Abstract
Introduction
Proximal junctional kyphosis (PJK) is one of the most common complications after thoracic AIS surgery. Previous studies reported that the etiology of PJK was associated with osteopenia and meanwhile the AIS patients were found osteopenia which could persist into adulthood. Recently, an MRI-based vertebral bone quality score (VBQ) was reported to be a promising tool which can assess preoperative bone quality.
Objective
This study aims to evaluate the utility of VBQ score in predicting PJK after corrective surgery for thoracic AIS (Lenke 1 and 2).
Methods
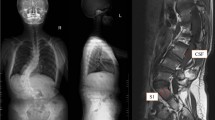
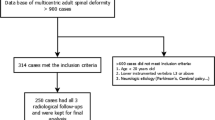
We conducted a retrospective study to identify the predictive efficiency of VBQ score for PJK in thoracic AIS patients. Demographic, radiographic parameters, and surgical variables were collected. VBQ score was calculated using preoperative T1-weighted MRI. Univariate analysis, linear regression, and multivariate logistic regression were performed to determine potential risk factors of PJK and correlation between other parameters and VBQ score. Receiver operating characteristic analysis and area under the curve values were utilized to evaluate the predictive efficiency of VBQ score for PJK.
Results
A total of 206 patients (aged 14.4 ± 2.3 years) were included, of which 33 (16.0%) developed PJK. VBQ scores were significantly different between the PJK and non-PJK groups (2.8 ± 0.2 vs 2.5 ± 0.2, P < 0.01). A significant positive correlation was found between VBQ score and PJA (R2 = 0.1728, P < 0.01).On multivariate analysis, VBQ score was the only significant predictor of PJK (odds ratio = 2.178, 95% CI = 1.644–2.885, P < 0.001), with a predictive accuracy of 83%.
Conclusion
Higher VBQ scores were independently associated with PJK occurrence after corrective surgery for thoracic AIS. Preoperative measurement of VBQ score on MRI may serve as a valuable tool in planning thoracic AIS surgery.




Similar content being viewed by others
Data availability
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Al-Mohrej OA, Aldakhil SS, Al-Rabiah MA, Al-Rabiah AM (2012) Surgical treatment of adolescent idiopathic scoliosis: complications. Annal Med Surg 2020(52):19–23. https://doi.org/10.1016/j.amsu.2020.02.004
Cerpa M, Sardar Z, Lenke L (2020) Revision surgery in proximal junctional kyphosis. Eur Spine J 29(Suppl 1):78–85. https://doi.org/10.1007/s00586-020-06320-y
Kuo CC, Soliman MAR, Aguirre AO, Ruggiero N, Kruk M, Khan A et al (2022) Vertebral bone quality score independently predicts proximal junctional kyphosis and/or failure after adult spinal deformity surgery. Neurosurgery. https://doi.org/10.1227/neu.0000000000002291
Yu WS, Chan KY, Yu FW, Yeung HY, Ng BK, Lee KM et al (2013) Abnormal bone quality versus low bone mineral density in adolescent idiopathic scoliosis: a case-control study with in vivo high-resolution peripheral quantitative computed tomography. Spine J 13(11):1493–1499. https://doi.org/10.1016/j.spinee.2013.05.018
Lam TP, Yang G, Pang H, Yip B, Lee W, Hung A et al (2021) A six years longitudinal cohort study on the changes in bone density and bone quality up to peak bone mass in adolescent idiopathic scoliosis (AIS) with and without 2 years of Calcium and Vit-D supplementation. Stud Health Technol Inf 280:31–34. https://doi.org/10.3233/shti210429
Kono H, Machida M, Saito M, Nishiwaki Y, Kato H, Hosogane N et al (2011) Mechanism of osteoporosis in adolescent idiopathic scoliosis: experimental scoliosis in pinealectomized chickens. J Pineal Res 51(4):387–393. https://doi.org/10.1111/j.1600-079X.2011.00901.x
Sawicki P, Tałałaj M, Życińska K, Zgliczyński WS, Wierzba W (2021) Current applications and selected technical details of dual-energy X-Ray absorptiometry. Med Sci Monitor 27:e930839. https://doi.org/10.12659/msm.930839
Tang GY, Lv ZW, Tang RB, Liu Y, Peng YF, Li W et al (2010) Evaluation of MR spectroscopy and diffusion-weighted MRI in detecting bone marrow changes in postmenopausal women with osteoporosis. Clin Rad 65(5):377–381. https://doi.org/10.1016/j.crad.2009.12.011
Shen W, Chen J, Punyanitya M, Shapses S, Heshka S, Heymsfield SB (2007) MRI-measured bone marrow adipose tissue is inversely related to DXA-measured bone mineral in Caucasian women. Osteoporosis Int 18(5):641–647. https://doi.org/10.1007/s00198-006-0285-9
Shen W, Scherzer R, Gantz M, Chen J, Punyanitya M, Lewis CE et al (2012) Relationship between MRI-measured bone marrow adipose tissue and hip and spine bone mineral density in AfricanAmerican and Caucasian participants: the CARDIA study. J Clinl Endocrinol Metabol 97(4):1337–1346. https://doi.org/10.1210/jc.2011-2605
