Abstract
Purpose
The aim of our study is to analyse mid- to long-term severe adult spinal deformity (ASD) surgery outcomes by comparing three-column osteotomies (3CO) and multiple anterior interbody fusion cages (AC).
Materials and methods
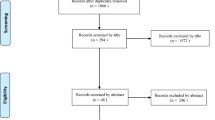
The PRISMA flowchart was used to systematically review the literature. Only articles with a minimum 24-month follow-up were examined, and 11 articles were included. The following radiological parameters were observed: pelvic incidence (PI), pelvic tilt (PT), lumbar lordosis (LL), sagittal vertical axis (SVA), Cobb angle and T1-sacrum plumbline. Clinical outcome was assessed using the visual analogue scale (VAS) and Oswestry disability index (ODI) scores. The main complications were analysed, and the two groups were compared.
Results
Except for age, the two populations were homogeneous. Both techniques had the same number of posterior instrumented levels (7.4 ± 1.7). The AC group had a mean 3 ± 1.4 interbody fusions per patient. In the PSO group, all patients had 1 3CO and 89.8% of the osteotomies were performed at L2 or L3 vertebrae. No difference was observed between the two groups in terms of clinical outcomes. Both techniques were effective in sagittal parameters restoration with a final PI–LL mismatch = 4.4°. The PSO group had a statistically higher rate of intraoperative blood loss (p = 0.036), major complications, pseudoarthrosis and dural tears (p < 0.001).
Conclusion
Both PSO and multiple AC are effective in treating ASD. Multiple AC seems more suitable when treating older patients because of a lower intraoperative blood loss, lower rate of major complications and fewer number of revision surgeries.

Similar content being viewed by others
References
Le Huec JC, Thompson W, Mohsinaly Y, Barrey C, Faundez A (2019) Sagittal balance of the spine. Eur Spine J 28(9):1889–1905. https://doi.org/10.1007/s00586-019-06083-1
Yilgor C, Sogunmez N, Boissiere L, Yavuz Y, Obeid I, Kleinstück F, Pérez-Grueso FJS, Acaroglu E, Haddad S, Mannion AF, Pellise F, Alanay A (2017) European spine study group (ESSG) global alignment and proportion (GAP) score: development and validation of a new method of analyzing spinopelvic alignment to predict mechanical complications after adult spinal deformity surgery. J Bone Jt Surg Am 99(19):1661–1672. https://doi.org/10.2106/JBJS.16.01594
Obeid I, Berjano P, Lamartina C, Chopin D, Boissière L, Bourghli A (2019) Classification of coronal imbalance in adult scoliosis and spine deformity a treatment-oriented guideline. Eur Spine J Jan 28(1):94–113. https://doi.org/10.1007/s00586-018-5826-3
Le Huec JC, Faundez A, Dominguez D, Hoffmeyer P, Aunoble S (2014) Evidence showing the relationship between sagittal balance and clinical outcomes in surgical treatment of degenerative spinal disease: a literature review. Int Orthopaedics 39(1):87–95. https://doi.org/10.1007/s00264-014-2516-6
Laouissat F, Sebaaly A, Gehrchen M, Roussouly P (2018) Classification of normal sagittal spine alignment: refounding the roussouly classification. Eur Spine J 27:2002–2011. https://doi.org/10.1007/s00586-017-5111-x
Berjano P, Lamartina C (2014) Classification of degenerative segment disease in adults with deformity of the lumbar or thoracolumbar spine. Eur Spine J 23:1815–1824. https://doi.org/10.1007/s00586-014-3219-9
Berjano P, Zanirato A, Compagnone D, Redaelli A, Damilano M, Lamartina C (2018) Hypercomplex pedicle subtraction osteotomies: definition, early clinical and radiological results and complications. Eur Spine J 27(Suppl 1):115–122. https://doi.org/10.1007/s00586-018-5463-x
