Abstract
Purpose
Many studies have been published on the beneficial effects of oral carbohydrate solutions (OCS) administered prior to surgery. However, the risk of pulmonary aspiration cannot be excluded in all patients undergoing anesthesia. But, there are few studies on the safety of OCS at lung aspiration.
Methods
Experiments were conducted with mice (Nine- to ten-week-old male BALB/c mice weighted 23–26 g). Lung aspiration was performed by intratracheal administration of OCS and its major constituents, fructose and maltodextrin. Bronchoalveolar lavage fluid (BALF) was collected 3 and 24 h after lung aspiration. The level of Tumor necrosis factor-α (TNF-α), interleukin-6 (IL-6) and macrophage inflammatory protein-2 (MIP-2) were measured in BALF. The total white blood cell, neutrophil counts, wet to dry ratio and histological examination were performed in BALF and lung tissue, respectively, at 24 h after aspiration.
Results
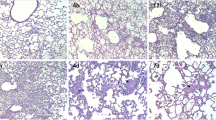
The OCS increased the level of TNF-α, IL-6 and MIP-2 at 3 h and the neutrophil count at 24 h in BALFs, compared to a phosphate-buffered saline (PBS) group. The increase in IL-6 level induced by OCS was maintained for 24 h. The OCS also increased the number of white blood cells and the percentage of neutrophils in BALFs. Compared to fructose, maltodextrin significantly increased the production of MIP-2 in BALFs. OCS and maltodextrin also increased neutrophil recruitment in lung tissue.
Conclusion
Aspiration of OCS may cause inflammation of the lungs. The preoperative use of OCS may require caution under specific clinical conditions, such as patients at risk of lung aspiration.





Similar content being viewed by others
References
Smith I, Kranke P, Murat I, Smith A, O'Sullivan G, Soreide E, et al. Perioperative fasting in adults and children: guidelines from the European Society of Anaesthesiology. Eur J Anaesthesiol. 2011;28(8):556–69.
Practice guidelines for preoperative fasting and the use of pharmacologic agents to reduce the risk of pulmonary aspiration: application to healthy patients undergoing elective procedures: an updated report by the American Society of Anesthesiologists Committee on Standards and Practice Parameters. Anesthesiology. 2011;114(3):495–511.
Schricker T, Lattermann R. Perioperative catabolism. Can J Anaesth. 2015;62:182–93.
Ljungqvist O, Scott M, Fearon KC. Enhanced recovery after surgery: a review. JAMA Surg. 2017;152:292–8.
Hausel J, Nygren J, Thorell A, Lagerkranser M, Ljungqvist O. Randomized clinical trial of the effects of oral preoperative carbohydrates on postoperative nausea and vomiting after laparoscopic cholecystectomy. Br J Surg. 2005;92:415–21.
Pogatschnik C, Steiger E. Review of preoperative carbohydrate loading. Nutr Clin Pract. 2015;30:660–4.
Hausel J, Nygren J, Lagerkranser M, Hellstrom PM, Hammarqvist F, Almstrom C, et al. A carbohydrate-rich drink reduces preoperative discomfort in elective surgery patients. Anesth Analg. 2001;93(5):1344–50.
Lobo DN, Hendry PO, Rodrigues G, Marciani L, Totman JJ, Wright JW, et al. Gastric emptying of three liquid oral preoperative metabolic preconditioning regimens measured by magnetic resonance imaging in healthy adult volunteers: a randomised double-blind, crossover study. Clin Nutr. 2009;28(6):636–41.
Nakamura M, Uchida K, Akahane M, Watanabe Y, Ohtomo K, Yamada Y. The effects on gastric emptying and carbohydrate loading of an oral nutritional supplement and an oral rehydration solution: a crossover study with magnetic resonance imaging. Anesth Analg. 2014;118(6):1268–73.
Vist GE, Maughan RJ. The effect of osmolality and carbohydrate content on the rate of gastric emptying of liquids in man. J Physiol. 1995;486:523–31.
Crapo PA, Reaven G, Olefsky J. Plasma glucose and insulin responses to orally administered simple and complex carbohydrates. Diabetes. 1976;25:741–7.
Kielhorn BA, Senagore AJ, Asgeirsson T. The benefits of a low dose complex carbohydrate/citrulline electrolyte solution for preoperative carbohydrate loading: focus on glycemic variability. Am J Surg. 2018;215:373–6.
Shime N, Ono A, Chihara E, Tanaka Y. [Current status of pulmonary aspiration associated with general anesthesia: a nationwide survey in Japan] (in Japanese with English abstract). Masui (Jpn J Anesthesiol). 2005;54:1177–85.
Smith MD, McCall J, Plank L, Herbison GP, Soop M, Nygren J. Preoperative carbohydrate treatment for enhancing recovery after elective surgery. Cochrane Database Syst Rev. 2014(8):Cd009161.
Asai T. Editorial II: who is at increased risk of pulmonary aspiration? Br J Anaesth. 2004;93:497–500.
