Abstract
Purpose
To assess the impact of problem and scripting-based learning (PSBL) on spine surgical trainees’ learning outcomes.
Methods
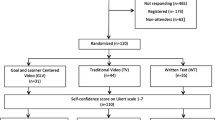
30 spine surgery postgraduate-year-1 residents (PGY-1s) from the First Hospital of China Medical University were randomly divided into two groups. The first group studied spine surgical skills and developed individual judgment under a conventional didactic model, whereas the PSBL group used PBL and Scripted model. A feedback questionnaire and the satisfaction of residents were evaluated by the first assistant surgeon immediately following each procedure. At the end of the study, residents filled out questionnaires focused on identifying the strengths of each teaching method and took a multiple-choice theoretical examination. The results were analyzed by t tests.
Results
Significant difference was found between the two groups in total mean score of preparedness and performance feedback statement (P = 0.01) and the questionnaire by PGY-1’s opinion on the effectiveness of the two teaching methods (P = 0.004). Compared with the non-PSBL group, the PSBL group had significantly higher mean score of pre-operative preparedness (P = 0.01), but there was no significant difference between the two groups in theoretical examination, intra-operative performance, and overall satisfaction with the PGY-1s. The residents found that PSBL could develop their judgment (P = 0.03) and provide greater satisfaction (P = 0.02), and would like to repeat the experience (P = 0.03).
Conclusions
The PSBL method can activate spine residents’ prior knowledge and building on existing cognitive frameworks, which is an important tool for improving pre-operative preparedness. We believe that PSBL is an important first step in training spine residents to become confident and safe spine surgeons.
Similar content being viewed by others
Abbreviations
- PSBL:
-
Problem and scripting-based learning
- PGY-1s:
-
Postgraduate-year-1 residents
- PBL:
-
Problem-based learning
References
Novick RJ, Lingard L, Cristancho SM (2015) The call, the save, and the threat: understanding expert help-seeking behavior during nonroutine operative scenarios. J Surg Educ 72:302–309. doi:10.1016/j.jsurg.2014.09.009
Gas BL, Mohan M, Jyot A, Buckarma EH, Farley DR (2016) Does scripting operative plans in advance lead to better preparedness of trainees? A pilot study. Am J Surg. doi:10.1016/j.amjsurg.2016.11.011
Neufeld VR, Barrows HS (1974) The “McMaster Philosophy”: an approach to medical education. J Med Educ 49:1040–1050
Kong J, Li X, Wang Y, Sun W, Zhang J (2009) Effect of digital problem-based learning cases on student learning outcomes in ophthalmology courses. Arch Ophthalmol 127:1211–1214. doi:10.1001/archophthalmol.2009.110
Neville AJ, Norman GR (2007) PBL in the undergraduate MD program at McMaster University: three iterations in three decades. Acad Med 82:370–374. doi:10.1097/ACM.0b013e318033385d
Finnesgard EJ, Aho JM, Pandian TK, Farley DR (2016) Effect of rehearsal modality on knowledge retention in surgical trainees: a pilot study. J Surg Educ 73:831–835. doi:10.1016/j.jsurg.2016.04.001
Friedman RJ, Haas S (2011) Strengths and limitations of standards of care to guide the orthopedic surgeon in VTE prevention. Orthopedics 34:121–128. doi:10.3928/01477447-20101221-25
Levy IM, Pryor KW, McKeon TR (2016) Is teaching simple surgical skills using an operant learning program more effective than teaching by demonstration? Clin Orthop Relat Res 474:945–955
Martin-Ferrero MA, Faour-Martin O, Simon-Perez C, Perez-Herrero M, de Pedro-Moro JA (2014) Ambulatory surgery in orthopedics: experience of over 10,000 patients. J Orthop Sci 19:332–338. doi:10.1007/s00776-013-0501-3
Zilbert NR, St-Martin L, Regehr G, Gallinger S, Moulton CA (2015) Planning to avoid trouble in the operating room: experts’ formulation of the preoperative plan. J Surg Educ 72:271–277. doi:10.1016/j.jsurg.2014.09.015
Ruetten S, Komp M, Merk H, Godolias G (2008) Full-endoscopic interlaminar and transforaminal lumbar discectomy versus conventional microsurgical technique: a prospective, randomized, controlled study. Spine (Phila Pa 1976) 33:931–939. doi:10.1097/BRS.0b013e31816c8af7
Dammers J, Spencer J, Thomas M (2001) Using real patients in problem-based learning: students’ comments on the value of using real, as opposed to paper cases, in a problem-based learning module in general practice. Med Educ 35:27–34
Kenny NP, Beagan BL (2004) The patient as text: a challenge for problem-based learning. Med Educ 38:1071–1079. doi:10.1111/j.1365-2929.2004.01956.x
Akhtar K, Sugand K, Sperrin M, Cobb J, Standfield N, Gupte C (2015) Training safer orthopedic surgeons. Construct validation of a virtual-reality simulator for hip fracture surgery. Acta Orthop 86:616–621
Gasco J, Patel A, Ortega-Barnett J, Branch D, Desai S, Kuo YF, Luciano C, Rizzi S, Kania P, Matuyauskas M, Banerjee P, Roitberg BZ (2014) Virtual reality spine surgery simulation: an empirical study of its usefulness. Neurol Res 36:968–973. doi:10.1179/1743132814y.0000000388
Berjano P, Villafañe JH, Vanacker G, Cecchinato R, Ismael M, Gunzburg R, Marruzzo D, Lamartina C (2016) The effect of case-based discussion of topics with experts on learners’ opinions: implications for spinal education and training. Eur Spine J. doi:10.1007/s00586-016-4860-2
Blencowe NS, Glasbey JC, McElnay PJ, Bhangu A, Gokani VJ, Harries RL, Council of the Association of Surgeons in Training (2017) Postgrad Med J. doi:10.1136/postgradmedj-2016-134737 (Epub ahead of print)
Brunckhorst O, Khan, Dasgupta P, Ahmed K (2017) Nontechnical skill training and the use of scenarios in modern surgical education. Curr Opin Urol. doi:10.1097/MOU.0000000000000402 (Epub ahead of print)
Okubo Y, Matsushita S, Takakuwa Y, Yoshioka T, Nitta K (2016) Longitudinal PBL in undergraduate medical education develops lifelong-learning habits and clinical competencies in social aspects. Tohoku J Exp Med 238:65–74. doi:10.1620/tjem.238.65
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study was supported by Doctor Research Startup Fund of Liaoning Province (201601114). The funders had no role in the study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Cong, L., Yan, Q., Sun, C. et al. Effect of problem and scripting-based learning on spine surgical trainees’ learning outcomes. Eur Spine J 26, 3068–3074 (2017). https://doi.org/10.1007/s00586-017-5135-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-017-5135-2