Zanirato A, Damilano M, Formica M, Piazzolla A, Lovi A, Villafane JH, Berjano P (2018) Complications in adult spine deformity surgery: a systematic review of the recent literature with reporting of aggregated incidences. Eur Spine J 27(9):2272–2284. https://doi.org/10.1007/s00586-018-5535-y
Formica M, Cavagnaro L, Zanirato A, Felli L, Formica C (2016) Proximal junctional spondylodiscitis after pedicle subtraction osteotomy. Spine J 6(2):e49-51. https://doi.org/10.1016/j.spinee.2015.09.050
Saville PA, Kadam AB, Smith HE, Arlet V (2016) Anterior hyperlordotic cages: early experience and radiographic results. J Neurosurg Spine 25:713–719. https://doi.org/10.3171/2016.4.SPINE151206
Buric J, Conti R, Peressutti S (2018) Lumbar lordosis correction with interbody hyperlordotic cages initial experience, learning curve, technical aspects, and complication incidence. Int J Spine Surg Aug 3 12(2):185–189. https://doi.org/10.14444/5026
Formica M, Quarto E, Zanirato A, Mosconi L, Lontaro-Baracchini M, Alessio-Mazzola M, Felli L (2020) ALIF in the correction of spinal sagittal misalignment. A systematic review of literature. Eur Spine J Sep 15. https://doi.org/10.1007/s00586-020-06598-y
Chan AK, Mummaneni PV, Shaffrey CI (2018) Approach selection: multiple anterior lumbar interbody fusion to recreate lumbar lordosis versus pedicle subtraction osteotomy: when, why, how? Neurosurg Clin N Am 29:341–354. https://doi.org/10.1016/j.nec.2018.03.004
Butler JS, PhD LDF, Malhotra K et al (2019) 360-degree complex primary reconstruction using porous tantalum cages for adult degenerative spinal deformity. Global Spine J 9(6):613–618. https://doi.org/10.1177/2192568218814531
OCEBM Levels of Evidence Working Group*. “The Oxford Levels of Evidence 2”. Oxford Centre for Evidence-Based Medicine. https://www.cebm.ox.ac.uk/resources/levels-of-evidence/ocebm-levels-of-evidence
Berven SH, Deviren V, Smith JA, Emami A, Hu SS, Bradford DS (2001) Management of fixed sagittal plane deformity: results of the transpedicular wedge resection osteotomy. Spine (Phila Pa 1976) Sep 15 26(18):2036–2043. https://doi.org/10.1097/00007632-200109150-00020
Boachie-Adjei O, Ferguson JA, Pigeon RG, Peskin MR (2006) Transpedicular lumbar wedge resection osteotomy for fixed sagittal imbalance: surgical technique and early results. Spine (Phila Pa 1976) Feb 15 31(4):485–492. https://doi.org/10.1097/01.brs.0000199893.71141.59
Bridwell KH, Lewis SJ, Lenke LG, Baldus C, Blanke K (2003) Pedicle subtraction osteotomy for the treatment of fixed sagittal imbalance. J Bone Joint Surg Am Mar 85(3):454–463. https://doi.org/10.2106/00004623-200303000-00009
Crandall DG, Revella J (2009) Transforaminal lumbar interbody fusion versus anterior lumbar interbody fusion as an adjunct to posterior instrumented correction of degenerative lumbar scoliosis: three year clinical and radiographic outcomes. Spine (Phila Pa 1976) Sep 15 34(20):2126–2133. https://doi.org/10.1097/BRS.0b013e3181b612db
Hyun SJ, Rhim SC (2010) Clinical outcomes and complications after pedicle subtraction osteotomy for fixed sagittal imbalance patients; a long-term follow-up data. J Korean Neurosurg Soc Feb 47(2):95–101. https://doi.org/10.3340/jkns.2010.47.2.95
Lee KY, Lee JH, Kang KC, Shin SJ, Shin WJ, Im SK, Park MS (2020) Minimally invasive multilevel lateral lumbar interbody fusion with posterior column osteotomy compared with pedicle subtraction osteotomy for adult spinal deformity. Spine J Jun 20(6):925–933. https://doi.org/10.1016/j.spinee.2019.12.001
Noun Z, Lapresle P, Missenard G (2001) Posterior lumbar osteotomy for flat back in adults. J Spinal Disord Aug 14(4):311–316. https://doi.org/10.1097/00002517-200108000-00005
