Abstract
Purpose
The inflammatory response triggered by transfusion is implicated in the pathophysiology of transfusion-related immunomodulation. The authors hypothesized that two distinctive autotransfusion methods, acute normovolemic hemodilution (ANH) and preoperative donation (PD), have different influences on both inflammatory mediator generation during storage and the inflammatory response after a transfusion. The purpose of this study was to compare the plasma concentrations of neutrophil elastase (NE), interleukin (IL)-6, IL-8, and IL-10 in patients who underwent either of these two autologous transfusion methods.
Methods
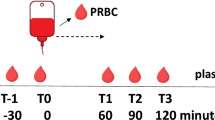
With institutional review board approval, the plasma concentrations of the above inflammatory mediators were determined in 23 patients with ANH and 8 patients with PD at the following time points: after anesthetic induction, at the end of the operation, and the morning of postoperative day 1. The concentrations of these inflammatory mediators were also measured in the donated blood obtained by either ANH or PD before retransfusion.
Results
The mean storage durations were 3.7 h and 6.1 days for ANH and PD, respectively. Higher concentrations of NE and IL-10 were detected in the PD blood than in the ANH blood. Long duration of storage and/or low temperature may have been responsible for the increased NE and IL-10 concentrations in the PD blood. However, the difference between the two groups in the extent of increased plasma concentrations of these inflammatory mediators was not statistically significant.
Conclusion
Inflammatory mediators were significantly increased in PD blood during storage compared to the blood obtained by ANH. However, their effects on the inflammatory response elicited in the recipients were not significantly different.
Similar content being viewed by others
References
Landers DF, Hill GE, Wong KC, Fox IJ. Blood transfusioninduced immunomodulation. Anesth Analg. 1996;82:187–204.
Blajchman MA. Allogeneic blood transfusions, immunomodulation, and postoperative bacterial infection: do we have the answers yet? Transfusion. 1997;37:121–125.
Heiss MM. Risk of allogeneic transfusions. Br J Anaesth. 1998;81(Suppl 1):16–19.
Jensen LS, Hokland M, Nielsen HJ. A randomized controlled study of the effect of bedside leucocyte depletion on the immunosuppressive effect of whole blood transfusion in patients undergoing elective colorectal surgery. Br J Surg. 1996;83:973–977.
Innerhofer P, Luz G, Spotl L, Hobisch-Hagen P, Schobersberger W, Fischer M, Nussbaumer W, Lochs A, Irschick E. Immunologic changes after transfusion of autologous or allogeneic buffy coatpoor versus white cell-reduced blood to patients undergoing arthroplasty. I. Proliferative T-cell responses and the balance of helper and suppressor T cells. Transfusion. 1999;39:1089–1096.
Weisbach V, Wanke C, Zingsem J, Zimmermann R, Eckstein R. Cytokine generation in whole blood, leukocyte-depleted and temporarily warmed red blood cell concentrates. Vox Sang. 1999;76:100–106.
Muylle L, Joos M, Wouters E, De Bock R, Peetermans ME. Increased tumor necrosis factor alpha (TNF alpha), interleukin 1, and interleukin 6 (IL-6) levels in the plasma of stored platelet concentrates: relationship between TNF alpha and IL-6 levels and febrile transfusion reactions. Transfusion. 1993;33:195–199.
Heddle NM, Klama L, Singer J, Richards C, Fedak P, Walker I, Kelton JG. The role of the plasma from platelet concentrates in transfusion reactions. N Engl J Med. 1994;331:625–628.
Silliman CC, Voelkel NF, Allard JD, Elzi DJ, Tuder RM, Johnson JL, Ambruso DR. Plasma and lipids from stored packed red blood cells cause acute lung injury in an animal model. J Clin Invest. 1998;101:1458–1467.
Looney MR, Gropper MA, Matthay MA. Transfusion-related acute lung injury: a review. Chest. 2004;126:249–258.
Heiss MM, Fraunberger P, Delanoff C, Stets R, Allgayer H, Strohlein MA, Tarabichi A, Faist E, Jauch KW, Schildberg FW. Modulation of immune response by blood transfusion: evidence for a differential effect of allogeneic and autologous blood in colorectal cancer surgery. Shock. 1997;8:402–408.
Avall A, Hyllner M, Bengtson JP, Carlsson L, Bengtsson A. Postoperative inflammatory response after autologous and allogeneic blood transfusion. Anesthesiology. 1997;87:511–516.
Biedler AE, Schneider SO, Seyfert U, Rensing H, Grenner S, Girndt M, Bauer I, Bauer M. Impact of alloantigens and storageassociated factors on stimulated cytokine response in an in vitro model of blood transfusion. Anesthesiology. 2002;97:1102–1109.
