Abstract
Purpose
To determine whether there is an association between preoperative 10-Item Patient Activation Measure (PAM-10) scores and clinical outcomes following MIS LD.
Methods
Patients undergoing a primary MIS LD were retrospectively reviewed and stratified according to their preoperative PAM-10 scores: “low PAM,” “moderate PAM,” and “high PAM.” Preoperative PAM score cohorts were tested for improvements in Oswestry Disability Index (ODI), 12-Item Short-Form Physical Component Score (SF-12 PCS), and Visual Analog Scale (VAS) back and leg pain using multivariate linear regression.
Results
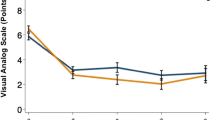
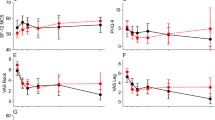
Eighty-nine patients were included: 29 had a low PAM score, 32 had a moderate PAM score, and 28 had a high PAM score. Cohorts experienced similar preoperative VAS back pain, VAS leg pain, ODI, and SF-12 PCS. Patients with low PAM scores experienced a trend of higher pain scores throughout 6 months with VAS back pain being significant at 3 months and VAS leg pain being significant at 6-week and 3-month follow-up. Patients with lower PAM scores experienced a worse improvement in ODI at 6-week, 3-month, and 6-month timepoints. Lastly, patients with lower PAM scores demonstrated less improvement in SF-12 PCS at 3-month and 6-month follow-up.
Conclusions
Lower preoperative PAM scores were associated with worse improvement in clinical outcomes following MIS LD. Patients with lower PAM scores had diminished improvement in long-term patient-reported outcomes including ODI, SF-12, and VAS back and leg pain. Our investigation suggests that preoperative PAM assessments may be an effective tool to predict postoperative outcomes following MIS LD.

Similar content being viewed by others
References
Skolasky RL, Mackenzie EJ, Wegener ST, Riley LH (2011) Patient activation and functional recovery in persons undergoing spine surgery. J Bone Joint Surg Am 93:1665–1671
Skolasky RL, Mackenzie EJ, Wegener ST, Riley LH 3rd (2008) Patient activation and adherence to physical therapy in persons undergoing spine surgery. Spine 33:E784–E791. https://doi.org/10.1097/BRS.0b013e31818027f1
Skolasky RL, Mackenzie EJ, Riley LH 3rd, Wegener ST (2009) Psychometric properties of the patient activation measure among individuals presenting for elective lumbar spine surgery. Qual Life Res 18:1357–1366. https://doi.org/10.1007/s11136-009-9549-0
Block AR (2016) Demoralization, patient activation, and the outcome of spine surgery. Healthcare (Basel). https://doi.org/10.3390/healthcare4010011
Hibbard JH, Stockard J, Mahoney ER, Tusler M (2004) Development of the patient activation measure (PAM): conceptualizing and measuring activation in patients and consumers. Health Serv Res 39:1005–1026. https://doi.org/10.1111/j.1475-6773.2004.00269.x
Hibbard JH, Tusler M (2007) Assessing activation stage and employing a “next steps” approach to supporting patient self-management. J Ambul Care Manag 30:2
Mosen DM, Schmittdiel J, Hibbard J et al (2007) Is patient activation associated with outcomes of care for adults with chronic conditions? J Ambul Care Manag 30:21–29. https://doi.org/10.1097/00004479-200701000-00005
Hibbard JH, Mahoney ER, Stockard J, Tusler M (2005) Development and testing of a short form of the patient activation measure. Health Serv Res 40:1918–1930. https://doi.org/10.1111/j.1475-6773.2005.00438.x
Jung C, Padman R (2015) Disruptive digital innovation in healthcare delivery: the case for patient portals and online clinical consultations. In: Agarwal R, Selen W, Roos G, Green R (eds) The handbook of service innovation. Springer, London, pp 297–318
