Abstract
Purpose
We conducted a double-blind placebo-controlled study to investigate the effects of the intraoperative intravenous infusion of adenosine 5′-triphosphate (ATP) on intraoperative hemodynamics and postoperative pain in patients undergoing major orofacial surgery.
Methods
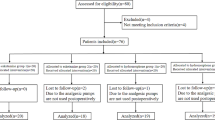
Thirty patients (age, 16–42 years; 16 males/14 females) scheduled for sagittal split ramus osteotomy were assigned in a double-blind fashion to receive intraoperative intravenous infusion of ATP (n = 15) or saline (n = 15). Anesthesia was induced and maintained with propofol, fentanyl, and vecuronium. Local anesthesia was added for intraoperative analgesia. In the ATP group, ATP was infused at a rate of 160 μg·kg−1·min−1 throughout surgery. Postoperative pain was managed with intravenous patient-controlled analgesia (PCA) with morphine. The intensity of postoperative pain was assessed with a verbal numeric rating scale (NRS). Morphine consumption was also assessed.
Results
There were no differences in demographic, anesthetic, and surgical data between the ATP and placebo groups. Intraoperatively, ATP effectively suppressed responses of blood pressure and heart rate to painful surgical stimuli. There were no differences in postoperative NRS scores between the two groups. However, postoperative morphine consumption was significantly less in the ATP group, compared with the placebo group, throughout the 72-h postoperative observation period. Cumulative morphine consumption for 72 h postoperatively was 47% less with ATP, compared with placebo. No adverse effect of ATP was observed.
Conclusion
Our data suggest that intraoperative ATP infusion can blunt hemodynamic responses to surgical stimuli and produce prolonged analgesia in patients undergoing major orofacial surgery.
Similar content being viewed by others
References
Sawynok J. Adenosine receptor activation and nociception. Eur J Pharmacol. 1998;317:1–11.
Segerdahl M, Ekblom A, Sandelin K, Wickman M, Sollevi A. Peroperative adenosine infusion reduces the requirements for isoflurane and postoperative analgesics. Anesth Analg. 1995;80:1145–1149.
Segerdahl M, Persson E, Ekblom A, Sollevi A. Peroperative adenosine infusion reduces isoflurane concentrations during general anesthesia for shoulder surgery. Acta Anaesthesiol Scand. 1996;40:792–797.
Segerdahl M, Irestedt L, Sollevi A. Antinociceptive effect of perioperative adenosine infusion in abdominal hysterectomy. Acta Anaesthesiol Scand. 1997;41:473–479.
Zarate E, Sa Rego MM, White PF, Duffy L, Shearer VE, Griffin JD, Whitten CW. Comparison of adenosine and remifentanil infusions as adjuvants to desflurane anesthesia. Anesthesiology. 1999;90:956–963.
Fukunaga AF, Alexander GE, Stark CW. Characterization of the analgesic actions of adenosine: comparison of adenosine and remifentanil infusions in patients undergoing major surgical procedures. Pain. 2003;101:129–138.
Chizh BA, Illes P. P2X receptors and nociception. Pharmacol Rev. 2001;53:553–568.
Jarvis MF. Contributions of P2X(3) homometric and heterometric channels to acute and chronic pain. Expert Opin Ther Targets. 2003;7:513–522.
Shinoda M, Ozaki N, Sugiura Y. Involvement of ATP and its receptors on nociception in rat model of masseter muscle pain. Pain. 2008;134:148–157.
Gordon JL. Extracellular ATP: effects, sources and fate. Biochem J. 1986;233:309–319.
Agteresch HJ, Dagnelie PC, van den Berg JW, Wilson JH. Adenosine triphosphate: established and potential clinical applications. Drugs. 1999;58:211–232.
Hayashida M, Fukuda K, Fukunaga A, Meno A, Sato K, Tarui K, Arita H, Kaneko Y, Hanaoka K. Analgesic effect of intravenous ATP on postherpetic neuralgia in comparison with responses to intravenous ketamine and lidocaine. J Anesth. 2005;19:31–35.
