Abstract
Purpose
Sagittal lumbar apex has been demonstrated to be a key parameter in sagittal plane morphology. Our aim was to understand its behavior with postural changes, analyzing two different concepts of lumbar apex.
Materials and methods
Prospective observational study with a cohort of patients presenting sagittal malalignment identified from a monocenter database of adult spinal deformities (ASD). Inclusion criteria were age > 30 years, SVA > 40 mm, and/or PT > 20. All patients had full-spine EOS radiographs in 2 different positions: (P1: natural position) and position 2 (P2: compensated position).
Sagittal alignment, spinopelvic values, and two different methods of assessing lordosis apex location were analyzed in both P1 and P2 positions. Changes between P1 and P2 were compared using a paired t test with a significance level at p < 0.05.
Results
Twenty-five patients were recruited (21 women and 4 men). The mean age was 64.8 years (range 21–79). The patient’s main compensation was based on an increase in the femoral shaft angle, and pelvic retroversion, with a subsequent decrease in sacral slope, and therefore of the lower lumbar arc.
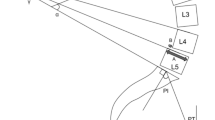
When the lumbar apex was calculated as the most anterior point touching the vertical line in a lateral radiograph, postural compensation changes modified its location usually shifting it to a more caudal position. When the lumbar apex was assessed as the most distant point of the global lumbar lordosis, its position remained stable regardless of compensation.
Conclusions
Postural changes can modify the location of the lumbar apex when understanding its location as the cornerstone of sagittal plane harmonic distribution. This concept can be useful as an additional sign to assess compensation. However, if the lumbar apex was calculated as the angular point of the global lordosis, its position remained stable regardless of postural changes. This concept can help to mold lumbar lordosis in ASD surgery.
Level of evidence IV
Diagnostic: individual cross-sectional studies with consistently applied reference standard and blinding.





Similar content being viewed by others
References
Diebo BG, Henry J, Lafage V, Berjano P (2015) Sagittal deformities of the spine: factors influencing the outcomes and complications. Eur Spine J 24(Suppl 1):S3-15. https://doi.org/10.1007/s00586-014-3653-8
Berthonnaud E, Dimnet J, Roussouly P, Labelle H (2005) Analysis of the sagittal balance of the spine and pelvis using shape and orientation parameters. J Spinal Disord Tech 18:40–47
Roussouly P, Pinheiro-Franco JL (2011) Sagittal parameters of the spine: biomechanical approach. Eur Spine J 20:578–585. https://doi.org/10.1007/s00586-011-1924-1
Roussouly P, Gollogly S, Berthonnaud E, Dimnet J (2005) Classification of the normal variation in the sagittal alignment of the human lumbar spine and pelvis in the standing position. Spine 30:346–353
Laouissat F, Sebaaly A, Gehrchen M, Roussouly P (2017) Classification of normal sagittal spine alignment: refounding the Roussouly classification. Eur Spine J 18:10–40. https://doi.org/10.1007/s00586-017-5111-x
Pan C, Wang G, Sun J (2020) Correlation between the apex of lumbar lordosis and pelvic incidence in asymptomatic adult. Eur Spine J 29:420–427. https://doi.org/10.1007/s00586-019-06183-y
Roussouly P, Nnadi C (2010) Sagittal plane deformity: an overview of interpretation and management. Eur Spine J 19:1824–1836. https://doi.org/10.1007/s00586-010-1476-9
Diebo BG, Ferrero E, Lafage R et al (2015) Recruitment of compensatory mechanisms in sagittal spinal malalignment is age and regional deformity dependent. Spine 40:642–649. https://doi.org/10.1097/BRS.0000000000000844
Sebaaly A, Riouallon G, Obeid I et al (2018) Proximal junctional kyphosis in adult scoliosis: comparison of four radiological predictor models. Eur Spine J 27:613–621. https://doi.org/10.1007/s00586-017-5172-x
