Abstract
Background
Osteoporotic vertebral compression fractures affect a large number of elderly people and cause significant issues with pain and mobility. Percutaneous vertebroplasty (PVP) and kyphoplasty (PKP) are employed to treat those who remain symptomatic, with comparable clinical outcomes. Although PVP is faster and less expensive, concerns around cement-leakage complications make PKP perceptively safer.
Methods
By means of systematic review, we sought to ascertain whether PVP did carry a higher risk of cement-leakage and associated symptomatic complications (neural compromise, pulmonary embolism and need for emergency decompression surgery).
Results
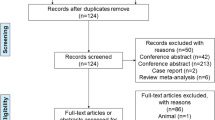
Our search of 138 articles returned six studies after shortlisting and manual review: three randomised-controlled trials, and three retrospective comparative studies which met our criteria and directly compared cement-leakage rates and complications between the two treatments. 532 PVPs and 493 PKPs recorded 213 (39.3%) and 143 (28.9%) leaks, respectively (p < 0.0005). Of these, no leaks resulted in any of the aforementioned leak-related complications. No meta-analysis was performed due to heterogeneity of the data.
Conclusions
We therefore concluded that whilst PVP does result in more cement leaks, this does not appear to be clinically significant. Further studies would add weight to this conclusion, and cost-effectiveness should be assessed to restore confidence in PVP.
Level of evidence
Level III Evidence.


Similar content being viewed by others
References
Melton LJ, Lane AW, Cooper C, Eastell R, O’Fallon WM, Riggs BL (1993) Prevalence and incidence of vertebral deformities. Osteoporos Int 3:113–119. https://doi.org/10.1007/BF01623271
Kanis JA, Kanis JA (1994) Assessment of fracture risk and its application to screening for postmenopausal osteoporosis: synopsis of a WHO report. Osteoporos Int 4:368–381. https://doi.org/10.1007/BF01622200
Edidin AA, Ong KL, Lau E, Kurtz SM (2011) Mortality risk for operated and nonoperated vertebral fracture patients in the medicare population. J Bone Miner Res 26:1617–1626. https://doi.org/10.1002/jbmr.353
Hofler RC, Jones GA (2020) Bracing for acute and subacute osteoporotic compression fractures: a systematic review of the literature. World Neurosurg 141:e453–e460. https://doi.org/10.1016/j.wneu.2020.05.199
Percutaneous vertebroplasty and percutaneous balloon kyphoplasty for treating osteoporotic vertebral compression fractures Technology appraisal guidance [TA279]. Published: 24 Apr 2013 www.nice.org.uk/guidance/ta279
Patel N, Jacobs D, John J, Fayed M, Nerusu L, Tandron M, Dailey W, Ayala R, Sibai N, Forrest P, Schwalb J, Aiyer R (2022) Balloon kyphoplasty versus vertebroplasty: a systematic review of height restoration in osteoporotic vertebral compression fractures. J Pain Res 15:1233–1245. https://doi.org/10.2147/JPR.S344191
Halvachizadeh S, Stalder AL, Bellut D, Hoppe S, Rossbach P, Cianfoni A, Schnake KJ, Mica L, Pfeifer R, Sprengel K, Pape HC (2021) Systematic review and meta-analysis of 3 treatment arms for vertebral compression fractures: a comparison of improvement in pain, adjacent-level fractures, and quality of life between vertebroplasty, kyphoplasty, and nonoperative management. JBJS Rev 9(10):34695056. https://doi.org/10.2106/JBJS.RVW.21.00045
Yeom JS, Kim WJ, Choy WS, Lee CK, Chang BS, Kang JW (2003) Leakage of cement in percutaneous transpedicular vertebroplasty for painful osteoporotic compression fractures. J Bone Joint Surg Br 85:83–89. https://doi.org/10.1302/0301-620x.85b1.13026
PROSPERO registration CD42022359178. https://www.crd.york.ac.uk/prospero/display_record.php?ID=CRD42022359178. Accessed 28 Sep 2022
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, Chou R, Glanville J, Grimshaw JM, Hróbjartsson A, Lalu MM, Li T, Loder EW, Mayo-Wilson E, McDonald S, McGuinness LA, Stewart LA, Thomas J, Tricco AC, Welch VA, Whiting P, Moher D (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 372:n71. https://doi.org/10.1136/bmj.n71
