Abstract
Introduction

Despite numerous descriptive publications, the guidelines for treatment of cervical spinal tuberculosis (TB) are not very clear. The authors report a case of a young girl with cervico-thoracic spinal TB extending from C5 to T3 vertebrae presenting with weakness of the right hand and unsteady gait.
Case report
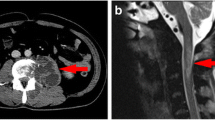
An 11-year-old female who is an immigrant to the UK from Afghanistan, presented to our clinic with a 10-day history of difficulty in walking with an unsteady gait and 3-month history of progressive weakness in both her arms, the right side more affected than the left. Her immunisation history was unclear. Examination of the arms showed bilateral thenar and hypothenar wasting, more so on the right than the left. An MRI scan revealed a large para-spinal abscess extending from C3/4 to T4/5 with a significant anterior epidural cord compression from C5/6 to T2/3. Therapeutic/diagnostic aspiration was performed under ultrasound guidance and the aspirate was sent for microbiology. She was started empirically on multidrug anti-tubercular treatment and steroids. Although Ziehl–Neelsen stain was negative for acid-fast bacilli, microbiological confirmation of TB was obtained by positive TB culture sensitive to all first-line anti-TB drugs. She made a dramatic improvement within 3 weeks of anti-tubercular treatment. A follow-up MRI scan at 8 months showed complete resolution of the abscess. At 2 years of follow-up, she was a healthy looking child, back to her school with no residual clinical signs/symptoms of the disease.
Conclusion
Our case of cervico-thoracic tuberculous abscess in a young child suggests that even with incomplete neurological deficit caused by epidural cord compression, ultrasound (or CT)-guided aspiration and anti-tubercular medication provide acceptable results at 2 years of follow-up.



Similar content being viewed by others
References
Derry DC (1938) Pott’s disease in ancient Egypt. Med Pres Circ 197:196–199
Arriaza BT, Salo W, Aufderheide AC, Holcomb TA (1995) Pre-Columbian tuberculosis in northern Chile: molecular and skeletal evidence. Am J Phys Anthropol 98:37
Pott P (2002) The chirurgical works of Percival Pott, FRS, surgeon to St. Bartholomew’s Hospital, a new edition, with his last corrections. 1808. Clin Orthop Relat Res 398:4–10
Dara M, Dadu A, Kremer K, Zaleskis R, Kluge HH (2012) Epidemiology of tuberculosis in WHO European Region and public health response. Eur Spine J, May 8 [Epub ahead of print]
Rasool MN (2001) Osseous manifestations of tuberculosis in children. J Pediatr Orthop 21(6):749–755
Teo HE, Peh WC (2004) Skeletal tuberculosis in children. Pediatr Radiol 34(11):853–860
Pellisé F (2012) Tuberculosis and Pott’s disease, still very relevant health problems. Eur Spine J, Oct 9 [Epub ahead of print]
Millet JP, Moreno A, Fina L et al (2012) Factors that influence current tuberculosis epidemiology. Eur Spine J, May 8 [Epub ahead of print]
Berney S, Goldstein M, Bishko F (1972) Clinical and diagnostic features of tuberculous arthritis. Am J Med 53:36–42
Moore SL, Rafii M (2001) Imaging of musculoskeletal and spinal tuberculosis. Radiol Clin North Am 39:329–342
Fitzgerald D, Haas DW (2005) Mycobacterium tuberculosis. In: Mandell GL, Bennett JE, Dolin R (eds) Mandell, Douglas, and Bennett’s: principles and practice of infectious diseases, 6th edn. Philadelphia, Elsevier Churchill, Livingstone, pp 2852–2886
Diagnostic standards and classification of tuberculosis in adults and children. This official statement of the American Thoracic Society and the Centres for Disease Control and Prevention was adopted by the ATS Board of Directors, July 1999 (2000) This statement was endorsed by the Council of the Infectious Disease Society of America, September 1999. Am J Respir Crit Care Med 161:1376–1395
Mondal A (1994) Cytological diagnosis of vertebral tuberculosis with fine-needle aspiration biopsy. J Bone Joint Surg Am 76:181–184
Pablos-Mendez A, Raviglione MC, Laszlo A (1998) Global surveillance for antituberculosis-drug resistance, 1994–1997. World Health Organization–International Union against tuberculosis and lung disease Working Group on anti-tuberculosis drug resistance surveillance. N Engl J Med 338:1641–1649
Mohan K, Rawall S, Pawar UM et al (2012) Drug resistance patterns in 111 cases of drug-resistant tuberculosis spine. Eur Spine J, May 11 [Epub ahead of print]
