Abstract
Purpose
To investigate the causes of late-onset, progressive neurological deficits in patients with severe angular kyphosis caused by spondylitis secondary to tuberculosis (TB spondylitis).
Methods
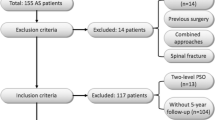
From 2000 to 2011, 36 patients with severe angular kyphosis secondary to TB spondylitis (TB kyphosis) were enrolled in the study. All patients had late-onset, progressive neurological deficits. The causes of these deficits were classified with respect to the level of the causative lesion. Group A (n = 25, 69.4 %) comprised patients whose neurological deficits resulted from the kyphosis itself. Patients in group B (n = 11, 30.6 %) had developed neurological symptoms related to a lesion cephalad or caudal from the kyphosis. Surgical intervention was performed in 23 patients; 13 patients were treated conservatively. Clinical outcomes were evaluated using the American Spinal Injury Association (ASIA) impairment scale.
Results
The late onset of neurological deficits was attributed to cord compression, pure cord distraction, stenosis, and instability above or below the level of the angular kyphosis. An improvement of the neurological symptoms at the cord level after surgical intervention, as indicated by a change from a non-ambulatory (ASIA impairment scale A/C) to an ambulatory (ASIA D/E) status, occurred in four of nine (44.4 %) surgically treated patients. However, only 2 of 10 (20.0 %) patients treated conservatively showed cord level improvement, as assessed using the ASIA impairment scale.
Conclusions
In their evaluation of paraplegic patients, spine surgeons should consider the many potential causes of late-onset neurological deficits in TB spondylitis to avoid performing unnecessary surgery. A simpler procedure may yield equivalent results.



Similar content being viewed by others
References
Moon MS, Moon JL, Kim SS, Moon YW (2007) Treatment of tuberculosis of the cervical spine. Operative versus nonoperative. Clin Orthop Relat Res 460:67–77
Jain AK (2010) Tuberculosis of the spine. A fresh look at an old disease. J Bone Joint Surg Br 92:905–913
Luk KD, Krishna M (1996) Spinal stenosis above a healed tuberculous kyphosis. A case report. Spine (Phila Pa 1976) 21:1098–1101
Chen Y, Lu XH, Yang LL, Chen DY (2009) Ossification of ligamentum flavum related to thoracic kyphosis after tuberculosis: case report and review. Spine (Phila Pa 1976) 34:E41–E44
Rajasekaran S (2007) Buckling collapse of the spine in childhood spinal tuberculosis. Clin Orthop Relat Res 460:86–92
Hodgson AR, Yau A (1967) Pott’s paraplegia: a classification based upon the living pathology. Paraplegia 5:1–16
Luk KDK (1999) Tuberculosis of the spine in the new millennium. Eur Spine J 8:338–345
Tuli SM (1995) Severe kyphotic deformity in tuberculosis of the spine. Int Orthop 19:327–331
Jain AK, Aggarwal PK, Arora A, Singh S (2004) Behaviors of the kyphotic angle in spinal tuberculosis. Int Orthop 28:110–114
Huang TJ, Hsu RW, Chen SH, Liu HP (2000) Video-assisted thoracoscopic surgery in managing tuberculous spondylitis. Clin Orhtop Relat Res 379:143–153
Kalra KP, Dhar SB, Shetty G, Dhariwal Q (2006) Pedicle subtraction osteotomy for rigid posttuberculous kyphosis. J Bone Joint Surg Br 888:925–927
Kalita J, Misra UK, Mandal SK, Srivastava M (2005) Prognosis of conservatively treated patients with Pott’s paraplegia: logistic regression analysis. J Neurol Neurosurg Psychiatry 76:866–868
Tuli SM (1975) Results of treatment of spinal tuberculosis by ‘middlepath’ regime. J Bone Joint Surg Br 57:13–23
Hsu LC, Cheung CL, Leong JC (1988) Pott’s paraplegia of late onset. The cause of compression and results after anterior decompression. J Bone Joint Surg Br 70:534–538
Rajeswari R, Ranjani R, Santha T, Sriram K, Prabhakar R (1997) Late onset paraplegia- a sequel to Pott’s disease. A report on imaging, prevention and management. Int J Tuebrc Lung Dis 1:468–473
Moon MS, Moon JL, Moon YW et al (2003) Pott’s paraplegia in patients with severely deformed dorsal or dorsolumbar spines: treatment and prognosis. Spinal Cord 41:164–171
Zhang Z (2012) Late onset Pott’s paraplegia in patients with upper thoracic sharp kyphosis. Int Orthop 36:381–385
Cheung WY, Luk KDK (2013) Clinical and radiological outcomes after conservative treatment of TB spondylitis: is the 15 years’ follow-up in the MRC study long enough? Eur Spine J 22:S594–S602
Moon MS, Ha KY, Sun DH et al (1996) Pott’s paraplegia-67 cases. Clin Orthop Relat Res 323:122–128
Suk SI, Kim JH, Kim WJ et al (2002) Posterior vertebral column resection for severe spinal deformities. Spine (Phila Pa 1976) 27:2374–2382
Bridwell KH, Lewis SJ, Lenke LG, Baldus C, Blanke K (2003) Pedicle subtraction osteotomy for the treatment of fixed sagittal imbalance. J Bone Joint Surg Am 85:454–463
Wang Y, Zhang Y, Zhang X et al (2008) A single posterior approach for multilevel modified vertebral column resection in adults with severe rigid congenital kyphoscoliosis: a retrospective study of 13 cases. Eur Spine J 17:361–372
Kawahara N, Tomita K, Baba H et al (2001) Closing-opening wedge osteotomy to correct angular kyphotic deformity by a single posterior approach. Spine (Phila Pa 1976) 26:391–402
Rajasekaran S, Rishi M, Kanna P, Shetty AP (2010) Closing–opening wedge osteotomy for severe, rigid, thoracolumbar post-tubercular kyphosis. Eur Spine J 20:343–348
Winter RB (1997) Neurologic safety in spinal deformity surgery. Spine (Phila Pa 1976) 22:1527–1533
Buchowski JM, Bridwell KH, Lenke LG et al (2007) Neurological complications of lumbar pedicle subtraction osteotomy. a 10-year assessment. Spine (Phila Pa 1976) 32:2245–2252
Bezer M, Kucukdurmaz F, Guven D (2007) Transpedicular decancellation osteotomy in the treatment of posttuberculous kyphosis. J Spinal Disord Tech 20:209–215
Rajasekaran S (2012) Kyphotic deformity in spinal tuberculosis and its management. Int Orthop 36:359–365
Boachie-Adjei O, Papadopoulos EC, Pellisé F et al (2013) Late treatment of tuberculosis-associated kyphosis: literature review and experience from a SRS-GOP site. Eur Spine J 22(Suppl 4):S641–S646
Conflict of interest
We declare that none of the authors have conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ha, KY., Kim, YH. Late onset of progressive neurological deficits in severe angular kyphosis related to tuberculosis spondylitis. Eur Spine J 25, 1039–1046 (2016). https://doi.org/10.1007/s00586-015-3997-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-015-3997-8