Campbell M, McKenzie JE, Sowden A, Katikireddi SV, Brennan SE, Ellis S, Hartmann-Boyce J, Ryan R, Shepperd S, Thomas J, Welch V, Thomson H (2020) Synthesis without meta-analysis (SWiM) in systematic reviews: reporting guideline. BMJ 368:l6890. https://doi.org/10.1136/bmj.l6890
Sterne JA, Hernán MA, Reeves BC, Savović J, Berkman ND, Viswanathan M, Henry D, Altman DG, Ansari MT, Boutron I, Carpenter JR, Chan A-W, Churchill R, Deeks JJ, Hróbjartsson A, Kirkham J, Jüni P, Loke YK, Pigott TD, Ramsay CR, Regidor D, Rothstein HR, Sandhu L, Santaguida PL, Schünemann HJ, Shea B, Shrier I, Tugwell P, Turner L, Valentine JC, Waddington H, Waters E, Wells GA, Whiting PF, Higgins JP (2016) ROBINS-I: a tool for assessing risk of bias in non-randomised studies of interventions. BMJ 355:i4919. https://doi.org/10.1136/bmj.i4919
Sterne JAC, Savović J, Page MJ, Elbers RG, Blencowe NS, Boutron I, Cates CJ, Cheng H-Y, Corbett MS, Eldridge SM, Emberson JR, Hernán MA, Hopewell S, Hróbjartsson A, Junqueira DR, Jüni P, Kirkham JJ, Lasserson T, Li T, McAleenan A, Reeves BC, Shepperd S, Shrier I, Stewart LA, Tilling K, White IR, Whiting PF, Higgins JPT (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366:l4898
Analyze a 2×2 contingency table. https://www.graphpad.com/quickcalcs/contingency1.cfm. Accessed 8 Nov 2022
Ding Y, Dong S, Wang J, Cui J, Cao Z, Lv S (2020) Comparison between hyperextension and neutral positions for vertebroplasty and kyphoplasty: which is best for osteoporotic vertebral compression fractures? J Pain Res 13:2509–2518. https://doi.org/10.2147/JPR.S268610
Wang F, Wang L-F, Miao D-C, Dong Z, Shen Y (2018) Which one is more effective for the treatment of very severe osteoporotic vertebral compression fractures: PVP or PKP? J Pain Res 11:2625–2631. https://doi.org/10.2147/JPR.S179022
Semaan H, Obri T, Bazerbashi M, Paull D, Liu X, Sarrouj M, Elgafy H (2018) Clinical outcome and subsequent sequelae of cement extravasation after percutaneous kyphoplasty and vertebroplasty: a comparative review. Acta radiol 59:861–868. https://doi.org/10.1177/0284185117732599
He C-J, Liu G-D (2018) Comparison of the efficacy and safety of bone-filling mesh container and simple percutaneous balloon kyphoplasty in the treatment of osteoporotic vertebral compression fractures. Pain Physician 21:259–268
Wang C-H, Ma J-Z, Zhang C-C, Nie L (2015) Comparison of high-viscosity cement vertebroplasty and balloon kyphoplasty for the treatment of osteoporotic vertebral compression fractures. Pain Physician 18:E187–E194
Vogl TJ, Pflugmacher R, Hierholzer J, Stender G, Gounis M, Wakhloo A, Fiebig C, Hammerstingl R (2013) Cement directed kyphoplasty reduces cement leakage as compared with vertebroplasty: results of a controlled, randomized trial. Spine 38:1730–1736. https://doi.org/10.1097/BRS.0b013e3182a14d15
Gu CN, Brinjikji W, Evans AJ, Murad MH, Kallmes DF (2016) Outcomes of vertebroplasty compared with kyphoplasty: a systematic review and meta-analysis. J Neurointerv Surg 8:636–642. https://doi.org/10.1136/neurintsurg-2015-011714
Funding
The study did not receive any funding which needs to be declared, and none of the authors have any financial interests in this subject matter.
Author information
Authors and Affiliations
Contributions
LR: Made substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data; or the creation of new software used in the work. Drafted the work or revised it critically for important intellectual content. Approved the version to be published. Agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
None of the authors have any conflicts of interest or competing interests to declare with this manuscript.
Ethical approval
No ethical approval was required for this study, as it was retrospectively collected clinical data.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Rose, L.D., Bateman, G. & Ahmed, A. Clinical significance of cement leakage in kyphoplasty and vertebroplasty: a systematic review. Eur Spine J 33, 1484–1489 (2024). https://doi.org/10.1007/s00586-023-08026-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-023-08026-3