Abstract
Objective
The goal of this study was to evaluate the possible associations between anemia and morphologic features of lumbar disc degeneration (LDD) in subjects with low back pain.
Materials and methods
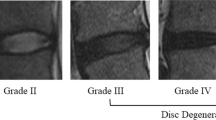
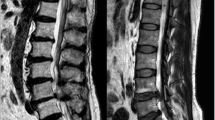
A total of 131 patients with normocytic or microcytic anemia (mean age 41.0 ± 6.4 yrs, BMI: 24.8 ± 3.3 kg/m2, 12.2% men) and a matched control group of 131 patients without anemia (mean age 41.0 ± 6.4 yrs, BMI: 24.9 ± 3.1 kg/m2, 12.2% men) were evaluated for LDD according to the Pfirrmann scoring system. The primary outcome was the difference of radiological features of LDD between two groups. The second outcome was the correlation between the hemoglobin (Hb) value and disc degeneration (DD). Statistical associations were assessed by Student's t-test, Chi-square test, and Spearman correlation.
Results
Anemic patients had a significantly higher number of degenerated discs than non-anemic patients in the level of L2/3 and L3/4 (p < 0.05). We also found that the severe DD occurred more frequently in the level of L2/3, L3/4 and L5/S1 among anemic patients (p < 0.05). In addition, we noticed that the incidence of multilevel LDD happened much more frequently in patients with anemia (p < 0.05). The Hb value showed a borderline negative correlation with the total score of DD (p = 0.056).
Conclusion
The results suggested that patients with anemia, and those without are radiologically different with varying patterns of DD. Patients with back pain and anemia were more likely to have extensive and severe DD. Although relevant mechanisms are not yet well understood, this study improved our understandings of the pathophysiology for LDD.



Similar content being viewed by others
Data availability
Raw data would be made available on reasonable request and with the permission of the institution where the data were generated. Hengrui Chang was the person to be contacted if someone wants to request the data from this study.
References
Katz JN (2006) Lumbar disc disorders and low-back pain: socioeconomic factors and consequences. J Bone Jt surg Am 88(Suppl 2):21–24. https://doi.org/10.2106/jbjs.E.01273
Lyu FJ, Cui H, Pan H, Mc Cheung K, Cao X, Iatridis JC, Zheng Z (2021) Painful intervertebral disc degeneration and inflammation: from laboratory evidence to clinical interventions. Bone Res 9:7. https://doi.org/10.1038/s41413-020-00125-x
Zhang B, Xu H, Wang J, Liu B, Sun G (2017) A narrative review of non-operative treatment, especially traditional Chinese medicine therapy, for lumbar intervertebral disc herniation. Biosci Trends 11:406–417. https://doi.org/10.5582/bst.2017.01199
Galbusera F, van Rijsbergen M, Ito K, Huyghe JM, Brayda-Bruno M, Wilke HJ (2014) Ageing and degenerative changes of the intervertebral disc and their impact on spinal flexibility. Eur Spine J 23(Suppl 3):S324-332. https://doi.org/10.1007/s00586-014-3203-4
Williams FM, Popham M, Sambrook PN, Jones AF, Spector TD, MacGregor AJ (2011) Progression of lumbar disc degeneration over a decade: a heritability study. Ann Rheum Dis 70:1203–1207. https://doi.org/10.1136/ard.2010.146001
Liuke M, Solovieva S, Lamminen A, Luoma K, Leino-Arjas P, Luukkonen R, Riihimäki H (2005) Disc degeneration of the lumbar spine in relation to overweight. Int J Obes 29:903–908. https://doi.org/10.1038/sj.ijo.0802974
Alpantaki K, Kampouroglou A, Koutserimpas C, Effraimidis G, Hadjipavlou A (2019) Diabetes mellitus as a risk factor for intervertebral disc degeneration: a critical review. Eur Spine J 28:2129–2144. https://doi.org/10.1007/s00586-019-06029-7
Teraguchi M, Yoshimura N, Hashizume H, Muraki S, Yamada H, Oka H, Minamide A, Ishimoto Y, Nagata K, Kagotani R, Tanaka S, Kawaguchi H, Nakamura K, Akune T, Yoshida M (2016) Metabolic syndrome components are associated with intervertebral disc degeneration: the Wakayama Spine Study. PLoS ONE 11:e0147565. https://doi.org/10.1371/journal.pone.0147565
Jang TW, Ahn YS, Byun J, Lee JI, Kim KH, Kim Y, Song HS, Lee CG, Kwon YJ, Yoon JH, Jeong K (2016) Lumbar intervertebral disc degeneration and related factors in Korean firefighters. BMJ Open 6:e011587. https://doi.org/10.1136/bmjopen-2016-011587
Guo Y, Li C, Shen B, Chen X, Hu T, Wu D (2022) Is intervertebral disc degeneration associated with reduction in serum ferritin? Eur Spine J. https://doi.org/10.1007/s00586-022-07361-1