Park HY, Ha KY, Kim YH, Chang DG, Kim SI, Lee JW, Ahn JH, Kim JB (2018) Minimally invasive lateral lumbar interbody fusion for adult spinal deformity: clinical and radiological efficacy with minimum two years follow-up. Spine (Phila Pa 1976) Jul 15 43(14):E813–E821. https://doi.org/10.1097/BRS.0000000000002507
Park SW, Ko MJ, Kim YB, Le Huec JC (2020) Correction of marked sagittal deformity with circumferential minimally invasive surgery using oblique lateral interbody fusion in adult spinal deformity. J Orthop Surg Res Jan 15 15(1):13. https://doi.org/10.1186/s13018-020-1545-7
Saigal R, Akbarnia BA, Eastlack RK, Bagheri A, Tran S, Brown D, Bagheri R, Mundis GM (2020) Anterior column realignment: analysis of neurological risk and radiographic outcomes. Neurosurgery Sep 87(3):E347–E354. https://doi.org/10.1093/neuros/nyaa064
Toyone T, Shiboi R, Ozawa T, Inada K, Shirahata T, Kamikawa K, Watanabe A, Matsuki K, Ochiai S, Kaiho T, Morikawa Y, Sota K, Yasuchika A, Gen I, Sumihisa O, Ohtori S, Takahashi K, Wada Y (2012) Asymmetrical pedicle subtraction osteotomy for rigid degenerative lumbar kyphoscoliosis. Spine Phila Pa Oct 1 37(21):1847–1852. https://doi.org/10.1097/BRS.0b013e31825bf644
Yoshida G, Hasegawa T, Yamato Y et al (2019) Minimum clinically important differences in Oswestry disability index domains and their impact on adult spinal deformity surgery. Asian Spine J 13(1):35–44. https://doi.org/10.31616/asj.2018.0077
Schwab F, Dubey A, Gamez L, El Fegoun AB, Hwang K, Pagala M, Farcy JP (2005) Adults scoliosis: prevalence, SF-36, and nutritional parameters in elderly volunteer population. Spine (Phila Pa 1976) 30:1082–1085. https://doi.org/10.1097/01.brs.0000160842.43482.cd
McAviney J, Roberts C, Sullivan B, Alevras AJ, Graham PL, Brown BT (2020) The prevalence of adult de novo scoliosis: a systematic review and meta-analysis. Eur Spine J Dec. 29(12):2960–2969. https://doi.org/10.1007/s00586-020-06453-0
Bridwell KH, Lewis SJ, Edwards C, Lenke LG, Iffrig TM, Berra A, Baldus C, Blanke K (2003) Complications and outcomes of pedicle subtraction osteotomies for fixed sagittal imbalance. Spine (Phila Pa 1976) Sep 15 28(18):2093–2101. https://doi.org/10.1097/01.BRS.0000090891.60232.70
Buchowski JM, Bridwell KH, Lenke LG, Kuhns CA, Lehman RA Jr, Kim YJ, Stewart D, Baldus C (2007) Neurologic complications of lumbar pedicle subtraction osteotomy: a 10-year assessment. Spine (Phila Pa 1976) Sep 15 32(20):2245–2252. https://doi.org/10.1097/BRS.0b013e31814b2d52
Formica M, Quarto E, Zanirato A, Mosconi L, Vallerga D, Zotta I, Baracchini ML, Formica C, Felli L (2020) Lateral lumbar interbody fusion: what is the evidence of indirect neural decompression? A systematic review of the literature. HSS J Jul 16(2):143–154. https://doi.org/10.1007/s11420-019-09734-7
Rao PJ, Maharaj MM, Phan K, Lakshan Abeygunasekara M, Mobbs RJ (2015) Indirect foraminal decompression after anterior lumbar interbody fusion: a prospective radiographic study using a new pedicle-to-pedicle technique. Spine J 1 15(5):817–824. https://doi.org/10.1016/j.spinee.2014.12.019
Formica M, Vallerga D, Zanirato A, Cavagnaro L, Basso M, Divano S, Mosconi L, Quarto E, Siri G, Felli L (2020) Fusion rate and influence of surgery-related factors in lumbar interbody arthrodesis for degenerative spine diseases: a meta-analysis and systematic review. Musculoskelet Surg Apr 104(1):1–15. https://doi.org/10.1007/s12306-019-00634-x
Cho KY, Kim KT, Kim WJ, Lee SH, Jung JH, Kim YT, Park HB (2013) Pedicle subtraction osteotomy in elderly patients with degenerative sagittal imbalance. Spine 38(24):E1561–E1566. https://doi.org/10.1097/BRS.0b013e3182a63c29
