Abstract
Purpose
Single-lung ventilation (SLV) is thought to reduce regional cerebral oxygen saturation (rSO2). In this study, we evaluated changes in rSO2 during SLV and their correlation with perioperative changes in cognitive function.
Methods
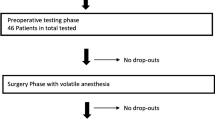
Sixty-nine patients participated in this study, each of whom received combined thoracic epidural and general anesthesia. rSO2 was measured using INVOS 5100 (Somanetics, Troy, MI, USA) before anesthesia (baseline value) and until SLV was completed. Patient cognitive function was assessed using the mini mental state examination (MMSE) on the day before surgery (baseline) and then repeated 4 days after surgery. The patients were classified into two groups: with (desaturation group, group D) and without (nondesaturation group, group N) cerebral desaturation during SLV. Cerebral desaturation was defined as a reduction of rSO2 during SLV less than 80% of the baseline value. An intergroup comparison was made between perioperative cognitive function findings (MMSE score change between baseline and 4th day after surgery). We also examined the correlation between the duration of desaturation during SLV and perioperative MMSE score changes in group D patients.
Results
Seventeen patients were included in group D. The MMSE score decrease was significantly higher in group D as compared to that in group N (P < 0.05). The duration of desaturation time was significantly negatively correlated with MMSE score change (r 2 = 0.444, P < 0.05).
Conclusion
Duration of cerebral desaturation time during SLV correlates with MMSE score. Additional studies are needed to determine whether intervention against cerebral desaturation during SLV can prevent postoperative cognitive dysfunction.

Similar content being viewed by others
References
Brodsky JB. Approaches to hypoxemia during single-lung ventilation. Curr Opin Anaesthesiol. 2001;14:71–6.
Jobis FF. Noninvasive, infrared monitoring of cerebral and myocardial oxygen sufficiency and circulatory parameters. Science. 1977;198:1264–7.
Taillefer MC, Denault AY. Cerebral near-infrared spectroscopy in adult heart surgery: systematic review of its clinical efficacy. Can J Anesth. 2005;52:79–87.
Kussman BD, Wypij D, DiNardo JA, Newburger J, Jonas RA, Bartlett J, McGrath E, Laussen PC. An evaluation of bilateral monitoring of cerebral monitoring of cerebral oxygen saturation during pediatric cardiac surgery. Anesth Analg. 2005;101:1294–300.
Murkin JM. Perioperative detection of brain oxygenation and clinical outcomes in cardiac surgery. Semin Cardiothorac Vasc Anesth. 2004;8:13–4.
Goldman S, Sutter F, Ferdinand F, Trace C. Optimizing intraoperative cerebral oxygen delivery using noninvasive cerebral oximetry decreases the incidence of stroke for cardiac surgical patients. Heart Surg Forum. 2004;7:376–81.
Casati A, Fanelli G, Pietropaoli P, Proietti R, Tufano R, Danelli G, Fierro G, Cosmo GD, Servillo G. Continuous monitoring of cerebral oxygen saturation in elderly patients undergoing major abdominal surgery minimizes brain exposure to potential hypoxia. Anesth Analg. 2005;101:740–7.
Green DW. A retrospective study of changes in cerebral oxygenation using a cerebral oximeter in older patients undergoing prolonged major abdominal surgery. Eur J Anaesthesiol. 2007;24:230–4.
Olsson C, Thelin S. Regional cerebral saturation monitoring with perfusion: diagnostic performance and relationship to postoperative stroke. J Thorac Cardiovasc Surg. 2006;131:371–9.
Ogasawara K, Konno H, Yukawa H, Endo H, Inoue T, Ogawa A. Transcranial regional cerebral oxygen saturation monitoring during carotid endarterectomy as a predictor of postoperative hyperperfusion. Neurosurgery. 2003;53:309–14.
Rigamonti A, Scandroglio M, Minicucci F, Magrin S, Carozzo A, Casati A. A clinical evaluation of near-infrared cerebral oximetry in the awake patient to monitor cerebral perfusion during carotid endarterectomy. J Clin Anesth. 2005;17:426–30.
