Abstract
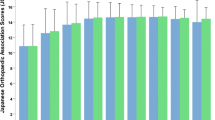
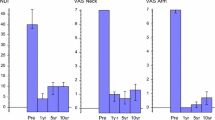
The interest in cervical total disc replacement (TDR) as an alternative to the so-far gold standard in the surgical treatment of degenerative disc disease (DDD), e.g anterior cervical discectomy and fusion (ACDF), is growing very rapidly. Many authors have established the fact that ACDF may result in progressive degeneration in adjacent segments. On the contrary, but still theoretically, preservation of motion with TDR at the surgically treated level may potentially reduce the occurrence of adjacent-level degeneration (ALD). The authors report the intermediate results of an undergoing multicentre prospective study of TDR with Mobi-C® prosthesis. The aim of the study was to assess the safety and efficacy of the device in the treatment of DDD and secondary to evaluate the radiological status of adjacent levels and the occurrence of ossifications, at 2-year follow-up (FU). 76 patients have performed their 2-year FU visit and have been analyzed clinically and radiologically. Clinical outcomes (NDI, VAS, SF-36) and ROM measurements were analyzed pre-operatively and at the different post-operative time-points. Complications and re-operations were also assessed. Occurrences of heterotopic ossifications (HOs) and of adjacent disc degeneration radiographic changes have been analyzed from 2-year FU X-rays. The mean NDI and VAS scores for arm and neck are reduced significantly at each post-operative time-point compared to pre-operative condition. Motion is preserved over the time at index levels (mean ROM = 9° at 2 years) and 85.5% of the segments are mobile at 2 years. HOs are responsible for the fusion of 6/76 levels at 2 years. However, presence of HO does not alter the clinical outcomes. The occurrence rate of radiological signs of ALD is very low at 2 years (9.1%). There has been no subsidence, no expulsion and no sub-luxation of the implant. Finally, after 2 years, 91% of the patients assume that they would undergo the procedure again. These intermediate results of TDR with Mobi-C® are very encouraging and seem to confirm the efficacy and the safety of the device. Regarding the preservation of the status of the adjacent levels, the results of this unconstrained device are encouraging, but longer FU studies are needed to prove it.









Similar content being viewed by others
References
Anderson P, Sasso RC, Riew KD (2007) Update on cervical artificial disk replacement. Instr Course Lect 56:237–245
Baba H, Furusawa N, Imura S, Kawahara N, Tsuchiya H, Tomita K (1993) Late radiographic findings after anterior cervical fusion for spondylotic myeloradiculopathy. Spine 18:2167–2173
Beaurain J, Bernard P, Dufour T, Fuentes JM, Hovorka I, Huppert J, Steib JP, Vital JM (2008) Mobi-C. In : Yue JJ, Bertagnoli R, McAfee P, An HS (eds) Motion preservation surgery of the spine: advanced techniques and controversies. Part III, Chap 27, Elsevier, Philadelphia, pp 231–237
Bernard P, Vital JM, Dufour T, Beaurain J, Fuentes JM, Huppert J, Hovorka I (2006) A new cervical disc prosthesis: Mobi-C. Preliminary results of a prospective study. In: Szpalski M, Gunzburg R, Le Huec JC, Brayda-Bruno M (eds) Non-fusion technologies in spine surgery. Lippincott Williams & Wilkins, pp 253–260
Bertagnoli R, Yue J, Pfeiffer F, Fenk-Mare A, Lawrence J, Kershaw T, Nanieva R (2005) Early results after Prodisc-C cervical disc replacement. J Neurosurg Spine 2:403–410
Bryan V (2002) Cervical motion segment replacement. Eur Spine J 11:S92–S97. doi:10.1007/s00586-002-0389-7
Cummins BH, Robertson JT, Gill SS (1998) Surgical experience with an implanted artificial cervical joint. J Neurosurg 88(6):943–948
