Abstract
Purpose
To determine whether motion preservation following oblique cervical corpectomy (OCC) for cervical spondylotic myelopathy (CSM) persists with serial follow-up.
Methods
We included 28 patients with preoperative and at least two serial follow-up neutral and dynamic cervical spine radiographs who underwent OCC for CSM. Patients with an ossified posterior longitudinal ligament (OPLL) were excluded. Changes in sagittal curvature, segmental and whole spine range of motion (ROM) were measured. Nathan’s system graded anterior osteophyte formation. Neurological function was measured by Nurick’s grade and modified Japanese Orthopedic Association (JOA) scores.
Results
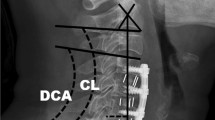
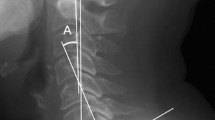
The majority (23 patients) had a single or 2-level corpectomy. The average duration of follow-up was 45 months. The Nurick’s grade and the JOA scores showed statistically significant improvements after surgery (p < 0.001). 17 % of patients with preoperative lordotic spines had a loss of lordosis at last follow-up, but with no clinical worsening. 77 % of the whole spine ROM and 62 % of segmental ROM was preserved at last follow-up. The whole spine and segmental ROM decreased by 11.2° and 10.9°, respectively (p ≤ 0.001). Patients with a greater range of segmental movement preoperatively had a statistically greater range of movement at follow-up. The analysis of serial radiographs indicated that the range of movement of the whole spine and the range of movement at the segmental spine levels significantly reduced during the follow-up period. Nathan’s grade showed increase in osteophytosis in more than two-thirds of the patients (p ≤ 0.01). The whole spine range of movement at follow-up significantly correlated with Nathan’s grade.
Conclusions
Although the OCC preserves segmental and whole spine ROM, serial measurements show a progressive decrease in ROM albeit without clinical worsening. The reduction in this ROM is probably related to degenerative ossification of spinal ligaments.

Similar content being viewed by others
Abbreviations
- CSM:
-
Cervical spondylotic myelopathy
- GE:
-
General electric
- JOA:
-
Japanese Orthopedic Association
- MRI:
-
Magnetic resonance imaging
- OCC:
-
Oblique cervical corpectomy
- OPLL:
-
Ossified posterior longitudinal ligament
- PACS:
-
Picture archival and retrieval system
- ROM:
-
Range of movement
- VA:
-
Vertebral artery
References:
Liu Y, Qi M, Chen H, Yang L, Wang X, Shi G, Gao R, Wang C, Yuan W (2012) Comparative analysis of complications of different reconstructive techniques following anterior decompression for multilevel cervical spondylotic myelopathy. Eur Spine J 21(12):2428–2435. doi:10.1007/s00586-012-2323-y
Rajshekhar V, Muliyil J (2007) Patient perceived outcome after central corpectomy for cervical spondylotic myelopathy. Surg Neurol 68:185–190. doi:10.1016/j.surneu.2006.10.071 discussion 190-181
Houten JK, Cooper PR (2003) Laminectomy and posterior cervical plating for multilevel cervical spondylotic myelopathy and ossification of the posterior longitudinal ligament: effects on cervical alignment, spinal cord compression, and neurological outcome. Neurosurgery 52:1081–1097. doi:10.1227/01.NEU.0000057746.74779.55
Song KJ, Lee KB, Song JH (2012) Efficacy of multilevel anterior cervical discectomy and fusion versus corpectomy and fusion for multilevel cervical spondylotic myelopathy: a minimum 5-year follow-up study. Eur Spine J 21(8):1551–1557. doi:10.1007/s00586-012-2296-x