Van de Putte P, Vernieuwe L, Jerjir A, Verschueren L, Tacken M, Perlas A. When fasted is not empty: a retrospective cohort study of gastric content in fasted surgical patientsdagger. Br J Anaesth. 2017;118:363–71.
Zadák Z, Kent-Smith L. Basics in clinical nutrition: commercially prepared formulas. E Spen Eur E J Clin Nutr Metab. 2009;4:e212–5.
Matute-Bello G, Downey G, Moore BB, Groshong SD, Matthay MA, Slutsky AS, et al. An official American Thoracic Society workshop report: features and measurements of experimental acute lung injury in animals. Am J Respir Cell Mol Biol. 2011;44(5):725–38.
Asti C, Ruggieri V, Porzio S, Chiusaroli R, Melillo G, Caselli GF. Lipopolysaccharide-induced lung injury in mice. I. Concomitant evaluation of inflammatory cells and haemorrhagic lung damage. Pulm Pharmacol Ther. 2000;13:61–9.
Ito Y, Betsuyaku T, Nasuhara Y, Nishimura M. Lipopolysaccharide-induced neutrophilic inflammation in the lungs differs with age. Exp Lung Res. 2007;33:375–84.
Practice Guidelines for Preoperative Fasting and the Use of Pharmacologic Agents to Reduce the Risk of Pulmonary Aspiration: Application to Healthy Patients Undergoing Elective Procedures: An Updated Report by the American Society of Anesthesiologists Task Force on Preoperative Fasting and the Use of Pharmacologic Agents to Reduce the Risk of Pulmonary Aspiration. Anesthesiology. 2017;126(3):376–93.
Bannister WK, Sattilaro AJ. Vomiting and aspiration during anesthesia. Anesthesiology. 1962;23:251–64.
Warner MA, Warner ME, Weber JG. Clinical significance of pulmonary aspiration during the perioperative period. Anesthesiology. 1993;78:56–62.
Blitt CD, Gutman HL, Cohen DD, Weisman H, Dillon JB. “Silent” regurgitation and aspiration during general anesthesia. Anesth Analg. 1970;49:707–13.
Muscedere J, Dodek P, Keenan S, Fowler R, Cook D, Heyland D. Comprehensive evidence-based clinical practice guidelines for ventilator-associated pneumonia: prevention. J Crit Care. 2008;23:126–37.
Nygren J. The metabolic effects of fasting and surgery. Best Pract Res Clin Anaesthesiol. 2006;20:429–38.
Ljungqvist O, Nygren J, Hausel J, Thorell A. Preoperative nutrition therapy—novel developments. Näringsforskning. 2000;44:3–7.
Thiele RH, Raghunathan K, Brudney CS, Lobo DN, Martin D, Senagore A, et al. American Society for Enhanced Recovery (ASER) and Perioperative Quality Initiative (POQI) joint consensus statement on perioperative fluid management within an enhanced recovery pathway for colorectal surgery. Perioper Med (Lond). 2016;5:24.
Hofman DL, van Buul VJ, Brouns FJ. Nutrition, health, and regulatory aspects of digestible maltodextrins. Crit Rev Food Sci Nutr. 2016;56:2091–100.
Sandhu BK, Jones BJ, Brook CG, Silk DB. Oral rehydration in acute infantile diarrhoea with a glucose-polymer electrolyte solution. Arch Dis Child. 1982;57:152–4.
O’Brien WJ, Rowlands DS. Fructose-maltodextrin ratio in a carbohydrate-electrolyte solution differentially affects exogenous carbohydrate oxidation rate, gut comfort, and performance. Am J Physiol Gastrointest Liver Physiol. 2011;300:G181–9.
Salgado RM, Cruz-Castañeda O, Elizondo-Vázquez F, Pat L, De la Garza A, Cano-Colín S, et al. Maltodextrin/ascorbic acid stimulates wound closure by increasing collagen turnover and TGF-β1 expression in vitro and changing the stage of inflammation from chronic to acute in vivo. J TissueViabil. 2017;26(2):131–7.
Kobayashi Y. Neutrophil infiltration and chemokines. Crit Rev Immunol. 2006;26:307–16.
McColl SR, Clark-Lewis I. Inhibition of murine neutrophil recruitment in vivo by CXC chemokine receptor antagonists. J Immunol. 1999;163:2829–35.
Tosun B, Yava A, Açıkel C. Evaluating the effects of preoperative fasting and fluid limitation. Int J Nurs Pract. 2015;21:156–65.
Bilku DK, Dennison AR, Hall TC, Metcalfe MS, Garcea G. Role of preoperative carbohydrate loading: a systematic review. Ann R Coll Surg Engl. 2014;96:15–22.
Acknowledgments
This study was supported by a grant (Number: CRI 16012-1) from Chonnam National University Hospital Research Institute of Clinical Medicine.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
All authors have no conflicts of interest to declare.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Kim, J., Kim, HS., Kim, M. et al. Oral carbohydrate solution cause an inflammatory response when aspirated into the lungs in mice. J Anesth 35, 86–92 (2021). https://doi.org/10.1007/s00540-020-02873-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-020-02873-w