Sebaaly A, Gehrchen M, Silvestre C et al (2019) Mechanical complications in adult spinal deformity and the effect of restoring the spinal shapes according to the Roussouly classification: a multicentric study. Eur Spine J 37:1763–1810. https://doi.org/10.1007/s00586-019-06253-1
Pizones J, Moreno-Manzanaro L, Sánchez Pérez-Grueso FJ et al (2019) Restoring the ideal Roussouly sagittal profile in adult scoliosis surgery decreases the risk of mechanical complications. Eur Spine J 14:925. https://doi.org/10.1007/s00586-019-06176-x
Pizones J, Perez-Grueso FJS, Moreno-Manzanaro L et al (2020) Ideal sagittal profile restoration and ideal lumbar apex positioning play an important role in postoperative mechanical complications after a lumbar PSO. Spine Deformity 8:491–498. https://doi.org/10.1007/s43390-019-00005-3
Horton WC, Brown CW, Bridwell KH et al (2005) Is there an optimal patient stance for obtaining a lateral 36" radiograph? A critical comparison of three techniques. Spine 30:427–433. https://doi.org/10.1097/01.brs.0000153698.94091.f8
Sebaaly A, Sylvestre C, El Quehtani Y et al (2018) Incidence and risk factors for proximal junctional kyphosis: results of a multicentric study of adult scoliosis. Clin Spine Surg 31:E178–E183. https://doi.org/10.1097/BSD.0000000000000630
Yamato Y, Sato Y, Togawa D et al (2019) Differences in the geometrical spinal shape in the sagittal plane according to age and magnitude of pelvic incidence in healthy elderly individuals. J Orthop Sci. https://doi.org/10.1016/j.jos.2019.07.005
Roussouly P, Gollogly S, Noseda O et al (2006) The vertical projection of the sum of the ground reactive forces of a standing patient is not the same as the C7 plumb line: a radiographic study of the sagittal alignment of 153 asymptomatic volunteers. Spine 31:E320–E325. https://doi.org/10.1097/01.brs.0000218263.58642.ff
Schwab F, Lafage V, Boyce R et al (2006) Gravity line analysis in adult volunteers: age-related correlation with spinal parameters, pelvic parameters, and foot position. Spine 31:E959–E967. https://doi.org/10.1097/01.brs.0000248126.96737.0f
Gelb DE, Lenke LG, Bridwell KH et al (1995) An analysis of sagittal spinal alignment in 100 asymptomatic middle and older aged volunteers. Spine 20:1351–1358
Bernhardt M, Bridwell KH (1989) Segmental analysis of the sagittal plane alignment of the normal thoracic and lumbar spines and thoracolumbar junction. Spine 14:717–721
Tono O, Hasegawa K, Okamoto M et al (2019) Lumbar lordosis does not correlate with pelvic incidence in the cases with the lordosis apex located at L3 or above. Eur Spine J 28:1948–1954. https://doi.org/10.1007/s00586-018-5695-9
Pesenti S, Lafage R, Stein D et al (2018) The amount of proximal lumbar lordosis is related to pelvic incidence. Clin Orthop Relat Res 476:1603–1611. https://doi.org/10.1097/CORR.0000000000000380
Barrey C, Roussouly P, Le Huec J-C et al (2013) Compensatory mechanisms contributing to keep the sagittal balance of the spine. Eur Spine J 22(Suppl 6):S834–S841. https://doi.org/10.1007/s00586-013-3030-z
Chernukha KV, Daffner RH, Reigel DH (1998) Lumbar lordosis measurement. A new method versus Cobb technique. Spine 23:74–79. https://doi.org/10.1097/00007632-199801010-00016
Hong J-Y, Suh S-W, Modi HN et al (2010) Reliability analysis for radiographic measures of lumbar lordosis in adult scoliosis: a case-control study comparing 6 methods. Eur Spine J 19:1551–1557. https://doi.org/10.1007/s00586-010-1422-x
Sebaaly A, Grobost P, Mallam L, Roussouly P (2018) Description of the sagittal alignment of the degenerative human spine. Eur Spine J 27:489–496. https://doi.org/10.1007/s00586-017-5404-0
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Iwai, C., Pizones, J., Boissière, L. et al. Static and dynamic sagittal lumbar apex: a new concept for the assessment of lumbar lordosis distribution in spinal deformity. Eur Spine J 30, 1155–1163 (2021). https://doi.org/10.1007/s00586-021-06767-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-021-06767-7