Abstract
Purpose
Patients with diffuse idiopathic skeletal hyperostosis (DISH) that extends to the lumbar segments (L-DISH) have a high risk of further surgery after lumbar decompression. However, few studies have focused on the ankylosis status of the residual caudal segments, including the sacroiliac joint (SIJ). We hypothesized that patients with more ankylosed segments beside the operated level, including the SIJ, would be at a higher risk of further surgery.
Methods
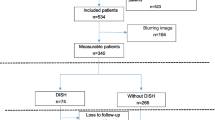
A total of 79 patients with L-DISH who underwent decompression surgery for lumbar stenosis at a single academic institution between 2007 and 2021 were enrolled. The baseline demographics and radiological findings by CT imaging focusing on the ankylosing condition of the residual lumbar segments and SIJ were collected. Cox proportional hazard analysis was conducted to investigate the risk factors for further surgery after lumbar decompression.
Results
The rate of further surgery was 37.9% during an average of 48.8 months of follow-up. Cox proportional hazard analysis demonstrated that the presence of fewer than three segments of non-operated mobile caudal segments was an independent predictor for further surgery (including both the same and adjacent levels) after lumbar decompression (adjusted hazard ratio 2.53, 95%CI [1.12–5.70]).
Conclusions
L-DISH patients with fewer than three mobile caudal segments besides index decompression levels are at a high risk of further surgery. Ankylosis status of the residual lumbar segments and SIJ should be thoroughly evaluated using CT during preoperative planning.





Similar content being viewed by others
References
Forestier J, Rotes-Querol J (1950) Senile ankylosing hyperostosis of the spine. Ann Rheum Dis 9:321–330. https://doi.org/10.1136/ard.9.4.321
Resnick D, Niwayama G (1976) Radiographic and pathologic features of spinal involvement in diffuse idiopathic skeletal hyperostosis (DISH). Radiology 119:559–568. https://doi.org/10.1148/119.3.559
Uehara M, Takahashi J, Ikegami S, Tokida R, Nishimura H, Sakai N, Kato H (2020) Prevalence of diffuse idiopathic skeletal hyperostosis in the general elderly population: a Japanese cohort survey randomly sampled from a basic resident registry. Clin Spine Surg 33:123–127. https://doi.org/10.1097/bsd.0000000000000919
Yamada K, Satoh S, Abe Y, Yanagibashi Y, Hyakumachi T, Masuda T (2018) Diffuse idiopathic skeletal hyperostosis extended to the lumbar segment is a risk factor of reoperation in patients treated surgically for lumbar stenosis. Spine 43:1446–1453. https://doi.org/10.1097/brs.0000000000002618
Otsuki B, Fujibayashi S, Tanida S, Shimizu T, Lyman S, Matsuda S (2019) Outcomes of lumbar decompression surgery in patients with diffuse idiopathic skeletal hyperostosis (DISH). J Orthop Sci Off J Jpn Orthop Assoc 24:957–962. https://doi.org/10.1016/j.jos.2019.09.003
Yahara Y, Yasuda T, Kawaguchi Y, Suzuki K, Seki S, Kondo M, Makino H, Kamei K, Kanamori M, Kimura T (2020) Sacroiliac joint variation associated with diffuse idiopathic skeletal hyperostosis. BMC Musculoskelet Disord 21:93. https://doi.org/10.1186/s12891-020-3105-z
Leibushor N, Slonimsky E, Aharoni D, Lidar M, Eshed I (2017) CT abnormalities in the sacroiliac joints of patients with diffuse idiopathic skeletal hyperostosis. AJR Am J Roentgenol 208:834–837. https://doi.org/10.2214/ajr.16.16994
Watanabe K, Matsumoto M, Ikegami T, Nishiwaki Y, Tsuji T, Ishii K, Ogawa Y, Takaishi H, Nakamura M, Toyama Y, Chiba K (2011) Reduced postoperative wound pain after lumbar spinous process-splitting laminectomy for lumbar canal stenosis: a randomized controlled study. J Neurosurg Spine 14:51–58. https://doi.org/10.3171/2010.9.Spine09933
Kellgren JH, Lawrence JS (1957) Radiological assessment of osteo-arthrosis. Ann Rheum Dis 16:494–502. https://doi.org/10.1136/ard.16.4.494
