Abstract
Purpose
In this work, a two-center study was performed to study the clinical presentation of cervical spine fractures in ankylosing spondylitis (AS) patients and assess the surgical management of these fractures.
Methods
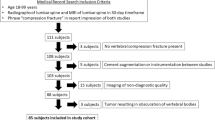
A retrospective analysis of prospectively collected data in two level-1 spine surgery centers was performed. Both spine centers have a standard database for all admitted patients. Inclusion criteria were surgically treated AS with cervical spine fracture diagnosis (from C1 to Th3) and postoperative follow-up minimum of 12 months.
Results
One hundred ten patients (105 male/5 female) were included. The mean age was 62 ± 10 years. The mean time between trauma and surgery was 49 ± 42 days. There was a history of mild trauma in 72 patients (65.4%). The clinical presentation was a pain in all patients. Twenty-seven (24.6%) had a neurological deficit at admission. The most common fracture level was C6/7 in 63 patients (57.23%). The VAS was 7 ± 1, and NDI was 34 ± 8 in the preoperative assessment. The mean preoperative kyphosis angle was 48 ± 26° between C2 and C7.
Positioning and preparing of the patients on the operation table took a mean of 57 ± 28 min. The surgical approach was dorsal in 59 patients (53.6%), combined in 45 patients (40.9%), and ventral in 6 patients (6,5%). The mean number of the fixed levels was 6 ± 2 levels.
Intraoperative complications occurred in 9 patients (8.2%). Postoperative Cobb angle improved to a mean of 17 ± 9 degrees. Neurological improvement occurred in 20/27 patients. In 12 patients, the recovery was complete. The mean postoperative follow-up was 46 ± 18 months. VAS improved to 3 ± 1, and NDI improved to 14 ± 6 at the last postoperative visit. The improvement was clinically significant (p = 0.01 and 0.00, respectively).
Conclusion
High suspicion of cervical spine fractures is necessary for patients with AS. CT and MRI images are necessary to rule out cervical spine fractures in AS patients, especially to detect occult fractures. Surgical treatment is safe, and the posterior approach with long-segment fusion is the approach of choice in this group of patients.




Similar content being viewed by others
References
Smith JA (2015) Update on ankylosing spondylitis: current concepts in pathogenesis. Curr Allergy Asthma Rep. https://doi.org/10.1007/s11882-014-0489-6
Golder V, Schachna L (2013) Ankylosing spondylitis: An update. Aust. Fam. Physician
Etame AB, Than KD, Wang AC et al (2008) Surgical management of symptomatic cervical or cervicothoracic kyphosis due to ankylosing spondylitis. Spine Phila Pa 1976. https://doi.org/10.1097/BRS.0b013e31817c6c64
Lazennec JY, d’Astorg H, Rousseau MA (2015) Cervical spine surgery in ankylosing spondylitis: Review and current concept. Orthop Traumatol Surg Res. https://doi.org/10.1016/j.otsr.2015.02.005
von der Höh NH, Henkelmann J, Jarvers JS et al (2020) Magnetic resonance tomography for the early detection of occult fractures of the spinal column in patients with ankylosing spondylitis. Eur spine J. https://doi.org/10.1007/s00586-020-06309-7
Hartmann S, Tschugg A, Wipplinger C, Thomé C (2017) Analysis of the literature on cervical spine fractures in ankylosing spinal disorders. Glob spine J. https://doi.org/10.1177/2192568217700108
Caron T, Bransford R, Nguyen Q, et al (2010) Spine fractures in patients with ankylosing spinal disorders. Spine (Phila. Pa. 1976).
Prieto-Alhambra D, Muñoz-Ortego J, De Vries F et al (2015) Ankylosing spondylitis confers substantially increased risk of clinical spine fractures: a nationwide case-control study. Osteoporos Int. https://doi.org/10.1007/s00198-014-2939-3
Robinson Y, Sandén B, Olerud C (2013) Increased occurrence of spinal fractures related to ankylosing spondylitis: A prospective 22-year cohort study in 17,764 patients from a national registry in Sweden. Patient Saf Surg. https://doi.org/10.1186/1754-9493-7-2
Lukasiewicz AM, Bohl DD, Varthi AG et al (2016) Spinal fracture in patients with ankylosing spondylitis: cohort definition distribution of injuries, and hospital outcomes. Spine Phila Pa 1976. https://doi.org/10.1097/BRS.0000000000001190
Ull C, Yilmaz E, Hoffmann MF et al (2021) Factors associated with major complications and mortality during hospitalization in patients with ankylosing spondylitis undergoing surgical management for a spine fracture. Glob spine J. https://doi.org/10.1177/2192568220980702
Westerveld LA, Verlaan JJ, Oner FC (2009) Spinal fractures in patients with ankylosing spinal disorders: A systematic review of the literature on treatment, neurological status and complications. Eur spine J. https://doi.org/10.1007/s00586-008-0764-0
Reinhold M, Knop C, Kneitz C, Disch A (2018) Spine fractures in ankylosing diseases: recommendations of the spine section of the German society for orthopaedics and trauma (DGOU). Glob Spine J. https://doi.org/10.1177/2192568217736268
Choi D (2015) Fractures in ankylosing disorders of the Spine: easy to miss and high risk of deterioration. World Neurosurg. https://doi.org/10.1016/j.wneu.2015.01.046
Anwar F, Al-Khayer A, Joseph G et al (2011) Delayed presentation and diagnosis of cervical spine injuries in long-standing ankylosing spondylitis. Eur spine J. https://doi.org/10.1007/s00586-010-1628-y
Gao Q, Zhang Z, Shao T et al (2021) Predictor of surgical outcomes in ankylosing spondylitis cervical spinal fracture: an at least 2 years follow-up retrospective study. Spine Phila. Pa 1976 46(1):31–36
Ilinani RR, Shetty AP (2018) Fractures in ankylosed spines: Current concepts. Indian spine J. https://doi.org/10.4103/isj.isj_19_18
Isla Guerrero A, Mansilla Fernández B, Hernández Garcia B et al (2018) Surgical outcomes of traumatic cervical fractures in patients with ankylosing spondylitis. Neurocirugia. https://doi.org/10.1016/j.neucir.2017.11.001
Ma J, Wang C, Zhou X et al (2015) Surgical therapy of cervical Spine fracture in patients with ankylosing spondylitis. Med (United States). https://doi.org/10.1097/MD.0000000000001663
He A, Xie D, Cai X et al (2017) One-stage surgical treatment of cervical spine fracture-dislocation in patients with ankylosing spondylitis via the combined anterior-posterior approach. Med (United States). https://doi.org/10.1097/MD.0000000000007432
Robinson Y, Robinson AL, Olerud C (2015) Complications and survival after long posterior instrumentation of cervical and cervicothoracic fractures related to ankylosing spondylitis or diffuse idiopathic skeletal hyperostosis. Spine Phila Pa 1976. https://doi.org/10.1097/BRS.0000000000000726
Shlobin NA, Dahdaleh NS (2020) Surgical stabilization of a cervical fracture in a patient with ankylosing spondylitis in the sitting position. Cureus. https://doi.org/10.7759/cureus.6625
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors certify that they have no affiliations with or involvement in any organization or entity with any financial interest or non-financial interest in the subject matter or materials discussed in this manuscript.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Alhashash, M., Shousha, M., Heyde, C. et al. Cervical spine fractures in ankylosing spondylitis patients: an analysis of the presentation and clinical results of 110 surgically managed patients in two spine centers. Eur Spine J 32, 2131–2139 (2023). https://doi.org/10.1007/s00586-023-07692-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-023-07692-7