Weingart SN, Rind D, Tofias Z, Sands DZ (2006) Who uses the patient internet portal? The Patient Site experience. J Am Med Inform Assoc 13:91–95. https://doi.org/10.1197/jamia.M1833
Zarcadoolas C, Vaughon WL, Czaja SJ et al (2013) Consumers’ perceptions of patient-accessible electronic medical records. J Med Internet Res 15:e168. https://doi.org/10.2196/jmir.2507
Hibbard JH, Greene J, Overton V (2013) Patients with lower activation associated with higher costs; delivery systems should know their patients’“scores”. Health Aff 32:216–222
Hassol A, Walker JM, Kidder D et al (2004) Patient experiences and attitudes about access to a patient electronic health care record and linked web messaging. J Am Med Inform Assoc 11:505–513
Peters AE, Keeley EC (2017) Patient engagement following acute myocardial infarction and its influence on outcomes. Am J Cardiol 120:1467–1471. https://doi.org/10.1016/j.amjcard.2017.07.037
Crandall KJ, Jason Crandall K, Western Kentucky University Center for Applied Science in Health and Aging, et al (2019) Assessing the impact of a game-centered mobile app on community-dwelling older adults’ health activation. OBM Integr Complement Med. 4:1
Yun PS, MacDonald CL, Orne J et al (2020) A novel surgical patient engagement model: a qualitative study of postoperative patients. J Surg Res 248:82–89. https://doi.org/10.1016/j.jss.2019.11.025
Tecson KM, Bass K, Felius J et al (2019) Patient “activation” of patients referred for advanced heart failure therapy. Am J Cardiol 123:627–631. https://doi.org/10.1016/j.amjcard.2018.11.013
Hibbard JH (2017) Assessing measurement properties of the PAM 10 and 13. Insignia Health website. https://s3.amazonaws.com/insigniahealth.com-assets/Comparing-PAM-10-to-PAM-13.pdf?mtime=20191206162413. Accessed 27 Apr 2020
Hibbard J (2017) Patient activation and health literacy: what’s the difference? How do each contribute to health outcomes. Stud Health Technol Inform 240:251–262
Howard JS, Toonstra JL, Meade AR et al (2016) Feasibility of conducting a web-based survey of patient-reported outcomes and rehabilitation progress. Digit Health 2:2055207616644844. https://doi.org/10.1177/2055207616644844
Schamber EM, Takemoto SK, Chenok KE, Bozic KJ (2013) Barriers to completion of patient reported outcome measures. J Arthroplast 28:1449–1453. https://doi.org/10.1016/j.arth.2013.06.025
Block AR (2016) Demoralization, patient activation, and the outcome of spine surgery. Healthcare (Basel). https://doi.org/10.3390/healthcare4010011
Marshall R, Beach MC, Saha S et al (2013) Patient activation and improved outcomes in HIV-infected patients. J Gen Intern Med 28:668–674. https://doi.org/10.1007/s11606-012-2307-y
Saft HL, Kilaru S, Moore E et al (2008) The impact of a patient activation measure on asthma outcomes: a pilot study. Chest 134:2S. https://doi.org/10.1378/chest.134.4_MeetingAbstracts.s2004
Rogvi S, Tapager I, Almdal TP et al (2012) Patient factors and glycaemic control–associations and explanatory power. Diabet Med 29:e382–e389. https://doi.org/10.1111/j.1464-5491.2012.03703.x
Block AR, Marek RJ, Ben-Porath YS, Kukal D (2017) Associations between pre-implant psychosocial factors and spinal cord stimulation outcome: evaluation using the MMPI-2-RF. Assessment 24:60–70. https://doi.org/10.1177/1073191115601518
Marek RJ, Block AR, Ben-Porath YS (2015) The minnesota multiphasic personality inventory-2-restructured form (MMPI-2-RF): incremental validity in predicting early postoperative outcomes in spine surgery candidates. Psychol Assess 27:114–124. https://doi.org/10.1037/pas0000035
Edwards RR, Klick B, Buenaver L et al (2007) Symptoms of distress as prospective predictors of pain-related sciatica treatment outcomes. Pain 130:47–55. https://doi.org/10.1016/j.pain.2006.10.026