Cappuccino A, Bellera F (2004) Clinical experience with the new PCM (Cervitech) Disc. Spine J 4:315S–321S. doi:10.1016/j.spinee.2004.07.024
Cote P, Cassidy JD, Yong-Hing K, Sibley J, Loewy J (1997) Apophysial joint degeneration, disc degeneration, and sagittal curve of the cervical spine. Can they be measured reliably on radiographs? Spine 22:859–864. doi:10.1097/00007632-199704150-00007
Dmitriev A, Cunningham B, Nianbin H, Sell G, Vigna F, McAfee P (2005) Adjacent level intradiscal pressure and segmental kinematics following a cervical total disc arthroplasty: an in vitro human cadaveric model. Spine 30:1165–1172. doi:10.1097/01.brs.0000162441.23824.95
Duggal N, Pickett G, Mitsis D, Keller J (2004) Early clinical and biomechanical results following cervical arthroplasty. Neurosurg Focus 17:E9. doi:10.3171/foc.2004.17.3.9
Eck JC, Humphreys SC, Lim TH, Jeong ST, Kim JG, Hodges SD, An HS (2002) Biomechanical study on the effect of cervical spine fusion on adjacent-level intradiscal pressure and segmental motion. Spine 27:2431–2434. doi:10.1097/00007632-200211150-00003
Fijn R, Koorevaar RT, Brouwers JR (2003) Prevention of heterotopic ossification after total hip replacement with NSAIDs. Pharm World Sci 25:138–145. doi:10.1023/A:1024830213832
Fransen M, Neal B (2004) Non-steroidal anti-inflammatory drugs for preventing heterotopic bone formation after hip arthroplasty. Cochrane Database Syst Rev 3:CD001160
Goffin J, Casey A, Kehr P, Liebig K, Lind B, Logroscino C, Pointillart V, Van Calenbergh F, van Loon J (2002) Preliminary clinical experience with the Bryan cervical disc prosthesis. Neurosurgery 51:840–845. doi:10.1097/00006123-200209000-00048
Goffin J, Van Calenbergh F, Von Loon J, Casey A, Kehr P, Liebig K, Lind B, Logroscino C, Sgrambiglia R, Pointillart V (2003) Intermediate follow-up after treatment of degenerative disc disease with the Bryan cervical disc prosthesis: single-level and bi-level. Spine 28:2673–2678. doi:10.1097/01.BRS.0000099392.90849.AA
Gore D, Sepic S, Gardner G (1986) Roentgenographic findings of the cervical spine in asymptomatic people. Spine 11:521–524. doi:10.1097/00007632-198607000-00003
Harrop JS, Youssef JA, Maltenfort M, Vorwald P, Jabbour P, Bono CM, Goldfarb N, Vaccaro AR, Hilibrand AS (2008) Lumbar adjacent segment degeneration and disease after arthrodesis and total disc arthroplasty. Spine 33:1701–1707
Hilibrand AS, Carlson GD, Palumbo MA, Jones PK, Bohlman HH (1999) Radiculopathy and myelopathy at segments adjacent to the site of a previous anterior cervical arthrodesis. J Bone Joint Surg Am 81:519–528
Hilibrand AS, Robbins M (2004) Adjacent segment degeneration and adjacent segment disease: the consequences of spinal fusion? Spine J 4:190S–194S. doi:10.1016/j.spinee.2004.07.007
Kettler A, Wilke H-J (2006) Review of existing grading systems for cervical or lumbar disc and facet joint degeneration. Eur Spine J 15:705–718. doi:10.1007/s00586-005-0954-y
Kim SH, Shin HC, Shin DA, Kim KN, Yoon DH (2007) Early clinical experience with the Mobi-C disc prosthesis. Yonsei Med J 48:457–464. doi:10.3349/ymj.2007.48.3.457
McAfee PC, Cunningham BW, Dmitriev A, Hu N, Woo KS, Cappuccino A, Pimenta L (2003) Cervical disc replacement-porous coated motion prosthesis: a comparative biomechanical analysis showing the key role of the posterior longitudinal ligament. Spine 28:S176–S185. doi:10.1097/01.BRS.0000092219.28382.0C
McAfee PC, Cunningham BW, Devine J, Williams E, Yu-Yahiro J (2003) Classification of heterotopic ossification (HO) in artificial disk replacement. J Spinal Disord Tech 16:384–389
Mehren C, Suchomel P, Grochulla F, Barsa P, Sourkova P, Hradil J, Korge A, Mayer HM (2006) Heterotopic Ossification in Total Cervical Artificial Disc Replacement. Spine 31:2802–2806. doi:10.1097/01.brs.0000245852.70594.d5
