Abstract
Objectives
Seizure duration and morphology, postictal suppression, and sympathetic nervous system activation are all recommended as assessments of adequate seizure in electroconvulsive therapy (ECT). However, blood pressure and heart rate are not typically assessed as part of sympathetic nervous system activation because of the administration of anesthetic or cardiovascular agents during ECT. Although the pupils are known to reflect to the activity of autonomic nervous system and the degree of brain damage, previous studies have not examined the relationship between seizure of electroconvulsive therapy and pupillary response.
Methods
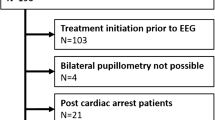
We conducted 98 sessions of ECT with 13 patients, divided into two groups according to seizure quality: (1) adequate or (2) inadequate. Pupillary light reflex [% constriction = (maximum resting pupil size {MAX} − minimum pupil size after light stimulation)/MAX × 100] was measured using a portable infrared quantitative pupilometer before anesthesia induction and immediately after electrical stimulation.
Results
The number regarded as adequate was 67 times and as inadequate was 31 times. Maximum pupil size at the control and immediately after electrical stimulation was similar between the adequate and inadequate groups. Pupillary light reflex was similar at the control between both groups, but significantly smaller immediately after stimulation in the adequate group (2.5 ± 3.6%) compared with the inadequate group (10.6 ± 11.5%). Receiver operating characteristic curve analysis revealed that pupillary light reflex (> 5.5%) predicted adequate seizure.
Conclusions
The current findings suggest that pupillary constriction immediately after ECT could provide a helpful method for assessing the efficacy of ECT.

Similar content being viewed by others
References
Saito S. Anesthesia management for electroconvulsive therapy: hemodynamic and respiratory management. J Anesth. 2005;19(2):142–9.
Abrams R. Stimulus titration and ECT dosing. J ECT. 2002;18(1):3–9. discussion 14 – 5.
Krystal AD, Coffey CE, Weiner RD, Holsinger T. Changes in seizure threshold over the course of electroconvulsive therapy affect therapeutic response and are detected by ictal EEG ratings. J Neuropsychiatry Clin Neurosci. 1998;10(2):178–86.
Sackeim HA, Devanand DP, Prudic J. Stimulus intensity, seizure threshold, and seizure duration: impact on the efficacy and safety of electroconvulsive therapy. Psychiatr Clin North Am. 1991;14(4):803–43.
Nishikawa K, Yamakage M. Effects of the concurrent use of a reduced dose of propofol with divided supplemental remifentanil and moderate hyperventilation on duration and morphology of electroconvulsive therapy-induced electroencephalographic seizure activity: a randomized controlled trial. J Clin Anesth. 2017;37:63–8.
Duma A, Pal S, Johnston J, Helwani MA, Bhat A, Gill B, Rosenkvist J, Cartmill C, Brown F, Miller JP, Scott MG, Sanchez-Conde F, Jarvis M, Farber NB, Zorumski CF, Conway C, Nagele P. High-sensitivity cardiac troponin elevation after electroconvulsive therapy: a prospective, observational cohort study. Anesthesiology. 2017;126(4):643–52.
Pourafkari N, Pourafkari L, Nader ND. Electroconvulsive therapy for depression following acute coronary syndromes: a concern for the anesthesiologist. J Clin Anesth. 2016;31:223–8.
Fasick V, Spengler RN, Samankan S, Nader ND, Ignatowski TA. The hippocampus and TNF: common links between chronic pain and depression. Neurosci Biobehav Rev. 2015;53:139–59.
Sud R, Spengler RN, Nader ND, Ignatowski TA. Antinociception occurs with a reversal in alpha 2-adrenoceptor regulation of TNF production by peripheral monocytes/macrophages from pro- to anti-inflammatory. Eur J Pharmacol. 2008;588(2–3):217–31.
Shirozu K, Setoguchi H, Tokuda K, Karashima Y, Ikeda M, Kubo M, Nakamura K, Hoka S. The effects of anesthetic agents on pupillary function during general anesthesia using the automated infrared quantitative pupillometer. J Clin Monit Comput. 2017;31(2):291–6.