Trief PM, Grant W, Fredrickson B (2000) A prospective study of psychological predictors of lumbar surgery outcome. Spine 25:2616–2621. https://doi.org/10.1097/00007632-200010150-00012
Voorhies RM, Jiang X, Thomas N (2007) Predicting outcome in the surgical treatment of lumbar radiculopathy using the Pain Drawing Score, McGill Short Form Pain Questionnaire, and risk factors including psychosocial issues and axial joint pain. Spine J 7:516–524
Chaichana KL, Mukherjee D, Adogwa O et al (2011) Correlation of preoperative depression and somatic perception scales with postoperative disability and quality of life after lumbar discectomy. J Neurosurg Spine 14:261–267
Basques BA, Varthi AG, Golinvaux NS et al (2014) Patient characteristics associated with increased postoperative length of stay and readmission after elective laminectomy for lumbar spinal stenosis. Spine 39:833–840. https://doi.org/10.1097/BRS.0000000000000276
Rihn JA, Hilibrand AS, Zhao W et al (2015) Effectiveness of surgery for lumbar stenosis and degenerative spondylolisthesis in the octogenarian population: analysis of the Spine Patient Outcomes Research Trial (SPORT) data. J Bone Joint Surg Am 97:177–185. https://doi.org/10.2106/JBJS.N.00313
Andrawis J, Akhavan S, Chan V et al (2015) Higher preoperative patient activation associated with better patient-reported outcomes after total joint arthroplasty. Clin Orthop Relat Res 473:2688–2697. https://doi.org/10.1007/s11999-015-4247-4
Gruber JS, Hageman M, Neuhaus V et al (2014) Patient activation and disability in upper extremity illness. J Hand Surg Am 39:1378–1383. https://doi.org/10.1016/j.jhsa.2014.03.042
Remmers C, Hibbard J, Mosen DM et al (2009) Is patient activation associated with future health outcomes and healthcare utilization among patients with diabetes? J Ambul Care Manag 32:320–327. https://doi.org/10.1097/JAC.0b013e3181ba6e77
Eastwood D, Manson N, Bigney E et al (2019) Improving postoperative patient reported benefits and satisfaction following spinal fusion with a single preoperative education session. Spine J 19:840–845. https://doi.org/10.1016/j.spinee.2018.11.010
Parai C, Hägg O, Lind B, Brisby H (2019) ISSLS prize in clinical science 2020: the reliability and interpretability of score change in lumbar spine research. Eur Spine J. https://doi.org/10.1007/s00586-019-06222-8
Hibbard JH, Cunningham PJ (2008) How engaged are consumers in their health and health care, and why does it matter? Research Gate website. https://www.researchgate.net/profile/Judith_Hibbard/publication/23411858_How_Engaged_Are_Consumers_in_Their_Health_and_Health_Care_and_Why_Does_It_Matter/links/0912f50b4c6c464b19000000/How-Engaged-Are-Consumers-in-Their-Health-and-Health-Care-and-Why-Does-It-Matter.pdf. Accessed 27 Apr 2020
Linden A (2015) Estimating measurement error of the patient activation measure for respondents with partially missing data. Biomed Res Int 2015:270168. https://doi.org/10.1155/2015/270168
Funding
No funds were received in support of this work. No benefits in any form have been or will be received from any commercial party related directly or indirectly to the subject of this manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that the article and its content were composed in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Ethical approval
IRB Approval: ORA #14051301.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Jenkins, N.W., Parrish, J.M., Mohan, S. et al. Preoperative patient activation is predictive of improvements in patient-reported outcomes following minimally invasive lumbar decompression. Eur Spine J 29, 2222–2230 (2020). https://doi.org/10.1007/s00586-020-06512-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-020-06512-6