Pertuiset E, Beaudreuil J, Liote F et al (1999) Spinal tuberculosis in adults. A study of 103 cases in a developed country, 1980–1994. Medicine 78:309–320
Dass B, Puet TA, Watanakunakorn C (2002) Tuberculosis of the spine (Potts disease) presenting as compression fractures. Spinal Cord 40:604–608
Hassan MG (2003) Anterior plating for lower cervical spine tuberculosis. Int Orthop 27:73–77
Jain AK, Kumar S, Tuli SM (1999) Tuberculosis of spine (C1–D4). Spinal Cord 37:362–369
Loembe P (1994) Tuberculosis of the lower cervical spine (C3–C7) in adults; diagnostic and surgical aspects. Acta Neurochir 131:125–129
Lukhele M (1996) Tuberculosis of the cervical spine. S Afr Med J 86:553–556
Moon MS, Ha KY, Sun DH, Moon JL, Moon YW, Chung JH (1996) Pott’s Paraplegia–67 cases. Clin Orthop Relat Res 323:122–128
Sinha S, Singh AK, Gupta V, Singh D, Takayasu M, Yoshida J (2003) Surgical management and outcome of tuberculous atlantoaxial dislocation: a 15-year experience. Neurosurgery 52:331–339
Ramani PS, Sharma A, Jituri S et al (2005) Anterior instrumentation for cervical spine tuberculosis: an analysis of surgical experience with 61 cases. Neurol India 53:83–89 (discussion 89)
Al Soub H (1996) Retropharyngeal abscess associated with tuberculosis of the cervical spine. Tuber Lung Dis 77(6):563–565
Boxer DI, Pratt C, Hine AL, McNicol M (1992) Radiological features during and following treatment of spinal tuberculosis. Br J Radiol 65:476–479
Rahman I, Bhatt H, Chillag S, Duffus W (2009) Mycobacterium chelonae vertebral osteomyelitis. South Med J 102(11):1167–1169
Petitjean G, Fluckiger U, Schären S (2004) Vertebral osteomyelitis caused by non-tuberculous mycobacteria. Clin Microbiol Infect 10(11):951–953
Solera J, Lozano E, Martínez-Alfaro E, Espinosa A, Castillejos ML, Abad L (1999) Brucellar spondylitis: review of 35 cases and literature survey. Clin Infect Dis 29(6):1440–1449
Moon MS, Moon JL, Kim SS, Moon YW (2007) Treatment of tuberculosis of the cervical spine: operative versus nonoperative. Clin Orthop Relat Res 460:67–77
Moon MS (1997) Tuberculosis of the spine; controversies and new challenges: spine update. Spine 22:1791–1797
Hsu LC, Leong JC (1984) Tuberculosis of the lower cervical spine (C2 to C7): a report on 40 cases. J Bone Joint Surg Br 66:1–5
Delogu G, Zumbo A, Fadda G (2012) Microbiological and immunological diagnosis of tuberculous spondylodiscitis. Eur Rev Med Pharmacol Sci 16(Suppl 2):73–78
Acosta FL Jr, Chin CT, Quiñones-Hinojosa A, Ames CP, Weinstein PR, Chou D (2004) Diagnosis and management of adult pyogenic osteomyelitis of the cervical spine. Neurosurg Focus 17(6):E2
McClay JE, Murray AD, Booth T (2003) Intravenous antibiotic therapy for deep neck abscesses defined by computed tomography. Arch Otolaryngol Head Neck Surg 129(11):1207–1212
Upadhyay SS, Saji MJ, Sell P, Hsu LC, Yau AC (1996) The effect of age on the change in deformity after anterior debridement surgery for tuberculosis of the spine. Spine 21:2356–2362
Cheung WY, Luk KD (2012) Clinical and radiological outcomes after conservative treatment of TB spondylitis: is the 15 years’ follow-up in the MRC study long enough? Eur Spine J, May 8 (Epub ahead of print)
Luk KD (1999) Tuberculosis of the spine in the new millennium. Eur Spine J 8(5):338–345
Prabhakar MM, Thakker T (2006) Anterior decompression for cervico-thoracic pathology: a study of 14 patients. J Spinal Cord Med 29:163–166
Pointillart V, Aurouer N, Gangnet N et al (2007) Anterior approach to the cervico-thoracic junction without sternotomy: a report of 37 cases. Spine 32:2875–2879
Govender S, Parbhoo AH, Kumar KP (2001) Tuberculosis of the cervicodorsal junction. J Pediatr Orthop 21:285–287
Fountain SS, Hsu LC, Yau AC, Hodgson AR (1975) Progressive kyphosis following solid anterior spine fusion in children with tuberculosis of the spine. J Bone Joint Surg Am 57:1104–1107
Schulitz KP, Kothe R, Leong JC, Wehling P (1997) Growth changes of solidly fused kyphotic bloc after surgery for tuberculosis: comparison of four procedures. Spine 22:1150–1155
Conflict of interest
No benefits or funds in any form have been received or will be received from a commercial party related directly or indirectly to the subject of this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Manoharan, S.R., Leitao, J., Emberton, P. et al. A large tuberculosis abscess causing spinal cord compression of the cervico-thoracic region in a young child. Eur Spine J 22, 1459–1463 (2013). https://doi.org/10.1007/s00586-013-2729-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-013-2729-1