Abstract
Purpose
The pathology of dropped head syndrome (DHS) is diverse, and reports of surgery for DHS are scarce. We aimed to describe surgery for DHS and to investigate the surgical outcomes thereof.
Methods
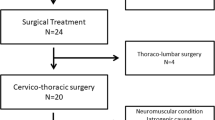
We enrolled 40 consecutive patients (six males and 34 females; average age at surgery, 72.0 years) with DHS who underwent correction surgeries at a single institute. Short fusion (SF), with the extent of fixation mainly at the cervical region, was performed for 27 patients; long fusion (LF), involving the cervical and thoracic spine, for 13. Clinical and radiological outcomes were investigated, and factors analyzed using the Japanese Orthopedic Association Cervical Myelopathy Evaluation Questionnaire (JOACMEQ).
Results
All patients were able to gaze horizontally at the follow-up. Instances of five transient C5 palsy results, and five distal junctional kyphosis results were found, but no revisions were reported due to recurrence. Patients whose T1 slope-20° was smaller than the C2–7 angle postoperatively exhibited better clinical outcomes in the three domains of the JOACMEQ, regardless of the extent of fixation.
Conclusion
For cases where the T1 slope is relatively small, and approximately 10° of cervical lordosis is predicted to be obtained postoperatively, SF is appropriate. Alternatively, for cases with higher T1 slope, obtaining a cervical lordosis over 20° has a risk of postoperative complications. For such cases, it is an option to perform an LF involving the cervical and thoracic spine.




Similar content being viewed by others
References
Kuncl RW, Cornblath DR, Griffin JW (1998) Assessment of thoracic paraspinal muscles in the diagnosis of ALS. Muscle Nerve 11:484–492. https://doi.org/10.1002/mus.880110512
Hoffman D, Gutmann L (1994) The dropped head syndrome with chronic inflammatory demyelinating polyneuropathy. Muscle Nerve 17:808–810. https://doi.org/10.1002/mus.880170717
Jaster JH, Bertorini TE, Swims MP, Dohan FC Jr, Menke PG, Becske T, Mönkemüller KE (1996) Cervical kyphosis after resolution of myopathic head drop. A case report. Spine (Phila Pa 1976) 21:2023–2025. https://doi.org/10.1097/00007632-199609010-00020
Rose MR, Levin KH, Griggs RC (1999) The dropped head plus syndrome: quantitation of response to corticosteroids. Muscle Nerve 22:115–118. https://doi.org/10.1002/(sici)1097-4598(199901)22:1%3c115::aid-mus18%3e3.0.co;2-c
Seidel C, Kuhnt T, Kortmann RD, Hering K (2015) Radiation-induced camptocormia and dropped head syndrome: review and case report of radiation-induced movement disorders. Strahlenther Onkol 191:765–770. https://doi.org/10.1007/s00066-015-0857-8
Mano T (2017) Reversal of dropped head syndrome after the cessation of dopaminergic agonist treatment in Parkinson disease. Clin Neuropharmacol 40:219–220. https://doi.org/10.1097/WNF.0000000000000243
Oliveira A, Massano J, Rosas MJ (2013) Dropped head syndrome in early-onset Parkinson disease treated with bilateral subthalamic stimulation: clinical, imaging, EMG, and biopsy findings. Neurol Sci 34:593–594. https://doi.org/10.1007/s10072-012-1089-7
Chu EC, Wong AY, Lin AF (2020) Isolated neck extensor myopathy associated with cervical spondylosis: a case report and brief review. Clin Med Insights Arthritis Musculoskelet Disord 13:1179544120977844. https://doi.org/10.1177/1179544120977844
Hashimoto K, Miyamoto H, Ikeda T, Akagi M (2018) Radiologic features of dropped head syndrome in the overall sagittal alignment of the spine. Eur Spine J 27:467–474. https://doi.org/10.1007/s00586-017-5186-4
Endo K, Sawaji Y, Aihara T, Suzuki H, Murata K, Matsuoka Y, Nishimura H, Takamatsu T, Konishi T, Yamamoto K (2021) Eight cases of sudden-onset dropped head syndrome: patient series. J Neurosurg Case Lessons 2:CASE21177. https://doi.org/10.3171/CASE21177
