Abstract
Purpose
Adult spinal deformity (ASD) surgery carries a higher risk of perioperative systemic complications. However, evidence for the effect of planned two-staged surgery on the incidence of perioperative systemic complications is scarce. Here, we evaluated the effect of two-staged surgery on perioperative complications following ASD surgery using lateral lumbar interbody fusion (LLIF).
Methods
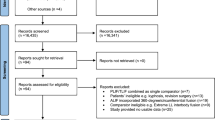
The study was conducted under a retrospective multi-center cohort design. Data on 293 consecutive ASD patients (107 in the two-staged group and 186 in the one-day group) receiving corrective surgery using LLIF between 2012 and 2021 were collected. Clinical outcomes included occurrence of perioperative systemic complications, reoperation, and intraoperative complications, operation time, intraoperative blood loss, transfusion, and length of hospital stay. The analysis was conducted using propensity score (PS)-stabilized inverse probability treatment weighting to adjust for confounding factors. Odds ratios (ORs) with 95% confidence intervals (CIs) were calculated in a PS-weighted cohort.
Results
In this cohort, 19 (18.4%) patients in the two-staged group and 43 (23.1%) patients in the one-day group experienced any systemic perioperative complication within 30 days following ASD surgery. In the PS-weighted cohort, compared with the patients undergoing one-day surgery, no association with the risk of systemic perioperative complications was seen in patients undergoing two-staged surgery (PS-weighted OR 0.78, 95% CI 0.37–1.63; p = 0.51).
Conclusion
Our study suggested that two-staged surgery was not associated with risk for perioperative systemic complications following ASD surgery using LLIF.



Similar content being viewed by others
References
Gum JL, Bridwell KH, Lenke LG et al (2015) SRS22R Appearance domain correlates most with patient satisfaction after adult deformity surgery to the sacrum at 5-year follow-up. Spine 40:1297–1302
Soroceanu A, Burton DC, Oren JH et al (2016) Medical complications after adult spinal deformity surgery: incidence, risk factors, and clinical impact. Spine 41:1718–1723
Bortz C, Pierce KE, Brown A et al (2021) Frequency and implications of concurrent complications following adult spinal deformity corrective surgery. Spine 46:E1155–E1160
Than KD, Mummaneni PV, Bridges KJ et al (2017) Complication rates associated with open versus percutaneous pedicle screw instrumentation among patients undergoing minimally invasive interbody fusion for adult spinal deformity. Neurosurg Focus 43:E7
Ohba T, Ebata S, Ikegami S et al (2020) Indications and limitations of minimally invasive lateral lumbar interbody fusion without osteotomy for adult spinal deformity. Eur Spine J 29:1362–1370
Yamato Y, Hasegawa T, Yoshida G et al (2021) Planned two-stage surgery using lateral lumbar interbody fusion and posterior corrective fusion: a retrospective study of perioperative complications. Eur Spine J 30:2368–2376
Lak AM, Lamba N, Pompilus F et al (2021) Minimally invasive versus open surgery for the correction of adult degenerative scoliosis: a systematic review. Neurosurg Rev 44:659–668
Kushioka J, Kaito T, Makino T et al (2018) Difference in the fusion rate and bone formation between artificial bone and iliac autograft inside an inter-body fusion cage–a comparison between porous hydroxyapatite/type 1 collagen composite and autologous iliac bone. J Orthop Sci 23:622–626
Gum JL, Lenke LG, Bumpass D et al (2016) Does planned staging for posterior-only vertebral column resections in spinal deformity surgery increase perioperative complications? Spine Deform 4:131–137
Safaee MM, Tenorio A, Osorio JA et al (2020) The effect of anterior lumbar interbody fusion staging order on perioperative complications in circumferential lumbar fusions performed within the same hospital admission. Neurosurg Focus 49:E6
Arzeno AH, Koltsov J, Alamin TF et al (2019) Short-term outcomes of staged versus same-day surgery for adult spinal deformity correction. Spine Deform 7:796-803.e1
Passias PG, Ma Y, Chiu YL et al (2012) Comparative safety of simultaneous and staged anterior and posterior spinal surgery. Spine 37:247–255
Passias PG, Poorman GW, Jalai CM et al (2017) Outcomes of open staged corrective surgery in the setting of adult spinal deformity. Spine J 17:1091–1099
Hu SS, Fontaine F, Kelly B, Bradford DS (1998) Nutritional depletion in staged spinal reconstructive surgery. The effect of total parenteral nutrition. Spine 23:1401–1405
Mandelbaum BR, Tolo VT, McAfee PC, Burest P (1988) Nutritional deficiencies after staged anterior and posterior spinal reconstructive surgery. Clin Orthop Relat Res 24:5–11
von Elm E, Altman DG, Egger M et al (2007) The strengthening the reporting of observational studies in epidemiology (STROBE) statement: guidelines for reporting observational studies. Lancet 370:1453–1457
Pierce KE, Naessig S, Kummer N et al (2021) the five-item modified frailty index is predictive of 30-day postoperative complications in patients undergoing spine surgery. Spine 46:939–943
Khalafallah AM, Huq S, Jimenez AE et al (2020) The 5-factor modified frailty index: an effective predictor of mortality in brain tumor patients. J Neurosurg 135:1–9
Schwab F, Blondel B, Chay E et al (2015) The comprehensive anatomical spinal osteotomy classification. Neurosurgery 76(Suppl 1):S33-41 (discussion S41)
Xu S, Ross C, Raebel MA et al (2010) Use of stabilized inverse propensity scores as weights to directly estimate relative risk and its confidence intervals. Value Health 13:273–277
Austin PC (2009) Balance diagnostics for comparing the distribution of baseline covariates between treatment groups in propensity-score matched samples. Stat Med 28:3083–3107
Yoshida G, Hasegawa T, Yamato Y et al (2018) Predicting perioperative complications in adult spinal deformity surgery using a simple sliding scale. Spine 43:562–570
Strom RG, Bae J, Mizutani J et al (2016) Lateral interbody fusion combined with open posterior surgery for adult spinal deformity. J Neurosurg Spine 25:697–705
Yamamoto T, Yagi M, Suzuki S et al (2021) Limited cost benefit of lateral interbody fusion for adult spinal deformity surgery. Spine 46:48–53
Makino T, Takenaka S, Sakai Y et al (2021) Factors related to length of hospital stay after two-stage corrective surgery for adult spinal deformity in elderly Japanese. J Orthop Sci 26:123–127
Acknowledgements
We thank Dr. Guy Harris DO of DMC Corp. (www.dmed.co.jp) for his support with the writing of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Masuda, S., Fujibayashi, S., Takemoto, M. et al. Association of two-staged surgery with systemic perioperative complications in lateral lumbar interbody fusion for adult spinal deformity: a propensity score-weighted study. Eur Spine J 32, 950–956 (2023). https://doi.org/10.1007/s00586-023-07539-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-023-07539-1