Abstract
Purpose
This study aimed to investigate the trends in infectious spondylitis over the past two decades.
Methods
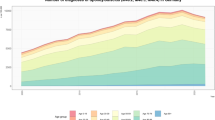
We included 157 cases, from 2000 to 2020, of infectious spondylitis. The cases were divided into two groups: 00 (cases during 2000–2009; 82 cases:) and 10 (cases during 2010–2020; 75 cases) groups. Patients’ age, sex, causative organism, and localization were examined and compared between the two groups.
Results
The proportions of women in the 00 and 10 groups were 30.5% and 38.7%, respectively, with no significant difference (P = 0.28). The average age was significantly higher in the 10 group (72.6 years) than in the 00 group (68.8 years; P < 0.01). A compromised host was the cause of infection in 52.4% and 36.0% of the patients in the 00 and 10 groups, respectively, showing a significant difference. The bacterial identification rates were 70.1% and 77.3% in the 00 and 10 groups, respectively (P < 0.01), and the genus Staphylococcus was the most common bacteria. The proportions of resistant bacteria such as methicillin-resistant Staphylococcus aureus in the 00 and 10 groups were 27.3% and 6.7%, respectively (P < 0.01). Conversely, infectious diseases caused by indigenous bacteria in the oral cavity and intestines were more common in the 10group (37.8%) than in the 00 group (13.0%), showing a significant difference (P < 0.01).
Conclusion
Recently, infections caused by indigenous bacteria in the oral cavity and intestines have increased more than those caused by resistant bacteria over the past two decade.




Similar content being viewed by others
Data availability
The data that support the findings of this study are available from the corresponding author, Shinji Tanishima, upon reasonable request.
References
Jensen AG, Espersen F, Skinhøj P, Rosdahl VT, Frimodt-Møller N (1997) Increasing frequency of vertebral osteomyelitis following Staphylococcus aureus bacteraemia in Denmark 1980–1990. J Infect 34:113–118. https://doi.org/10.1016/s0163-4453(97)92395-1
Mylona E, Samarkos M, Kakalou E, Fanourgiakis P, Skoutelis A (2009) Pyogenic vertebral osteomyelitis: a systematic review of clinical characteristics. Semin Arthritis Rheum 39:10–17. https://doi.org/10.1016/j.semarthrit.2008.03.002
Nagashima H, Yamane K, Nishi T, Nanjo Y, Teshima R (2010) Recent trends in spinal infections: retrospective analysis of patients treated during the past 50 years. Int Orthop 34:395–399. https://doi.org/10.1007/s00264-009-0741-1
Tsuzuki S, Matsunaga N, Yahara K, Gu Y, Hayakawa K, Hirabayashi A, Kajihara T, Sugai M, Shibayama K, Ohmagari N (2020) National trend of blood-stream infection attributable deaths caused by Staphylococcus aureus and Escherichia coli in Japan. J Infect Chemother 26:367–371. https://doi.org/10.1016/j.jiac.2019.10.017
Wyllie DH, Walker AS, Miller R, Moore C, Williamson SR, Schlackow I, Finney JM, O’Connor L, Peto TE, Crook DW (2011) Decline of meticillin-resistant Staphylococcus aureus in Oxfordshire hospitals is strain-specific and preceded infection-control intensification. BMJ Open 1:e000160. https://doi.org/10.1136/bmjopen-2011-000160
Iijima K, Arai H, Akishita M, Endo T, Ogasawara K, Kashihara N, Hayashi YK, Yumura W, Yokode M, Ouchi Y (2021) Toward the development of a vibrant, super-aged society: the future of medicine and society in Japan. Geriatr Gerontol Int 21:601–613. https://doi.org/10.1111/ggi.14201
Ota M, Hirao S, Uchimura K (2023) Age-period-cohort analysis on tuberculosis cases in Japan, 1953–2022. Int J Mycobacteriol 12:486–490. https://doi.org/10.4103/ijmy.ijmy_188_23
Hagiya H, Koyama T, Zamami Y, Minato Y, Tatebe Y, Mikami N, Teratani Y, Ohshima A, Shinomiya K, Kitamura Y, Sendo T, Hinotsu S, Tomono K, Kano MR (2018) Trends in incidence and mortality of tuberculosis in Japan: a population-based study, 1997–2016. Epidemiol Infect 147:e38. https://doi.org/10.1017/S095026881800290X
Tong SY, Davis JS, Eichenberger E, Holland TL, Fowler VG Jr (2015) Staphylococcus aureus infections: epidemiology, pathophysiology, clinical manifestations, and management. Clin Microbiol Rev 28:603–661. https://doi.org/10.1128/CMR.00134-14
Hassoun A, Linden PK, Friedman B (2017) Incidence, prevalence, and management of MRSA bacteremia across patient populations-a review of recent developments in MRSA management and treatment. Crit Care 21:211. https://doi.org/10.1186/s13054-017-1801-3
Allard C, Carignan A, Bergevin M, Boulais I, Tremblay V, Robichaud P, Duperval R, Pepin J (2008) Secular changes in incidence and mortality associated with Staphylococcus aureus bacteraemia in Quebec, Canada, 1991–2005. Clin Microbiol Infect 14:421–428. https://doi.org/10.1111/j.1469-0691.2008.01965.x
El Atrouni WI, Knoll BM, Lahr BD, Eckel-Passow JE, Sia IG, Baddour LM (2009) Temporal trends in the incidence of Staphylococcus aureus bacteremia in Olmsted county, Minnesota, 1998 to 2005: a population-based study. Clin Infect Dis 49:e130–e138. https://doi.org/10.1086/648442