Dahl BT, Harris JA, Gudipally M et al (2017) Kinematic efficacy of supplemental anterior lumbar interbody fusion at lumbosacral levels in thoracolumbosacral deformity correction with and without pedicle subtraction osteotomy at L3: an in vitro cadaveric study. Eur Spine J 26(11):2773–2781. https://doi.org/10.1007/s00586-017-5222-4
Ayhan S, Aykac B, Guler UO et al (2016) Safety and efficacy of osteotomies in adult deformity: what happens in the first year? Eur Spine J 25:2471–2479. https://doi.org/10.1007/s00586-015-3981-3
Le Huec JC, Richards J, Tsoupras A, Price R, Leglise A, Faundez AA (2018) The mechanism in junctional failure of thoraco-lumbar fusions. Part I: biomechanical analysis of mechanism responsible of vertebral overstress and description of cervical inclination angle (CIA). Eur Spine J Feb 27(Suppl 1):129–138. https://doi.org/10.1007/s00586-017-5425-8
Faundez AA, Richards J, Maxy P, Price R, Leglise A, Le Huec JC (2018) The mechanism in junctional failure of thoraco-lumbar fusions. Part II: analysis of a series of PJK after thoraco-lumbar fusion to determine parameters allowing to predict the risk of junctional breakdown. Eur Spine J Feb 27(Suppl 1):139–148. https://doi.org/10.1007/s00586-017-5426-7
Schwab FJ, Blondel B, Bess S et al (2013) Radiographical spinopelvic parameters and disability in the setting of adult spinal deformity: a prospective multicenter analysis. Spine (Phila Pa 1976) 38(13):E803-12. https://doi.org/10.1097/BRS.0b013e318292b7b9
Alzakri A, Boissière L, Cawley DT, Bourghli A, Pointillart V, Gille O, Vital JM, Obeid I (2018) L5 pedicle subtraction osteotomy: indication, surgical technique and specificities. Eur Spine J Mar 27(3):644–651. https://doi.org/10.1007/s00586-017-5403-1
Jang JS, Lee SH, Min JH, Maeng DH (2007) Changes in sagittal alignment after restoration of lower lumbar lordosis in patients with degenerative flat back syndrome. J Neurosurg Spine Oct 7(4):387–392. https://doi.org/10.3171/SPI-07/10/387
Lafage V, Schwab F, Vira S, Hart R, Burton D, Smith JS, Boachie-Adjei O, Shelokov A, Hostin R, Shaffrey CI, Gupta M, Akbarnia BA, Bess S, Farcy JP (2011) Does vertebral level of pedicle subtraction osteotomy correlate with degree of spinopelvic parameter correction? J Neurosurg Spine (Phila Pa 1976) 14(2):184–191. https://doi.org/10.3171/2010.9.SPINE10129
Saigal R, Mundis GM Jr, Eastlack R, Uribe JS, Phillips FM, Akbarnia BA (2016) Anterior Column Realignment (ACR) in Adult Spinal Deformity Correction: Technique and Review of the Literature. Spine Phila Pa Apr 41(Suppl 8):66–73. https://doi.org/10.1097/BRS.0000000000001483
Leveque JC, Yanamadala V, Buchlak QD, Sethi RK (2017) Correction of severe spinopelvic mismatch: decreased blood loss with lateral hyperlordotic interbody grafts as compared with pedicle subtraction osteotomy. Neurosurg Focus Aug 43(2):E15. https://doi.org/10.3171/2017.5.FOCUS17195
Lau D, Haddad AF, Deviren V, Ames CP (2020) Asymmetrical pedicle subtraction osteotomy for correction of concurrent sagittal-coronal imbalance in adult spinal deformity: a comparative analysis. J Neurosurg Spine Aug 7:1–8. https://doi.org/10.3171/2020.5.SPINE20445
Funding
No funding was received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This is a systematic review of the literature, and no ethical approval was necessary for this study.
Informed consent
Informed consent was not applicable to this study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
E., Q., A., Z., C., U. et al. Adult spinal deformity surgery: posterior three-column osteotomies vs anterior lordotic cages with posterior fusion. Complications, clinical and radiological results. A systematic review of the literature. Eur Spine J 30, 3150–3161 (2021). https://doi.org/10.1007/s00586-021-06925-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-021-06925-x