Fukuda K, Hayashida M, Fukunaga A, Kasahara M, Koukita Y, Ichinohe T, Kaneko Y. Pain-relieving effects of intravenous ATP in chronic intractable orofacial pain: an open-label study. J Anesth. 2007;21:24–30.
Segerdahl M, Sollevi A. Adenosine and pain relief: a clinical overview. Drug Dev Res. 1998;45:151–158.
Hayashida M, Fukuda K, Fukunaga A. Clinical application of adenosine and ATP for pain control. J Anesth. 2005;19:225–235.
Ramsay MA, Savege TM, Simpson BR, Goodwin R. Controlled sedation with alphaxalone-alphadolone. BMJ 1974;2:656–659.
Biaggioni I, Olafsson B, Robertson RM, Hollister AS, Robertson D. Cardiovascular and respiratory effects of adenosine in conscious man; evidence for chemoreceptor activation. Circ Res. 1987;61:779–786.
Fukunaga AF. Adenosine compounds. In: White PF, editor. Textbook of intravenous anesthesia. Baltimore: Williams & Wilkins; 1997. 413–432.
Schindler M, Harris CA, Hayes B, Papotti M, Humphrey PP. Immunohistochemical localization of adenosine A1 receptors in human brain regions. Neurosci Lett. 2001;297:211–215.
Goadsby PJ, Hoskin KL, Storer RJ, Edvinsson L, Connor HE. Adenosine A1 receptor agonists inhibit trigeminovascular nociceptive transmission. Brain. 2002;125:1392–1401.
Hayashida M, Fukunaga A, Fukuda K, Sakurai S, Mamiya H, Ichinohe T, Kaneko Y, Hanaoka K. The characteristics of intravenous adenosine-induced antinociception in a rabbit model of acute nociceptive pain: a comparative study with remifentanil. Anesth Analg. 2006;103:1004–1010.
Faulds D, Chrisp P, Buckley MM. Adenosine. An evaluation of its use in cardiac diagnostic procedures, and in the treatment of paroxysmal supraventricular tachycardia. Drugs. 1991;41:596–624.
Satya P. Kunapuli SP, Daniel JL. P2 receptor subtypes in the cardiovascular system. Biochem J. 1998;336:513–523.
Rongen GA, Floras JS, Lenders JW, Thien T, Smits P. Cardiovascular pharmacology of purines. Clin Sci (Lond). 1997;92:13–24.
Burnstock G. Pathophysiology and therapeutic potential of purinergic signaling. Pharmacol Rev. 2006;58:58–86.
Fukunaga AF, Flacke WE, Bloor BC. Hypotensive effects of adenosine and adenosine triphosphate compared with sodium nitroprusside. Anesth Analg. 1982;61:273–278.
Tamai I, Tsuji A. Transporter-mediated permeation of drugs across the blood-brain barrier. J Pharm Sci. 2000;89:1371–1388.
Murakami H, Ohkura A, Takanaga H, Matsuo H, Koyabu N, Naito M, Tsuruo T, Ohtani H, Sawada Y. Functional characterization of adenosine transport across the BBB in mice. Int J Pharm. 2005;290:37–44.
Cansev M. Uridine and cytidine in the brain: their transport and utilization. Brain Res Rev. 2006;52:389–397.
Cronstein BN. Adenosine, an endogenous anti-inflammatory agent. J Appl Physiol. 1994;76:5–13.
Montesinos MC, Desai A, Delano D, Chen JF, Fink JS, Jacobson MA, Cronstein BN. Adenosine A2A or A3 receptors are required for inhibition of inflammation by methotrexate and its analog MX-68. Arthritis Rheum. 2003;48:240–247.
Author information
Authors and Affiliations
About this article
Cite this article
Handa, T., Fukuda, KI., Hayashida, M. et al. Effects of intravenous adenosine 5′-triphosphate on intraoperative hemodynamics and postoperative pain in patients undergoing major orofacial surgery: a double-blind placebo-controlled study. J Anesth 23, 315–322 (2009). https://doi.org/10.1007/s00540-009-0751-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-009-0751-6