Costa F, Tomei M, Sassi M, Cardia A, Ortolina A, Servello D, Fornari M (2012) Evaluation of the rate of decompression in anterior cervical corpectomy using an intra-operative computerized tomography scan (O-Arm system). Eur Spine J 21(2):359–363. doi:10.1007/s00586-011-2028-7
Lin Q, Zhou X, Wang X, Cao P, Tsai N, Yuan W (2011) A comparison of anterior cervical discectomy and corpectomy in patients with multilevel cervical spondylotic myelopathy. Eur Spine J 21(3):474–481. doi:10.1007/s00586-011-1961-9
Kristof RA, Kiefer T, Thudium M, Ringel F, Stoffel M, Kovacs A, Mueller CA (2009) Comparison of ventral corpectomy and plate-screw-instrumented fusion with dorsal laminectomy and rod-screw-instrumented fusion for treatment of at least two vertebral-level spondylotic cervical myelopathy. Eur Spine J 18(12):1951–1956. doi:10.1007/s00586-009-1110-x
Bruneau M, Cornelius JF, George B (2007) Multilevel oblique corpectomies: surgical indications and technique. Neurosurgery 61:106–112. doi:10.1227/01.neu.0000289723.89588.72 discussion 112
Chacko AG, Daniel RT (2007) Multilevel cervical oblique corpectomy in the treatment of ossified posterior longitudinal ligament in the presence of ossified anterior longitudinal ligament. Spine 32(20):E575–E580. doi:10.1097/BRS.0b013e31814b84fe
Chibbaro S, Mirone G, Makiese O, George B (2009) Multilevel oblique corpectomy without fusion in managing cervical myelopathy: long-term outcome and stability evaluation in 268 patients. J Neurosurg Spine 10(5):458–465. doi:10.3171/2009.1.SPINE08186
Kiris T, Kilincer C (2008) Cervical spondylotic myelopathy treated by oblique corpectomy: a prospective study. Neurosurgery 62(3):674–682. doi:10.1227/01.neu.0000317316.56235.a7 discussion 674–682
Koc RK, Menku A, Akdemir H, Tucer B, Kurtsoy A, Oktem IS (2004) Cervical spondylotic myelopathy and radiculopathy treated by oblique corpectomies without fusion. Neurosurg Rev 27(4):252–258. doi:10.1007/s10143-004-0322-0
Moses V, Daniel RT, Chacko AG (2010) The value of intraoperative ultrasound in oblique corpectomy for cervical spondylotic myelopathy and ossified posterior longitudinal ligament. Br J Neurosurg 24:518–525. doi:10.3109/02688697.2010.504049
Turel MK, Chacko AG (2011) Delayed resolution of extensive T2-weighted intramedullary signal changes after oblique corpectomy for cervical spondylotic myelopathy. Br J Neurosurg 25(6):772–774. doi:10.3109/02688697.2011.584989
Rocchi G, Caroli E, Salvati M, Delfini R (2005) Multilevel oblique corpectomy without fusion: our experience in 48 patients. Spine 30(17):1963–1969. doi:10.1097/01.brs.0000176327.04725.1b
George B, Gauthier N, Lot G (1999) Multisegmental cervical spondylotic myelopathy and radiculopathy treated by multilevel oblique corpectomies without fusion. Neurosurgery 44(1):81–90. doi:10.1097/00006123-199901000-00046
Chacko AG, Joseph M, Turel MK, Prabhu K, Daniel RT, Jacob KS (2012) Multilevel oblique corpectomy for cervical spondylotic myelopathy preserves segmental motion. Eur Spine J 21(7):1360–1367. doi:10.1007/S00586-011-2137-3
Nurick S (1972) The pathogenesis of the spinal cord disorder associated with cervical spondylosis. Brain 95(1):87. doi:10.1093/brain/95.1.87
Benzel EC, Lancon J, Kesterson L, Hadden T (1991) Cervical laminectomy and dentate ligament section for cervical spondylotic myelopathy. J Spinal Disord Tech 4(3):286. doi:10.1097/00002517-199109000-00005
