Abstract

Introduction
Anterior access to the lumbar spine is established for disc replacement surgery and anterior interbody fusion in the lumbar spine. The spine is accessed normally from the left side either by a transperitoneal or retroperitoneal approach through a midline or oblique skin incision. After reaching the retroperitoneum and depending on the level of exposure, the surgeon has to mobilise and retract the aorta or left common iliac artery, as well as the left common iliac vein or internal vena cava to the right lateral border to address the whole disc space. The left common iliac artery is especially stretched during intervertebral disc exposure putting it at a greater risk of adverse events. Not surprisingly, vascular adverse events like direct injuries, thrombosis and embolism are feared complications in anterior surgery. Permanent intra-operative left leg oxygen saturation surveillance via pulse oximetry can help detecting embolic situations thereby allowing immediate treatment minimising the leg ischemia or preventing limb loss.
Case report
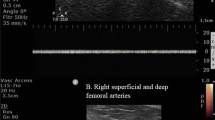
In the presented case, a 61-year-old male patient undergoing a two-level anterior interbody fusion lost oxygen saturation in the left leg after vessel retraction for exposure. After cage insertion and release of the retractor blades, the pulse oximetry signal did not return and no pulses were found during instant Doppler investigation below the femoral artery, indicating severe embolism in the left leg. The left common iliac artery was clamped and opened showing a ruptured calcified plaque with adherent fresh thrombotic material. An endovascular embolectomy in the superficial and deep femoral artery revealed several small thrombi. An artherectomy of the common iliac artery followed by patch closure was performed. Immediately after clamp release, pulse oximetry returned and Doppler signals were detectable at the tibialis posterior and dorsalis pedis artery. Post-operative recovery was uneventful and pulses were palpable at all times.
Conclusion
Arterial adverse events in anterior access surgery are rare complications but none the less, it is of paramount importance to detect and treat these situations immediately. This case highlights the need of routine pulse monitoring during the whole anterior surgery to prevent embolic complications. Even manual pulse control might not be sufficient to rule out any distal embolic events creating severe leg ischemia.







Similar content being viewed by others
References
Mayer HM (2000) The ALIF concept. Eur Spine J 9:35–43
Brau SA (2002) Mini-open approach to the spine for anterior lumbar interbody fusion: description of the procedure, results and complication. Spine J 2(3):216–223
Brau SA, Delamarter RB, Schiffman ML, Williams LA, Watkins RG (2004) Vascular injury during anterior lumbar surgery. Spine J 4(4):409–412
Garg J, Woo K, Hirsch J, Bruffey JD, Dilley RB (2010) Vascular complications of exposure for anterior lumbar interbody fusion. J Vasc Surg 51(4):946–950
Fantini GA, Pappou IP, Girardi FP, Sandhu HS, Cammisa FP Jr (2007) Major vascular injury during anterior lumbar spinal surgery: incidence, risk factors, and management. Spine 32(24):2751–2758
Wood KB, Devine J, Fischer D, Dettori JR, Janssen M (2010) Vascular injury in elective anterior lumbosacral surgery. Spine 35(9 Suppl):S66–S75
Rajaraman V, Vingan R, Roth P, Heary RF, Conklin L, Jacobs GB (1999) Visceral and vascular complications resulting from anterior lumbar interbody fusion. J Neurosurg 91(1 Suppl):60–64
Oskouian RJ Jr, Johnson JP (2002) Vascular complications in anterior thoracolumbar spinal reconstruction. J Neurosurg 96(1 Suppl):1–5
Hamdan AD, Malek JY, Schermerhorn ML, Aulivola B, Blattman SB, Pomposelli FB Jr (2008) Vascular injury during anterior exposure of the spine. J Vasc Surg 48(3):650–654
Bingol H, Cingoz F, Yilmaz AT, Yasar M, Tatar H (2004) Vascular complications related to lumbar disc surgery. J Neurosurg 100(3 Suppl Spine):249–253
Brau SA, Delamarter RB, Schiffman ML, Williams LA, Watkins RG (2004) Left iliac artery thrombosis during anterior lumbar surgery. Ann Vasc Surg 18(1):48–51
Brau SA, Spoonamore MJ, Snyder L, Gilbert C, Rhonda G, Williams LA, Watkins RG (2003) Nerve monitoring changes related to iliac artery compression during anterior lumbar spine surgery. Spine J 3(5):351–355
Kulkarni SS, Lowery GL, Ross RE, Ravi Sankar K, Lykomitros V (2003) Arterial complications following anterior lumbar interbody fusion: report of eight cases. Eur Spine J 12(1):48–54
Kim JS, Choi KC, Jung B, Lee SH (2009) Thrombosis of the left common iliac artery following lumber interbody fusion: Case report and review of the literature. J Korean Neurosurg Soc 45(4):249–252
Marsicano J, Mirovsky Y, Remer S, Bloom N, Neuwirth M (1994) Thrombotic occlusion of the left common iliac artery after an anterior retroperitoneal approach to the lumbar spine. Spine 19(3):357–359
Raskas DS, Delamarter RB (1997) Occlusion of the left iliac artery after retroperitoneal exposure of the spine. Clin Orthop Relat Res 338:86–89
Hackenberg L, Liljenqvist U, Halm H, Winkelmann W (2001) Occlusion of the left common iliac artery and consecutive thromboembolism of the left popliteal artery following anterior lumbar interbody fusion. J Spinal Disord 14(4):365–368
Khazim R, Boos N, Webb JK (1998) Progressive thrombotic occlusion of the left common iliac artery after anterior lumbar interbody fusion. Eur Spine J 7(3):239–241
Cappuccino A, Cornwall GB, Turner AW, Fogel GR, Duong HT, Kim KD, Brodke DS (2010) Biomechanical analysis and review of lateral lumbar fusion constructs. Spine 35(26 Suppl):S361–S367
Videbaek TS, Bünger CE, Henriksen M, Neils E, Christensen FB (2011) Sagittal spinal balance after lumbar spinal fusion: the impact of anterior column support results from a randomized clinical trial with an 8–13-year radiographic follow-up. Spine 36(3):183–191
Conflict of interest
No benefits or funds in any form have been received or will be received from a commercial party related directly or indirectly to the subject of this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
König, M.A., Leung, Y., Jürgens, S. et al. The routine intra-operative use of pulse oximetry for monitoring can prevent severe thromboembolic complications in anterior surgery. Eur Spine J 20, 2097–2102 (2011). https://doi.org/10.1007/s00586-011-1900-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-011-1900-9