Zhang C, Wang B, Zhao X, Li X, Lou Z, Chen X, Zhang F (2018) Iron deficiency accelerates intervertebral disc degeneration through affecting the stability of DNA polymerase epsilon complex. Am J Transl Res 10:3430–3442
Mirza FG, Abdul-Kadir R, Breymann C, Fraser IS, Taher A (2018) Impact and management of iron deficiency and iron deficiency anemia in women’s health. Expert Rev Hematol 11:727–736. https://doi.org/10.1080/17474086.2018.1502081
Camaschella C (2015) Iron deficiency: new insights into diagnosis and treatment. Hematol Am Soc Hematol Educ Progr 2015:8–13. https://doi.org/10.1182/asheducation-2015.1.8
Nutritional Anaemias (1972) Report of a WHO group of experts. World Health Organization technical report series
Schümann K, Solomons NW (2017) Perspective: what makes it so difficult to mitigate worldwide anemia prevalence? Adv Nutr 8:401–408. https://doi.org/10.3945/an.116.013847
Harrison LB, Chadha M, Hill RJ, Hu K, Shasha D (2002) Impact of tumor hypoxia and anemia on radiation therapy outcomes. Oncologist 7:492–508. https://doi.org/10.1634/theoncologist.7-6-492
Özdemir Z, Törer B, Hanta D, Cetinkaya B, Gulcan H, Tarcan A (2017) Determination of tissue hypoxia by physicochemical approach in premature anemia. Pediatr Neonatol 58:425–429. https://doi.org/10.1016/j.pedneo.2016.09.003
Yuan FL, Zhao MD, Jiang DL, Jin C, Liu HF, Xu MH, Hu W, Li X (2016) Involvement of acid-sensing ion channel 1a in matrix metabolism of endplate chondrocytes under extracellular acidic conditions through NF-κB transcriptional activity. Cell Stress Chaperones 21:97–104. https://doi.org/10.1007/s12192-015-0643-7
Gilbert HTJ, Hodson N, Baird P, Richardson SM, Hoyland JA (2016) Acidic pH promotes intervertebral disc degeneration: acid-sensing ion channel -3 as a potential therapeutic target. Sci Rep 6:37360. https://doi.org/10.1038/srep37360
Razaq S, Wilkins RJ, Urban JP (2003) The effect of extracellular pH on matrix turnover by cells of the bovine nucleus pulposus. Eur Spine J 12:341–349. https://doi.org/10.1007/s00586-003-0582-3
Kiraz M, Demir E (2020) Relationship of lumbar disc degeneration with hemoglobin value and smoking. Neurochirurgie 66:373–377. https://doi.org/10.1016/j.neuchi.2020.06.133
Chang H, Gao X, Li X, Zhao R, Ding W (2022) Anemia was associated with multilevel lumbar disc degeneration in patients with low back pain: a single-center retrospective study. Eur Spine J 31:1897–1905. https://doi.org/10.1007/s00586-022-07259-y
World Health Organization (2000) Obesity: preventing and managing the global epidemic. Report of a WHO consultation. World Health Organization technical report series
Rickenbacher P (2015) Update arterial hypertension 2015. Praxis 104:461–465. https://doi.org/10.1024/1661-8157/a001991
American Diabetes Association (2020) Classification and diagnosis of diabetes: Standards of Medical Care in Diabetes-2020. Diabetes Care 43:S14–S31. https://doi.org/10.2337/dc20-S002
Charlson ME, Pompei P, Ales KL, MacKenzie CR (1987) A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 40:373–383. https://doi.org/10.1016/0021-9681(87)90171-8
Pfirrmann CW, Metzdorf A, Zanetti M, Hodler J, Boos N (2001) Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine 26:1873–1878. https://doi.org/10.1097/00007632-200109010-00011
Ravindra VM, Senglaub SS, Rattani A, Dewan MC, Härtl R, Bisson E, Park KB, Shrime MG (2018) Degenerative lumbar spine disease: estimating global incidence and worldwide volume. Glob Spine J 8:784–794. https://doi.org/10.1177/2192568218770769
Safiri S, Kolahi AA, Noori M, Nejadghaderi SA, Karamzad N, Bragazzi NL, Sullman MJM, Abdollahi M, Collins GS, Kaufman JS, Grieger JA (2021) Burden of anemia and its underlying causes in 204 countries and territories, 1990–2019: results from the global burden of disease study 2019. J Hematol Oncol 14:185. https://doi.org/10.1186/s13045-021-01202-2
Pattappa G, Li Z, Peroglio M, Wismer N, Alini M, Grad S (2012) Diversity of intervertebral disc cells: phenotype and function. J Anat 221:480–496. https://doi.org/10.1111/j.1469-7580.2012.01521.x
Lu S, Song Y, Luo R, Li S, Li G, Wang K, Liao Z, Wang B, Ke W, Xiang Q, Chen C, Wu X, Zhang Y, Ling L, Yang C (2021) Ferroportin-dependent iron homeostasis protects against oxidative stress-induced nucleus pulposus cell ferroptosis and ameliorates intervertebral disc degeneration in vivo. Oxid Med Cell Longev 2021:6670497. https://doi.org/10.1155/2021/6670497