Koda M, Furuya T, Kinoshita T, Miyashita T, Ota M, Maki S, Ijima Y, Saito J, Takahashi K, Yamazaki M, Aramomi M, Mannoji C (2016) Dropped head syndrome after cervical laminoplasty: a case control study. J Clin Neurosci 32:88–90. https://doi.org/10.1016/j.jocn.2016.03.027
Bajaj HS, Chapman AW (2022) Dropped head syndrome: report of a rare complication after multilevel bilateral cervical radiofrequency neurotomy. PAIN Rep 7:e1037. https://doi.org/10.1097/PR9.0000000000001037
Nakanishi K, Taneda M, Sumii T, Yabuuchi T, Iwakura N (2007) Cervical myelopathy caused by dropped head syndrome. Case report and review of the literature. J Neurosurg Spine 6:165–168. https://doi.org/10.3171/spi.2007.6.2.165
Chaouat D, Belange G (1999) Dropped head syndrome. Three case-Rep Rev Rhum 66:430–433
Miyamoto H, Ikeda T, Hashimoto K, Akagi M (2018) An algorithmic strategy of surgical intervention for cervical degenerative kyphosis. J Orthop Sci 23:635–642. https://doi.org/10.1016/j.jos.2018.03.012
Hyun SJ, Kim KJ, Jahng TA, Kim HJ (2017) Clinical impact of T1 slope minus cervical lordosis after multilevel posterior cervical fusion surgery: a minimum 2-year follow up data. Spine (Phila Pa 1976) 42:1859–1864. https://doi.org/10.1097/BRS.0000000000002250
Jones EL, Heller JG, Silcox DH, Hutton WC (1997) Cervical pedicle screws versus lateral mass screws. Anatomic feasibility and biomechanical comparison. Spine (Phila Pa 1976) 22:977–982. https://doi.org/10.1097/00007632-199705010-00009
Kim HJ, Iyer S (2016) Proximal junctional kyphosis. J Am Acad Orthop Surg 24:318–326. https://doi.org/10.5435/JAAOS-D-14-00393
Passias PG, Vasquez-Montes D, Poorman GW, Protopsaltis T, Horn SR, Bortz CA, Segreto F, Diebo B, Ames C, Smith J, LaFage V, LaFage R, Klineberg E, Shaffrey C, Bess S, Schwab F, ISSG (2018) Predictive model for distal junctional kyphosis after cervical deformity surgery. Spine J 18:2187–2194. https://doi.org/10.1016/j.spinee.2018.04.017
Wada E, Fukui M, Takahashi K, Takeuchi D, Hashizume H, Kanamori M, Hosono N, Kanchiku T, Kasai Y, Sekiguchi M, Konno SI, Kawakami M, Yonenobu K (2019) Japanese orthopaedic association cervical myelopathy evaluation questionnaire (JOACMEQ): part 5. Determination of responsiveness. J Orthop Sci 24:57–61. https://doi.org/10.1016/j.jos.2018.08.015
Kurakawa T, Miyamoto H, Kaneyama S, Sumi M, Uno K (2016) C5 nerve palsy after posterior reconstruction surgery: predictive risk factors of the incidence and critical range of correction for kyphosis. Eur Spine J 25:2060–2067. https://doi.org/10.1007/s00586-016-4548-7
Kudo Y, Toyone T, Endo K, Matsuoka Y, Okano I, Ishikawa K, Matsuoka A, Maruyama H, Yamamura R, Emori H, Tani S, Shirahata T, Hayakawa C, Hoshino Y, Ozawa T, Suzuki H, Aihara T, Murata K, Takamatsu T, Inagaki K (2020) Impact of spinopelvic sagittal alignment on the surgical outcomes of dropped head syndrome: a multi-center study. BMC Musculoskelet Disord 21:382. https://doi.org/10.1186/s12891-020-03416-w
Yagi M, Ohne H, Konomi T, Fujiyoshi K, Kaneko S, Komiyama T, Takemitsu M, Yato Y, Machida M, Asazuma T (2016) Teriparatide improves volumetric bone mineral density and fine bone structure in the UIV+1 vertebra, and reduces bone failure type PJK after surgery for adult spinal deformity. Osteoporos Int 27:3495–3502. https://doi.org/10.1007/s00198-016-3676-6
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was approved by the ethical committee of the institute (No. R02-041).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Miyamoto, H., Ikeda, T., Aoyama, S. et al. Dropped head syndrome: a treatment strategy and surgical intervention. Eur Spine J 32, 1275–1281 (2023). https://doi.org/10.1007/s00586-023-07563-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-023-07563-1