Ehresman J, Pennington Z, Schilling A, Lubelski D, Ahmed AK, Cottrill E et al (2020) Novel MRI-based score for assessment of bone density in operative spine patients. Spine J 20(4):556–562. https://doi.org/10.1016/j.spinee.2019.10.018
Zhong J, Cao K, Wang B, Li H, Zhou X, Xu X et al (2019) Incidence and risk factors for proximal junctional kyphosis in adolescent idiopathic scoliosis after correction surgery: a meta-analysis. World Neurosurgery 125:e326–e335. https://doi.org/10.1016/j.wneu.2019.01.072
Ferrero E, Bocahut N, Lefevre Y, Roussouly P, Pesenti S, Lakhal W et al (2018) Proximal junctional kyphosis in thoracic adolescent idiopathic scoliosis: risk factors and compensatory mechanisms in a multicenter national cohort. Eur Spine J 27(9):2241–2250. https://doi.org/10.1007/s00586-018-5640-y
Boeckenfoerde K, Schulze Boevingloh A, Gosheger G, Bockholt S, Lampe LP, Lange T (2022) Risk factors of proximal junctional kyphosis in adolescent idiopathic scoliosis-the spinous processes and proximal rod contouring. J Clin Med 11(20):11206098. https://doi.org/10.3390/jcm11206098
Lee J, Park YS (2016) Proximal junctional kyphosis: diagnosis, pathogenesis, and treatment. Asian Spine J 10(3):593–600. https://doi.org/10.4184/asj.2016.10.3.593
Lonner BS, Ren Y, Newton PO, Shah SA, Samdani AF, Shufflebarger HL et al (2017) Risk factors of proximal junctional kyphosis in adolescent idiopathic scoliosis-the pelvis and other considerations. Spine Deformity 5(3):181–188. https://doi.org/10.1016/j.jspd.2016.10.003
Tambe AD, Panikkar SJ, Millner PA, Tsirikos AI (2018) Current concepts in the surgical management of adolescent idiopathic scoliosis. Bone Joint J 100b(4):415–424. https://doi.org/10.1302/0301-620x.100b4.Bjj-2017-0846.R2
Pahys JM, Vivas AC, Samdani AF, Cunn G, Betz RR, Newton PO et al (2018) Assessment of proximal junctional kyphosis and shoulder balance with proximal screws versus hooks in posterior spinal fusion for adolescent idiopathic scoliosis. Spine 43(22):e1322–e1328. https://doi.org/10.1097/brs.0000000000002700
Tamai K, Terai H, Suzuki A, Nakamura H, Watanabe K, Katsumi K et al (2019) Risk factors for proximal junctional fracture following fusion surgery for osteoporotic vertebral collapse with delayed neurological deficits: a retrospective cohort study of 403 patients. Spine Surg Related Res 3(2):171–177. https://doi.org/10.22603/ssrr.2018-0068
Mikula AL, Lakomkin N, Pennington Z, Pinter ZW, Nassr A, Freedman B et al (2022) Association between lower Hounsfield units and proximal junctional kyphosis and failure at the upper thoracic spine. J Neurosurg Spine 2022:1–9. https://doi.org/10.3171/2022.3.Spine22197
Razzouk J, Ramos O, Ouro-Rodrigues E, Samayoa C, Wycliffe N, Cheng W et al (2023) Comparison of cervical, thoracic, and lumbar vertebral bone quality scores for increased utility of bone mineral density screening. Eur Spine J 32(1):20–26. https://doi.org/10.1007/s00586-022-07484-5
Kuo CC, Soliman MAR, Aguirre AO, Ruggiero N, Kruk M, Khan A et al (2023) Vertebral bone quality score independently predicts proximal junctional kyphosis and/or failure after adult spinal deformity surgery. Neurosurgery 92(5):945–954. https://doi.org/10.1227/neu.0000000000002291
Clément JL, Pesenti S, Ilharreborde B, Morin C, Charles YP, Parent HF et al (2021) Proximal junctional kyphosis is a rebalancing spinal phenomenon due to insufficient postoperative thoracic kyphosis after adolescent idiopathic scoliosis surgery. Eur Spine J 30(7):1988–1997. https://doi.org/10.1007/s00586-021-06875-4
Shariatzadeh H, Modaghegh BS, Mirzaei A (2017) the effect of dynamic hyperextension brace on osteoporosis and hyperkyphosis reduction in postmenopausal osteoporotic women. Arch Bone Joint Surg 5(3):181–185
Acknowledgements
Not applicable.
Funding
This study was supported in part by the Projects of the Science & Technology Department of Sichuan Province (2022ZDZX0029 and 2021YFS0218), the National Natural Science Foundation of China (81871772; 82172495; 82072434 and 82272546), and the 1·3·5 project for disciplines of excellence–Clinical Research Incubation Project, West China Hospital, Sichuan University (2021HXFH003).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no competing interests.
Ethical approval
This study was approved by the Ethics Committee of the West China Hospital. The participant consent was written and was performed in accordance with the ethical standards of the Declaration of Helsinki.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, J., Chen, Q., Ai, Y. et al. Vertebral bone quality score as a novel predictor of proximal junctional kyphosis after thoracic adolescent idiopathic scoliosis surgery. Eur Spine J 32, 3996–4002 (2023). https://doi.org/10.1007/s00586-023-07894-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-023-07894-z