Mata S, Chhem RK, Fortin PR, Joseph L, Esdaile JM (1998) Comprehensive radiographic evaluation of diffuse idiopathic skeletal hyperostosis: development and interrater reliability of a scoring system. Semin Arthritis Rheum 28:88–96. https://doi.org/10.1016/s0049-0172(98)80041-3
Otsuki B, Fujibayashi S, Takemoto M, Kimura H, Shimizu T, Matsuda S (2015) Diffuse idiopathic skeletal hyperostosis (DISH) is a risk factor for further surgery in short-segment lumbar interbody fusion. Eur Spine J 24:2514–2519. https://doi.org/10.1007/s00586-014-3603-5
Yamada K, Abe Y, Yanagibashi Y, Hyakumachi T, Nakamura H (2021) Risk factors for reoperation at same level after decompression surgery for lumbar spinal stenosis in patients with diffuse idiopathic skeletal hyperostosis extended to the lumbar segments. Spine Surg Relat Res 5:381–389. https://doi.org/10.22603/ssrr.2020-0227
Okada E, Yagi M, Fujita N, Suzuki S, Tsuji O, Nagoshi N, Nakamura M, Matsumoto M, Watanabe K (2019) Lumbar spinal canal stenosis in patients with diffuse idiopathic skeletal hyperostosis: surgical outcomes after posterior decompression surgery without spinal instrumentation. J Orthop Sci 24:999–1004. https://doi.org/10.1016/j.jos.2019.08.010
Habibi H, Toyoda H, Terai H, Yamada K, Hoshino M, Suzuki A, Takahashi S, Tamai K, Salimi H, Hori Y, Yabu A, Nakamura H (2022) Incidence of postoperative progressive segment degeneration at decompression and adjacent segments after minimally invasive lumbar decompression surgery: a 5-year follow-up study. J Neurosurg Spine 37:1–8. https://doi.org/10.3171/2021.12.Spine211151
Yokoyama K, Yamada M, Tanaka H, Ito Y, Sugie A, Wanibuchi M, Kawanishi M (2020) Factors of adjacent segment disease onset after microsurgical decompression for lumbar spinal canal stenosis. World Neurosurg 144:e110–e118. https://doi.org/10.1016/j.wneu.2020.08.012
Bydon M, Macki M, De la Garza-Ramos R, McGovern K, Sciubba DM, Wolinsky JP, Witham TF, Gokaslan ZL, Bydon A (2016) Incidence of adjacent segment disease requiring reoperation after lumbar laminectomy without fusion: a study of 398 patients. Neurosurgery 78:192–199. https://doi.org/10.1227/neu.0000000000001007
Nagamoto Y, Iwasaki M, Sakaura H, Sugiura T, Fujimori T, Matsuo Y, Kashii M, Murase T, Yoshikawa H, Sugamoto K (2015) Sacroiliac joint motion in patients with degenerative lumbar spine disorders. J Neurosurg Spine 23:209–216. https://doi.org/10.3171/2014.12.Spine14590
Asada M, Tokunaga D, Arai Y, Oda R, Fujiwara H, Yamada K, Kubo T (2019) Degeneration of the sacroiliac joint in hip osteoarthritis patients: a three-dimensional image analysis. J Belgian Soc Radiol 103:36. https://doi.org/10.5334/jbsr.1648
Nakajima H, Watanabe S, Honjoh K, Kubota A, Matsumine A (2021) Pathomechanism and prevention of further surgery after posterior decompression for lumbar spinal canal stenosis in patients with diffuse idiopathic skeletal hyperostosis. Spine J 21:955–962. https://doi.org/10.1016/j.spinee.2021.01.009
Funding
No funds were received in support of this work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial connections relevant to this work.
Ethical approval
This study was approved by the institutional review board of Kyoto University (IRB #R2901). This manuscript does not contain information about medical devices/drugs.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Tanaka, A., Shimizu, T., Kawai, T. et al. Risk of further surgery after decompression in patients with diffuse idiopathic skeletal hyperostosis extending to the lumbar segments: focus on the number of residual lumbar/lumbosacral and sacroiliac mobile segments. Eur Spine J 32, 2336–2343 (2023). https://doi.org/10.1007/s00586-023-07773-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-023-07773-7