Laupland KB, Ross T, Gregson DB (2008) Staphylococcus aureus bloodstream infections: risk factors, outcomes, and the influence of methicillin resistance in Calgary, Canada, 2000–2006. J Infect Dis 198:336–343. https://doi.org/10.1086/589717
Romagna A, Troeltzsch M, Birkenmaier C, Schwartz C, Suchorska B, Zausinger S (2018) Oral cavity infection: an underestimated source of pyogenic spondylodiscitis? J Neurol Surg A Cent Eur Neurosurg 79:218–223. https://doi.org/10.1055/s-0037-1608823
Nakamizo S, Egawa G, Honda T, Nakajima S, Belkaid Y, Kabashima K (2015) Commensal bacteria and cutaneous immunity. Semin Immunopathol 37:73–80. https://doi.org/10.1007/s00281-014-0452-6
Devine DA, Marsh PD, Meade J (2015) Modulation of host responses by oral commensal bacteria. J Oral Microbiol 7:26941. https://doi.org/10.3402/jom.v7.26941
Grönbeck Lindén I, Hägglin C, Gahnberg L, Andersson P (2017) Factors affecting older persons’ ability to manage oral hygiene: a qualitative study. JDR Clin Trans Res 2:223–232. https://doi.org/10.1177/2380084417709267
Morishita S, Watanabe Y, Ohara Y, Edahiro A, Sato E, Suga T, Hirano H (2016) Factors associated with older adults’ need for oral hygiene management by dental professionals. Geriatr Gerontol Int 16:956–962. https://doi.org/10.1111/ggi.12585
Klotz AL, Grill SK, Hassel AJ, Rammelsberg P, Ze Nthöfer A (2020) Differences between the oral health of people aged 50 and 70 years—an exploratory cohort study. Oral Health Prev Dent 18:239–243. https://doi.org/10.3290/j.ohpd.a43363
Sauer S, Kliem M (2010) Mass spectrometry tools for the classification and identification of bacteria. Nat Rev Microbiol 8:74–82. https://doi.org/10.1038/nrmicro2243
Lavigne JP, Espinal P, Dunyach-Remy C, Messad N, Pantel A, Sotto A (2013) Mass spectrometry: a revolution in clinical microbiology? Clin Chem Lab Med 51:257–270. https://doi.org/10.1515/cclm-2012-0291
Tatara Y, Niimura T, Mihara H (2020) Paraparesis and bilateral pulmonary abscesses secondary to pyogenic spondylodiscitis caused by Streptococcus anginosus Group bacteria. Spine Surg Relat Res 4:190–191. https://doi.org/10.22603/ssrr.2019-0069
Quast MB, Carr CM, Hooten WM (2017) Multilevel lumbar spine infection due to poor dentition in an immunocompetent adult: a case report. J Med Case Rep 11(1):328. https://doi.org/10.1186/s13256-017-1492-z
Berbari EF, Kanj SS, Kowalski TJ, Darouiche RO, Widmer AF, Schmitt SK, Hendershot EF, Holtom PD, Huddleston PM, Petermann GW, Osmon DR, Infectious Diseases Society of America (2015) 2015 Infectious diseases society of America (IDSA) clinical practice guidelines for the diagnosis and treatment of native vertebral osteomyelitis in adults. Clin Infect Dis 61:e26–e46. https://doi.org/10.1093/cid/civ482
Gordon AM, Ng MK, Erez O, Wong CH, Mont MA (2023) The importance of oral history: does dental implant placement or caries one year before or after primary total knee arthroplasty increase medical complications and periprosthetic joint infections? J Arthroplasty 38:476–483. https://doi.org/10.1016/j.arth.2022.10.013
Gouliouris T, Aliyu SH, Brown NM (2010) Spondylodiscitis: update on diagnosis and management. J Antimicrob Chemother 65(suppl 3):iii11–iii24. https://doi.org/10.1093/jac/dkq303
Nagashima H, Tanishima S, Tanida A (2018) Diagnosis and management of spinal infections. J Orthop Sci 23:8–13. https://doi.org/10.1016/j.jos.2017.09.016
Funding
This study doesn’t have any Fundings.
Author information
Authors and Affiliations
Contributions
S.T. designed the study, the main conceptual ideas, and the proof outline. C.T, T.M. and S.F and collected the data. T.M, C.T. and H.N. aided in interpreting the results and worked on the manuscript. H.N. supervised the project. S.T. wrote the manuscript with support from T.M. and C.T. All authors discussed the results and commented on the manuscript.
Corresponding author
Ethics declarations
Conflict of interests
There are no competing interests.
Ethics approval
The Ethics Committee of the Faculty of Medicine of Tottori University (approval No. 21A142).
Consent
We used the opt-out method to obtain consent from the patients to participate in this study. However, some patients died before the study. Hence, informed consent was not obtained. The Tottori University Ethics Committee has decided to exclude the data of the patients who died if the patients’ family refuses to provide consent based on the opt-out method. In fact, there were no cases waived by the families’ offer.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tanishima, S., Mihara, T., Takeda, C. et al. Trends in infectious spondylitis from 2000 to 2020. Eur Spine J (2024). https://doi.org/10.1007/s00586-024-08286-7
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1007/s00586-024-08286-7