Mille T, Tachimiri ME, Klersy C, Ticozzelli G, Bellinzona G, Blangetti I, Pirrelli S, Lovotti M, Odero A. Near infrared spectroscopy monitoring during carotid endarterectomy: which threshold value is critical? Eur J Vasc Endovasc Surg. 2004;27:646–50.
Dujovny M, Slavin KV, Hernandez G, Geremia GK, Ausman JL. Use of cerebral oximetry to monitor brain oxygenation reserves for skull base surgery. Skull Base Surg. 1994;4:117–21.
Edmonds HL Jr. Multi-modality neurophysiologic monitoring for cardiac surgery. Heart Surg Forum. 2002;5:225–8.
Hemmerling TM, Bluteau MC, Kazan R, Braco D. Significant decrease of cerebral oxygen saturation during single-lung ventilation measured using absolute oximetry. Br J Anaesth. 2008;101:870–5.
Tonner PH, Kampen J, Scholz J. Pathophysiological changes in the elderly. Best Pract Res Clin Anaesthesiol. 2003;17:163–77.
Liu LL, Wiener-Kronish JP. Perioperative anesthesia issues in the elderly. Crit Care Clin. 2003;19:641–56.
Newman S, Stygall J, Hirani S, Shaefi S, Maze M. Postoperative cognitive dysfunction after noncardiac surgery: a systematic review. Anesthesiology. 2007;106:572–90.
Moller JT, Cluitmans P, Rasmussen LS, Houx P, Rasmussen H, Canet J, Rabbitt P, Jolles J, Larsen K, Hanning CD, Langeron O, Johnson T, Lauven PM, Kristensen PA, Bielder A, van Beem H, Fraidakis O, Silverstein JH, Beneken JE, Gravenstein JS. Long-term postoperative cognitive dysfunction in the elderly ISPOCD 1 study. ISPOCD investigators. International Study of Post-Operative Cognitive Dysfunction. Lancet. 1998;351:857–61.
Newman MF, Kirchner JL, Phillips-Bute B, Gaver V, Grocott H, Jones RH, Mark DB, Reves JG, Blumenthal JA. Longitudinal assessment of neurocognitive function after coronary-artery bypass surgery. N Engl J Med. 2001;344:395–402.
Paquet C, Deschamps A, Denault AY, Couture P, Carrier M, Babin D, Levesque S, Piquette D, Lambert J, Tardif JC. Baseline regional cerebral oxygen saturation correlates with left ventricular systolic and diastolic function. J Cardiothorac Vasc Anesth. 2008;22:840–6.
Tonz M, Bachmann D, Mettler D, Kaiser G. Effects of one-lung ventilation on pulmonary hemodynamics and gas exchange in the newborn. Eur J Pediatr Surg. 1997;7:212–5.
Slater JP, Guarino T, Stack J, Vinod K, Bustami RT, Brown JM, Rodriguez AL, Magovern CL, Zaubler T, Freundlich K, Parr GVS. Cerebral oxygen desaturation predicts cognitive decline and longer hospital stay after cardiac surgery. Ann Thorac Surg. 2009;87:36–45.
Hong SW, Shim JK, Choi YS, Kim DH, Chang BC, Kwak YL. Prediction of cognitive dysfunction and patients outcome following valvular heart surgery and the role of cerebral oximetry. Eur J Cardiothorac Surg. 2008;33:560–5.
Sauer AM, Kalkman C, Dijk DV. Postoperative cognitive decline. J Anesth. 2009;23:256–9.
Folstein M, Folstein S, McHygh P. “MMSE”. A practical method for grading the cognitive state of patients for clinician. J Psychiatry Res. 1975;12:189–99.
Mondimore FM, Damlouji N, Folstein MF, Tune L. Post-ECT confusional states associated with elevated serum anticholinergic levels. Am J Psychiatry. 1983;140:930–1.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Suehiro, K., Okutai, R. Duration of cerebral desaturation time during single-lung ventilation correlates with mini mental state examination score. J Anesth 25, 345–349 (2011). https://doi.org/10.1007/s00540-011-1136-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-011-1136-1