, Pierrepont J, Topham M, Baré J, McMahon S, Shimmin AJ (2016) Patient-specific instrumentation improves the accuracy of acetabular component placement in total hip arthroplasty. Bone Joint J 98-B(10):1342–1346
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The author(s) declare that they have no competing interests.
Ethical approval
All procedures performed in studies were in accordance with the ethical standards of our institutional ethical committee. In accordance with the requirements of this study, all patients were provided informed consent.
Rights and permissions
About this article
Cite this article
Inoue, D., Kabata, T., Kimura, H. et al. A prospective clinical trial to assess the accuracy of an MRI-based patient-specific acetabular instrument guide in total hip arthroplasty. Eur J Orthop Surg Traumatol 29, 65–71 (2019). https://doi.org/10.1007/s00590-018-2279-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00590-018-2279-7