Vergroesen PP, Kingma I, Emanuel KS, Hoogendoorn RJ, Welting TJ, van Royen BJ, van Dieën JH, Smit TH (2015) Mechanics and biology in intervertebral disc degeneration: a vicious circle. Osteoarthr Cartil 23:1057–1070. https://doi.org/10.1016/j.joca.2015.03.028
Grunhagen T, Shirazi-Adl A, Fairbank JC, Urban JP (2011) Intervertebral disk nutrition: a review of factors influencing concentrations of nutrients and metabolites. Orthop Clin North Am 42:465–477. https://doi.org/10.1016/j.ocl.2011.07.010
Sakai D, Grad S (2015) Advancing the cellular and molecular therapy for intervertebral disc disease. Adv Drug Deliv Rev 84:159–171. https://doi.org/10.1016/j.addr.2014.06.009
Hee HT, Chuah YJ, Tan BH, Setiobudi T, Wong HK (2011) Vascularization and morphological changes of the endplate after axial compression and distraction of the intervertebral disc. Spine 36:505–511. https://doi.org/10.1097/BRS.0b013e3181d32410
Urban JP, Smith S, Fairbank JC (2004) Nutrition of the intervertebral disc. Spine 29:2700–2709. https://doi.org/10.1097/01.brs.0000146499.97948.52
Kauppila LI (2009) Atherosclerosis and disc degeneration/low-back pain–a systematic review. Eur J Vasc Endovasc Surg 37:661–670. https://doi.org/10.1016/j.ejvs.2009.02.006
Kurunlahti M, Tervonen O, Vanharanta H, Ilkko E, Suramo I (1999) Association of atherosclerosis with low back pain and the degree of disc degeneration. Spine 24:2080–2084. https://doi.org/10.1097/00007632-199910150-00003
Turgut AT, Sönmez I, Cakıt BD, Koşar P, Koşar U (2008) Pineal gland calcification, lumbar intervertebral disc degeneration and abdominal aorta calcifying atherosclerosis correlate in low back pain subjects: a cross-sectional observational CT study. Pathophysiology 15:31–39. https://doi.org/10.1016/j.pathophys.2007.12.001
Seitz AE, Eberhardt MS, Lukacs SL (2018) Anemia prevalence and trends in adults aged 65 and older: U.S. national health and nutrition examination survey: 2001–2004 to 2013–2016. J Am Geriatr Soc 66:2431–2432. https://doi.org/10.1111/jgs.15530
Hare GM, Freedman J, David Mazer C (2013) Review article: risks of anemia and related management strategies: can perioperative blood management improve patient safety? Canadian journal of anaesthesia Journal Canadien d’anesthesie 60:168–175. https://doi.org/10.1007/s12630-012-9861-y
Liu J, Tao H, Wang H, Dong F, Zhang R, Li J, Ge P, Song P, Zhang H, Xu P, Liu X, Shen C (2017) Biological behavior of human nucleus pulposus mesenchymal stem cells in response to changes in the acidic environment during intervertebral disc degeneration. Stem Cells Dev 26:901–911. https://doi.org/10.1089/scd.2016.0314
Bartels EM, Fairbank JC, Winlove CP, Urban JP (1998) Oxygen and lactate concentrations measured in vivo in the intervertebral discs of patients with scoliosis and back pain. Spine. 23:1–7. https://doi.org/10.1097/00007632-199801010-00001. (discussion 8)
Short MW, Domagalski JE (2013) Iron deficiency anemia: evaluation and management. Am Fam Physician 87:98–104
Camaschella C (2017) New insights into iron deficiency and iron deficiency anemia. Blood Rev 31:225–233. https://doi.org/10.1016/j.blre.2017.02.004
Munro MG, Mast AE, Powers JM, Kouides PA, O’Brien SH, Richards T, Lavin M, Levy BS (2023) The relationship between heavy menstrual bleeding, iron deficiency, and iron deficiency anemia. Am J Obstet Gynecol. https://doi.org/10.1016/j.ajog.2023.01.017
Díaz-Castro J, López-Frías MR, Campos MS, López-Frías M, Alférez MJ, Nestares T, Ojeda ML, López-Aliaga I (2012) Severe nutritional iron-deficiency anaemia has a negative effect on some bone turnover biomarkers in rats. Eur J Nutr 51:241–247. https://doi.org/10.1007/s00394-011-0212-5
Funding
Not applicable.
Author information
Authors and Affiliations
Contributions
WYD designed the study; HRC and JXX searched relevant studies; HRC, JXX and DLY analyzed and interpreted the data; HRC wrote the manuscript; and WYD approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors reported no conflicts of interest to declare in this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chang, H., Xu, J., Li, X. et al. Association between anemia and lumbar disc degeneration in patients with low back pain: an observational retrospective study. Eur Spine J 32, 2059–2068 (2023). https://doi.org/10.1007/s00586-023-07652-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-023-07652-1