Domen RE. Adverse reactions associated with autologous blood transfusion: evaluation and incidence at a large academic hospital. Transfusion. 1998;38:296–300.
Covin RB, Ambruso DR, England KM, Kelher MR, Mehdizadehkashi Z, Boshkov LK, Masuno T, Moore EE, Kim FJ, Silliman CC. Hypotension and acute pulmonary insufficiency following transfusion of autologous red blood cells during surgery: a case report and review of the literature. Transfus Med. 2004;14:375–383.
Lisander B, Ivarsson I, Jacobsson SA. Intraoperative autotransfusion is associated with modest reduction of allogeneic transfusion in prosthetic hip surgery. Acta Anaesthesiol Scand. 1998;42:707–712.
Zallen G, Offner PJ, Moore EE, Blackwell J, Ciesla DJ, Gabriel J, Denny C, Silliman CC. Age of transfused blood is an independent risk factor for postinjury multiple organ failure. Am J Surg. 1999;178:570–572.
Kristiansson M, Soop M, Saraste L, Sundqvist KG. Cytokines in stored red blood cell concentrates: promoters of systemic inflammation and simulators of acute transfusion reactions? Acta Anaesthesiol Scand. 1996;40:496–501.
Shanwell A, Kristiansson M, Remberger M, Ringden O. Generation of cytokines in red cell concentrates during storage is prevented by prestorage white cell reduction. Transfusion. 1997;37:678–684.
Tolksdorf B, Frietsch T, Quintel M, Kirschfink M, Becker P, Lorentz A. Humoral immune response to autologous blood transfusion in hip surgery: whole blood versus packed red cells and plasma. Vox Sang. 2001;81:180–186.
Biffl WL, Moore EE, Offner PJ, Ciesla DJ, Gonzalez RJ, Silliman CC. Plasma from aged stored red blood cells delays neutrophil apoptosis and primes for cytotoxicity: abrogation by poststorage washing but not prestorage leukoreduction. J Trauma. 2001;50:426–431.
Leal-Noval SR, Jara-Lopez I, Garcia-Garmendia JL, Marin-Niebla A, Herruzo-Aviles A, Camacho-Larana P, Loscertales J. Influence of erythrocyte concentrate storage time on postsurgical morbidity in cardiac surgery patients. Anesthesiology. 2003;98:815–822.
Koch CG, Li L, Sessler DI, Figueroa P, Hoeltge GA, Mihaljevic T, Blackstone EH. Duration of red-cell storage and complications after cardiac surgery. N Engl J Med. 2008;358:1229–1239.
Goodnough LT. Acute normovolemic hemodilution. Vox Sang. 2002;83(Suppl 1):211–215.
Jamnicki M, Kocian R, van der Linden P, Zaugg M, Spahn DR. Acute normovolemic hemodilution: physiology, limitations, and clinical use. J Cardiothorac Vasc Anesth. 2003;17:747–754.
Hodge G, Markus C, Nairn J, Hodge S. Effect of blood storage conditions on leucocyte intracellular cytokine production. Cytokine. 2005;32:7–11.
Tylman M, Bengtson JP, Avall A, Hyllner M, Bengtsson A. Release of interleukin-10 by reinfusion of salvaged blood after knee arthroplasty. Intensive Care Med. 2001;27:1379–1384.
Aguilera A, Selgas R. Effect of recombinant human erythropoietin on inflammatory status in dialysis patients. Nephrol Dial Transplant. 2004;19(Suppl 5):V46–V53.
Oldenburg B, van Berge Henegouwen GP, Rennick D, Van Asbeck BS, Koningsberger JC. Iron supplementation affects the production of pro-inflammatory cytokines in IL-10 deficient mice. Eur J Clin Invest. 2000;30:505–510.
Lang K, Suttner S, Boldt J, Kumle B, Nagel D. Volume replacement with HES 130/0.4 may reduce the inflammatory response in patients undergoing major abdominal surgery. Can J Anaesth. 2003;50:1009–1016.
Ickx BE, Bepperling F, Melot C, Schulman C, Van der Linden PJ. Plasma substitution effects of a new hydroxyethyl starch HES 130/0.4 compared with HES 200/0.5 during and after extended acute normovolaemic haemodilution. Br J Anaesth. 2003;91:196–202.
Author information
Authors and Affiliations
About this article
Cite this article
Kotake, Y., Yamamoto, M., Matsumoto, M. et al. Difference in autologous blood transfusion-induced inflammatory responses between acute normovolemic hemodilution and preoperative donation. J Anesth 23, 61–66 (2009). https://doi.org/10.1007/s00540-008-0706-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00540-008-0706-3