Nathan H (1962) Osteophytes of the Vertebral Column An Anatomical Study of Their Development According to Age, Race, and Sex with Considerations as to Their Etiology and Significance. J Bone Joint Surg Am 44:243–268
Cagli S, Chamberlain RH, Sonntag VK, Crawford NR (2004) The biomechanical effects of cervical multilevel oblique corpectomy. Spine 29(13):1420–1427. doi:10.1097/01.BRS.0000129896.80044.B6
Simpson AK, Biswas D, Emerson JW, Lawrence BD, Grauer JN (2008) Quantifying the effects of age, gender, degeneration, and adjacent level degeneration on cervical spine range of motion using multivariate analyses. Spine 33:183–186. doi:10.1097/BRS.0b013e31816044e8
Choi D, Melcher R, Harms J, Crockard A (2010) Outcome of 132 operations in 97 patients with chordomas of the craniocervical junction and upper cervical spine. Neurosurgery 66(1):59–65. doi:10.1227/01.NEU.0000362000.35742.3D
Lee SE, Chung CK, Jahng TA (2012) Early development and progression of heterotopic ossification in cervical total disc replacement. J Neurosurg Spine 16(1):31–36. doi:10.3171/2011.8.SPINE11303
Baba H, Furusawa N, Imura S, Kawahara N, Tsuchiya H, Tomita K (1993) Late radiographic findings after anterior cervical fusion for spondylotic myeloradiculopathy. Spine 18(15):2167–2173
Shin DA, Yi S, Yoon DH, Kim KN, Shin HC (2009) Artificial disc replacement combined with fusion versus two-level fusion in cervical two-level disc disease. Spine 34(11):1153–1159. doi:10.1097/BRS.0b013e31819c9d39
Vedantam A, Revanappa KK, Rajshekhar V (2011) Changes in the range of motion of the cervical spine and adjacent segments at ≥24 months after uninstrumented corpectomy for cervical spondylotic myelopathy. Acta Neurochir (Wien) 153(5):995–1001. doi:10.1007/s00701-011-0986-5
Kadaňka Z, Bednařík J, Novotný O, Urbánek I, Dušek L (2011) Cervical spondylotic myelopathy: conservative versus surgical treatment after 10 years. Eur Spine J 20(9):1533–1538. doi:10.1007/s00586-011-1811-9
Nakamura K, Kurokawa T, Hoshino Y, Saita K, Takeshita K, Kawaguchi H (1998) Conservative Treatment for Cervical Spondylotic Myelopathy: achievement and Sustainability of a Level of “No Disability”. J Spinal Disord 11(2):175–179
Upadhyaya CD, Wu JC, Trost G, Haid RW, Traynelis VC, Tay B, Coric D, Mummaneni PV (2012) Analysis of the three United States Food and Drug Administration investigational device exemption cervical arthroplasty trials. J Neurosurg Spine 16(3):216–228. doi:10.3171/2011.6.SPINE10623
Goffin J, van Loon J, Van Calenbergh F, Plets C (1995) Long-term results after anterior cervical fusion and osteosynthetic stabilization for fractures and/or dislocations of the cervical spine. J Spinal Disord 8(6):500–508 discussion 499
Richards O, Choi D, Timothy J (2012) Cervical arthroplasty: the beginning, the middle, the end? Br J Neurosurg 26(1):2–6. doi:10.3109/02688697.2011.595846
Acknowledgments
The authors would like to acknowledge Debashree Turel and Dr K. Srinivas Babu for their assistance in the artwork.
Conflict of interest
The authors report no financial support or conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Turel, M.K., Sarkar, S., Prabhu, K. et al. Reduction in range of cervical motion on serial long-term follow-up in patients undergoing oblique corpectomy for cervical spondylotic myelopathy. Eur Spine J 22, 1509–1516 (2013). https://doi.org/10.1007/s00586-013-2724-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-013-2724-6