Taylor WR, Chen JW, Meltzer H, Gennarelli TA, Kelbch C, Knowlton S, Richardson J, Lutch MJ, Farin A, Hults KN, Marshall LF. Quantitative pupillometry, a new technology: normative data and preliminary observations in patients with acute head injury. Technical note. Journal of neurosurgery. 2003;98(1):205–13.
Zafar SF, Suarez JI. Automated pupillometer for monitoring the critically ill patient: a critical appraisal. J Crit Care. 2014;29(4):599–603.
Yuan D, Spaeth EB, Vernino S, Muppidi S. Disproportionate pupillary involvement in diabetic autonomic neuropathy. Clin Auton Res. 2014;24(6):305–9.
Rollins MD, Feiner JR, Lee JM, Shah S, Larson M. Pupillary effects of high-dose opioid quantified with infrared pupillometry. Anesthesiology. 2014;121(5):1037–44.
Sawayama E, Takahashi M, Inoue A, Nakajima K, Kano A, Sawayama T, Okutomi T, Miyaoka H. Moderate hyperventilation prolongs electroencephalogram seizure duration of the first electroconvulsive therapy. J ECT. 2008;24(3):195–8.
Azuma H, Fujita A, Sato K, Arahata K, Otsuki K, Hori M, Mochida Y, Uchida M, Yamada T, Akechi T, Furukawa TA. Postictal suppression correlates with therapeutic efficacy for depression in bilateral sine and pulse wave electroconvulsive therapy. Psychiatry Clin Neurosci. 2007;61(2):168–73.
Porter RJ, Douglas K, Knight RG. Monitoring of cognitive effects during a course of electroconvulsive therapy: recommendations for clinical practice. J ECT. 2008;24(1):25–34.
Kranaster L, Hoyer C, Janke C, Sartorius A. Bispectral index monitoring and seizure quality optimization in electroconvulsive therapy. Pharmacopsychiatry. 2013;46(4):147–50.
Akobeng AK. Understanding diagnostic tests 3: receiver operating characteristic curves. Acta Paediatr. 2007;96(5):644–7.
Perkins NJ, Schisterman EF. The inconsistency of “optimal” cutpoints obtained using two criteria based on the receiver operating characteristic curve. Am J Epidemiol. 2006;163(7):670–5.
McCall WV, Andrade C, Sienaert P. Searching for the mechanism(s) of ECT’s therapeutic effect. J ECT. 2014;30(2):87–9.
Vutskits L. General anesthetics to treat major depressive disorder: clinical relevance and underlying mechanisms. Anest Analg. 2018;126(1):208–16.
Bar KJ, Ebert A, Boettger MK, Merz S, Kiehntopf M, Jochum T, Juckel G, Agelink MW. Is successful electroconvulsive therapy related to stimulation of the vagal system? J Affect Disord. 2010;125(1–3):323–9.
Couret D, Boumaza D, Grisotto C, Triglia T, Pellegrini L, Ocquidant P, Bruder NJ, Velly LJ. Reliability of standard pupillometry practice in neurocritical care: an observational, double-blinded study. Crit Care. 2016;20:99.
Li X, Chen CJ, Tan F, Pan JR, Xing JB, Zhu QQ, Hei ZQ, Zhou SL. Effect of dexmedetomidine for attenuation of propofol injection pain in electroconvulsive therapy: a randomized controlled study. J Anesth. 2018;32(1):70–6.
Bryson EO, Aloysi AS, Farber KG, Kellner CH. Individualized anesthetic management for patients undergoing electroconvulsive therapy: a review of current practice. Anesthesia analgesia. 2017;124(6):1943–56.
McNett M, Moran C, Janki C, Gianakis A. Correlations between hourly pupillometer readings and intracranial pressure values. J Neurosci Nurs. 2017;49(4):229–34.
Funding
Supported by departmental funding only.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declared that they have no conflict of interest.
Additional information
Faculty of Medical sciences, Kyushu University Institutional Review Board Clinical Research number #28-77.
About this article
Cite this article
Shirozu, K., Murayama, K., Karashima, Y. et al. The relationship between seizure in electroconvulsive therapy and pupillary response using an automated pupilometer. J Anesth 32, 866–871 (2018). https://doi.org/10.1007/s00540-018-2566-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-018-2566-9