Mummaneni PV, Burkus JK, Haid RW, Traynelis VC, Zdeblick TA (2007) Clinical and radiographic analysis of cervical disc arthroplasty compared with allograft fusion: a randomized controlled clinical trial. J Neurosurg Spine 6:198–209. doi:10.3171/spi.2007.6.3.198
Nabhan A, Ahlhelm F, Pitzen T, Steudel WI, Jung J, Shariat K, Steimer O, Bachelier F, Pape D (2007) Disc replacement using Pro-Disc C versus fusion: a prospective randomised and controlled radiographic and clinical study. Eur Spine J 16:423–430. doi:10.1007/s00586-006-0226-5
Nabhan A, Ahlhelm F, Shariat K, Pitzen T, Steimer O, Steudel WI, Pape D (2007) The ProDisc-C prothesis clinical and radiological experience 1 year after surgery. Spine 32:1935–1941. doi:10.1097/BRS.0b013e31813162d8
Park JH, Roh KH, Cho JY, Ra YS, Rhim SC, Noh SW (2008) Comparative analysis of cervical arthroplasty using Mobi-C® and anterior cervical discectomy and fusion using the solis®-cage. J Korean Neurosurg Soc 44:217–221. doi:10.3340/jkns.2008.44.4.217
Phillips MF, Garfin SR (2005) Cervical disc replacement. Spine 30:S27–S33. doi:10.1097/01.brs.0000175192.55139.69
Pickett GE, Sekhon LH, Sears WR, Duggal N (2006) Complications with cervical arthroplasty. J Neurosurg Spine 4:98–105. doi:10.3171/spi.2006.4.2.98
Porchet F, Metcalf N (2004) Clinical outcomes with the Prestige II Cervical Disc: preliminary results from a prospective randomized clinical trial. Neurosurg Focus 17:E6. doi:10.3171/foc.2004.17.3.6
Puttlitz CM, Rousseau MA, Xu Z, Hu S, Tay BK, Lotz JC (2004) Intervertebral disc replacement maintains cervical spine kinetics. Spine 29:2809–2814. doi:10.1097/01.brs.0000147739.42354.a9
Robertson JT, Papadopoulos SM, Traneylis VC (2005) Assessment of adjacent-segment disease in patients treated with cervical fusion or arthroplasty: a prospective 2-year study. J Neurosurg Spine 3:417–423
Robertson JT, Metcalf NH (2004) Long-term outcome after implantation of the Prestige I disc in an end-stage indication: 4 year results from a pilot study. Neurosurg Focus 17:E10. doi:10.3171/foc.2004.17.3.10
Sasso RC, Best NM (2008) Cervical Kinematics after fusion and Bryan Disc Arthroplasty. J Spinal Disord Tech 21:19–22. doi:10.1097/BSD.0b013e3180500778
Sekhon L (2004) Cervical arthroplasty in the treatment of spondylotic myelopathy: 18-month results. Neurosurg Focus 17(3):E8. doi:10.3171/foc.2004.17.3.8
Sola S, Hebecker R, Knoop M, Mann S (2005) Bryan cervical disc prosthesis—three years follow-up. Eur Spine J 14(Suppl 1):38
Vital JM, Pointillart V, Gille O, Aurouer N (2007) Les prothèses cervicales constituent-elles un réel progrès dans la pathologie dégénérative? e-mémoires de l’Académie Nationale de Chirurgie 6(3):45–50
Wigfield C, Gill S, Nelson R, Metcalf N, Robertson J (2002) The new Frenchay artificial cervical joint: results from a two-year pilot study. Spine 27:2446–2452. doi:10.1097/00007632-200211150-00006
Wigfield C, Gill S, Nelson R, Langdon I, Metcalf N, Robertson J (2002) Influence of an artificial cervical joint compared with fusion on adjacent-level motion in the treatment of degenerative cervical disc disease. J Neurosurg 96(Suppl 1):17–21
Acknowledgments
We are grateful to the following co-investigators, who participated in the study: P. DAM-HIEU, MD, Brest, France; N. GANGNET, MD, Bordeaux, France; P. MANGIONE, MD, Pessac, France; H. PERSON, MD, Brest, France; J. STECKEN, MD, Orléans, France.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Beaurain, J., Bernard, P., Dufour, T. et al. Intermediate clinical and radiological results of cervical TDR (Mobi-C®) with up to 2 years of follow-up. Eur Spine J 18, 841–850 (2009). https://doi.org/10.1007/s00586-009-1017-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-009-1017-6