Abstract
Purpose
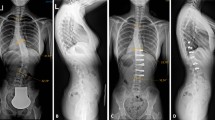
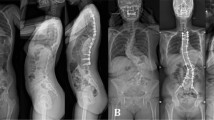
To develop a clinically feasible classification for severe spinal deformity based on X-ray features.
Methods
A total of 223 consecutive severe spinal deformity cases who underwent corrective operation were enrolled from 2004 to 2015 retrospectively. Based on X-ray features, a novel classification was developed containing three components: curve types, curve angle and apex location. There were five curve types as follows: single scoliosis (SS), kyphoscoliosis (KS), angular deformity (AD), long curve (LC), and double curves (DC). Curve angle subsection on coronal and sagittal planes including A:90–109, B:110–129, C:130–149, D: > 150. Apex location means the exact level of apex located. Reliability of the classification was tested.
Results
The kappa values for inter-observer and intra-observer reliability of the curve types, curve angle, and apex level were larger than 0.80. X-ray classification for overall patients with severe spinal deformity showed that there were 101 SS cases, 47 KS, 46 AD, 19 LC and 10 DC. For the curve angle, there were grade A 123 cases, B 43, C 18, D 15 on coronal plane and grade A 38, B 17, C 16, and D 19 on sagittal plane. Apex location showed there were 27 patients at T7 or upper levels, 31 on T8, 58 on T9, 45 on T10, 18 on T11, and 44 at T12 or lower levels.
Conclusion
A novel classification for severe spinal deformity was described based on X-ray morphology. A high value for inter-observer and intra-observer reliability was shown. Each subgroup has its particular influence on decision-making and prognostic prediction.


Similar content being viewed by others
References
King HA, Moe JH, Bradford DS et al (1983) The selection of fusion levels in thoracic idiopathic scoliosis. J Bone Joint Surg Am 65:1302–1313
Lenke LG, Betz RR, Harms J et al (2001) Adolescent idiopathic scoliosis: a new classification to determine extent of spinal arthrodesis. J Bone Joint Surg Am. 83:1169–1181
Qiu G, Li Q, Wang Y et al (2008) Comparison of reliability between the PUMC and Lenke classification systems for classifying adolescent idiopathic scoliosis. Spine 33(22):E836-842
Schwab F, Farcy JP, Bridwell K et al (2006) A clinical impact classification of scoliosis in the adult. Spine 31(18):2109–2114
Silva FE, Lenke LG (2010) Adult degenerative scoliosis: evaluation and management. Neurosurg Focus 28(3):E1
Kawakami N, Tsuji T, Imagama S et al (2009) Spinal deformity study group classification of congenital scoliosis and kyphosis: a new approach to the three-dimensional classification for progressive vertebral anomalies requiring operative treatment. Spine. 34(17):1756–1765
Williams BA, Matsumoto H, McCalla DJ et al (2014) Development and initial validation of the classification of early-onset scoliosis (C-EOS). J Bone Joint Surg Am 96(16):1359–1367
Yang JL, Huang ZF, Yin JQ et al (2016) A proposed classification system for guiding surgical strategy in cases of severe spinal deformity based on spinal cord function. Eur Spine J 25(6):1821–1829
Karikari IO, Pang H, Yankey KP et al (2019) A novel radiographic classification of severe spinal curvatures exceeding 100°: the Omega (Ω), gamma (γ) and alpha (α) deformities. Eur Spine J 28(6):1265–1276
Maclure M, Willett WC (1987) Misinterpretation and misuse of the kappa statistic. Am J Epidemiol 126(2):161–169
Wang Y, Xie J, Zhao Z et al (2016) Preoperative short-term traction prior to posterior vertebral column resection: procedure and role. Eur Spine J 25(3):687–697
Xie JM, Chen ZQ, Shen JX et al (2017) Expert consensus for PVCR in severe, rigid and angular spinal deformity treatment: the kunming consensus. J Orthop Surg (Hong Kong) 25(2):2309499017713939
Sucato DJ (2010) Management of severe spinal deformity: scoliosis and kyphosis. Spine 35(25):2186–2192
Auerbach JD, Lenke LG, Bridwell KH et al (2012) Major complications and comparison between 3-column osteotomy techniques in 105 consecutive spinal deformity procedures. Spine 37(14):1198–1210
Xie JM, Zhang Y, Wang YS et al (2014) The risk factors of neurologic deficits of one-stage posterior vertebral column resection for patients with severe and rigid spinal deformities. Eur Spine J 23(1):149–156
Wang Y, Xie J, Zhao Z et al (2015) Perioperative major non-neurological complications in 105 patients undergoing posterior vertebral column resection procedures for severe rigid deformities. Spine 40(16):1289–1296
Iyer S, Boachie-Adjei O, Duah HO et al (2019) Halo gravity traction can mitigate preoperative risk factors and early surgical complications in complex spine deformity. Spine 44(9):629–636
Xie J, Lenke LG, Li T et al (2015) Preliminary investigation of high-dose tranexamic acid for controlling intraoperative blood loss in patients undergoing spine correction surgery. Spine J 15(4):647–654
Lenke LG, Boachie-Adjie O, Sucato DJ, et al (2014) The deformity angular ratio accurately predicts risk of intraoperative spinal cord monitoring alerts during surgery for severe pediatric spinal deformity. E-poster presented at: SRS 49th Annual Meeting; Anchorage, AK.
Wang XB, Lenke LG, Thuet E et al (2016) Deformity angular ratio describes the severity of spinal deformity and predicts the risk of neurologic deficit in posterior vertebral column resection surgery. Spine 41(18):1447–1455
Lewis ND, Keshen SG, Lenke LG et al (2015) The deformity angular ratio: does it correlate with high-risk cases for potential spinal cord monitoring alerts in pediatric 3-Column thoracic spinal deformity corrective surgery? Spine 40(15):879–885
Fan H, Li X, Huang Z et al (2017) Radiologic parameters can affect the preoperative decision making of three-column spinal osteotomies in the treatment of severe and stiff kyphoscoliosis. Spine 42(23):1371–1379
Chen J, Shao XX, Sui WY et al (2020) Risk factors for neurological complications in severe and rigid spinal deformity correction of 177 cases. BMC Neurol 20(1):433
McMaster MJ, Glasby MA, Singh H et al (2007) Lung function in congenital kyphosis and kyphoscoliosis. J Spinal Disord Tech 20(3):203–208
Funding
The manuscript submitted does not contain information about medical device(s)/drug(s). This work was supported by Fund from the National Natural Science Foundation of China (Grant No 81860403) and the “Special and Joint Program” of Yunnan Provincial Science and Technology Department & Kunming Medical University [Grant No. 2017FE467(-009)].
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
No benefits in any form have been or will be received from a commercial party related directly or indirectly to the subject of this manuscript.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Consent for publication
Patients signed informed consent regarding publishing their data and photographs.
Ethics approval
This study was approved by the Institutional Review Board (IRB) of the Second Affiliated Hospital of Kunming Medical University. All patients provided written informed consent for the operation and the related study.
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhu, T., Wang, Y., Xie, J. et al. Development and initial validation of classification for severe spinal deformity based on X-ray features. Eur Spine J 31, 79–87 (2022). https://doi.org/10.1007/s00586-021-07028-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-021-07028-3