Abstract
Purpose
We hypothesized that cooling hyperbaric bupivacaine from 23 to 5 °C may limit the intrathecal spread of bupivacaine and therefore increase the success rate of unilateral spinal anesthesia and decrease the rate of hemodynamic complications.
Methods
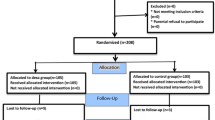
A hundred patients scheduled for elective unilateral inguinal hernia surgery were randomly allocated to receive 1.8 ml of 0.5 % hyperbaric bupivacaine intrathecally at either 5 °C (group I, n = 50) or at 23 °C (group II, n = 50). Following spinal block at the L2-3 interspace, the lateral decubitus position was maintained for 15 min. Unilateral spinal anesthesia was assessed and confirmed at 15 and 30 min. The levels of sensory and motor block on the operative side were evaluated until complete resolution.
Results
The rate of unilateral spinal anesthesia at 15 and 30 min was significantly higher in group I (p = 0.015 and 0.028, respectively). Hypotensive events and bradycardia were significantly rarer in group I (p = 0.014 and 0.037, respectively). The density and viscosity of the solution at 5 °C was significantly higher than at 23 °C (p < 0.0001). Compared with group II, sensory block peaked later in group I (17.4 vs 12.6 min) and at a lower level (T9 vs T7), and two-segment regression of sensory block (76.4 vs 84.3 min) and motor block recovery was shorter (157.6 vs 193.4 min) (p < 0.0001).
Conclusions
Cooling of hyperbaric bupivacaine to 5 °C increased the density and viscosity of the solution and the success rate of unilateral spinal anesthesia, and decreased the hemodynamic complication rate.
Similar content being viewed by others
References
Casati A, Fanelli G, Berti M, et al. Cardiac performance during unilateral lumbar spinal block after crystalloid preload. Can J Anaesth. 1997;44:623–8.
Casati A, Fanelli G, Cappelleri G, Borghi B, Cedrati V, Torri G. Low dose hyperbaric bupivacaine for unilateral spinal anaesthesia. Can J Anaesth. 1998;45:850–4.
Fanelli G, Casati DA, Aldegheri G, Beccaria P, Berti M, Leoni A. Cardiovascular effects of two different regional anaesthetic techniques for unilateral leg surgery. Acta Anaesthesiol Scand. 1998;42:80–4.
Cappelleri G, Aldegheri G, Danelli G, et al. Spinal anesthesia with hyperbaric levobupivacaine and ropivacaine for outpatient knee arthroscopy: a prospective, randomized, double-blind study. Anesth Analg. 2005;101:77–82.
Fanelli G, Borghi B, Casati A, Bertini L, Montebugnoli M, Torri G. Unilateral bupivacaine spinal anesthesia for outpatient knee arthroscopy. Can J Anaesth. 2000;47:746–51.
Enk D. Unilateral spinal anaesthesia: gadget or tool? Curr Opin Anaesthesiol. 1998;11:511.
Esmaoglu A, Boyaci A, Ersoy O, Guler G, Talo R, Tercan E. Unilateral spinal anaesthesia with hyperbaric bupivacaine. Acta Anaesthesiol Scand. 1998;42:1083–7.
Apaydın Y, Erk G, Sacan O, Tiryaki C, Taspinar V. Characteristics of unilateral spinal anesthesia at different speeds of intrathecal injection. J Anesth. 2011; 25(3):380-5.
Arai YCP, Ueda W, Takimoto E, Manabe M. The influence of hyperbaric bupivacaine temperature on the spread of spinal anesthesia. Anesth Analg. 2006;102:272–5.
Stienstra R, Van Poorten F, Gielen M, Kroon JANW. The influence of temperature and speed of injection on the distribution of a solution containing bupivacaine and methylene blue in a spinal canal model. Reg Anesth. 1990;15:6.
Stienstra R, Gielen M, van Poorten F, Kroon JW. Spinal anesthesia with plain bupivacaine 0.5%: regression of sensory and motor blockade with different temperatures of the anesthetic solution. Anesth Analg. 1989;69:593–7.
Beardsworth D, Lambert DH. Warming 0.5% bupivacaine to 37 degrees C increases duration of spinal anesthesia. Reg Anesth. 1989;14:199.
Callesen T, Jarnvig I, Thage B, Krantz T, Christiansen C. Influence of temperature of bupivacaine on spread of spinal analgesia. Anaesthesia. 1991;46:17–9.
Hanci VYS, Bostankolu E, Ayoglu H, Okyay RD, Erdogan G, Yilmaz M, Turan IO. Lowering the temperature of levobupivacaine limits its spread in spinal anaesthesia. J Turk Anaesth Int Care. 2010;38:364–71.
McLeod G. Density of spinal anaesthetic solutions of bupivacaine, levobupivacaine, and ropivacaine with and without dextrose. Br J Anaesth. 2004;92:547–51.
Lui AP, Polis T, Cicutti N. Densities of cerebrospinal fluid and spinal anaesthetic solutions in surgical patients at body temperature. Can J Anaesth. 1998;45:297–303.
Borghi B, Stagni F, Bugamelli S, et al. Unilateral spinal block for outpatient knee arthroscopy: a dose-finding study. J Clin Anesth. 2003;15:351–6.
Casati A, Fanelli G, Cappelleri G, et al. Effects of spinal needle type on lateral distribution of 0.5% hyperbaric bupivacaine. Anesth Analg. 1998;87:355–9.
Kuusniemi K, Leino K, Lertola K, Pihlajamaki K, Pitkanen M. Comparison of two spinal needle types to achieve a unilateral spinal block. J Anesth. 2013;27:224–30.
Casati A, Fanelli G, Cappelleri G, et al. Does speed of intrathecal injection affect the distribution of 0.5% hyperbaric bupivacaine? Br J Anaesth. 1998;81:355–7.
Casati A, Fanelli G, Cappelleri G, et al. Effects of speed of intrathecal injection on unilateral spinal block by 1% hyperbaric bupivacaine. A randomized, double-blind study. Minerva Anestesiol. 1999;65:5–10.
Enk D, Prien T, Van Aken H, Mertes N, Meyer J, Brüssel T. Success rate of unilateral spinal anesthesia is dependent on injection flow. Reg Anesth. 2001;26:420.
Meyer J, Enk D, Penner M. Unilateral spinal anesthesia using low-flow injection through a 29-gauge Quincke needle. Anesth Analg. 1996;82:1188–91.
Acknowledgments
The authors wish to acknowledge the help of Prof. Dr. Leyla Karaoglu for her valuable help with statistical analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors have no conflict of interest to disclose.
About this article
Cite this article
Tomak, Y., Erdivanli, B., Sen, A. et al. Effect of cooled hyperbaric bupivacaine on unilateral spinal anesthesia success rate and hemodynamic complications in inguinal hernia surgery. J Anesth 30, 26–30 (2016). https://doi.org/10.1007/s00540-015-2081-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-015-2081-1